Life Extension Magazine®
You may not be taking the right vitamin
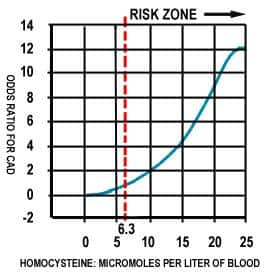
Cardiovascular disease causes 44% of all deaths in the United States. Alzheimer's dementia affects four million Americans. Both cardiovascular and Alzheimer's disease have now been linked to the accumulation of a toxic amino acid called homocysteine. Vitamin supplement users have assumed they are being protected against homocysteine overload, but this article will expose this fallacy and recommend a scientific course of action to follow. The medical establishment woke up to the dangers of homocysteine when The New England Journal of Medicine (Apr 9 1998) and The Journal of the Medical Association (Dec 18 1996) published articles suggesting that vitamin supplements be used to lower homocysteine levels. This same message was published by The Life Extension Foundation 18 years earlier (see "Anti-Aging News"; Nov 1981; pp-85-86). The Life Extension Foundation has uncovered a flaw in the theory that a person can blindly take vitamin supplements to adequately reduce homocysteine levels. While folic acid, vitamin B12, B6, and trimethylglycine (TMG) all lower homocysteine levels, it is impossible for any individual to know if they are taking the proper amount of nutrients unless they have a homocysteine blood test. The clear message from new scientific findings is that there is no safe "normal range" for homocysteine. While commercial laboratories state that normal homocysteine can range from 5 to 15 micro moles per liter of blood, epidemiological data reveals that homocysteine levels above 6.3 cause a steep progressive risk of heart attack (see The American Heart Association's journal Circulation, Nov 15 1995, pp- 2825-2830). One study found each 3-unit increase in homocysteine caused a 35% increase in heart attack risk (see the American Journal of Epidemiology 1996; vol 143, no. 9 845-859). People taking vitamin supplements think they are being protected against the lethal effects of homocysteine, when in reality, even supplement users can have homocysteine levels far above the safe level of 6.3 to 7.0. The Foundation has identified several cases were people suffering from coronary artery disease have lethal levels of homocysteine despite taking the recommended dose (and higher) of vitamin supplements. One case involved a 60-year old man who had previous bypass surgery, but was again suffering angina pain with significant restenosis (re-clogging of the coronary arteries) verified by angiography. This man knew about the dangers of homocysteine, and had been taking more than 15,000 mcg a day of folic acid, along with other homocysteine-lowering vitamins. Because of the angina pain and restenosis, The Foundation recommended a homocysteine blood test. The results came back showing this man had a shockingly high homocysteine reading of 18 in his blood. (Homocysteine levels over 15 have been shown to be extremely dangerous.) The Foundation immediately suggested this man take 6 grams a day of TMG (trimethylglycine), and within one month, his homocysteine level dropped to 4. This case was a wake-up call that one or more homocysteine-lowering factors are not always the solution to keeping homocysteine levels in the safest range (below 7 ). It was also a confirmation of our position that people who want to lower homocysteine must take all of the factors involved into account. Another case involved a healthy person who was taking a 500 mg TMG supplement, 4000 mcg of folic acid, and high doses of many other vitamins on a daily basis. A homocysteine blood test revealed a reading of 11.3 which is far above the safe range of under 7. The addition of 6000 mg of TMG and 500 mg of vitamin B6 was added to his daily program and the homocysteine level dropped to under 9 within 30 days. Homocysteine and Degenerative Diseases Elevated homocysteine can be a sign of a methylation deficiency throughout the body. Methylation is fundamental to DNA repair. If DNA is not adequately repaired, mutations and strand breaks will result. This will lead to accelerated aging, as greater amounts of faulty proteins are synthesized from the damaged DNA. The liver depends on methylation to perform the numerous enzymatic reactions required to detoxify every drug and foreign substance that the body is exposed to. Methylation is required for the growth of new cells. Without it, new cells cannot be made. A study published in the journal Medical Hypothesis (1998, Vol 51, Iss 3, pp-179-221) provides evidence that aging may be exclusively a result of cellular "demethylation," or said differently, the aging process is caused by the depletion of enzymatic "remethylation" activity that is required to maintain and repair cellular DNA. This study suggests that aging may be reversible if aged cells could be programmed to remethylate rather than demethylate. Homocysteine induces cellular damage by interfering with the methylation process. Methylation will be compromised if homocysteine is elevated, and elevated homocysteine is a warning sign that the methylation cycle is not functioning properly. Homocysteine may also damage cells directly by promoting oxidative stress. There is a growing consensus that deficient methylation is the major cause of the degenerative diseases of aging. The consumption of methylation-enhancing nutrients such as TMG, choline, folic acid and vitamin B12 may be one of the most readily available and effective anti-aging therapies presently known. However, it is important to tailor the intake of methylation enhancing nutrients to one's individual biochemistry. The best way of assessing your body's rate of methylation is to measure blood levels of homocysteine. Elevated serum homocysteine is the classic sign of a methylation deficiency (or demethylation) that is correctable with the proper intake of methylation enhancing nutrients such as TMG, folic acid, vitamin B12, etc.
