Life Extension Magazine.
On February 1, 2022, the Journal of the American Medical Association (JAMA) published a report showing that melatonin consumption “significantly increased” from 1999 to 2018 in the United States.1
The authors point to this trend of “self-administered” melatonin as a reason to raise “safety concerns” about the lack of long-term clinical data. They make insinuations about the poor quality of melatonin supplements sold by certain commercial companies.
Concerns were also raised about insufficient study of people taking melatonin in nightly doses above 5 mg.
It was 30 years ago when our Life Extension group introduced the world to melatonin. We provided purified melatonin to researchers for human studies, and to our supporters.
We’ve had interactions with thousands of people who have used a wide range of melatonin potencies since we launched it in 1992.
Rather than defend our long-term observed safe use of melatonin, this article will provide a rationale for some people to consider higher doses. I’ve self-experimented with these higher potencies for the last two years without experiencing adverse reactions.
The main reason I increased my nightly melatonin dose is the potential for immune benefits.2
In reviewing evidence about higher-dose melatonin, I recalled our 40-year history of erring on the side of safety when introducing health-promoting compounds.
Below are examples of dosage increases of nutrients that Life Extension helped pioneer over the decades:
Ingredient |
Initial Dose |
Current Average Dose |
CoQ10 |
10-30 mg |
100-200 mg. |
Vitamin D |
400-800 IU |
2,000-5,000 IU |
Resveratrol |
20 mg |
100-250 mg |
Vitamin K |
45-65 mcg |
2,000-45,000 mcg |
NAD+ precursor (nicotinamide riboside) |
100 mg |
300 mg |
These higher potencies are made practical by price reductions for ingredients like CoQ10 and resveratrol.
CoQ10 costs a fraction of what it did when Life Extension introduced it in 1983, as does resveratrol that we launched in 2003.
Given our history of using published data to increase suggested doses, I decided to try 50 mg of melatonin each night and found some sleep improvement.
I’ve since lowered my overall melatonin dose to incorporate more sustained-release formulas, so my average nightly dose is now around 20 mg.
This article describes what researchers are finding as it relates to additional benefits that may be achieved using a wide range of melatonin doses.
The phrase “sleep like a baby” refers to tranquil, deep sleep patterns like those young children typically enjoy.
What few people know is that nighttime blood levels of melatonin in children ages 1 to 3 years are very high and then progressively drop by 80% during the remainder of childhood.3
Total melatonin secretion further declines with increasing age, beginning perhaps as early as the third decade of life.4,5
Data like these prompted some physician-scientists to hypothesize that adults might benefit from higher potencies of melatonin when dealing with serious illnesses.
While many studies support some sleep-enhancing properties of low- and moderate-dose melatonin,6,7 lacking are tightly controlled human studies measuring the nocturnal effects of high-dose melatonin.
What are not missing are an abundant number of studies describing the potential of melatonin to help prevent and combat cancer.
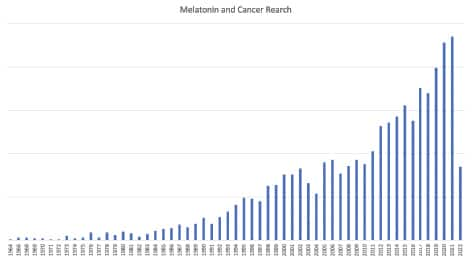
Melatonin and Cancer
In the early 1990s, I went on national TV talk shows to announce the lifesaving benefits of melatonin. The data back then showed that melatonin improved immunity and might prevent and/or help fight certain cancers.8,9
Move forward to 2022, and there are over 3,000 published studies investigating the potential of melatonin to be useful in cancer prevention or as an adjuvant agent in therapy for cancer patients.
Data demonstrating anti-cancer or other beneficial effects of melatonin in patients are still limited, but results are encouraging.
In a handful of completed clinical trials in patients with primary brain tumors, colorectal cancer, non-small-cell lung cancer, breast cancer, and brain metastasis, researchers found that melatonin, in doses up to 40 mg daily, worked well with conventional treatments.
Researchers also noted improved quality of life in cancer patients when no other treatment was available.10-16
In two separate reviews of clinical trials assessing the use of melatonin during chemotherapy or radiation for the treatment of solid tumors, melatonin was found to decrease negative side effects such as fatigue and low platelet counts, improve response to treatment, and increase one-year survival.17,18
You can access study abstracts about “melatonin and cancer” for free on the National Library of Medicine website at www.PubMed.gov
At the end of this editorial there is a summary of studies excerpted from the National Library of Medicine website about the role of melatonin in reducing cancer incidence and mortality.
Melatonin Use in Rheumatoid Arthritis
By enhancing certain immune functions, some early preclinical research suggests melatonin may increase the severity of rheumatoid arthritis, which is an autoimmune disease.33-35
This is in contradiction to beneficial effects of melatonin in other autoimmune inflammatory diseases.36
Evidence from clinical studies indicates that low-dose melatonin (≤10 mg) does not seem to cause harmful effects in subjects with autoimmune diseases, such as multiple sclerosis, ulcerative colitis, lupus, and inflammatory bowel disease.37-43
In the past decade, some studies demonstrated that melatonin can alleviate rheumatoid arthritis through the inhibition of specific inflammatory factors.44-48
In fact, a 2021 study found that treatment with 6 mg of melatonin daily for 12 weeks improved many markers of disease in rheumatoid arthritis patients.49
The use of melatonin at doses under 10 mg in rheumatoid arthritis patients may need consideration by treating physicians.
It is unknown whether high-dose melatonin ≥50 mg may exert any harmful effects in those with autoimmune diseases, especially in rheumatoid arthritis patients.
