Life Extension Magazine®
Popular multivitamin supplements still don’t provide enough vitamin D to yield optimal health benefits. Most commercial multivitamins contain 400 to 600 IU of vitamin D, a potency that provides little real-world benefit.
With evidence showing reduced mortality in those with higher vitamin D blood levels, an urgent need exists to alert the public about the importance of taking the proper dose of this low-cost vitamin. Failure to properly supplement contributes to a host of premature illnesses along with increased national health care costs.
Compelling research has demonstrated that vitamin D blood levels in the range of 50 to 80 ng/mL are associated with reduced mortality and a lower risk of common diseases.1,2
A considerable volume of published literature documents a connection of insufficient or deficient 25-hydroxyvitamin D blood levels3 with higher risks of cancer,4-6 vascular disease,7-10 and chronic inflammation.11-13
Low vitamin D status has long been associated with loss of bone density. This limited view of vitamin D’s biological effects is still taught in many medical textbooks, leading some doctors to view vitamin D only for its value in reducing osteoporosis risk.
Yet vitamin D has clinical applications for a vast array of health conditions. This article reviews some recent findings that reveal an even wider range of protective benefits conferred by this readily available dietary supplement.
Reduced Mortality in Hospital Patients
Some of the most impressive research discovered on vitamin D has been on ICU (intensive care unit) patients. The New England Journal of Medicine first reported in 2009 a striking 45% mortality (death) rate in vitamin D-deficient ICU patients compared to only a 16% mortality rate in sufficient vitamin D patients. This study showed that vitamin D deficiency results in almost 3-times more patients dying in the ICU.14
Vitamin D deficiency is an all-cause mortality risk factor and since the publication of this study in 2009, there has been even more data released to substantiate this claim.15-17
A fascinating study reported in 2015 showed very similar results to the aforementioned study. This study entailing 135 ICU patients revealed a 32.2% risk of mortality when vitamin D levels were below 12 ng/mL compared to a 13.2% risk of mortality if levels were greater. This finding shows that vitamin D deficient patients die at a 2.4-fold greater rate.18
Not all studies of seriously ill patients in the intensive care units (ICU) show lifesaving effects of vitamin D. Giving ICU patients large doses of vitamin D has not consistently reversed their life-threatening conditions.19 This indicates that to benefit from the life-protective effects of vitamin D, higher blood levels should be maintained on a constant basis. Overall, patients armed with higher levels of vitamin D before they enter ICU show better clinical outcomes than those who do not.20-22
Post Stroke Functional Outcome

Stroke is the leading cause of serious long-term disability. An estimated 6.8 million Americans (2.8% of the entire adult population) are living after having had a stroke.23,24
When a stroke occurs, 40% of its victims experience moderate to severe debilitation requiring special care, and 15% die shortly thereafter.25
Vitamin D deficiency is pervasive among stroke victims, and those with the lowest levels of vitamin D have been shown to have the poorest functional outcomes. In fact, a recent study showed that for each 10 ng/mL decrement in vitamin D, the odds of a poor 90-day post stroke functional outcome doubled.26,27
To put this in perspective, those who don’t supplement with high doses of vitamin D typically have 25-hydroxyvitamin D levels under 20 ng/mL. Those who properly supplement should strive to obtain levels of 25-hydroxyvitamin D over 50-80 ng/mL. Based on this study’s findings, people with these higher vitamin D levels would be far more likely to avoid permanent institutional confinement if they suffered an ischemic stroke.
Another recent study involving 818 stroke patients showed very similar results. Those with an adequate vitamin D level of 30 ng/mL or above showed a 90% better improvement in functional outcomes compared to those who were severely deficient (<10 ng/mL ).28
Experts believe that in order to prevent many of the age-related diseases, people should maintain a vitamin D blood level between 50 to 80 ng/mL.1,2
These stroke studies are showing robust improvement in functional outcome with just a sufficient vitamin D blood level. Based on the number of studies showing vascular protective benefits of vitamin D, those who maintain optimal vitamin D levels, along with comprehensive blood testing to correct other risk factors, will likely decrease their stroke risk and reduce the odds of permanent disability in the event one of their cerebral arteries becomes occluded (ischemic stroke).29
Support for Diabetics
Beta cells are insulin-producing cells in the pancreas. When the beta cells die, people become insulin-dependent diabetics. Without insulin, there is nothing to deliver glucose into cells for energy production. This leads to high circulating glucose blood levels that contribute to a long list of deadly disorders that include heart disease,30 Alzheimer’s,31 and cancer.32
Vitamin D has been documented to prevent high glucose-induced beta cell apoptosis (death). This is because beta cells contain active receptors for vitamin D, just like every other cell in the body.33-35
What You Need to Know
 |
Why Supplementing with Vitamin D Is Vital to Good Health
- Most doctors still associate vitamin D with bone loss and osteoporosis, but numerous studies reveal vitamin D blood levels in the range of 50 to 80 ng/mL are associated with reduced mortality and a lower risk of common diseases.
