Life Extension Magazine®
Alpha Lipoic AcidThe "Universal" Antioxidant That Generates Energy And Is An Effective Treatment For Diabetes |
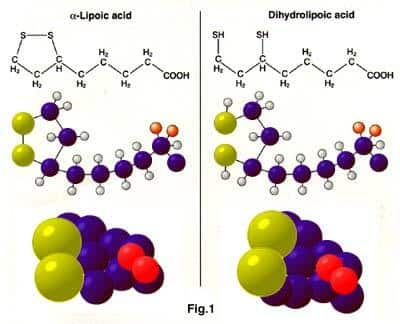
| Until recently, the antioxidants that fight damaging free radicals within the body were thought to be largely specialized in function. For example, the major function or the enzyme superoxide dismutase (SOD) is to inhibit superoxide radicals beta carotene's primary role is to quench singlet oxygen radicals; vitamin E's main role is to break lipid peroxide chains in cell membranes the primary function of glutathione is to knock out damaging hydroxyl radicals,and coenzyme Q10 (CoQ) fights off oxyradicals produced in the mitochondria (the power plants of the cells),which occurs in part as a result of CoQ's role in the generation of energy. Universal AntioxidantsIn recent years, however, Dr. Russell J. Reiter of the University of Texas at Austin and other scientists have produced evidence that the pineal hormone melatonin is a highly potent "universal" antioxidant found in virtually every cell of the body, and that it counteracts excessive free radical activity via several mechanisms in cell membranes as well as in the interior of cells. Melatonin plays an especially important role in fighting free radicals in the brain, where far more oxyradicals are generated than in any other part of the body because of the enormous amount of oxygen needed for brain metabolism. The discovery of the "universal" antioxidant power of melatonin is evidence of the existence of all purpose antioxidants that have across the board action against a wide spectrum of free radicals, and which, presumably, can substitute for the more specialized antioxidants when this becomes necessary. The "Universal" Action of Alpha Lipoic AcidThere is now evidence of another "universal" antioxidant called alpha lipoic acid, which not only has potent,antioxidant action in virtually all the tissues of the body, but also is a co-factor for some of the key enzymes (alpha keto acid dehydrogeneses) involved to generating energy from food and oxygen in mitochondria. Alpha Lipoic Acid is known by a variety of names including thioctic acid, 1,2-dithiolane-3-pentanoic acid, 1,2-dithiolane-3 valeric acid, and 6,8-thioctic acid. Alpha lipoic acid functions as a co-factor for energy production as lipomide and is also called lipoate when functioning in this manner. When alpha lipoic acid was first isolated in the early 195Os, it was tentatively classified as a vitamin because of its vitamin like properties, but was later found (unlike vitamins) to be synthesized in both animals and humans. The method by which alpha lipoic acid is synthesized within the body has not yet been fully characterized but it appears as if two of its precursors are octanoate and the sulphur amino acid cysteine. Recent findings show that both alpha lipoic acid and its reduced form dihydrolipoic acid (DHLA) (Fig. 1) function as potent within the body and that both these compounds may be effective in preventing and treating the complications of diabetes and, perhaps, aging itself. Before we delve into the potential therapeutic benefits of alpha lipoic acid and DHLA, let's take a look at the findings showing their antioxidant properties. |
Alpha Lipoic Acid |
Criteria For The Evaluation Of AntioxidantsOne of the leading free radical researchers in the world is Lester packer, who leads the Membrane Bioenergetics Group and Department of Molecular & Cell Biology at the University of California at Berkeley. Dr. Packer's recent review article entitled "Alpha-Lipoic Acid As A Biological Antioxidant" (in the journal Free radical Biology & Medicine--see Life Extension Abstracts presents a compelling case for the "universal" antioxidant properties of alpha lipoic acid. In his article, Dr. Packer proposes that the following biochemical criteria be considered when evaluating the antioxidant potential of a compound:
Dr. Packer then presents other important criteria when considering the preventive and therapeutic applications of antioxidant:
After presenting these criteria, Dr. Packer makes it clear that an antioxidant need only meet a few of them to play an important role in the body. "A substance need not excel in meeting all the criteria to be considered a good antioxidant. For example, Vitamin E acts only in the membrane or lipid domains, its dominant action is to quench lipid peroxyl, and it has little or no activity against radicals in the aqueous phase, yet it is considered one of the central antioxidants of the body. Epidemiological studies are confirming its role in the prevention of numerous oxidant related diseases, such as heart disease". This is also true with regard to betacarotene, which has a specialized role (the quenching of singlet oxygen radicals) in the body, The long awaited findings of a long awaited findings of a long term study of the