Preclinical Studies on Low-and High-Dose Melatonin
In seeking to ascertain the effects of high-dose melatonin we came across some interesting findings suggesting benefits with higher dosing. Summaries from these studies are copied below:
- In a mouse model of amyotrophic lateral sclerosis (ALS), a high-dose oral melatonin delayed disease progression and extended survival.19
- High-dose melatonin administered intraperitoneally before myocardial (heart) injury offered protection against cardiac ischemia-reperfusion injury in Sprague-Dawley rats.20
- High-dose melatonin injected intraperitoneally for 56 days reduced myocardial hyper-trophy and preserved cardiac function in diabetic Wistar rats.21
- High-dose melatonin (human equivalent of 55 mg a day for 30 days) in senescence-prone mice showed that age-related increases in markers of inflammation, oxidative stress and apoptosis were effectively reduced by both low- and high-melatonin doses studied.22
- Two additional studies with almost identical experimental designs found protective effects of high-dose melatonin on heart and lung tissue alterations in a mouse model of aging.23,24
Human Studies of High-Dose Melatonin
In a clinical safety study of ALS (also called Lou Gehrig’s disease) patients, a chronic high dose (300 mg/day) of enteral melatonin was well tolerated for up to two years. In this study, a surrogate marker for oxidative stress that is elevated in ALS patients was normalized by melatonin treatment. This implies a neuroprotective effect through reduction of oxidative stress. 19
A crossover clinical study including 12 healthy male volunteers investigated the effects of high-dose (100 mg) intravenous melatonin and found no adverse effects. This study did not find a greater sedative effect with the 100 mg intravenous melatonin relative to a 10 mg dose.25
Indole melatonin (50 mg) administered intravenously to three male narcoleptics dramatically increased the amount of REM sleep and decreased REM sleep latency.26
At doses ranging from 10 to 40 mg daily, melatonin in combination with IL-2 immunotherapy has been shown to improve outcomes in patients being treated for metastatic cancer.27-30
A 20 mg daily oral dose of melatonin, divided into two 10 mg doses, administered to septic newborns, improved their clinical outcomes after 24 and 48 hours and prevented death. All the newborns treated with melatonin survived, while three of the 10 babies in the non-melatonin group died.31
Currently, a clinical trial of antioxidant therapy in adult patients critically ill with septic shock is evaluating the efficacy of a 50 mg nighttime dose of melatonin. Results are pending (NCT03557229).32
Short-Term Studies Using High-Dose Melatonin in Humans
A surprising number of human studies have been done using varying melatonin doses without serious side effects being found.
In an analysis of 50 studies evaluating the efficacy of oral melatonin supplementation (1-20 mg), less than half the studies reported adverse events, which were typically minor and transient. Fatigue was seen most often in studies in which melatonin was taken during daytime hours.50
A double-blind, placebo-controlled study evaluating the utility of 5-20 mg of sublingual melatonin in patients undergoing gynecological surgical procedures reported neither dose-dependent nor dose-independent adverse events.51
General Safety Data on High-Dose Melatonin
A member of our scientific team did a comprehensive search of the published medical literature. Below is an Executive Summary of this literature review:
Executive Summary: Safety of High-Dose Melatonin
Based on a thorough and comprehensive evaluation of the most up-to-date scientific evidence from reputable sources, the conclusions of our review on efficacy and toxicity/safety of high-dose melatonin are as follows:
-- High-dose melatonin (doses 50 mg and above) has been used in preclinical and clinical settings, and data collectively show that melatonin even at high doses has a good safety profile and is beneficial, improving disease outcomes.
However, at this time preclinical as well as clinical evidence does not clearly demonstrate that increasing the dose of melatonin is accelerating and/or amplifying melatonin benefits. That is because studies specifically addressing dose-dependent effects of melatonin in various settings are lacking.
-- There are no clinical data showing whether high-dose 50 mg melatonin may exert any harmful effects in patients with autoimmune diseases, especially rheumatoid arthritis.
-- There is currently no compelling clinical evidence clearly showing that high-dose melatonin (50 mg and above) supplementation may interact with prescription drugs and decrease their effectiveness when taken concomitantly.
Oral administration of 1,000 mg a day of melatonin to five adults for 25 to 30 days resulted in drowsiness being noted as an adverse effect. There were no severe and/or irreversible impacts on clinical parameters (blood pressure, heart rate, ECG, serum chemistry, urine analysis) in these people taking a massive 1,000 mg dose of melatonin each night for 25 to 30 days.52
Three separate studies did not report adverse side effects using the following high doses of melatonin:
- 90 mg, on average, intravenously administered to healthy patients as well as individuals with seizure disorder and Parkinson’s disease,53
- 10 mg per kilogram (intravenous) in preterm infants and septic neonates,54 and
- 100 mg (intravenous) in healthy subjects.25
These findings suggest that extremely high doses of oral melatonin (1,000 mg/day), enteral melatonin (300 mg/day) and intravenous melatonin (1-100 mg) are safe and do not cause clinically significant side effects.
I am not recommending these high doses, just reporting on what’s already been studied in people.
The studies reported in this section were short term and not the long-term, rigorous human trials that the authors of the February 2022 published JAMA report1 and we at Life Extension would like to see conducted.
The dilemma is who is going to pay for a multimillion-dollar, long-term clinical trial using high-dose melatonin when it has been available as a low-cost dietary supplement for the last 30 years?
High-Dose Melatonin and Prescription Drugs
There is currently no compelling clinical evidence clearly showing that high-dose melatonin (30-50 mg) supplementation will interact with prescription drugs and decrease their effectiveness when taken concomitantly.
