Life Extension Magazine®
Alcohol abuse and viral hepatitis are well-known causes of liver disease.
Few people are aware that Nonalcoholic fatty liver disease (NAFLD) and its more severe form, nonalcoholic steatohepatitis (NASH), are responsible for a large share of chronic liver disease cases.1-4
The rates of both NAFLD and NASH have grown exponentially and are expected to increase by 21% and 63%, respectively, by the year 2030.5
NAFLD shows no obvious symptoms until potentially irreversible liver damage has occurred. And there are no medications currently available to treat it.
But researchers have discovered a close link between the health of the liver and the health of the gut.6
They found that unhealthy gut bacteria contribute to NAFLD and beneficial bacteria protect against it, when combined with a healthy lifestyle.6-8
Recent clinical trials have shown that a specialized blend of probiotics, in combination with a healthy lifestyle, can reduce the severity of NAFLD and even stop the harm it does to the liver.7,8
In one study, probiotic supplementation plus following healthy lifestyle advice led to a remarkable 54% reduction in C-reactive protein levels, a measure of inflammation.7
The Threat of Nonalcoholic Fatty Liver Disease
The most common sources of chronic liver damage and liver failure used to be alcohol abuse, and infection of the liver by viruses such as hepatitis B and C.
In recent years, however, liver disease not associated with alcohol or infection has skyrocketed. In this condition, known as Nonalcoholic fatty liver disease (NAFLD), high levels of fatty tissue build up in the liver, slowly destroying it.
NAFLD currently affects approximately 25% of the entire U.S. population, accounts for over 75% of all chronic liver disease, and is a major contributor to the incidence of advanced liver disease.5,9-11
Those people most at risk are the obese and individuals who suffer from high blood sugar.
Men and women with NAFLD usually have no symptoms. It is diagnosed through a combination of blood tests and medical scans. In cases where the diagnosis is not clear,12 a biopsy may be necessary.
Few people give their liver a second thought, but it works tirelessly to filter the blood and detoxify the body.
In the long term, NAFLD can cause fibrosis (scarring) of the liver, significantly impairing normal liver function.13-15 Advanced scarring, known as liver cirrhosis, is irreversible and can lead to liver failure, that is eventually fatal. The only treatment at that point is a liver transplant.16
What You Need to Know
Synbiotics Combat NAFLD
-
Nonalcoholic fatty liver disease (NAFLD) is the most common cause of chronic liver damage. It affects 25% of the U.S. population, and much higher rates of older adults and people who are overweight.
-
There are generally no warning signs or symptoms of NAFLD until damage to the liver is already severe and irreversible. No drugs are currently approved to treat it.
-
Scientists have discovered that the health of the liver is closely related to gut microbiota, the mix of bacteria in the digestive tract.
-
Clinical trials have shown that a carefully designed probiotic and prebiotic blend, combined with following dietary and lifestyle advice, can significantly reduce several markers of NAFLD severity, and even appears to stop the damage it does to the liver.
The Gut-Liver Connection
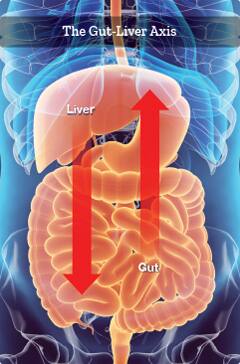
The microorganisms that live in our intestines, or gut, have a critical impact on overall health throughout the body.
An unhealthy mix of gut microbes is increasingly common in populations that consume a modern Western diet. This imbalance has been found to be tied to many chronic ailments.17-19
Improving gut health through diet and the use of probiotics may help reduce the risk of some of these diseases.
The impact of gut microbiota is particularly profound for liver health—so much so that the link is known as the gut-liver axis.18
Here’s why: The majority of blood that circulates away from the intestines feeds directly into the liver through a large vessel called the portal vein. This vein then splits into tiny capillaries that run throughout the liver.
What this means is that most blood-borne substances coming from the digestive system pass through the liver before circulating to other organs and tissues, giving the liver a first shot at processing nutrients, and filtering out and neutralizing toxins.
But this gut-liver axis has a downside: It makes the liver particularly susceptible to harmful compounds and microorganisms coming from the gut. While the liver neutralizes most of these harmful substances, it can be damaged in the process.