role of beta carotene in the prevention of age related diseases will show that subjects who took high levels of beta carotene every other day for 5 years had 50% fewer coronary or vascular events than subjects not taking beta carotene, and that the subjects taking beta carotene developed only a small fraction of the cancers developed in the control group. We'll be reporting the extraordinary details of these findings in Life Extension Magazine as soon as they are published. Dr. Packer's Conclusions About After reviewing hundreds of studies dealing with the antioxidant properties of alpha lipoic acid, Dr. Packer came to the following conclusions: "An 'ideal' antioxidant would fulfill all of the above criteria. The alpha lipoic redox couple approaches the ideal; it has been called the 'universal antioxidant'. Alpha lipoic acid is readily absorbed from the diet. It is rapidly converted to DHLA in many tissues, as recent advances in assay technique have made evident. One or both of the components of the redox couple in both lipid and aqueous domains. Both DHLA and alpha lipoic acid have metal chelating activity. DHLA acts syngeristically with other antioxidants, including that it is capable of regenerating other antioxidants from their radical or inactive forms. Finally, there is evidence that they may have effects on regulatory proteins and on genes involved in normal growth and metabolism.
|
| LE Magazine March 1996 |
Alpha Lipoic Acid |
Regeneration Of Other AntioxidantsOne of the most beneficial effects of both alpha lipoic acid and DHLA is their ability to regenerate other essential antioxidants such as vitamin C, vitamin E, coenzyme Q10, and glutathione. The evidence is especially strong for the ability of DHLA to recycle vitamin E, which is apparently achieved directly by quenching tocopherol radicals or indirectly by reducing vitamin C or increasing the levels of ubiquinol (a derivative of CoQ) and glutathione, which, in turn, help to regenerate tissue levels oi vitamin E.
According to Dr. Packer: A schematic model has been put together (Fig. 3) showing the known biochemical pathways by which vitamin E is regenerated in cell membranes, so it can do battle again with the damaging lipid peroxide (peroxyl) radicals found in these membranes. Increasing Cellular Glutathione Levels Recent studies have shown that when alpha lipoic acid is added to various types of animal and human cells in tissue culture, it causes a 30-70% increase in cellular glutathione (GSH) levels. GSH levels have been found to increase dramatically in the lungs, liver, and kidney cells of mice injected daily with varying doses of alpha Iipoic acid for 11 days. GSH is an essential antioxidant, which scavenges hydroxyl radicals, the most dangerous type of free radicals found in the body. Analysis of these studies led Dr. Packer to conclude that: "It appears that alpha lipoic acid and DHLA act as antioxidants not only directly, through radical quenching and metal chelation, but indirectly as well, through recycling of other antioxidants and through the induction of increased intracellular levels of glutathione."
|
Alpha Lipoic Acid | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| For Diabetes, Atherosclerosis And Aging Could you use more energy? Most lO-year-olds are bursting with energy. At age 30 most of us still have plenty of energy. By 40 we're beginning to slow down, but experience allows us shortcuts to reduce our energy needs. However by age 60, our energy levels are so depleted that even the wisdom of our years can't make up for our decline. If we make it to 80, we're just a shadow of our former selves. And if we reach 100, we're thrilled just to be alive. It's not just our body as a whole that needs energy it's our individual cells as well. Our brain cells need energy to think, our heart cells need energy to keep our blood circulating, our lung cells need energy to process oxygen, our kidney cells need energy to excrete waste, our bone and muscle and cells need energy for structure and strength, and our immune cells need energy to fight off invading organisms. Depletion of EnergyAlthough most diseases aren't caused by defects in the generation of energy, they're all characterized by energy depletion. Cancer stroke, heart disease, diabetes, and Alzheimer's disease are different in their origin and expression, but they have one thing in common: depletion of the energy-generating capacity of essential cells. Energy depletion caused by diseases produces feelings of weakness, lassitude, depression, despair and hopelessness. Its endpoint is death. As you know such feelings don't just come from overt diseases. Lack of energy is one of the most common complaints in people of all ages Whether reduced energy is caused by subclinical disease states, unpleasant or traumatic experiences, the "normal" ups and downs of life, or the ravages of aging, the feelings are the