The comprehensive 2019 review of 50 studies described earlier including 17 studies in which participants were taking a variety of common medications or receiving treatment for cancer, did not find reports of apparent drug interactions.50
The caveat, however, is that there are relatively little human data enabling us to know this for certain.
My only concern is for those with a propensity for low blood pressure, especially because blood pressure normally drops lower at night.
Melatonin has beneficial blood pressure-lowering effects.55-57
Those with high blood pressure often take their antihypertensive drug(s) at night for maximal efficacy. Melatonin may provide additional blood pressure-reducing effects, especially for those challenged to achieve optimal blood pressure levels.
Those concerned with blood pressure dropping too low, but who still want to try higher-dose melatonin, may consider starting with perhaps 6-10 mg a night, using an at-home monitor to self-assess blood pressure, and adjusting the melatonin dose upwards if blood pressure does not drop too low.
I hope every one of our readers has an at-home blood pressure monitor, whose prices continue to drop to an affordable range.
The 30-50 mg nightly doses of melatonin I have taken over the past two years have not caused any apparent side effects in me.
Some of you who do not rapidly metabolize melatonin will likely face next-day grogginess and may not want to take this high melatonin dose.
Melatonin Put Life Extension® on the Map
When Life Extension® introduced melatonin to the world in 1992, virtually no one had ever heard the term. It’s now a household name liberally described in the mainstream media as facilitating better sleep.
When the New York Academy of Sciences published a book on the multiple benefits of melatonin, the media picked up on it and I became a guest on some of the most popular talk shows in America.
The JAMA report (February 1, 2022) warns about unknown risks of long-term “self-administered” melatonin. JAMA is the American Medical Association’s most widely read journal.
Contrary to the position taken in the JAMA report, I present published data in this editorial as to why I am self-experimenting with higher-dose melatonin.
In particular, I am intrigued by the consistency of data indicating that melatonin may reduce cancer risk and improve outcomes of cancer patients treated with conventional therapy. These findings, which you can read for yourself at www.PubMed.gov, provide a compelling reason for most aging humans to supplement with at least a few milligrams of melatonin each night.
Copied at the end of this article are the results of a recent database search using the terms “melatonin and cancer.”
Those who self-experiment as I do may consider trying 10 mg or more of melatonin about 30 minutes before bedtime. I started off with 10 mg and added some sustained-release melatonin so as not to wake up too early. My average nightly melatonin dose now is around 20 mg.
In this month’s issue…
The world has woken up to the fact that normal aging is accompanied by loss of immune functions. The article on page 32 describes the immune enhancing properties of specific mushrooms.
Vitamin K helps maintain bone density and protect against soft tissue calcification. The article on page 50 reviews research showing how vitamin K can improve heart health.
Other articles this month describe the systemic effects of N-aceytl-L-cysteine and a popular way people today are taking their nightly melatonin.
For longer life,
William Faloon
Our Ongoing Support of Biomedical Research
Life Extension® donates supplements to physician-scientists who use them in clinical trials to ascertain efficacy against a wide range of degenerative disorders.
In 2021, a study was published using 20 mg melatonin capsules that Life Extension® specially formulated to study on non-small-cell lung cancer patients. We also provided identical-looking placebo capsules for this outside research group.
The data below highlight the improved survival in those receiving 20 mg of melatonin compared to placebo:
DAILY EVENING MELATONIN PROLONGS SURVIVAL AMONG PATIENTS WITH ADVANCED NON-SMALL-CELL LUNG CANCER10
- 20 mg melatonin as an adjunctive to standard chemo treatment.
- Evening supplementation of melatonin reduced risk of death by 39%.
- Individuals with normal baseline sleep had a median survival of 17.6 months with evening melatonin compared to 10.4 months in the placebo group.
Acknowledgments: We would like to thank William Faloon of Life Extension for providing melatonin and placebo for this study.
Biological Rhythm Research. 2021:1-15.
National Library of Medicine
Titles and Descriptions of Published Studies About Melatonin and Cancer
These pages contain titles and brief descriptions of studies that were published in 2021 and 2022, listed on the federal government’s National Library of Medicine’s data base (www.pubmed.gov).
What we reprinted is only a small portion of the hundreds of studies about “melatonin and cancer” one can easily access by logging on to www.PubMed.gov
Melatonin in Cancer Treatment: Current Knowledge and Future Opportunities.
Talib WH, Alsayed AR, Abuawad A, Daoud S, Mahmod AI.
Molecules. 2021 Apr 25;26(9):2506. doi: 10.3390/molecules26092506.PMID: 33923028 Free PMC article. Review.
Epidemiological and experimental studies have documented that melatonin could inhibit different types of cancer in vitro and in vivo. ...Studies discussed in this review will provide a solid foundation for researchers and physicians to design and develop new…
Melatonin-A New Prospect in Prostate and Breast Cancer Management.
Anim-Koranteng C, Shah HE, Bhawnani N, Ethirajulu A, Alkasabera A, Onyali CB, Mostafa JA.
Cureus. 2021 Sep 20;13(9):e18124. doi: 10.7759/cureus.18124. eCollection 2021 Sep.PMID: 34692334 Free PMC article. Review.
Melatonin exerts its oncostatic effect by inhibiting angiogenesis, preventing cancer spread and growth, and improving the sensitivity of cancer cells to radiation and chemotherapy in both prostate and breast cancer. This review aims to highlight some…
Circadian Rhythm and Concentration of Melatonin in Breast Cancer Patients.