Homocysteine Detox Mechanisms Elevated homocysteine can be reduced (or detoxified) in two ways. The most common pathway is via the remethylation process, where "methyl groups" are donated to homocysteine to transform it into methionine and s-adenosylmethionine (SAMe). A potent remethylation agent is TMG, which stands for tri-methyl-glycine. The "tri" means there are three "methyl" groups on each "glycine" molecule that can be transferred to homocysteine to transform (remethylate) it into methionine and SAMe. The remethylation (or detoxification) of homocysteine requires the following minimum factors: Folic acid, vitamin B12, Zinc and TMG. Choline is another "methyl donor" that helps to lower elevated homocysteine levels and this conversion doesn't require co-factors. However, choline only enhances remethylation in the liver and kidney, which is why it is so important to take adequate amounts of remethylating factors such as folic acid and vitamin B12 to protect the brain and the heart. The published literature emphasizes that folic acid and vitamin B12 are critical nutrients in the remethylation (detoxification) pathway of homocysteine. The other pathway whereby elevated homocysteine is reduced is via its conversion into cysteine and eventually glutathione via the "transsulfuration" pathway. This pathway is dependent on vitamin B6. The amount of vitamin B6 required to lower homocysteine has considerable individual variability. Methionine is the only amino acid that creates homocysteine. People who eat foods that are high in methionine such as red meat and chicken may need more vitamin B6. Elevated homocysteine can occur when there are insufficient vitamin co-factors (such as folate and vitamin B6) to detoxify the amount of methionine being ingested in the diet. Elevated homocysteine can also be caused by a a genetic defect that blocks the transsulfuration pathway by inducing a deficiency of the B6-dependent enzyme cystathione-B-synthase. In this case, high doses of vitamin B6 are required to suppress excessive homocysteine accumulation. Since one would not want to take excessive doses of vitamin B6 (greater than 300-500 mg a day for a long time period), a homocysteine blood test can help determine whether you are taking enough B6 to keep homocysteine levels in a safe range. There are some people who lack an enzyme to convert vitamin B6 into its biologically active form pyridoxal-5-phosphate. In this case, if low-cost vitamin B6 supplements do not sufficiently lower homocysteine levels, then a high cost pyridoxal-5-phosphate supplement may be required. For many people, the daily intake of 500 mg of TMG, 800 mcg of folic acid, 1000 mcg of vitamin B12, 250 mg of choline, 250 mg of inositol, 30 mg of zinc and 100 mg of vitamin B6 will keep homocysteine levels in a safe range. But the only way to really know is to have your blood tested to make sure your homocysteine levels are under 7. If homocysteine levels are too high, then up to 9000 mg of TMG may be needed along wit higher amounts of other remethylation cofactors. Some people with cystathione-B synthase deficiencies will require 500 mg a day or more of vitamin B6 to reduce homocysteine to a safe level. For the prevention of cardiovascular disease, you would want your homocysteine blood level to be under 7. For the prevention of aging, some people have suggested an even lower level is desirable, but more research needs to be done before any scientific conclusions can be made. Alzheimer's Ties to Homocysteine Recent studies show that people with dementia of the Alzheimer's type have elevated levels of homocysteine in their blood. At an international scientific conference held in the Netherlands the week of April 27, 1998, a team of scientists unveiled findings showing a definitive link between elevated homocysteine and Alzheimer's disease. The scientists advocated that people have their blood tested for homocysteine in order to determine how much folic acid should be taken to drop homocysteine levels to the safe range. While the scientists speculated that Alzheimer's disease could be avoided if people reduced their homocysteine levels, it has not yet been determined if homocysteine itself contributes to Alzheimer's disease. A more likely explanation is that elevated homocysteine is an indication of the severe disruption in the methylation pathway that occurs in the brains of Alzheimer's patients. It has been reported that people with Alzheimer's disease have virtually no s-adenosylmethionine (SAMe) in their brains. SAMe is required for DNA methylation (maintenance and repair) of brain cells. Thus, while homocysteine itself may not cause Alzheimer's disease, it appears to represent