Life Extension Magazine®
Acetyl-L-Carnitine Reduces Oxidative Damage in Brains | |
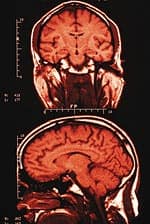
Acetyl-L-carnitine decreases oxidative stress in aging brains, according to researchers at the University of California, Berkeley.* L-carnitine plays an essential role in energy production by transporting fatty acids into the mitochondrial matrix for oxidation. Both L-carnitine and its metabolite, acetyl-L-carnitine, have been reported to improve mitochondrial function. The California research-ers compared the effects of equal doses of L-carnitine and acetyl-L-carnitine on brain and plasma levels of carnitine, movement activity, and markers of oxidative stress in rats. Aged rats were supplemented with either L-carnitine or its activated form, acetyl-L-carnitine, for four weeks. Plasma and brain levels of L-carnitine and acetyl- L-carnitine were then measured. Ambulatory activity of the rats was assessed, as were markers of oxidative damage in the brain tissue. Both L-carnitine and acetyl-L-carnitine supplementation raised circulating and brain levels of carnitine. Both forms were also effective in improving ambulatory activity in the aged rats. When measures of oxidative stress in the brain were examined, however, acetyl-L-carnitine was found to decrease oxidative damage, while L-carnitine was not effective. Since tissue levels of L-carnitine decline with age, supplementing with either L-carnitine or acetyl-L-carnitine may be beneficial for adults. Both forms boost plasma and brain levels of carnitine, while increasing ambulatory activity. For protecting brain health, however, only acetyl-L-carnitine appears to offer neuroprotection from oxidative stress. This finding may have important applications for the prevention and management of neurodegenerative disorders. —Linda M. Smith, RN | |
| Reference | |
| Liu J, Head E, Kuratsune H, Cotman CW, Ames BN. Comparison of the effects of L-carnitine and acetyl-L-carnitine on carnitine levels, ambulatory activity, and oxidative stress biomarkers in the brain of old rats. Ann NY Acad Sci. 2004 Nov;1033:117-31. | |
Fish Oil Improves Cognition in Older Adults | |
| Omega-3 fatty acids from fish oil supplements are associated with improved cognitive function in later life, report scientists at the University of Aberdeen in the United Kingdom.* Cognitive decline commonly occurs with advancing age. Although no single cause of this decline has been determined, risk factors include age, genetics, elevated cholesterol levels, and high blood pressure. Severe cognitive impairment and Alzheimer’s disease-related dementia currently affect 4.5 million elderly adults in the US, and it is conservatively estimated that 15 million US adults will be affected by the year 2050. The well-designed United King-dom study examined 350 men and women. The subjects had been IQ-tested at the age of 11, and now, at the age of 64, they were given a battery of tests to assess diverse cognitive functions. In addition, the subjects completed a food questionnaire designed to quantify their use of fish oil and other supplements. Omega-3 fatty acid content of red blood cell membranes was also assessed. The fish oil supplement users performed significantly better than non-users on measures of cognitive function, and demonstrated higher omega-3 fatty acid levels in red blood cell membranes. The subjects who used fish oil supplements also consumed more vitamin C and more vegetable and cereal fiber than did the participants who did not use supplements. The authors concluded that fish oil supplement use and red blood cell membrane omega-3 content are associated with improved cognitive aging. Optimizing omega-3 fatty acid intake may thus help to maintain cognitive function with increasing age. —Linda M. Smith, RN | |
| Reference | |
| Whalley LJ, Fox HC, Wahle KW, Starr JM, Deary IJ. Cognitive aging, childhood intelligence, and the use of food supplements: possible involvement of n-3 fatty acids. Am J Clin Nutr. 2004 Dec;80(6):1650-7. | |
CoQ10 Counters Harmful Side Effect of Statins | |
| An adverse effect on cardiac function caused by a cholesterol-lowering medication can be reversed with coenzyme Q10 (CoQ10) supplementation, conclude researchers in Illinois and Texas.* Individuals using the statin drug atorava-statin (Lipitor®) experienced dysfunctional left ventricular diastolic function that was improved using supplemental CoQ10. Statin drugs are widely prescribed to lower cholesterol and decrease the risk of fatal and nonfatal cardiovascular events. While statins are well tolerated by many users, among their potentially lethal complications is muscle injury, including injury to cardiac muscle. Statin drugs decrease the production of both cholesterol and CoQ10, an essential cofactor required for energy production throughout the body and indispensable for normal cardiac function. Some researchers have suggested that a drop in CoQ10 level alone could provoke cardiac dysfunction. The study enrolled 14 patients, all of whom had abnormal cholesterol profiles and were not taking statin drugs. Cholesterol and CoQ10 levels were measured, and a two-dimensional echocardiogram was performed on each participant, at the study’s onset. After beginning statin therapy with atorvastatin, laboratory tests and echocardiogram were repeated at three to six months later. At follow-up, 10 of the 14 patients exhibited impairment of left-sided heart activity. All participants were then offered CoQ10 supplementation with continued statin therapy. As early as three months later, all but one patient demonstrated a reversal of the cardiac abnormality. While statin therapy may be indicated for some individuals with abnormal cholesterol profiles, this and other studies indicate that supplemental CoQ10 may help preserve cardiac function during prescription drug therapy. —Linda M. Smith, RN | |
| Reference | |
| Silver MA, Langsjoen PH, Szabo S, Patil H, Zelinger A. Effect of atorvastatin on left ventricular diastolic function and ability of coenzyme Q10 to reverse that dysfunction. Am J Cardiol. 2004 Nov 15;94(10):1306-10. |