Ahabrach H, El Mlili N, Errami M, Cauli O.
Endocr Metab Immune Disord Drug Targets. 2021;21(10):1869-1881. doi: 10.2174/1871530320666201201110807.PMID: 33261546 Review.
Melatonin has also been shown to display anti-proliferative effects on breast cancer growth and proliferation. ...CONCLUSION: Circadian rhythm and the concentration of melatonin in the blood are altered in patients with breast cancers, and it can…
Melatonin and Pathological Cell Interactions: Mitochondrial Glucose Processing in Cancer Cells.
Reiter RJ, Sharma R, Rosales-Corral S, Manucha W, Chuffa LGA, Zuccari DAPC.
Int J Mol Sci. 2021 Nov 19;22(22):12494. doi: 10.3390/ijms222212494.PMID: 34830375 Free PMC article. Review.
Melatonin is synthesized in the pineal gland at night. Since melatonin is produced in the mitochondria of all other cells in a non-circadian manner, the amount synthesized by the pineal gland is less than 5% of the total. Melatonin produced in mitochondria in …
Usefulness of Melatonin and Other Compounds as Antioxidants and Epidrugs in the Treatment of Head and Neck Cancer.
Guerra J, Devesa J.
Antioxidants (Basel). 2021 Dec 24;11(1):35. doi: 10.3390/antiox11010035.PMID: 35052539 Free PMC article. Review.
Along with genetic mutations, aberrant epigenetic alterations are the initiators of head and neck cancer carcinogenesis. Currently, several drugs are being developed to correct these epigenetic alterations, known as epidrugs. ...The objective of this review is to describe …
Sleep disorders and cancer: State of the art and future perspectives.
Mogavero MP, DelRosso LM, Fanfulla F, Bruni O, Ferri R.
Sleep Med Rev. 2021 Apr;56:101409. doi: 10.1016/j.smrv.2020.101409. Epub 2020 Nov 28.PMID: 33333427 Review.
A bidirectional connection between sleep and cancer exists; however, the specific associations between individual sleep disorders and particular tumors are not very clear. An accurate assessment of sleep disorders in cancer patients is necessary to improve patient …
Involvement of NRF2 in Breast Cancer and Possible Therapeutical Role of Polyphenols and Melatonin.
Tascioglu Aliyev A, Panieri E, Stepanić V, Gurer-Orhan H, Saso L.
Molecules. 2021 Mar 25;26(7):1853. doi: 10.3390/molecules26071853.PMID: 33805996 Free PMC article. Review.
Due to its regulatory role in the expression of numerous cytoprotective genes involved in the antioxidant and anti-inflammatory responses, the modulation of NRF2 seems to be a promising approach in the prevention …
Role and Therapeutic Potential of Melatonin in Various Type of Cancers.
Gurunathan S, Qasim M, Kang MH, Kim JH.
Onco Targets Ther. 2021 Mar 18;14:2019-2052. doi: 10.2147/OTT.S298512. eCollection 2021.PMID: 33776451 Free PMC article. Review.
Lung, prostate, colorectal, stomach, and liver cancers are the most common types of cancer in men, whereas breast, colorectal, lung, cervical, and thyroid cancers are the most common among women. ...The combination of melatonin with conventional drugs …
The effect of melatonin on sleep quality and insomnia in patients with cancer: a systematic review study.
Jafari-Koulaee A, Bagheri-Nesami M.
Sleep Med. 2021 Jun;82:96-103. doi: 10.1016/j sleep. 2021.03.040. Epub 2021 Apr 25.PMID: 33910162 Review.
Therefore, the aim of the present systematic review was to investigate effect of melatonin on sleep quality and insomnia in patients with cancer. METHODS: The present systematic review was conducted in 2021. ...CONCLUSIONS: The present review study showed that melatonin may be …
Pan-cancer analyses reveal genomics and clinical characteristics of the melatonergic regulators in cancer.
Zhang J, Jiang H, Du K, Xie T, Wang B, Chen C, Reiter RJ, Cen B, Yuan Y.
J Pineal Res. 2021 Oct;71(3):e12758. doi: 10.1111/jpi.12758. Epub 2021 Sep 5.PMID: 34289167
Melatonin, an endogenous hormone, plays protective roles in cancer. ...In the present study, we performed a comprehensive characterization of melatonin regulators in 9,125 tumor samples across 33 cancer types using multi-omic data from The Cancer Genome Atlas …
Melatonin inhibits proliferation and viability and promotes apoptosis in colorectal cancer cells via upregulation of the microRNA-34a/449a cluster.
Ji G, Zhou W, Li X, Du J, Li X, Hao H.
Mol Med Rep. 2021 Mar;23(3):187. doi: 10.3892/mmr. 2021.11826. Epub 2021 Jan 5.PMID: 33398374 Free PMC article.
Melatonin exerts anticarcinogenic effects via various mechanisms; however, the identified underlying molecular mechanisms do not explain the full breadth of anti-CRC effects mediated by melatonin. ...Therefore, melatonin may serve as a potential therapeutic …
A New Paradigm in the Relationship between Melatonin and Breast Cancer: Gut Microbiota Identified as a Potential Regulatory Agent.
Laborda-Illanes A, Sánchez-Alcoholado L, Boutriq S, Plaza-Andrades I, Peralta-Linero J, Alba E, González-González A, Queipo-Ortuño MI.
Cancers (Basel). 2021 Jun 23;13(13):3141. doi: 10.3390/cancers13133141.PMID: 34201776 Free PMC article. Review.