same. No one likes to feel weak. No one likes to be unable to do things they need to do. No one likes to see life as dark, colorless and unexciting. No one likes pain and suffering. And no one likes to feel as if their life is slipping away from them. The Central Failure In Human LifeThe central failure in human Iife is weakness: lack of strength; lack of purpose; lack of character; and lack of will. The appropriate reaction to weakness and feelings of inadequacy is to build oneself up, but all too often people strive to tear others down, or to rely on others for their self esteem. The results in social terms have been personal conflict, estrangement, war, and victimization. Effects On Health And Medical CareThe effects on health and medical care have been reliance on doctors to "cure" us rather than taking responsibility for our own lives, the focus on the treatment of diseases rather than their prevention, and the attempt to destroy our enemies (viruses, bacteria, and other organisms) rather than to maintain our youth, become stronger, and build up our defenses. A tragic example of the failure of our medical system is the story of Coenzyme Q, (CoQ10 )- an essential component of our energy-generating system -- whose structure and function was discovered in the United States in the late 1950s, but whose role in health care has been almost totally ignored by the U.S. medical establishment, except for the heroic efforts of Dr. Karl Folkers of the University of Texas at Austin. The Discovery Of Coenzyme Q10 In 1956, scientists at the University of Wisconsin under Dr. David E. Green isolated a crystalline yellow compound from beef heart mitochondria (the energy factories of the cell). They gave a few milligrams of this sample to Dr Folkers, who was head of a biochemical research team at Merck Sharp And Dohme Research Laboratories in Rahway, New Jersey. Dr. Folkers and his coworkers at Merck determined that the chemical structure of CoQ is 2,3-dimethoxy-5-methly-6-decaprenyl-1,4-benzoquinone. This structure was revealed at the International Congress on Biochemistry in Vienna in 1958 and published that year in the Journal of the American Chemical Society (60:4752). FIGURE 1
Concentration And Biosynthesis Of CoQCoQ is found in high concentrations (bound to three different proteins) in the heart, liver kidney, and pancreas. The total body content of CoQ has been estimated to be 0.5-1.5 grams. About 50% of the CoQ in the body is found within the mitochondria, where energy is generated on a continuous basis, and where CoQ has three major functions: to help several mitochondrial enzymes convert dietary nutrients (in the presence of oxygen) into the energy "currency" of the body ATP (Adenosine Triphosphate); to help quench some of the free radicals generated in the energy making process; and to help protect the integrity of the mitochondrial membrane. CoQ levels have been shown to be well below normal in patients with a wide variety of diseases including heart disease, cancer and muscular dystrophy, as well as in normally aging people. One likely reason for these age and disease-related declines in CoQ may be the complexity of the process by which CoQ is synthesized within the body. CoQ is biosynthesized from the amino acids phenylalanine and tyrosine with the help of at least eight vitamins and trace elements (figure 2) all of which have vital biochemical functions in the body in addition to the manufacture of CoQ. Anyone with deficiencies of any of these nutrients is likely to become deficient in CoQ. When you add the aging-related breakdown of mitochondrial function which includes unrepairable DNA mutations - it's no wonder that our bodies hunger so much for this remarkable, life-enhancing nutrient. Figure 2The steps in the sequence for the
|
| Possible Therapeutic Mechanisms of Coenzyme Q10 Cardiovascular Disease |
| 1. Correction of CoQ deficiency state. |
| 2. Direct free radical scavenger via semiquinone species. |
| 3. Direct membrane stabilizing activity due to phospholipid protein interactions. |
| 4. Correction of mitochondrial "leak" of electrons during oxidative respiration. |
| 5. Induction of DT diaphorase. |
| 6. Possible effects on prostaglandin metabolism. |
| 7. Inhibition of intracellular phospholipases. |
| 8. Preservation of myocardial Na+- K+ ATPase activity. |
| 9. Stabilization of integrity of Ca+2dependent slow channels. |
Italian Multicenter Study
The Italian study looked at CoQ as an adjunct to conventional drugs in 2,664 heart patients in 173 clinical centers over a 3-month period. The daily dosage of CoQ was 50-150 mg daily with the majority of patients (78%) receiving 100 mg/day. The patients in the study were all rated Class II and III (moderately ill) according to a rating scale based upon the guidelines formulated by the New York Heart Association (NYHA) regarding the symptoms associated with congestive heart failure.
