Life Extension Magazine®
Scientific studies confirm that even tiny elevations in homocysteine can significantly increase the risk of heart attack and stroke.
Homocysteine is also related to a host of other negative conditions including depression and a type of blindness. Everyone has homocysteine, just as everyone has cholesterol. It’s a matter of how much. Problems occur when levels get too high. The good news is that homocysteine can be controlled with low-cost dietary supplements. These simple vitamins are scientifically proven to work quickly, without side effects.
What it is
Homocysteine is created when the body uses the amino acid, methionine, for methylation. Methylation is an important reaction in the body, but it leaves homocysteine as a by-product. Normally homocysteine is converted back to methionine, or used to create cysteine and other useful substances. If these conversions are blocked, however, homocysteine accumulates.
Efficient conversion of homocysteine requires certain nutrients. These nutrients neutralize homocysteine’s toxicity by transforming it into useful substances. The most well-studied of the nutrients are folate, vitamin B12 and vitamin B6. Riboflavin, zinc, magnesium and other nutrients also help detoxify homocysteine. Folate deficiency is the most common deficiency associated with homocysteine in Western populations. Studies show that folate supplements (0.5-5 mg/day) have a significant impact on reducing homocysteine levels.
Heart attack and stroke
Homocysteine got a bad rap from its cozy relationship with heart attacks and stroke. The data on homocysteine and these artery diseases is so compelling that researchers have labeled homocysteine an independent risk factor for both stroke and heart attack—a risk similar to smoking, hypertension and diabetes. High cholesterol is a concern for many people, but elevated homocysteine may be a stronger indicator that a person may have a second, or even a first, heart attack.
Homocysteine promotes artery problems in more than one way. Most research centers on its adverse effects on blood flow. Researchers have repeatedly demonstrated that if they give a person a drink containing methionine, homocysteine will shoot up, and blood flow will shrink up. If they give the person a gram of vitamin C before they give the methionine, blood flow will be maintained. It’s assumed that free radicals generated by homocysteine interfere with the ability of blood vessels to expand. Homocysteine interferes with nitric oxide, a substance that relaxes blood vessels. However, this phenomenon may only happen in older people. Taiwanese researchers recently showed that while homocysteine impairs blood flow in people who are 50-70 years old, it doesn’t in people 21-40 years old.
When cholesterol is elevated, usually so is homocysteine. And homocysteine promotes the oxidation of low density lipoprotein (LDL) cholesterol—a phenomenon associated with heart disease. Iron enhances this oxidation, which can be prevented by vitamin E. It apparently takes a fair amount, however. In one study, vitamin E had to be increased three times normal to prevent homocysteine from oxidizing LDL in the presence of iron.
Besides promoting free radicals, homocysteine also creates problems by activating or deactivating genes. The effects are very serious. In blood vessels, homocysteine activates genes that promote coagulation. It also causes smooth muscle cells to proliferate, having the effect of narrowing arteries.
Homocysteine also affects the heart’s energy plants, mitochondria. In the presence of iron or copper, homocysteine creates free radicals that do great damage. The damage in mitochandria is not necessarily stopped by vitamins C and E, according to a new study. People who suspect they might have elevated homocysteine would do well to stay away from food and supplements containing iron or copper. A natural enzyme in the body, catalase, can stop homocysteine reactions in mitochondria. And precursors of glutathione (cysteine, glutamate and glycine) can also prevent homocysteine from damaging mitochondria. But one can be depleted of these enzymes and not know it.
Eye problems
Just as blood vessels leading to and from the heart and brain can be adverstely affected by homocysteine, so can other blood vessels in the body. Central retinal vein occlusion (CRVO), central retinal artery occlusion (CRAO), and nonarteritic anterior ischemic optic neuropathy (NAION) are three eye conditions associated with elevated homocysteine. All are serious conditions that can lead to vision loss. Ischemic CRVO, which usually occurs in one eye only, leads to all sorts of complications including neovascular glaucoma and macular degeneration. There is no good treatment, and in fact, some researchers believe that treatment will make the condition worse.
In a new study from the University of Michigan, the average homocysteine level was 11.58 micromoles per liter for people with CRVO versus 9.49 for people without. Elevated homocysteine was present in half of all eyes with severe loss of vision caused by CRVO. Because these eye conditions are frequently associated with diabetes, hypertension, cardiovascular and other systemic diseases, a complete physical is highly recommended for anyone diagnosed with any of these eye problems.
Erectile dysfunction
If you’re a man taking Viagra for impotence, you may already know you have heart disease. And you may know you have elevated homocysteine. If you’re taking Viagra for impotence and have never been diagnosed with artery disease, it might be prudent to get some heart tests done, including homocysteine levels. If the impotence is being caused by bad blood vessels, there may be problems in other areas of the body as well (such as the heart). Don’t wait until you’re laying on a gurney in the emergency room to find out you’ve got cardiovascular disease.