- Further research documents a connection of insufficient or deficient vitamin D with sharply higher risks of cancer, vascular disease, and chronic inflammation.
- The New England Journal of Medicine first reported in 2009 a striking 45% mortality rate in vitamin D-deficient ICU patients compared to only a 16% mortality rate in sufficient vitamin D patients.
- Vitamin D deficiency is also linked to stroke. Studies show that those with optimal vitamin D levels decrease their stroke risk and reduce the odds of permanent disability in the event of a stroke.
- Lower vitamin D levels are associated with an increased risk for the autoimmune disease MS, and more than 90% of people with MS have deficient vitamin D levels. Low levels are also linked with psychiatric disorders, such as ADHD and schizophrenia.
A Link between Vitamin D and Multiple Sclerosis
It is well known that there are higher rates of vitamin D deficiency in colder climates of the world due to the lack of sun. This has caused a greater chance of having an immune system-related illness.
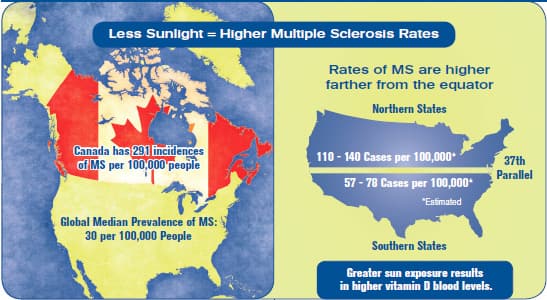
Multiple sclerosis (MS) is an autoimmune disease caused when the body’s own T lymphocytes, B lymphocytes, and macrophages attack the myelin sheath of neurons.36 Those living in the northern part of the United States are twice as likely to develop multiple sclerosis, and those in Canada have a 5-times greater risk compared to people residing in the southern US. This geographical data, along with a multitude of studies that explain the mechanisms and causation, has led many researchers to believe that MS is heavily influenced by vitamin D deficiency.37
A study published by PLOS Medicine identified single nucleotide polymorphisms that were strongly associated with lower 25-hydroxyvitamin D levels.38 The researchers studied the odds of MS on those with genetically lower vitamin D levels from the International Multiple Sclerosis Consortium study. Considered the largest genetic association study to date for MS, it included 14,498 subjects with MS and 24,091 healthy controls. The authors concluded that genetically lowered vitamin D levels were strongly associated with an increased risk for MS.38
This new data heavily reinforces the statistics and research on vitamin D for MS. Trials show that more than 90% of people with MS have deficient vitamin D.39 Deficient is defined at a level below 20 ng/mL.3
Vitamin D can even mediate the direct effects of the immune cells that attack the myelin sheath, a hallmark pathological mechanism of MS. When these aggressive immune cells were extracted from MS patients and exposed to vitamin D, their division was slowed. This signifies the imposing control vitamin D can have on autoimmune diseases such as MS.40
Vitamin D Lowers Inflammatory Biomarkers
Interleukin-6 (IL-6) is an inflammatory cytokine. At high levels, this cytokine has been linked with several types of cancers.41 Overweight individuals have much higher rates of inflammatory cytokines like interleukin-6.42
A compelling study documented marked reductions of interleukin-6 when vitamin D is combined with weight loss. The study involved 218 overweight postmenopausal women who were divided into two groups. Both groups had weight loss interventions, but one group was given 2,000 IU per day of oral vitamin D3.