The results showed improvement in virtually all functions measured in the CoQ-treated patients. The proportions of patients exhibiting significant improvement (of at least one point) in clinical symptoms was as follows (Tables 2 and 3): cyanosis 78.1%, edema 78.6%, pulmonary rate 77.8%, enlargement of liver 49.3%, jugular reflex 71.8%, dyspnoea 52.7%, palpitations 75.4%, sweating 79.8%, arrhythmias 63.4%, insomnia 66.8%, and vertigo 73.1%. They also found significant improvement in at least three symptoms in 54% of the patients, indicating major improvement in the quality of their lives.
The investigators summed up their results as follows:
"A significant reduction in blood pressure and heart rate, both in supine and sitting position, was observed in our study. These data confirm the results of a recent study in which CoQ, therapy led to a reduction in peripheral vascular resistance, resulting in a significant decrease in blood pressure. An inhibitory effect of CoQ10 on plasma catecholamine levels in heart failure has been recently reported. In our patients, the reduction in peripheral vascular resistance may be related to an inhibition by CoQ, of the sympathetic overactivity known to be present early in heart failure. The reduction in sweating and palpitations, reported by our patients may result from the same mechanism."
Table 2
Clinical Signs Assessment Results
| Description |
Present at baseline(n) |
Improved at least 1 point after 3 months of CoQ10 treatment (%) |
Statistical signifiance of score variations* |
| Cyanosis |
675 |
78.67 |
P<0.01 |
| Odema |
1764 |
78.06 |
P<0.01 |
| Pulmonary Rates |
1752 |
77.85 |
P<0.01 |
| Enlargement of liver area |
1285 |
49.26 |
P<0.01 |
| Jugular reflux |
713 |
71.81 |
P<0.01 |
Table 3
Clinical Symptoms Assessment Results
| Description |
Present at baseline(n) |
Improved at least 1 point after 3 months of CoQ10 treatment (%) |
Statistical signifiance of score variations* |
| Dyspnoea |
2163 |
52.75 |
P<0.01 |
| Palpitations |
1903 |
75.46 |
P<0.01 |
| Sweating |
1044 |
79.79 |
P<0.01 |
| Subjective arrhythima |
1143 |
63.43 |
P<0.01 |
| Insomnia |
1597 |
62.87 |
P<0.01 |
| Dizziness |
1282 |
73.13 |
P<0.01 |
| Nocturia |
1541 |
53.67 |
P<0.01 |
Treatment Of Hypertension With CoQ
We've been recommending CoQ to patients with cardiovascular disease for years with very good results. Most of these patients start taking CoQ in addition to the conventional drugs they are using. In many cases, they find that prolonged use of CoQ eliminates their need for such prescription drugs, A recent study of the use of CoQ in patients suffering from hypertension (high blood pressure) showed how CoQ can' help patients dispense with their drugs.
This study was conducted by scientists (including Karl Folkers) at the University of Texas at Austin. A total of 109 patients with hypertension were given a variable dose of from 75 to 360 mg/day of CoQ in addition to the existing drug regimen. The patients were followed closely with frequent clinic visits to record blood pressure and make the necessary adjustments in dosage. No side effects or drug interactions were found in any of the patients in the study.
Figure 3
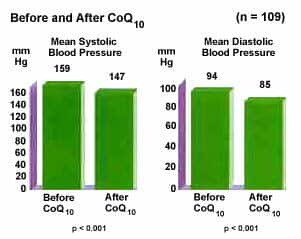 They found that mean systolic blood pressure improved from 159 to 147 and mean diastolic blood pressure improved from 94 to 85 (Figure 3). They also found that, as the patients' functional status and blood pressure improved, and there was a gradual decrease in the need far antihypertensive drugs. Thirty-seven percent of the patients were able to discontinue one drug, 11% discontinued two drugs, and 4% discontinued three drugs. The average time before stopping an anti- hypertensive drug was 4.4 months after starting CoQ, with 62% requiring 3 or more months (Figure 4).
They found that mean systolic blood pressure improved from 159 to 147 and mean diastolic blood pressure improved from 94 to 85 (Figure 3). They also found that, as the patients' functional status and blood pressure improved, and there was a gradual decrease in the need far antihypertensive drugs. Thirty-seven percent of the patients were able to discontinue one drug, 11% discontinued two drugs, and 4% discontinued three drugs. The average time before stopping an anti- hypertensive drug was 4.4 months after starting CoQ, with 62% requiring 3 or more months (Figure 4).