With an unhealthy mix of gut microbes, damage occurs to the lining of the intestines, increasing the number of harmful compounds and cells that get into the portal vein and make their way to the liver.18
The makeup of the gut microbiota therefore has a dramatic impact on liver health. While beneficial bacteria are protective, the wrong microbes can do a huge amount of damage to the liver. Researchers believe this is one of the major contributing factors to nonalcoholic fatty liver disease.6
Probiotics Protect Against NAFLD
Due to the rapid increase in NAFLD rates, scientists have been scrambling to find ways to shield the liver against the damage it causes.
Because of the strong link between gut microbes and NAFLD, they decided to focus on probiotics.
Scientists designed a blend of microorganisms they believed was ideal to improve gut health and favorably impact the liver, reducing risk and severity of nonalcoholic fatty liver disease (NAFLD).
This probiotic blend consists of seven beneficial bacteria that are considered to be a part of a healthy gut microbiome. They are:
-
Lactobacillus casei PXN® 37,
-
Lactobacillus rhamnosus PXN® 54,
-
Streptococcus thermophilus PXN® 66,
-
Bifidobacterium breve PXN® 25,
-
Lactobacillus acidophilus PXN® 35,
-
Bifidobacterium longum PXN® 30, and
-
Lactobacillus bulgaricus PXN® 39.
But probiotic organisms can only work if they survive and thrive in the intestines, outcompeting harmful bacteria. Combining the probiotics with prebiotics, compounds that help support the health and functioning of the bacteria, give the probiotic organisms an added boost.
The blend of probiotics and prebiotics is often referred to as synbiotics because of their synergistic activity in improving gut health.
Results of Human Trials

Two randomized clinical trials have evaluated the impact of this new probiotic-prebiotic blend on Nonalcoholic fatty liver disease.
The first study recruited volunteers who were overweight or obese and had a diagnosis of NAFLD. Patients were randomized to receive either the synbiotic blend or a placebo for 28 weeks.7 Both groups were advised to follow recommendations for physical activity and balanced diet.
To determine the effectiveness, researchers evaluated different markers of NAFLD severity. The first was levels of two liver enzymes, ALT (alanine aminotransferase) and AST (aspartate aminotransferase), which spill into the bloodstream when there’s damage to the liver. Higher levels in the blood indicate more liver damage.
The subjects in this study all started out with elevated liver enzyme levels due to NAFLD. At the end of the study, both groups saw a decline in liver enzymes, but those who received the probiotic had a greater drop in levels of ALT and AST of such magnitude that they returned to a normal range.
By the end of the study, another marker of NAFLD severity, the fibrosis score (showing how much scarring is present in the liver), dropped, on average, into the normal range in the probiotic-prebiotic group.
Lastly, this study looked at C-reactive protein, a marker of the inflammation resulting from NAFLD. The probiotic-prebiotic group had a 54% reduction in C-reactive protein levels by the end of the study.
The second study tested the same probiotic-prebiotic blend plus healthy lifestyle advice on people with Nonalcoholic fatty liver disease who were not overweight or obese.8
In these subjects, those taking the probiotic-prebiotic blend saw a larger average drop in liver enzymes, including a significant 17% reduction in AST. The fibrosis score also dropped significantly in the synbiotic group, falling into the normal range, on average, and C-reactive protein was reduced by 46%.
The outcomes of these trials indicate that the new probiotic-prebiotic blend significantly reduces signs of nonalcoholic fatty liver disease (NAFLD) severity, regardless of body weight.
Summary

Nonalcoholic fatty liver disease (NAFLD) occurs in 25% of the U.S. population, and in much higher rates in older and in overweight people.
Over time, without dietary and lifestyle changes, it can progress and damage the liver, potentially leading to liver cirrhosis and liver failure.
There are currently no FDA-approved medical treatments to prevent or reduce liver damage. However, scientists have discovered that liver health is tied to a healthy mix of gut microbes.
A carefully chosen blend of probiotic micro-organisms, combined with a prebiotic to support their survival, has been shown in clinical trials to reduce the severity of liver disease caused by NAFLD.