Both groups achieved a 5% to 10% weight loss, but the group that received the vitamin D supplement showed an impressive 37.3% reduction in interleukin-6 levels compared to the placebo which only had a 17.2% reduction.43
Psychiatric Disorders
Interesting research is showing higher levels of vitamin D play an important role during pregnancy for preventing many different psychiatric disorders.44,45
The vitamin D receptor emerges in the brain stem through the embryonic development of rats. This indicates and reinforces the idea that vitamin D is important for gestational development.46,47 Additional studies have shown that vitamin D deficiency in the mother can lead to impaired growth of the fetus.48
Attention Deficit Hyperactive Disorder (ADHD)
A fascinating study analyzing vitamin D blood levels in 1,650 mothers showed that for each 10 ng/mL increment in vitamin D levels, their children had 11% less ADHD-like symptoms.45
This type of research has heavily influenced the demand for prenatal vitamins. However, most multivitamins only contain a fraction of the vitamin D that is needed to be therapeutic. The trivial amount of vitamin D in most prenatal vitamins is not enough to raise a vitamin D level by 10 ng/mL.1,2
Schizophrenia
An imbalance of dopamine has been hypothesized to be a cause of schizophrenia.49 The vitamin D receptor emerges in the brain stem at the same time as the peak period of dopamine cell birth in rat embryos.47
There has been a high correlation between vitamin D deficiency and schizophrenia.50,51 The correlation has influenced a study to show if vitamin D deficiency was prevalent in those having an acute episode.52
The study subjects were divided into three groups: 40 patients who were reported to be having an acute episode, 41 patients in remission, and 40 healthy controls.52
Those who reported to be having an onset of schizophrenic episodes had far lower levels of vitamin D compared to schizophrenics in remission. The healthy controls had the highest levels of vitamin D.
Ignored Age-Related Panacea
Life Extension® has been writing about the health benefits of vitamin D for many decades. Fortunately, researchers are finally catching up with these findings and devoting resources to discovering and documenting new applications of vitamin D. What might be surprising is that the new research discussed in this article was released just within this last year.
There is an immense archive of literature documenting the health benefits of this single vitamin. Every day, more research findings are being published. In fact, by the time this article is published, there will be even more noteworthy studies released.
Current medical teachings need to be updated to include evidence that vitamin D provides support to not just bone health, but also to reducing all-cause mortality through its system-wide benefits. Vitamin D is the only vitamin that has receptors for it located on every cell. With the cumulative and consistent evidence backing its efficacy, this vitamin should be an essential part of everyone’s daily health regimen.
The cost of conventional treatment for age-related diseases is staggering and Medicare is on the hook for a huge unfunded liability.53
People today have an unprecedented opportunity to reduce their risk of needing conventional treatment using a low-cost vitamin supplement. The typical dose range is 5,000 to 8,000 IU of vitamin D3 daily taken with a meal for better absorption.
Annual blood tests can enable one to know if they are taking the proper dose of vitamin D they need to achieve optimal levels of 25-hydroxyvitamin D.
Summary
While the use of vitamin D has increased dramatically, levels in common commercial multivitamins (400 to 600 IUs) are still far too low to provide real-world benefits.
Extensive research has demonstrated that higher vitamin D blood levels are associated with reduced mortality risk and specific diseases such as diabetes, stroke, and multiple sclerosis, along with other autoimmune diseases and psychological disorders.
Vitamin D dosing in the range of 5,000 to 8,000 IU each day should be taken with a meal for better absorption.
If you have any questions on the scientific content of this article, please call a Life Extension® Wellness Specialist at 1-866-864-3027.
References
- Available at: https://www.lifeextension.com/magazine/2010/1/startling-findings-about-vitamin-d-levels-in-life-extension-members/page-01. Accessed October 8, 2015.
- Available at: https://www.lifeextension.com/magazine/2012/ss/vitamin-d-blood-levels/page-01. Accessed October 8, 2015.
- Holick MF, Binkley NC, Bischoff-Ferrari HA, et al. Evaluation, treatment, and prevention of vitamin D deficiency: an Endocrine Society clinical practice guideline. J Clin Endocrinol Metab. 2011;96(7):1911-30.
- Wu K, Feskanich D, Fuchs CS, et al. A nested case control study of plasma 25-hydroxyvitamin D concentrations and risk of colorectal cancer. J Natl Cancer Inst. 2007;99(14):1120-9.
- Edlich R, Mason SS, Chase ME, et al. Scientific documentation of the relationship of vitamin D deficiency and the development of cancer. J Environ Pathol Toxicol Oncol. 2009;28(2):133-41.
- Garland CF, Gorham ED, Mohr SB, et al. Vitamin D for cancer prevention: global perspective. Ann Epidemiol. 2009;19(7):468-83.
- Giovannucci E, Liu Y, Hollis BW, et al. 25-hydroxyvitamin D and risk of myocardial infarction in men: a prospective study. Arch Intern Med. 2008;168(11):1174-80.