 Figure 4
Figure 4
They concluded that:
"CoQ, a both remarkably safe and cost effective and should be considered among the initial therapeutic modalities alongside such fundamental recommendations as diet exercise and stress reduction and should certainly be considered prior to embarking upon on escalating course of pharmacologic interventions with all of their well established medical and economic hazards."
Interestingly, the Texas scientists found that the most effective way of raising blood levels of CoQ in patients was to give it with a fat containing food (usually peanut butter), which "more than doubled the blood CoQ level on any given dosage." This is not surprising because CoQ is a fat-soluble nutrient that assimilates better in the presence of fat. For this reason, The Foundation now offers CoQ in oil-based, soft-gel capsules, which maximizes its bioavailability within the body.
The Bioavaliability of CoQ
Recent studies at the Royal Danish School of Pharmacy in Denmark have demonstrated that "CoQ in soy bean oil in soft gelatine capsules has higher bioavailability than CoQ formulated with other inert substances." These studies compared CoQ in dry powder form (in capsules) and in tablets with various oil-based formulations of CoQ. It is on the basis of these studies that we now offer CoQ in the same soy-bean-oil formula shown in these studies to produce optimal absorption of CoQ into the body. For further information about this product, call 1-800-64414440 or you can order CoQ10 On-line.
Alpha Lipoic Acid |
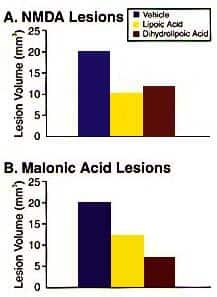
Treatment Of Diabetic NeuropathiesOne of the most damaging complications of diabetes is nerve damage at various sites of the body, which inactivates and weakens muscles, can be extremely painful, and can cause blindness when the retina of the eye is attacked (diabetic retinopathy). Alpha lipoic acid has been shown to be highly effective in treating such neuropathies. The clinical benefits of alpha lipoic acid in diabetics was discovered by Beck and Schneeweiss in 1959. There have been a half dozen or so studies since then confirming these results. In a placebo controlled, double blind study, 20 diabetics were given intravenous infusions of 200 mg a day of alpha lipoic acid or placebo for 21 days. The results showed dramatic improvement in some clinical symptoms in some of the experimental subjects. For example, before being treated with alpha lipoic acid, four patients had severe pain and six patients had moderate pain. After treatment, five of the patients had no pain, four had moderate pain, and only one had severe pain. 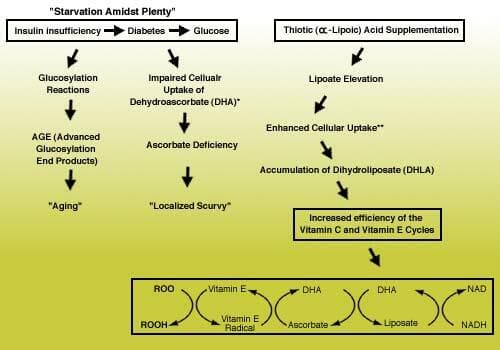 In neither of the above studies, was any improvement found in motor or sensory nerve condition velocity, but scientists point out that such neurophysiology changes can take months or years to occur and that the clear cut clinical benefits found in these studies indicate that continued treatment in diabetics with alpha lipoic acid would likely improve all the functions damaged in diabetic neuropathies. Fig. 4 is a schematic diagram showing the various mechanisms by which alpha lipoic acid supplementation benefits diabetes patients. Alpha Lipoic Acid Protects Against Nerve Cell DeathIn recent years, scientists have found found a method of nerve cell death in stroke and neurodegenerative disorders such as Parkinson's disease and Huntington's disease is excitotoxicity (excessive activation) of NMDA (N-methyl-D-aspartate receptors, and the subsequent generation of nitric oxide, free radical induced lipid peroxidation, aberrantly increased calcium concentration, and mitochondrial dysfunction leading to, depleted energy supplies. There is evidence that depletion of reduced glutathione makes neurons more susceptible to excitotoxicity, and that intact mitochondrial function is essential for neuronal resistance to to excitotoxic attack. It is believed, for example, that reduced levels of