Liver damage
Most of the studies on homocyteine’s toxicity has focused on arteries. A new study shows that homocysteine can also damage the liver. Researchers in China fed rodents diets containing no folate, low folate, moderate folate and normal folate for four weeks. The lower the folate got, the higher homocysteine levels rose. As homocysteine rose, so did oxidative stress and free radicals.
And, as levels of oxidative stress rose, the activity of two important antioxidant enzymes fell (superoxide dismutase and glutathione peroxidase). Normally these enzymes would increase to meet the challenge of oxidative stress. The researchers think homocysteine interferes with the genes controlling the enzymes. (Editor’s note: the genes for superoxide dismutase and glutathione peroxidase are controlled at least partially by the methylation status of their DNA. Since homocysteine interferes with methylation, it’s reasonable to assume that, over time methylation patterns on the genes are disrupted, causing inactivation. This has been documented in tumor cells which are frequently deficient in the enzymes. The cause is disrupted methylation patterns).
Does coffee increase homocysteine?
 |
Coffee drinkers, take note. Several studies indicate that coffee can influence homocysteine levels. It seems to depend, however, on what kind and how much you drink. Devotees of the French press may want to rethink their brew. According to a recent study, six cups of unfiltered
coffee a day can raise homocysteine levels 10% in two weeks. The average level of homocysteine went from 12.8 micromoles per liter to 14 in a study from the Netherlands.The association between coffee drinking and homocysteine has been noted in other studies, including one conducted in the U.S. which shows that drinking an average of three to four cups of coffee a day (filtered) can increase homocysteine levels one or two micromoles. In the context of heart disease, this is significant.
However, it may be possible to counteract the effects of coffee with folate. Researchers in Norway found that middle-aged people who drank one to four cups of coffee a day, but who had high folate levels, averaged 12.1 µgmol/L of homocysteine compared to 13.8 for people with the least folate. If a person drank five or more cups of coffee a day, but had high folate intake, they could keep their homocysteine levels to 12.1 µgmol/L compared to 15.2 for people with the lowest folate intake.
Although these studies suggest that coffee elevates homocysteine, more work needs to be done. Researchers don’t know how coffee could have this effect. It has been speculated that the brew antagonizes vitamin B6, and one study did find B6 declines in coffee drinkers (vitamin B6 participates in a mechanism that detoxifies homocysteine). Decaf doesn’t seem to affect homocysteine, and tea doesn’t either. Certain types of coffee, or ways of preparing it, apparently do. Cholesterol will elevate along with homocysteine, but only if the coffee is unfiltered. Filtering eliminates diterpenes, the parties responsible. Organic coffee has never been tested.
Depression
People with depression have changes in the biochemistry of their brain. The most well-studied changes relate to neurotransmitters known as serotonin, dopamine and noradrenaline. These neurotransmitters influence mood, and they’re the targets of tricyclic antidepressants.
Mood enhancers are created in the brain in a process that involves methylation. Since methylation is part of the cycle that creates homocysteine, researchers have reasoned that it’s likely these neurotransmitters are affected by homocysteine.
In the first of its kind, a new study shows that homocysteine, depression, neurotransmitters and folate are connected. A clear association exists between elevated homocysteine and major depression. It also shows that depressed people with the highest elevations in homocysteine (>12 micromoles/liter) have significantly less SAMe—which means they have less capacity to create mood-enhancing neurotransmitters. Low levels of neurotransmitters were, in fact, confirmed in the people with the highest homocysteine and lowest levels of SAMe. In the whole group, higher homocysteine equalled lower SAMe. A clear association exists between elevated homocysteine and major depression.
Since folate deficiency is one of the main reasons for elevated homocysteine, the researchers also looked at folate levels, both in the blood and in cerebral spinal fluid. They found that the group with the highest homocysteine levels (>12 µmol/l) had significantly lower folate in cerebral spinal fluid, red cells and serum. Folate was also lower in red blood cells of the depressed group as a whole. Nearly a third of the depressed inpatients in the study had red cell folate levels below normal (<150 µg/l). At the same time, half of them had homocysteine levels higher than the levels of two control groups.
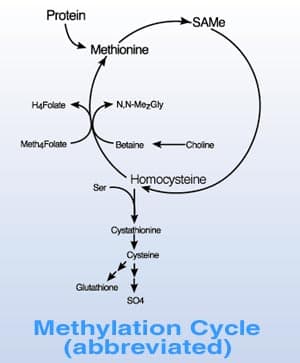
Homocysteine, SAMe and folate all link up in the methylation cycle where methionine is converted to SAMe, used for methylation, leaving homocysteine which is then converted back to methionine with enzymes that use folate. One depends on the other. If folate is not available to promote the conversion of homocysteine, it can build up and block methylation.