If you have any questions on the scientific content of this article, please call a Life Extension® Wellness Specialist at 1-866-864-3027.
References
- Armstrong MJ, Adams LA, Canbay A, et al. Extrahepatic complications of nonalcoholic fatty liver disease. Hepatology. 2014 Mar;59(3):1174-97.
- Available at: https://www.ncbi.nlm.nih.gov/pubmed/. Accessed October 2, 2019.
- Wong RJ, Aguilar M, Cheung R, et al. Nonalcoholic steatohepatitis is the second leading etiology of liver disease among adults awaiting liver transplantation in the United States. Gastroenterology. 2015 Mar;148(3):547-55.
- Younossi ZM, Stepanova M, Afendy M, et al. Changes in the prevalence of the most common causes of chronic liver diseases in the United States from 1988 to 2008. Clin Gastroenterol Hepatol. 2011 Jun;9(6):524-30 e1; quiz e60.
- Estes C, Razavi H, Loomba R, et al. Modeling the epidemic of nonalcoholic fatty liver disease demonstrates an exponential increase in burden of disease. Hepatology. 2018 Jan;67(1):123-33.
- Shen F, Zheng RD, Sun XQ, et al. Gut microbiota dysbiosis in patients with Nonalcoholic fatty liver disease. Hepatobiliary Pancreat Dis Int. 2017 Aug 15;16(4):375-81.
- Eslamparast T, Poustchi H, Zamani F, et al. Synbiotic supplementation in nonalcoholic fatty liver disease: a randomized, double-blind, placebo-controlled pilot study. Am J Clin Nutr. 2014 Mar;99(3):535-42.
- Mofidi F, Poustchi H, Yari Z, et al. Synbiotic supplementation in lean patients with Nonalcoholic fatty liver disease: a pilot, randomised, double-blind, placebo-controlled, clinical trial. Br J Nutr. 2017 Mar;117(5):662-8.
- Alkhouri N, Scott A. An Update on the Pharmacological Treatment of Nonalcoholic Fatty Liver Disease: Beyond Lifestyle Modifications. Clin Liver Dis (Hoboken). 2018 Apr;11(4):82-6.
- Hassan K, Bhalla V, El Regal ME, et al. Nonalcoholic fatty liver disease: a comprehensive review of a growing epidemic. World J Gastroenterol. 2014 Sep 14;20(34):12082-101.
- Younossi Z, Anstee QM, Marietti M, et al. Global burden of NAFLD and NASH: trends, predictions, risk factors and prevention. Nat Rev Gastroenterol Hepatol. 2018 Jan;15(1):11-20.
- Available at: https://www.mayoclinic.org/diseases-conditions/nonalcoholic-fatty-liver-disease/symptoms-causes/syc-20354567. Accessed October 2, 2019.
- Calzadilla Bertot L, Adams LA. The Natural Course of Nonalcoholic Fatty Liver Disease. Int J Mol Sci. 2016 May 20;17(5):774.
- Musso G, Gambino R, Cassader M, et al. Meta-analysis: natural history of Nonalcoholic fatty liver disease (NAFLD) and diagnostic accuracy of non-invasive tests for liver disease severity. Ann Med. 2011 Dec;43(8):617-49.
- Noureddin M, Vipani A, Bresee C, et al. NASH Leading Cause of Liver Transplant in Women: Updated Analysis of Indications For Liver Transplant and Ethnic and Gender Variances. Am J Gastroenterol. 2018 Nov;113(11):1649-59.
- Available at: https://www.uptodate.com/contents/cirrhosis-beyond-the-basics. Accessed October 2, 2019.
- Biragyn A, Ferrucci L. Gut dysbiosis: a potential link between increased cancer risk in ageing and inflammaging. The Lancet Oncology. 2018;19(6):e295-e304.
- Tripathi A, Debelius J, Brenner DA, et al. The gut-liver axis and the intersection with the microbiome. Nat Rev Gastroenterol Hepatol. 2018 Jul;15(7):397-411.
- Zhang YJ, Li S, Gan RY, et al. Impacts of gut bacteria on human health and diseases. Int J Mol Sci. 2015 Apr 2;16(4):7493-519.