the energy currency of the cell (ATP) that accompanies loss of mitochondrial function causes depolarization of neuronal membrane, which exposes NMDA receptors to excessive levels of glutamate. The resulting neurohormonal cascade leads, in many cases, to the death of neurons in the brain, and central and peripheral nervous systems. Scientists have been trying to develop, antyi-excitotoxic therapies that are NMDA receptor antagonists this counter this kind of neuronal cell death. A recent study at the Dept. Of Neurology at the University of Rochester, N.Y.at the University of Rochester Medical Center in Rochester, N.Y. demonstrated that alpha lipoic acid protected against glutamate and malonic acid induced lesions in the brains of male Sprague-Dawley rats. They found a significant reduction of Iesions in animals receiving 10 mg/kg injections of either alpha lipoic: acid or DHLA (Fig. 5). The University of Rochester scientists concluded that: "Excessive activation of NMDA receptors by glutamate has been implicated in the neuronal damage associated with hypoxia/ischemia and hypoglycemia. In contrast, it is hypothesized that chronic neurodegenerative disorders may involve a form of secondary excitotoxicity induced by metabolic or membrane defects rather than excessive glumate release. The fact that thiotic acid (alpha lipoic acid) and dihydrolipoic acid (DHLA) are neuroprotective against both direct and secondary excitotocity suggest a possible role for these endogenous compounds in the treatment of acute and chronic neurological disorders. In this regard, it is worth nothing that thiotic acid is an approved drug for the treatment of diabetic polyneuropathy in Germany" |
Alpha Lipoic Acid |
Sprouting Neurites in Rat NeuronsFurther evidence that alpha lipoic acid can provide therapeutic benefits in patients with neuropathies comes from tissue culture studies in which exposure to alpha lipoic acid resulted in the sprouting of neurites (the small branches at the end of neurons) in early stage rat neurons that far exceeded that round in control neurons.
In this study, which was conducted at the Max Planck Institute For Physiology in Frankfort, Germany, the length of the neurites in the alpha lipoic acid treated neurons was five times that of the untreated neurons and there were far more branchings in the experimental tissue culture neurons. These changes were dose dependent. The more alpha lipoic acid added to the culture medium the greater the density and length of the neurons. The scientists concluded that, since the first step in neuronal regeneration consists of neuronal regeneration consists of neurite elongation, this finding suggests that alpha lipoic acid may be able to help regenerate neurons in humans, which would make it a potentially useful therapy for brain diseases such as Alzheimer's disease, Parkinson's disease, Lou Gehrig's disease, and other age-related neurodegenerative diseases. Improved Memory In Aged MiceTo test the hypothesis treatment with the appropriate free radical scavenger can improve age-related memory deficit, researchers at the Clinical Institute for Mental Health in Mannheim , Germany used aged female NMRI mice, who have demonstrated to exhibit specific well defined memory deficits with advancing age, as well as deficits of NMDA receptors density, which have been linked to age-related cognitive decline. The German scientists gave old. but healthy 20-23 month old female alpha lipoic acid at 100 mg/kg of body weight dissolved in Methocel (1%) administered orally once a day for 15 days, with controls receiving Methocel alone. The treatment was started 14 days before the beginning of behavioral memory testing. A second group of aged mice used for biochemical analysis was also treated for 15 days, and a third group of young (3-4 months) mice were tested as well. The mice were tested on their ability to explore a series of maze like compartments within a special area.