an important measurable biomarker of a methylation deficit that could cause Alzheimer's and a host of other degenerative diseases. Research reported from Tufts University in 1995 documented the same finding linking elevated homocysteine and Alzheimer's disease and recommended supplementation with folic acid and vitamin B12. It should be noted that dementia can be caused by a deficiency of vitamin B12, folic acid and other nutrients, so another reason that people with dementia of the Alzheimer's type have elevated homocysteine levels is that they could be suffering from a common vitamin deficiency. Numerous studies conducted on the elderly show that deficiencies of folic acid, vitamin B12 and other nutrients is epidemic in the elderly who do not take vitamin supplements. Since both elevated homocysteine and vitamin deficiencies have been linked to dementia, the best approach to prevent and treat dementia (including Alzheimer's dementia) would appear to be testing the blood for elevated homocysteine and taking methylation enhancing nutrients such as folic acid, TMG and vitamin B12. A review of the published literature provides compelling evidence that elevated homocysteine is common in people suffering from dementia of the Alzheimer's type. Since Alzheimer's disease cannot be positively diagnosed until after death, it is impossible to state if all the people in a scientific study are really suffering from Alzheimer's disease. Dementia can be caused by multi-infarct cerebral vascular disease or even by simple vitamin deficiencies. In a study published in the International Journal of Geriatric Psychiatry (Apr 1998, pp-235-239), Dr. McCaddon and his group were able to confirm that patients diagnosed with senile dementia of the Alzheimer's type have significantly elevated levels of homocysteine compared to age-matched controls. An earlier study published in Journal of Gerontology and Biological Sciences (Mar 1997, 76-79) also showed that homocysteine levels were significantly elevated in Alzheimer's disease patients compared to controls. This study found that folic acid and vitamin B12 deficiencies were present in both the Alzheimer's disease patients and the age-matched case controls. The reason why homocysteine levels are so high in people suffering from dementia of the Alzheimer's type is not fully understood. Scientists speculate that severe aberrations in the methylation cycle might be involved in the disease process and that elevated homocysteine is a sign of the breakdown of the methylation cycle. (European Neuropsychoparmacol June 1995, pp-107-114). Other researchers report that abnormal amino acid metabolism early in Alzheimer's causes elevated homocysteine levels. This may lead to neuronal damage that occurs as the disease progresses (Journal of Neural Transmission 1998, 105:2-3, pp 287-294). Remember, the repair and maintenance of cellular DNA is dependent on healthy methylation processes. Methylation deficiencies result in severe damage to brain cells. Under-methylation can cause severe damage to brain cells. Methylation is required for the maintenance of the myelin sheath and the repair of DNA in the brain. Elevated levels of homocysteine in the blood indicate some degree of methylation deficiency that is correctable with an individualized supplement program. The studies showing that homocysteine is a biomarker for the development of dementia of the Alzheimer's type mandates that those seeking to avoid senility should have their blood tested in order to ascertain their homocysteine levels. While it was apparent in the year 1969 that homocysteine was a major cause of vascular disease, the evidence that homocysteine represents a marker of brain cell degeneration is of very recent origin, and has been overlooked by many conventional neurologists. Despite the evidence linking elevated homocysteine to methylation deficiencies that are involved in the Alzheimer's disease process, the Alzheimer's Disease Society has criticized the recommendation that people take folic acid supplements to lower their homocysteine levels. What follows is a direct quote from that organization, "No one knows whether taking (folic acid) supplements will help prevent the disease or whether it will affect the rate at which the disease progresses. The only way this will be discovered is by doing further studies on many, many more patients over a long period of time." The Life Extension Foundation finds perplexing that anybody would warn against taking folic acid supplements at a time when the conventional medical establishment has acknowledged that taking folic acid lowers homocysteine and protects against heart attack, stroke and colon cancer. |