In this review we summarize a possible connection between gut microbiota, melatonin production, and breast cancer. An imbalance in gut bacterial population composition (dysbiosis), or changes in the production of melatonin (circadian disruption) alters …
The Intricate Relationship between Melatonin and Breast Cancer: A Short Review.
Pistioli L, Katsarelias D, Audisio RA, Olofsson Bagge R.
Chirurgia (Bucur). 2021 Mar-Apr;116(2 Suppl):24-34.PMID: 33963691 Free article.
There is ongoing research investigating the deterrent relationship between melatonin and malignancies and in particular breast cancer. The aim of this article is to review some of the most important findings concerning the effect of melatonin on cancer …
Melatonin and its derivative disrupt cancer stem-like phenotypes of lung cancer cells via AKT downregulation.
Phiboonchaiyanan PP, Puthongking P, Chawjarean V, Harikarnpakdee S, Sukprasansap M, Chanvorachote P, Priprem A, Govitrapong P.
Clin Exp Pharmacol Physiol. 2021 Dec;48(12):1712-1723. doi: 10.1111/1440-1681.13572. Epub 2021 Aug 31.PMID: 34396568
Cancer stem cells (CSCs), a small subpopulation of tumour cells, have properties of self-renewal and multipotency, which drive cancer progression and resistance to current treatments. Compounds potentially targeting CSCs have been recently developed. This study show …
Melatonin and Cancer: A Polyhedral Network Where the Source Matters.
Bonmati-Carrion MA, Tomas-Loba A.
Antioxidants (Basel). 2021 Feb 1;10(2):210. doi: 10.3390/antiox10020210.PMID: 33535472 Free PMC article. Review.
Indeed, this activity has been demonstrated to be mediated by interfering with various cancer hallmarks, and different epidemiological studies have also linked light at night (melatonin suppression) with a higher incidence of different types of cancer.
Melatonin interrupts osteoclast functioning and suppresses tumor-secreted RANKL expression: implications for bone metastases.
Liu PI, Chang AC, Lai JL, Lin TH, Tsai CH, Chen PC, Jiang YJ, Lin LW, Huang WC, Yang SF, Tang CH.
Oncogene. 2021 Feb;40(8):1503-1515. doi: 10.1038/s41388-020-01613-4. Epub 2021 Jan 15.PMID: 33452455
We also observed that melatonin inhibits RANKL production in lung and prostate cancer cells by downregulating the p38 MAPK pathway, which in turn prevents cancer-associated osteoclast differentiation. ...These findings show promise for melatonin in the …
Melatonin inhibits lung cancer development by reversing the Warburg effect via stimulating the SIRT3/PDH axis.
Chen X, Hao B, Li D, Reiter RJ, Bai Y, Abay B, Chen G, Lin S, Zheng T, Ren Y, Xu X, Li M, Fan L.
J Pineal Res. 2021 Sep;71(2):e12755. doi: 10.1111/jpi.12755. Epub 2021 Jul 30.PMID: 34214200
Recently, the morbidity and mortality from lung cancer have continued to increase. Mitochondrial dysfunction plays a key role in apoptosis, proliferation, and the bioenergetic reprogramming of cancer cells, especially for energy metabolism. Herein, we investigated …
Effects of melatonin and doxorubicin on primary tumor and metastasis in breast cancer model.
Tanriover G, Dilmac S, Aytac G, Farooqi AA, Sindel M.
Anticancer Agents Med Chem. 2021 Dec 12. doi: 10.2174/1871520621666211213094258. Online ahead of print.PMID: 34961467
BACKGROUND: Melatonin exerts oncostatic effects on breast cancer via immunomodulation and anti-oxidation. ...Based on these results, melatonin is a promising candidate for combinatory use with conventional chemotherapeutics for breast cancer treatment. …
MT1 and MT2 melatonin receptors play opposite roles in brain cancer progression.
Kinker GS, Ostrowski LH, Ribeiro PAC, Chanoch R, Muxel SM, Tirosh I, Spadoni G, Rivara S, Martins VR, Santos TG, Markus RP, Fernandes PA.
J Mol Med (Berl). 2021 Feb;99(2):289-301. doi: 10.1007/s00109-020-02023-5. Epub 2021 Jan 3.PMID: 33392634
Primary brain tumors remain among the deadliest of all cancers. Glioma grade IV (glioblastoma), the most common and malignant type of brain cancer, is associated with a 5-year survival rate of < 5%. ...However, our understanding of the specific effects mediated …
Melatonin inhibits gallbladder cancer cell migration and invasion via ERK-mediated induction of epithelial-to-mesenchymal transition.
Tang H, Shi X, Zhu P, Guo W, Li J, Yan B, Zhang S.
Oncol Lett. 2021 Aug;22(2):609. doi: 10.3892/ol.2021.12870. Epub 2021 Jun 15.PMID: 34188711 Free PMC article.
However, little is known regarding the effects of melatonin on gallbladder cancer (GBC) cells. The present study aimed to investigate the role of melatonin on the prevention of GBC cell invasion. ...Thus, melatonin may be used as a potential novel …
Melatonin indirectly decreases gastric cancer cell proliferation and invasion via effects on cancer-associated fibroblasts.
Liu D, Shi K, Fu M, Chen F.
Life Sci. 2021 Jul 15;277:119497. doi: 10.1016/j.lfs.2021.119497. Epub 2021 Apr 18.PMID: 33864820
Recent studies have revealed the potential value of melatonin in cancer therapy, but its role in gastric cancer and CAFs requires further exploration. ...SIGNIFICANCE: This study provides insights into the role of melatonin in the tumor microenvironment …
Alcohol and melatonin.
Kurhaluk N.
