Life Extension Magazine®
You slip and take what seems like a minor tumble—and feel pain and possibly hear a crack.
For adults over age 50, it’s a shockingly common occurrence, and often the first sign they have the bone disease osteoporosis.1
About 50% of American women and 25% of American men over 50 will break a bone due to osteoporosis.1
Fractures are a leading cause of disability in older adults.
Within a year of suffering a hip fracture, more than 20% of patients may die.2,3
For decades, physicians in Japan have used high doses of vitamin K2 to prevent bone loss and protect against fractures.4
Vitamin K2 is available in the U.S. at the same doses—without a prescription.
Clinical trials show that 45 mg (45,000 mcg) of vitamin K2 helps to:5-10
- Slow bone loss,
- Reduce fracture risk, and
- Build new bone.
A study of older osteoporosis patients showed that high-dose vitamin K2 cut the number of new vertebral fractures by more than half.10
Other nutrients taken with vitamin K2, such as vitamin D and calcium, provide further support for skeletal health.
Osteoporosis Increases Mortality Risk
The impact of osteoporosis-related bone fractures is staggering. After suffering one fracture, the risk of future fractures increases by a whopping 86%.2
Fractures of the hip and vertebra, in particular, are associated with loss of mobility and risk of death. People who suffer a vertebral fracture have an eight-fold increase in mortality compared to other individuals their age.2
But almost any kind of broken bone increases the risk of death in older people.11 That’s why it is imperative not just to slow, but to reverse bone loss as soon as it begins.
Creeping Bone Loss
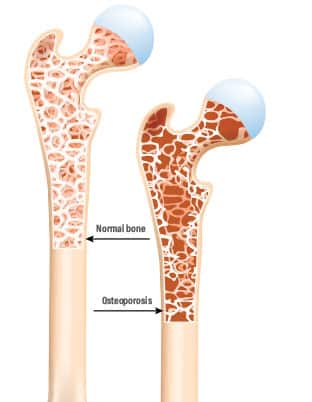
When we’re young, our bones are tightly packed with calcium and other minerals in an intricate structure that looks like a honeycomb.1
Even before age 40, bone density starts to decrease.12 This decline continues into old age. In women, the speed of bone loss accelerates with the onset of menopause.
This drop in bone-mineral density causes bones to become weak, brittle, and prone to fractures. Bone breaks may result from minor injuries. Stress fractures may even occur during normal movement.
The early stage of weakening bones is called osteopenia. As bone density continues to fall, osteoporosis develops. Osteoporosis means “bone full of pores or holes.”
Suffering a fracture, especially if it occurs during normal movement, is when many people first discover they have osteoporosis.
The good news is that we can do something to prevent age-related bone loss and risk of fractures.
High-Dose Vitamin K2
In low doses, vitamin K promotes normal blood clotting. This small amount of vitamin K is normally obtained from dietary sources.
But as far back as 1999, scientists at Life Extension recognized that higher doses of vitamin K could better keep calcium in bones and help prevent calcification of soft tissues such as heart values, arteries, and brain cells.
It’s important to understand that high doses of vitamin K do not cause greater coagulation.
Japanese doctors have long been treating osteoporosis by prescribing a specific form of vitamin K2 called menaquinone-4 (or MK-4), without any clotting issues.7
In high doses of 45,000 mcg or 45 mg, they have found that vitamin K2 safely improves bone health and helps prevent fractures in older adults.5,6,8-10
Boosting Bone Density
To study vitamin K2 under the most challenging circumstances, scientists tested high doses on older people who had already developed osteoporosis.
In one study, Japanese researchers randomized older osteoporosis patients into two groups. One received 150 mg a day of calcium alone. The other received the same calcium dose plus 45 mg of vitamin K2 (as MK-4) daily.10
Over a two-year period:10
- Patients who received only calcium continued to lose bone density in their lumbar spine, which dropped by about 3%.
- Patients also receiving 45 mg of vitamin K2 plus 150 mg of calcium maintained their bone mineral density.
That’s a life-saving difference.
A 10% drop in bone density more than doubles the risk for fractures of the vertebra and hip.13
Patients in this study treated with calcium-only had an increased risk of fracture.
Adding vitamin K2 largely arrested bone loss, reducing fracture risk.10
What you need to know
Build Stronger Bones with Vitamin K2
- Age-related bone loss can lead to osteoporosis and fractures, significantly increasing risk of disability in people over 50.
- High-dose vitamin K2 (in the form of MK-4) has been used as a prescription treatment for osteoporosis in Japan for decades. These doses are available in the U.S. without a prescription.
- Vitamin K2 improves bone health by restoring balance to the process of bone breakdown and formation, favoring new bone growth.