- Dobnig H, Pilz S, Scharnagl H, et al. Independent association of low serum 25-hydroxyvitamin d and 1,25-dihydroxyvitamin d levels with all-cause and cardiovascular mortality. Arch Intern Med. 2008;168(12):1340-9.
- Szabo B, Merkely B, Takacs I. The role of vitamin D in the development of cardiac failure. Orv Hetil. 2009;150(30):1397-402.
- Gouni-Berthold I, Krone W, Berthold HK. Vitamin D and cardiovascular disease. Curr Vasc Pharmacol. 2009;7(3):414-22.
- Suzuki Y, Ichiyama T, Ohsaki A, et al. Anti-inflammatory effect of 1alpha,25-dihydroxyvitamin D(3) in human coronary arterial endothelial cells: Implication for the treatment of Kawasaki disease. J Steroid Biochem Mol Biol. 2009;113(1-2):134-8.
- Dietrich T, Nunn M, Dawson-Hughes B, et al. Association between serum concentrations of 25-hydroxyvitamin D and gingival inflammation. Am J Clin Nutr. 2005;82(3):575-80.
- Xia JB, Wang CZ, Ma JX, et al. Immunoregulatory role of 1, 25-dihydroxyvitamin D(3)-treated dendritic cells in allergic airway inflammation. Zhonghua Yi Xue Za Zhi. 2009;89(8):514-8.
- Lee P, Eisman JA, Center JR. Vitamin D deficiency in critically ill patients. New Engl J Med. 2009;360(18):1912-4.
- Williams S, Heuberger R. Outcomes of vitamin D supplementation in adults who are deficient and critically ill: A Review of the Literature. Am J Ther. 2015.
- Vogt S, Decke S, de Las Heras Gala T, et al. Prospective association of vitamin D with frailty status and all-cause mortality in older adults: Results from the KORA-Age Study. Prev Med. 2015;73:40-6.
- Lo Gullo A, Mandraffino G, Bagnato G, et al. Vitamin D Status in Rheumatoid Arthritis: Inflammation, Arterial Stiffness and Circulating Progenitor Cell Number. PLoS One. 2015;10(8):e0134602.
- Moraes RB, Friedman G, Wawrzeniak IC, et al. Vitamin D deficiency is independently associated with mortality among critically ill patients. Clinics (Sao Paulo). 2015;70(5):326-32.
- Dickerson RN, Berry SC, Ziebarth JD, et al. Dose-response effect of ergocalciferol therapy on serum 25-hydroxyvitamin D concentration during critical illness. Nutrition. 2015;31(10):1219-23.
- Brook K, Camargo CA, Christopher KB, et al. Admission vitamin D status is associated with discharge destination in critically ill surgical patients. Ann Intensive Care. 2015;5(1):23.
- Higgins DM, Wischmeyer PE, Queensland KM, et al. Relationship of vitamin D deficiency to clinical outcomes in critically ill patients. JPEN J Parenter Enteral Nutr. 2012;36(6):713-20.
- Zajic P, Amrein K. Vitamin D deficiency in the ICU: a systematic review. Minerva Endocrinol. 2014;39(4):275-87.
- Available at: http://www.cdc.gov/stroke/facts.htm. Accessed October 8, 2015.
- Available at: http://www.uhnj.org/stroke/stats.htm. Accessed October 8, 2015.
- Available at: http://www.ninds.nih.gov/disorders/stroke/stroke_rehabilitation.htm. Accessed October 8, 2015.
- Available at: http://consumer.healthday.com/cardiovascular-health-information-20/misc-stroke-related-heart-news-360/low-vitamin-d-levels-in-stroke-survivors-a-bad-sign-study-finds-696093.html. Accessed October 8, 2015.
- Turetsky A, Goddeau RP, Jr., Henninger N. Low serum vitamin D is independently associated with larger lesion volumes afterischemic stroke. J Stroke Cerebrovasc Dis. 2015;24(7):1555-63.
- Park KY, Chung PW, Kim YB, et al. Serum vitamin D status as a predictor of prognosis in patients withacute ischemic stroke. Cerebrovasc Dis. 2015;40(1-2):73-80.
- Majumdar V, Prabhakar P, Kulkarni GB, et al. Vitamin D status, hypertension and ischemic stroke: a clinical perspective. J Hum Hypertens. 2015;29(11):669-74.
- Hartog JW, Voors AA, Schalkwijk CG, et al. Clinical and prognostic value of advanced glycation end-products in chronic heart failure. Eur Heart J. 2007;28(23):2879-85.