Chronobiol Int. 2021 Jun;38(6):785-800. doi: 10.1080/07420528.2021.1899198. Epub 2021 Mar 24.PMID: 33761823 Review.
It discusses the main clinical effects of melatonin on alcohol injury and the main targets as a therapy for alcohol disorders. Chronobiological effects of ethanol are related to melatonin suppression that has been associated with, among others, cancer risk …
Melatonin reduces proliferation and promotes apoptosis of bladder cancer cells by suppressing O-GlcNAcylation of cyclin-dependent-like kinase 5.
Wu J, Tan Z, Li H, Lin M, Jiang Y, Liang L, Ma Q, Gou J, Ning L, Li X, Guan F.
J Pineal Res. 2021 Oct;71(3):e12765. doi: 10.1111/jpi.12765. Epub 2021 Sep 18.PMID: 34487576
Dysregulated glycosylation, particularly O-GlcNAcylation, is often a biomarker of cancer cells. In this study, elevated O-GlcNAc level in bladder cancer was inhibited by melatonin treatment. Melatonin treatment inhibited proliferation and migration and …
Associations between artificial light at night and risk for thyroid cancer: A large US cohort study.
Zhang D, Jones RR, James P, Kitahara CM, Xiao Q.
Cancer. 2021 May 1;127(9):1448-1458. doi: 10.1002/cncr.33392. Epub 2021 Feb 8.PMID: 33554351
BACKGROUND: Light at night (LAN) inhibits nighttime secretion of melatonin and may cause circadian disruption, which may be a risk factor for cancer. Recent studies have linked high LAN exposure with elevated breast cancer risk. Given that breast cancer …
Melatonin Targets Metabolism in Head and Neck Cancer Cells by Regulating Mitochondrial Structure and Function.
Guerra-Librero A, Fernandez-Gil BI, Florido J, Martinez-Ruiz L, Rodríguez-Santana C, Shen YQ, García-Verdugo JM, López-Rodríguez A, Rusanova I, Quiñones-Hinojosa A, Acuña-Castroviejo D, Marruecos J, De Haro T, Escames G.
Antioxidants (Basel). 2021 Apr 14;10(4):603. doi: 10.3390/antiox10040603.PMID: 33919790 Free PMC article.
In this study, we aim to investigate the role of melatonin in mitochondrial metabolism and its functional consequences in head and neck cancer. ...Our findings highlight new molecular pathways involved in melatonin’s oncostatic activity, suggesting …
Melatonin Inhibits Migration and Invasion in LPS-Stimulated and-Unstimulated Prostate Cancer Cells Through Blocking Multiple EMT-Relative Pathways.
Tian QX, Zhang ZH, Ye QL, Xu S, Hong Q, Xing WY, Chen L, Yu DX, Xu DX, Xie DD.
J Inflamm Res. 2021 May 25;14:2253-2265. doi: 10.2147/JIR.S305450. eCollection 2021.PMID: 34079331 Free PMC article.
PURPOSE: Gram-negative bacteria are usually found in prostate cancer (PCa) tissues. This study aims to investigate the role of lipopolysaccharide (LPS), a glycolipid compound found in the outer membrane of gram-negativebacteria, on the migration and invasion of PCa cells, …
National Library of Medicine
Back in the 1980s, finding medical studies was an arduous task.
To uncover published data, our group spent days in medical libraries using an archaic paper system (Index Medicus) to find relevant medical journals.
We then had to hope the library subscribed to that journal, photocopy relevant articles, bring them back to our office and mail information to others for further analysis.
In the early 1990s, a subscription service became available whereby I received four large floppy disks with new medical studies every Saturday. I would load the disks onto my computer and search items of interest. This was a huge improvement compared to spending days at a medical library.
Then in 1997 the National Library of Medicine offered free public access to medical articles dating back to the late 1970s. The National Library of Medicine is operated by the United States government and is the world’s largest medical library.
This free service not only makes my work more efficient but enables anyone who reads Life Extension Magazine® to check out studies we write about and find out as many details as they’d like.
References
- Li J, Somers VK, Xu H, et al. Trends in Use of Melatonin Supplements Among US Adults, 1999-2018. JAMA. 2022 Feb 1;327(5):483-5.
- Bondy SC, Campbell A. Melatonin and Regulation of Immune Function: Impact on Numerous Diseases. Curr Aging Sci. 2020;13(2):92-101.
- Waldhauser F, Kovacs J, Reiter E. Age-related changes in melatonin levels in humans and its potential consequences for sleep disorders. Exp Gerontol. 1998 Nov-Dec;33(7-8):759-72.
- Kennaway DJ, Lushington K, Dawson D, et al. Urinary 6-sulfatoxymelatonin excretion and aging: new results and a critical review of the literature. J Pineal Res. 1999 Nov;27(4):210-20.
- Zhou JN, Liu RY, van Heerikhuize J, et al. Alterations in the circadian rhythm of salivary melatonin begin during middle-age. J Pineal Res. 2003 Jan;34(1):11-6.
- Ferracioli-Oda E, Qawasmi A, Bloch MH. Meta-analysis: melatonin for the treatment of primary sleep disorders. PLoS One. 2013;8(5):e63773.
- van Geijlswijk IM, Korzilius HP, Smits MG. The use of exogenous melatonin in delayed sleep phase disorder: a meta-analysis. Sleep. 2010 Dec;33(12):1605-14.
- Lissoni P, Barni S, Cazzaniga M, et al. Efficacy of the concomitant administration of the pineal hormone melatonin in cancer immunotherapy with low-dose IL-2 in patients with advanced solid tumors who had progressed on IL-2 alone. Oncology. 1994 Jul-Aug;51(4):344-7.