- Human trials show that daily intake of 45 mg of vitamin K2 maintains or increases bone density while reducing fracture risk. In a two-year study on older adults with osteoporosis, it cut the number of new vertebral fractures by more than half.
- Other nutrients, including calcium and vitamin D, support bone health by other mechanisms and can be taken with vitamin K2.
Preventing Fractures
The same study also assessed the effect of high-dose vitamin K2 on the incidence of bone fractures.
During the two-year study, the group receiving calcium alone sustained 35 fractures, compared to only 14 fractures in the vitamin K2 group.10 And these study subjects were not treated with other critical bone supporting nutrients like magnesium, boron, and vitamin D.
In another clinical trial on postmenopausal women with osteoporosis, taking 45 mg of oral vitamin K2 daily:6
- Maintained mineral density to a significantly greater degree than in control women, and
- Reduced the incidence of vertebral fractures to a degree similar to the drug etidronate.
Bisphosphonate drugs like risedronate (Actonel®) and alendronate (Fosamax®) are medications commonly used to treat osteoporosis.14
These medications are associated with various, though rare, side effects. These include osteonecrosis of the jaw, low blood calcium, reflux, ulcers, and more.15,16
Vitamin K2, on the other hand, is not associated with significant side effects, even at high doses.
How Vitamin K2 Keeps Bones Strong
Vitamin K2 works by restoring a healthy balance between the two types of bone cells that influence bone density.
Osteoclasts break down old bone, while osteoblasts build new bone. Healthy bone relies on a balance of activity between these two types of skeletal cells.
As we age, osteoclast activity begins to outstrip osteoblast activity. Bone is broken down faster than new bone is built up. Bone density drops and osteopenia and osteoporosis develop.
In preclinical studies, vitamin K2 was shown to promote:17,18
- An increase in bone-building osteoblast activity, and
- A reduction in bone-destroying osteoclast activity.
With this balance restored, more bone is built, less is destroyed, and bone mineral density is maintained or even increased.
Additionally, in order to build bone, osteoblasts need a protein called osteocalcin. This protein binds to calcium, helping osteoblasts turn this mineral into healthy new bone. Vitamin K2 helps convert osteo-calcin into its active form, which is required for its bonebuilding activities.18,19
In the Japanese study of older osteoporosis patients, the group receiving vitamin K2 had a significant increase in levels of active osteocalcin, which may be a mechanism by which the vitamin reduced fracture incidence.10
Vitamin K2 May Enhance Osteoporosis Drugs
Bisphosphonates are drugs prescribed to slow the bone loss of osteoporosis. They include medications such as alendronate (Fosamax®) and risedronate (Actonel®).
Vitamin K2 does not interfere with bisphosphonates and can safely be used at the same time.
Research even suggests that they may have an additive effect, protecting bone density better together than either one does alone.17
Nutrients That Support Vitamin K2
The powerful bone-rebuilding effects of vitamin K2 may be even greater when combined with other nutrients that support strong and healthy bones.
Calcium is the major mineral that forms the hard matrix of bone. Adequate calcium intake substantially decreases the rate at which bone breakdown and mineral loss occur.20,21
Vitamin D helps the body absorb calcium from the gut after a meal and stimulates the production of osteocalcin.19 Research suggests vitamin D also facilitates the transfer of calcium to the bones, which may further support bone strength.22
Magnesium, like calcium, makes up the mineral matrix of bone and is needed to maintain healthy bone density.23 About half of all magnesium in the body is stored in bone.23
Zinc, manganese, silicon, and boron are minerals that play important roles in optimal bone formation and health. Low levels of each of these minerals may contribute to bone loss, and increased intake improves bone health in animal and/or human studies.24
Taken with these nutrients, vitamin K2 can provide powerful protection against bone loss and fractures.
Summary
As our bones become thinner and weaker with age, the risk of life-threatening fractures increases.
High-dose vitamin K2 has successfully and safely been used for decades in Japan to treat the bone disease osteoporosis.
Human trials demonstrate that daily intake of 45 mg of vitamin K2 maintains or increases bone-mineral density and reduces the risk of fractures.
Along with other nutrients crucial for bone health, vitamin K2 can help build stronger, healthier bones.
If you have any questions on the scientific content of this article, please call a Life Extension Wellness Specialist at 1-866-864-3027.
Vitamin K2 May Provide Cardiovascular Benefits
Vitamin K2 promotes new bone growth in part by increasing calcification, the buildup of calcium deposits, in the bone.
In soft tissues, however, calcification can be extremely dangerous. In blood vessels, it contributes to the buildup of atherosclerotic plaque associated with cardiovascular disease.