The results showed that two factors influenced learning and memory age and treatment with alpha lipoic acid. The scientists found that long term memory, but not short term memory or learning was impaired in aged female NMRI mice with the repetition of trials. On the other hand, the mice treated with alpha lipoic acid showed marked improvement in learning and memory when compared to aged, untreated controls. This improvement of cognitive function was correlated with an increase in NMDA receptor density, suggesting that the memory enhancing effects of alpha lipoic acid may be linked to the age related decline in the density of these receptors. Effects On Cataract FormationAnother common complication of diabetes is cataract formation in the eye, which can lead to blindness. In animal studies supplementation with alpha lipoic acid has prevented cataract formation caused by inhibition of glutathione synthesis. These studies showed that alpha lipoic acid reduced cataract formation by 40% by protecting the lens of the eye from the loss of vitamin C, vitamin E, and glutathione, which occurred in unsupplemented control animals. Protection Against AtherosclerosisDiabetics have a significantly higher incidence of atherosclerosis than healthy people. There is substantial evidence that the ability of alpha lipoic acid to counteract glucose modification of proteins (glycation) plays an important role in protecting us against atherosclerosis. Both alpha lipoic acid and DHLA have been shown to protect a wide variety of tissues from the protein cross links produced by glycation, and the oxidation of LDL cholesterol, which plays a critical role in the formation of atherosclerotic plaques. This process is a cause of high blood pressure, heart attacks and strokes. Much has been written about the ability of aminoguanidine and chromium to counteract the molecular cross links caused by glycation, but it appears as if alpha lipoic acid may be even more effective than both these compounds in countering the degenerative effects of glycation. This suggests that alpha lipoic acid may play a role in preventing some of the aspects of normal aging, as well as in protecting us against diabetes and neurodegenerative diseases. Protection Against Other PathologiesAmong the other therapeutic uses for alpha lipoic acid has been the treatment of liver disease caused by excessive alcohol intake, as an antidote for various types of Coed poisoning, as a means of countering the effects of ischemic (reduced blood flow) and reperfusion injury, as a means of protecting against heavy metal poisoning, radiation in- jury, and the effects of cigarette smoking. No Adverse Side EffectsIn all the clinical studies to date with alpha lipoic acid, there have been no reported serious adverse side effects, even at the high doses used to treat diabetics and patients suffering from neurodegenerative diseases. Among the mild, reversible side effects found in some patients have been allergic skin reactions, and possible hypoglycemia in diabetics. |

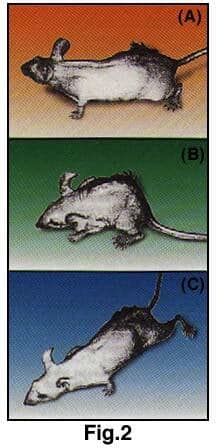 The ability of alpha lipoic acid to regenerate vitamin E was shown graphically in an experiment in which three groups of nude (hairless) 12 week old mice were studied for six weeks. The first group of mice, (A), which received a normal diet during this period, developed normally. The second group of mice, (B), which were fed a vitamin E deficient diet showed marked signs of atrophy and degeneration. The third group of mice, (C), were fed a vitamin E deficient diet supplemented with alpha lipoic acid. These animals showed none of the atrophy and degeneration found in the second group, indicating that the alpha lipoic acid had protected them against the degenerative effects of vitamin E deficiency. (Fig. 2).
The ability of alpha lipoic acid to regenerate vitamin E was shown graphically in an experiment in which three groups of nude (hairless) 12 week old mice were studied for six weeks. The first group of mice, (A), which received a normal diet during this period, developed normally. The second group of mice, (B), which were fed a vitamin E deficient diet showed marked signs of atrophy and degeneration. The third group of mice, (C), were fed a vitamin E deficient diet supplemented with alpha lipoic acid. These animals showed none of the atrophy and degeneration found in the second group, indicating that the alpha lipoic acid had protected them against the degenerative effects of vitamin E deficiency. (Fig. 2).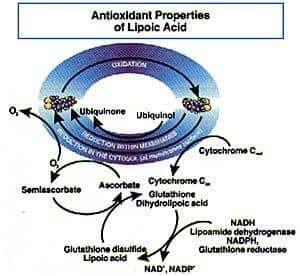
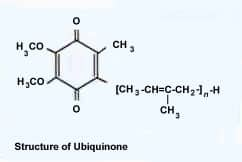 Their discovery was given the name Coenzyme Q10 because it has the biochemical role of a coenzyme (it aids in the action of enzymes) because the letter Q is the first letter of the word quinone, and because it has 10 isoprenoid units on its side chain (figure 1). Dr R.A. Morton and associates at the University of Liverpool in England named CoQ ubiquinone in their 1958 paper in Nature (182:1764) because it is found in virtually every cell of the body.
Their discovery was given the name Coenzyme Q10 because it has the biochemical role of a coenzyme (it aids in the action of enzymes) because the letter Q is the first letter of the word quinone, and because it has 10 isoprenoid units on its side chain (figure 1). Dr R.A. Morton and associates at the University of Liverpool in England named CoQ ubiquinone in their 1958 paper in Nature (182:1764) because it is found in virtually every cell of the body.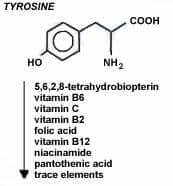 The Japanese Take The Lead
The Japanese Take The Lead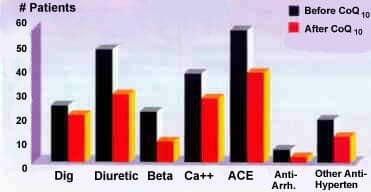 Figure 4
Figure 4