- Conti A, Maestroni GJ. The clinical neuroimmunotherapeutic role of melatonin in oncology. J Pineal Res. 1995 Oct;19(3):103-10.
- Hrushesky WJM, Lis CG, Levin RD, et al. Daily evening melatonin prolongs survival among patients with advanced non-small-cell lung cancer. Biological Rhythm Research. 2021:1-15.
- Lissoni P, Barni S, Mandala M, et al. Decreased toxicity and increased efficacy of cancer chemotherapy using the pineal hormone melatonin in metastatic solid tumour patients with poor clinical status. Eur J Cancer. 1999 Nov;35(12):1688-92.
- Lissoni P, Paolorossi F, Tancini G, et al. A phase II study of tamoxifen plus melatonin in metastatic solid tumour patients. Br J Cancer. 1996 Nov;74(9):1466-8.
- Lissoni P, Barni S, Meregalli S, et al. Modulation of cancer endocrine therapy by melatonin: a phase II study of tamoxifen plus melatonin in metastatic breast cancer patients progressing under tamoxifen alone. Br J Cancer. 1995 Apr;71(4):854-6.
- Lissoni P, Barni S, Ardizzoia A, et al. A randomized study with the pineal hormone melatonin versus supportive care alone in patients with brain metastases due to solid neoplasms. Cancer. 1994 Feb 1;73(3):699-701.
- Lissoni P, Barni S, Cattaneo G, et al. Clinical results with the pineal hormone melatonin in advanced cancer resistant to standard antitumor therapies. Oncology. 1991;48(6):448-50.
- Barni S, Lissoni P, Paolorossi F, et al. A study of the pineal hormone melatonin as a second line therapy in metastatic colorectal cancer resistant to fluorouracil plus folates. Tumori. 1990 Feb 28;76(1): 58-60.
- Seely D, Wu P, Fritz H, et al. Melatonin as adjuvant cancer care with and without chemotherapy: a systematic review and meta-analysis of randomized trials. Integr Cancer Ther. 2012 Dec;11(4):293-303.
- Wang YM, Jin BZ, Ai F, et al. The efficacy and safety of melatonin in concurrent chemotherapy or radiotherapy for solid tumors: a meta-analysis of randomized controlled trials. Cancer Chemother Pharmacol. 2012 May;69(5):1213-20.
- Weishaupt JH, Bartels C, Polking E, et al. Reduced oxidative damage in ALS by high-dose enteral melatonin treatment. J Pineal Res. 2006 Nov;41(4):313-23.
- Ceyran H, Narin F, Narin N, et al. The effect of high dose melatonin on cardiac ischemia- reperfusion Injury. Yonsei Med J. 2008 Oct 31;49(5):735-41.
- Kandemir YB, Tosun V, Guntekin U. Melatonin protects against streptozotocin-induced diabetic cardiomyopathy through the mammalian target of rapamycin (mTOR) signaling pathway. Adv Clin Exp Med. 2019 Sep;28(9):1171-7.
- Cuesta S, Kireev R, Garcia C, et al. Beneficial effect of melatonin treatment on inflammation, apoptosis and oxidative stress on pancreas of a senescence accelerated mice model. Mech Ageing Dev. 2011 Nov-Dec;132(11-12):573-82.
- Puig A, Rancan L, Paredes SD, et al. Melatonin decreases the expression of inflammation and apoptosis markers in the lung of a senescence-accelerated mice model. Exp Gerontol. 2016 Mar; 75:1-7.
- Forman K, Vara E, Garcia C, et al. Beneficial effects of melatonin on cardiological alterations in a murine model of accelerated aging. J Pineal Res. 2010 Oct;49(3):312-20.
- Andersen LP, Werner MU, Rosenkilde MM, et al. Pharmacokinetics of high-dose intravenous melatonin in humans. J Clin Pharmacol. 2016 Mar;56(3):324-9.
- Pavel S, Goldstein R, Petrescu M. Vasotocin, melatonin and narcolepsy: possible involvement of the pineal gland in its patho-physiological mechanism. Peptides. 1980 Winter;1(4):281-4.
- Barni S, Lissoni P, Cazzaniga M, et al. A randomized study of low-dose subcutaneous interleukin-2 plus melatonin versus supportive care alone in metastatic colorectal cancer patients progressing under 5-fluorouracil and folates. Oncology. 1995 May-Jun;52(3):243-5.
- Lissoni P, Brivio F, Fumagalli L, et al. Neuroimmunomodulation in medical oncology: application of psychoneuroimmunology with subcutaneous low-dose IL-2 and the pineal hormone melatonin in patients with untreatable metastatic solid tumors. Anticancer Res. 2008 Mar-Apr;28(2B):1377-81.
- Lissoni P, Barni S, Fossati V, et al. A randomized study of neuroimmunotherapy with low-dose subcutaneous interleukin-2 plus melatonin compared to supportive care alone in patients with untreatable metastatic solid tumour. Support Care Cancer. 1995 May;3(3):194-7.
- Lissoni P, Tisi E, Barni S, et al. Biological and clinical results of a neuroimmunotherapy with interleukin-2 and the pineal hormone melatonin as a first line treatment in advanced non-small cell lung cancer. Br J Cancer. 1992 Jul;66(1):155-8.
- Gitto E, Karbownik M, Reiter RJ, et al. Effects of melatonin treatment in septic newborns. Pediatr Res. 2001 Dec;50(6):756-60.
- Available at: https://clinicaltrials.gov/ct2/show/NCT03557229. Accessed March 24, 2022.