Research has shown that while vitamin K2 causes beneficial calcification in bones, it prevents harmful calcification in soft tissues, including blood vessels.25,26 This occurs because it activates matrix Gla protein, which inhibits calcification of blood vessels.27
For this reason, vitamin K2 may be protective against cardiovascular disease.26,28
Vitamin K2 has been shown to be safe to use in healthy, older osteoporotic patients not taking oral vitamin K antagonist anticoagulants (e.g. warfarin), without having an adverse impact on clotting.29
Even studies with high doses of vitamin K have demonstrated its safety, without any adverse events.7-9,30
Still, anyone taking warfarin, a powerful anticoagulant, should consult a physician before taking any form of vitamin K.
Warfarin functions by blocking vitamin K activity in the body, which means warfarin users are to avoid vitamin K supplements and foods high in vitamin K. Newer drugs such as Eliquis®, Pradaxa®, and Xarelto® provide anticoagulant effects without the need to restrict vitamin K intake.
Medications That Promote Osteoporosis
Many common drugs can contribute to osteoporosis risk and bone loss, including:
- Cancer-fighting drugs that inhibit sex hormones, such as anti-androgen therapy (which reduces levels of testosterone) and aromatase inhibitors (which reduce estrogen activity).31,32
- Corticosteroids such as prednisone, hydrocortisone, dexamethasone, and many others.33,34
- Warfarin (Coumadin®), which is used to treat blood clots.35,36
- Proton-pump inhibitors such as Nexium®, Prilosec®, and Prevacid®, which are used to decrease stomach acid.37,38
Do not stop taking these drugs unless directed by your doctor. Butpeople taking these medications may want to carefully monitor their bone mineral status.
References
- Available at: https://www.nof.org/patients/what-is-osteoporosis/. Accessed December 3, 2021.
- Available at: https://www.osteoporosis.foundation/facts-statistics/epidemiology-of-osteoporosis-and-fragility-fractures. Accessed December 3, 2021.
- Panula J, Pihlajamaki H, Mattila VM, et al. Mortality and cause of death in hip fracture patients aged 65 or older: a population-based study. BMC Musculoskelet Disord. 2011 May 20;12:105.
- Iwamoto J. Vitamin K(2) therapy for postmenopausal osteoporosis. Nutrients. 2014 May 16;6(5):1971-80.
- Iwamoto J, Takeda T, Ichimura S. Effect of combined administration of vitamin D3 and vitamin K2 on bone mineral density of the lumbar spine in postmenopausal women with osteoporosis. J Orthop Sci. 2000;5(6):546-51.
- Iwamoto J, Takeda T, Ichimura S. Effect of menatetrenone on bone mineral density and incidence of vertebral fractures in postmenopausal women with osteoporosis: a comparison with the effect of etidronate. J Orthop Sci. 2001;6(6):487-92.
- Jiang Y, Zhang ZL, Zhang ZL, et al. Menatetrenone versus alfacalcidol in the treatment of Chinese postmenopausal women with osteoporosis: a multicenter, randomized, double-blinded, double-dummy, positive drug-controlled clinical trial. Clin Interv Aging. 2014;9:121-7.
- Purwosunu Y, Muharram, Rachman IA, et al. Vitamin K2 treatment for postmenopausal osteoporosis in Indonesia. J Obstet Gynaecol Res. 2006 Apr;32(2):230-4.
- Ushiroyama T, Ikeda A, Ueki M. Effect of continuous combined therapy with vitamin K(2) and vitamin D(3) on bone mineral density and coagulofibrinolysis function in postmenopausal women. Maturitas. 2002 Mar 25;41(3):211-21.
- Shiraki M, Shiraki Y, Aoki C, et al. Vitamin K2 (menatetrenone) effectively prevents fractures and sustains lumbar bone mineral density in osteoporosis. J Bone Miner Res. 2000 Mar;15(3):515-21.
- Tran T, Bliuc D, Hansen L, et al. Persistence of Excess Mortality Following Individual Nonhip Fractures: A Relative Survival Analysis. J Clin Endocrinol Metab. 2018 Sep 1;103(9):3205-14.
- Berger C, Goltzman D, Langsetmo L, et al. Peak bone mass from longitudinal data: implications for the prevalence, pathophysiology, and diagnosis of osteoporosis. J Bone Miner Res. 2010 Sep;25(9):1948-57.
- Services DoHaH. Bone Health and Osteoporosis: A Report of the Surgeon General. 2004.
- Hinshaw WB, DeLong AF. An Evaluative History of Bisphosphonate Drugs: Dual Physiologic Effects of Pyrophosphate as Inspiration for a Novel Pharmaceutical Class. J Osteoporos. 2016 2016/10/05;2016:1426279.
- Watts NB, Diab DL. Long-term use of bisphosphonates in osteoporosis. J Clin Endocrinol Metab. 2010 Apr;95(4):1555-65.