- Xu W, Qiu C, Winblad B, et al. The effect of borderline diabetes on the risk of dementia and Alzheimer’s disease. Diabetes. 2007;56(1):211-6.
- Noto H, Osame K, Sasazuki T, et al. Substantially increased risk of cancer in patients with diabetes mellitus: a systematic review and meta-analysis of epidemiologic evidence in Japan. J Diabetes Complications. 2010;24(5):345-53.
- Talaei A, Mohamadi M, Adgi Z. The effect of vitamin D on insulin resistance in patients with type 2 diabetes. Diabetol Metab Syndr. 2013;5(1):8.
- Oh YS, Jun HS. Role of bioactive food components in diabetes prevention: effects on Beta-cell function and preservation. Nutr Metab Insights. 2014;7:51-9.
- Yang Z, Liu F, Qu H, et al. 1, 25(OH)2D3 protects beta cell against high glucose-induced apoptosis through mTOR suppressing. Mol Cell Endocrinol. 2015;414:111-9.
- Noseworthy JH, Lucchinetti C, Rodriguez M, et al. Multiple sclerosis. N Engl J Med. 2000;343(13):938-52.
- Available at: http://www.healthline.com/health/multiple-sclerosis/facts-statistics-infographic. Accessed October 13, 2015.
- Mokry LE, Ross S, Ahmad OS, et al. Vitamin D and risk of multiple sclerosis: a mendelian randomization study. PLoS Med. 2015;12(8):e1001866.
- Available at: https://clinicaltrials.gov/ct2/show/study/NCT01285401?term=NCT01285401&rank=1. Accessed October 13, 2015.
- Correale J, Ysrraelit MC, Gaitan MI. Immunomodulatory effects of vitamin D in multiple sclerosis. Brain. 2009;132(Pt 5):1146-60.
- Guo Y, Xu F, Lu T, et al. Interleukin-6 signaling pathway in targeted therapy for cancer. Cancer Treat Rev. 2012;38(7):904-10.
- Eder K, Baffy N, Falus A, et al. The major inflammatory mediator interleukin-6 and obesity. Inflamm Res. 2009;58(11):727-36.
- Duggan C, de Dieu Tapsoba J, Mason C, et al. Effect of vitamin D3 supplementation in combination with weight loss on inflammatory biomarkers in postmenopausal women: a randomized controlled trial. Cancer Prev Res (Phila). 2015;8(7):628-35.
- McGrath J. Does ‘imprinting’ with low prenatal vitamin D contribute to the risk of various adult disorders? Med Hypotheses. 2001;56(3):367-71.
- Morales E, Julvez J, Torrent M, et al. Vitamin D in pregnancy and attention deficit hyperactivity disorder-like symptoms in childhood. Epidemiology. 2015;26(4):458-65.
- Hawes JE, Tesic D, Whitehouse AJ, et al. Maternal vitamin D deficiency alters fetal brain development in the BALB/c mouse. Behav Brain Res. 2015;286:192-200.
- Cui X, Pertile R, Liu P, et al. Vitamin D regulates tyrosine hydroxylase expression: N-cadherin a possible mediator. Neuroscience. 2015;304:90-100.
- Brunvand L, Quigstad E, Urdal P, et al. Vitamin D deficiency and fetal growth. Early Hum Dev. 1996;45(1-2):27-33.
- Kesby JP, Cui X, Burne TH, et al. Altered dopamine ontogeny in the developmentally vitamin D deficient rat and its relevance to schizophrenia. Front Cell Neurosci. 2013;7:111.
- Valipour G, Saneei P, Esmaillzadeh A. Serum vitamin D levels in relation to schizophrenia: a systematic review and meta-analysis of observational studies. J Clin Endocrinol Metab. 2014;99(10):3863-72.
- Shivakumar V, Kalmady SV, Amaresha AC, et al. Serum vitamin D and hippocampal gray matter volume in schizophrenia. Psychiatry Res. 2015;233(2):175-9.
- Yuksel RN, Altunsoy N, Tikir B, et al. Correlation between total vitamin D levels and psychotic psychopathology in patients with schizophrenia: therapeutic implications for add-on vitamin D augmentation. Ther Adv Psychopharmacol. 2014;4(6):268-75.
- Available at: https://www.washingtonpost.com/blogs/fact-checker/wp/2013/10/23/does-the-united-states-have-128-trillion-in-unfunded-liabilities. Accessed October 13, 2015.