Serotonin and other brain chemicals require methylation to be synthesized. When methylation factor, SAMe, is injected into rats, certain areas of the brain synthesize more serotonin. In turn, serotonin and SAMe both are necessary for the synthesis of melatonin, an important hormone for sleep. It’s easy to see how homocysteine (which blocks SAMe) can have far-reaching effects.
People with folate deficiency have decreased synthesis of serotonin and dopamine. It has been reported that people with folate deficiencies do not respond to Prozac as well as people who have sufficient folate. Folate deficiency alone can cause severe depression, as can vitamin B12 deficiency (note: the usual methods of measuring these two vitamins in people is not very accurate, plus because they work together, it’s sometimes hard to tell which vitamin is deficient).
What you can do
There are three principle vitamins involved in the conversion of homocysteine: folate, vitamins B6 and B12. Vitamin B2 (riboflavin) is required for the B6 pathway of homocysteine reduction.
Folate adequately lowers homocysteine in some people. Published studies show that folate supplements (0.5-5 mg/day) reduce homocysteine anywhere from 12% to 30%. In a recent study on cervical dysplasia, women were given 10 mg of folic acid a day, whether they were deficient or not. Homocysteine was significantly reduced at eight weeks, with a continuing trend downwards at six months.
Folate is one answer to homocysteine, but it’s not the only answer. Other vitamins help too. Vitamin B12 must be available for folate to work, and vitamin B6 must be present for homocysteine to be converted to cysteine and other beneficial sulfur-type molecules.
Another pathway for the detoxification of homocysteine utilizes betaine (TMG) and requires no vitamin cofactors. Betaine can be taken in conjunction with folate if folate doesn’t reduce homocysteine to a satisfactory level. (Relying on betaine alone, however, is not advisable since folate has numerous important functions in addition to reducing homocysteine.
Diet and homocysteine
Diet can have a major impact on homocysteine. Homocysteine derives from methionine which is more abundant in animal protein than plant protein. Folate is found mostly in vegetables and legumes. This would suggest that people on vegetarian diets would have higher folate and lower homocysteine. This is in fact the case. One recent study shows that a supervised vegan diet (no animal products whatsoever, and excluding tobacco, alcohol and caffeine) lowers homocysteine 13% in one week without supplements.
However, there is a caveat about vegetarianism. A seperate study on unsupervised vegetarians shows that vegetarians can have elevated
homocysteine if they don’t take supplemental vitamin B12. B12 is found abundantly in animal products, and rarely in plants. The only known non-animal sources of B12 are fermented foods (such as tempeh), seaweed and supplements. Ovolacto vegetarians (vegetarians who eat eggs and dairy products) can obtain B12 through those animal products.Vegetarians beware. You are frequently B12 deficient according to published studies. This recent study on homocysteine demonstrates how important the vitamin is for lowering homocysteine—something that doesn’t show up in most studies where the participants are usually meat-eaters. (Despite this, studies show that vegatarians have a significantly reduced risk of heart attack).
Several large studies have looked at whether adding or subtracting things from the typical American meat-based diet can lower homocysteine. At Johns Hopkins, researchers put 118 people, average age 49, on three different diets. The first was a diet typical of what Americans eat: red meat, high-fat, low in fruits, vegetables and whole grains, with not too many dairy products, no nuts, seeds or legumes (control diet). The second diet (fruits and vegetables) was a typical American diet with added fruits and vegetables. It had more beef, pork and ham, less poultry, less dairy, but more nuts, seeds, legumes and vegetables than the control diet. It also had a lot more fruit. The third diet (combination) was built around low-fat dairy products, fruits and vegetables (somewhat similar to a vegetarian diet). It had the most vegetables and the least beef, pork and ham. It had more fish and dry cereals than the other two diets.
After eight weeks on the diets (11 weeks for the control), homocysteine levels went up in the control and fruits-and-vegetables diets, and down in the combination (vegetarian-like) diet. The researchers estimate that the homocysteine-lowering effect of the vegetarian-like diet reduced the risk of heart disease by 7-9% after eight weeks. It’s important to note that the combination diet increased serum folate and B12 more than the other diets. Of vitamins B12, B6 and folate, folate was the only vitamin of three that correlated with reduced homocysteine in the study.
Homocysteine is a danger signal that should not be ignored. In addition to heart disease, eye conditions, depression and other diseases mentioned above, elevated homocysteine occurs in diabetes, lupus and renol disease. People with the highest homocysteine have the most complications from these diseases.
Age is another factor that elevates homocysteine. Unfortunately, age-related hyperhomocysteinemia hasn’t been adequately investigated. However, the data on the dangers of homocysteine is already so compelling that researchers are now urging doctors to do routine testing.