- Whitaker M, Guo J, Kehoe T, et al. Bisphosphonates for osteoporosis--where do we go from here? N Engl J Med. 2012 May 31;366(22):2048-51.
- Akbari S, Rasouli-Ghahroudi AA. Vitamin K and Bone Metabolism: A Review of the Latest Evidence in Preclinical Studies. Biomed Res Int. 2018;2018:4629383.
- Palermo A, Tuccinardi D, D’Onofrio L, et al. Vitamin K and osteoporosis: Myth or reality? Metabolism. 2017 May;70:57-71.
- van Ballegooijen AJ, Pilz S, Tomaschitz A, et al. The Synergistic Interplay between Vitamins D and K for Bone and Cardiovascular Health: A Narrative Review. Int J Endocrinol. 2017;2017:7454376.
- Straub DA. Calcium supplementation in clinical practice: a review of forms, doses, and indications. Nutr Clin Pract. 2007 Jun;22(3):286-96.
- Kalluru R, Ames R, Mason B, et al. Bone density in healthy men after cessation of calcium supplements: 20-month follow-up of a randomized controlled trial. Osteoporos Int. 2015 Jan;26(1):173-8.
- Schild A, Herter-Aeberli I, Fattinger K, et al. Oral Vitamin D Supplements Increase Serum 25-Hydroxyvitamin D in Postmenopausal Women and Reduce Bone Calcium Flux Measured by 41Ca Skeletal Labeling. J Nutr. 2015 Oct;145(10):2333-40.
- Matsuzaki H. [Prevention of osteoporosis by foods and dietary supplements. Magnesium and bone metabolism]. Clin Calcium. 2006 Oct;16(10):1655-60.
- Pepa GD, Brandi ML. Microelements for bone boost: the last but not the least. Clin Cases Miner Bone Metab. 2016 Sep-Dec;13(3):181-5.
- El Asmar MS, Naoum JJ, Arbid EJ. Vitamin k dependent proteins and the role of vitamin k2 in the modulation of vascular calcification: a review. Oman Med J. 2014 May;29(3):172-7.
- van den Heuvel EG, van Schoor NM, Lips P, et al. Circulating uncarboxylated matrix Gla protein, a marker of vitamin K status, as a risk factor of cardiovascular disease. Maturitas. 2014 Feb;77(2):137-41.
- Jaminon AMG, Dai L, Qureshi AR, et al. Matrix Gla protein is an independent predictor of both intimal and medial vascular calcification in chronic kidney disease. Sci Rep. 2020 Apr 20;10(1):6586.
- Harshman SG, Shea MK. The Role of Vitamin K in Chronic Aging Diseases: Inflammation, Cardiovascular Disease, and Osteoarthritis. Curr Nutr Rep. 2016 Jun;5(2):90-8.
- Asakura H, Myou S, Ontachi Y, et al. Vitamin K administration to elderly patients with osteoporosis induces no hemostatic activation, even in those with suspected vitamin K deficiency. Osteoporos Int. 2001 Dec;12(12):996-1000.
- Cockayne S, Adamson J, Lanham-New S, et al. Vitamin K and the prevention of fractures: systematic review and meta-analysis of randomized controlled trials. Arch Intern Med. 2006 Jun 26;166(12):1256-61.
- Lumachi F, Luisetto G, Basso SM, et al. Endocrine therapy of breast cancer. Curr Med Chem. 2011;18(4):513-22.
- Mazziotti G, Canalis E, Giustina A. Drug-induced osteoporosis: mechanisms and clinical implications. Am J Med. 2010 Oct;123(10):877-84.
- Briot K, Roux C. Drug-induced osteoporosis: beyond glucocorticoids. Curr Rheumatol Rep. 2008 Apr;10(2):102-9.
- Mirza F, Canalis E. Management of endocrine disease: Secondary osteoporosis: pathophysiology and management. Eur J Endocrinol. 2015 Sep;173(3):R131-51.
- Namba S, Yamaoka-Tojo M, Hashikata T, et al. Long-term warfarin therapy and biomarkers for osteoporosis and atherosclerosis. BBA Clin. 2015 Dec;4:76-80.
- Namba S, Yamaoka-Tojo M, Kakizaki R, et al. Effects on bone metabolism markers and arterial stiffness by switching to rivaroxaban from warfarin in patients with atrial fibrillation. Heart Vessels. 2017 Aug;32(8):977-82.
- Andersen BN, Johansen PB, Abrahamsen B. Proton pump inhibitors and osteoporosis. Curr Opin Rheumatol. 2016 Jul;28(4):420-5.
- Lin SM, Yang SH, Liang CC, et al. Proton pump inhibitor use and the risk of osteoporosis and fracture in stroke patients: a population-based cohort study. Osteoporos Int. 2018 Jan;29(1):153-62.