- Hansson I, Holmdahl R, Mattsson R. The pineal hormone melatonin exaggerates development of collagen-induced arthritis in mice. J Neuroimmunol. 1992 Jul;39(1-2):23-30.
- Bang J, Chang HW, Jung HR, et al. Melatonin attenuates clock gene cryptochrome1, which may aggravate mouse anti-type II collagen antibody-induced arthritis. Rheumatol Int. 2012 Feb;32(2):379-85.
- Jimenez-Caliani AJ, Jimenez-Jorge S, Molinero P, et al. Dual effect of melatonin as proinflammatory and antioxidant in collagen-induced arthritis in rats. J Pineal Res. 2005 Mar;38(2):93-9.
- Zhao CN, Wang P, Mao YM, et al. Potential role of melatonin in autoimmune diseases. Cytokine Growth Factor Rev. 2019 Aug;48:1-10.
- Nabatian-Asl M, Ghorbanihaghjo A, Malek Mahdavi A, et al. Effects of melatonin supplementation on serum oxidative stress markers and disease activity in systemic lupus erythematosus patients: A randomised, double-blind, placebo-controlled trial. Int J Clin Pract. 2021 Jul;75(7):e14246.
- Adamczyk-Sowa M, Sowa P, Adamczyk J, et al. Effect of melatonin supplementation on plasma lipid hydroperoxides, homocysteine concentration and chronic fatigue syndrome in multiple sclerosis patients treated with interferons-beta and mitoxantrone. J Physiol Pharmacol. 2016 Apr;67(2):235-42.
- Adamczyk-Sowa M, Pierzchala K, Sowa P, et al. Influence of melatonin supplementation on serum antioxidative properties and impact of the quality of life in multiple sclerosis patients. J Physiol Pharmacol. 2014 Aug;65(4):543-50.
- Mozaffari S, Abdollahi M. Melatonin, a promising supplement in inflammatory bowel disease: a comprehensive review of evidences. Curr Pharm Des. 2011 Dec;17(38):4372-8.
- Chojnacki C, Wisniewska-Jarosinska M, Walecka-Kapica E, et al. Evaluation of melatonin effectiveness in the adjuvant treatment of ulcerative colitis. J Physiol Pharmacol. 2011 Jun;62(3):327-34.
- Sanchez-Barcelo EJ, Mediavilla MD, Tan DX, et al. Clinical uses of melatonin: evaluation of human trials. Curr Med Chem. 2010;17(19):2070-95.
- Todisco M. Effectiveness of a treatment based on melatonin in five patients with systemic sclerosis. Am J Ther. 2006 Jan-Feb;13(1):84-7.
- Forrest CM, Mackay GM, Stoy N, et al. Inflammatory status and kynurenine metabolism in rheumatoid arthritis treated with melatonin. Br J Clin Pharmacol. 2007 Oct;64(4):517-26.
- Huang CC, Chiou CH, Liu SC, et al. Melatonin attenuates TNF-alpha and IL-1beta expression in synovial fibroblasts and diminishes cartilage degradation: Implications for the treatment of rheumatoid arthritis. J Pineal Res. 2019 Apr;66(3):e12560.
- Nah SS, Won HJ, Park HJ, et al. Melatonin inhibits human fibroblast-like synoviocyte proliferation via extracellular signal-regulated protein kinase/P21(CIP1)/P27(KIP1) pathways. J Pineal Res. 2009 Aug;47(1):70-4.
- Rudra DS, Pal U, Maiti NC, et al. Melatonin inhibits matrix metalloproteinase-9 activity by binding to its active site. J Pineal Res. 2013 May;54(4):398-405.
- MacDonald IJ, Huang CC, Liu SC, et al. Reconsidering the Role of Melatonin in Rheumatoid Arthritis. Int J Mol Sci. 2020 Apr 20;21(8).
- Esalatmanesh K, Loghman A, Esalatmanesh R, et al. Effects of melatonin supplementation on disease activity, oxidative stress, inflammatory, and metabolic parameters in patients with rheumatoid arthritis: a randomized double-blind placebo-controlled trial. Clin Rheumatol. 2021 Sep;40(9):3591-7.
- Foley HM, Steel AE. Adverse events associated with oral administration of melatonin: A critical systematic review of clinical evidence. Complement Ther Med. 2019 Feb;42:65-81.
- Naguib M, Samarkandi AH. Premedication with melatonin: a double-blind, placebo-controlled comparison with midazolam. Br J Anaesth. 1999 Jun;82(6):875-80.
- Nordlund JJ, Lerner AB. The effects of oral melatonin on skin color and on the release of pituitary hormones. J Clin Endocrinol Metab. 1977 Oct;45(4):768-74.
- Anton-Tay F, Diaz JL, Fernandez-Guardiola A. On the effect of melatonin upon human brain. Its possible therapeutic implications. Life Sci I. 1971 Aug 1;10(15):841-50.
- Gitto E, Reiter RJ, Cordaro SP, et al. Oxidative and inflammatory parameters in respiratory distress syndrome of preterm newborns: beneficial effects of melatonin. Am J Perinatol. 2004 May;21(4): 209-16.
- Grossman E. Should melatonin be used to lower blood pressure? Hypertens Res. 2013 Aug;36(8):682-3.
- Grossman E, Laudon M, Zisapel N. Effect of melatonin on nocturnal blood pressure: meta-analysis of randomized controlled trials. Vasc Health Risk Manag. 2011;7:577-84.
- Brzezinski A. Melatonin in humans. N Engl J Med. 1997 Jan 16;336(3):186-95.