Note: For additional information on what can be done to lower homocysteine levels when folic acid supplements fail, refer to the March 1999 issue of Life Extension (“A Lethal Misconception”) or refer to the Internet magazine archives section at www.lifeextension.com.
References
Appel LJ, et al. 2000. Effect of dietary patterns on serum homocysteine: results of a randomized, controlled feeding study. Circulation 102:852-57.
Aronow WS, et al. 2000. Increased plasma homocysteine is an independent predictor of new atherothrombotic brain infarction in older persons. Am J Cardiol 86:585-6, A10.
Aronow WS, et al. 2000. Increased plasma homocysteine is an independent predictor of new coronary events in older persons. Am J Cardiol 86:346-7.
Austin RC, et al. 1998. Homocysteine-dependent alterations in mitochondrial gene expression, function and structure. Homocysteine and H2O2 act synergistically to enhance mitochondrial damage. J Biol Chem 273(46):30808-17.
Botez MI, et al. 1982. Effect of folic acid and vitamin B12 deficiencies on 5-hydroxyindoleacetic acid in human cerebrospinal fluid. Ann Neurol 12:479-84.
Chambers JC, et al. 1999. Demonstration of rapid onset vascular endothelial dysfunction after hyperhomocysteinemia: an effect reversible with vitamin C therapy. Circulation 99:1156-60.
Chao CL, et al. 2000. Effects of methiionine-induced hyperhomocysteinemia on endothelium-dependent vasodilation and oxidative status in healthy adults. Circulation 101:485-90.
DeRose DJ, et al. 2000. Vegan diet-based lifestyle program rapidly lowers homocysteine levels. Prev Med 30:225-33.
Fava M, et al. 1997. Folate, vitamin B12 and homocysteine in major depressive disorder. Am J Psychiatry 154:426-8.
Grubben MJ, et al. 2000. Unfiltered coffee increases plasma homocystene concentrations in healthy volunteers: a randomized trial. Am J Clin Nutr 71:480-4.
Hirano K, et al. 1994. Homocysteine induces iron-catalyzed lipid peroxidation of low-density lipoprotein that is prevented by alpha-tocopherol. Free Radic Res 21:267-76.
Kanani PM, et al. 1999. Role of oxidant stress in endothelial dysfunction produced by experimental hyperhomocyst(e)inemia in humans. Circulation 100:1161-8.
Key TJ, et al. 1996. Dietary habits and mortalityin 11,000 vegetarians and health conscious people: results of a 17 year follow up. BMJ 313:775-9.
Khajuria A, et al. 2000. Induction of monocyte tissue factor expression by homocysteine: a possible mechanism for thrombosis. Blood 96:966-72.
Khan MA, et al. 1999. The interaction of homocysteine and copper makedly inhibits the relaxation of rabbit ocrpus cavernosum: new risk factors for angiopathic erectile dysfunction? BJU Int 84:720-4.
Ling Q, et al. 2000. Inhibition of endothelial cell thromboresistance by homocysteine. J Nutr 130(2S Suppl):373S-76S.
Mann NJ, et al. 1999. The effect of diet on plasma homocysteine concentrations in healthy male subjects. Eur J Clin Nutr 53:895-9.
Nygärd O, et al. 1998. Major lifestyle determinants of plasma total homocysteine distribution: the Hordaland Homocysteine Study. Am J Clin Nutr 67:263-70.
Omland T, et al. 2000. Serum homocysteine concentration as an indicator of survival in patients with acute coronary syndromes. Arch Intern Med 160:1834-40.
Otero-Losada ME, et al. 1989. Acute changes in 5-HT metabolism after S-adenosyl-L-methionine administration. Gen Pharmacol 20:403-6.
Pianka P, et al. 2000. Hyperhomocystinemia in patients with nonarteritic anterior ischemic optic neuropathy, central retinal artery occlusion, and central retinal vein occlusion. Ophthalmology 107:1588-92.
Rwei-Fen SH, et al. 2001. Folate depletion and elevated plasma homocysteine promote oxidative stress in rat livers. J Nutr 131:33-38.
Stolzenberg-Solomon, RZ, et al. 1999. Association of dietary protein intake and coffee consumption with serum homocysteine concentrations in an older population. Am J Clin Nutr 69:467-75.
Surtees R, et al. 1994. Association of cerebrospinal fluid deficiency of 5-methyltetrahydrofolate, but not S-adenosylmethionine, with reduced concentrations of the acid metabolites of 5-hydroxytryptamine and dopamine. Clin Sci (Colch) 86:697-702.
Thomson SW, et al. 2000. Correlates of total plasma homocysteine: folic acid, copper, and cervical dysplasia. Nutrition 16:411-16.
Vine AK. 2000. Hyperhomocysteinemia: a risk factor for central retinal vein occlusion. Am J Ophthalmol 129:640-4.
