
Fibrocystic Breast Changes
Fibrocystic Breast Changes
Last Section Update: 06/2015
1 Overview
Summary and Quick Facts for Fibrocystic Breast Changes
- Fibrocystic breast changes are noncancerous lumps or abnormalities in the breast tissue. Between 50% and 90% of women will experience benign changes in their breast tissue during their lifetime, with the 30s and 40s being the most common age of occurrence.
- This protocol describes the signs and symptoms of fibrocystic breast changes and provides information concerning conventional treatment, novel and emerging strategies, diet and lifestyle considerations, and integrative interventions.
- There are several actions women can take on their own that may help ease symptoms caused by fibrocystic breast changes and reduce the incidence of these conditions. If changes in a woman's breast tissue are determined to be benign and do not cause symptoms, then no treatment is necessary.
Fibrocystic breast changes are non-cancerous lumps or abnormalities in the breast tissue. Between 50% and 90% of women will experience benign changes in their breast tissue during their lifetime, with 30s and 40s being the most common age of occurrence.
It is important for women who notice changes in their breast tissue to let their doctor know right away so that breast cancer or another serious disease can be ruled out.
Symptoms of fibrocystic breast changes include:
- Tenderness in both breasts
- Sense of fullness
- Pain that is generally worse before the menstrual period and relieved within a few days of the onset of the menstrual period
- Breast lumps that are tender, can be moved easily, may be present symmetrically in both breasts, and may change in size with the menstrual cycle
- Nipple discharge may occur in up to 15% of women
Natural interventions that can help ease symptoms and reduce incidence include vitamin E, plant lignans, and chasteberry (also known as Vitex agnus-castus).
Risk Factors:
Several risk factors promote fibrocystic breast changes:
- Peak occurrence in 30s and 40s
- Alcohol intake during adolescence and early adulthood
Diagnosis:
Certain tests beyond breast self-exam, clinical exam or mammography may be necessary to distinguish benign breast changes from breast cancer:
- Ultrasound
- Breast biopsy, including fine needle aspiration, core needle biopsy, image-guided biopsy, or surgical biopsy
- Near-infrared imaging with contrast since cancerous breast tissue is more likely to absorb contrast media than benign breast tissue
Conventional Medical Treatments:
Drugs that may address the symptoms of fibrocystic breast changes include:
- Non-steroidal anti-inflammatory drugs (NSAIDs) and acetaminophen
- Medications that influence hormones, including oral contraceptives, cabergoline, tamoxifen, and danazol
- Ormeloxifene, currently used as an oral contraceptive primarily in India
Dietary and Lifestyle Changes:
- Dietary fiber for improved estrogen metabolism
- Increased fruit and vegetable intake; higher citrus fruit consumption was associated with 57% reduced odds, and higher fruit (other than citrus) with 65% reduced odds
- A fiber-rich, plant-based diet high in healthy fats from sources such as olive oil and fish, and low in red meat
Integrative Interventions:
- Chasteberry: Chasteberry, also known as Vitex agnus-castus, is commonly used for breast pain, especially premenstrual breast tenderness.
- Plant lignans: Lignans are compounds present in a variety of plant foods, with high concentrations found in flaxseeds and sesame seeds, as well as in certain plant extracts such as Norway spruce. Women who consumed the most food sources of lignans were 52% less likely to have benign breast changes than those with the lowest consumption of these foods.
- Vitamin E: Vitamin E was shown to be effective in reducing the most severe premenstrual breast pain in a clinical trial.
- Evening primose oil/gamma-linolenic acid (GLA): Evening primrose oil, which contains GLA, was found to reduce the most severe premenstrual breast pain when taken at a daily dose of 3 g for six months.
- Omega-3 fatty acids: Breast pain intensity was reduced by about 42% in women given omega-3 fatty acids after two menstrual cycles, while women who did not receive the omega-3 supplement experienced a reduction of only about 17%.
2 Introduction
Fibrocystic breast changes are non-cancerous (benign) lumps or abnormalities in the breast tissue. Fibrocystic breasts are very common: estimates suggest that between 50% and 90% of all women will experience benign changes in their breast tissue during their lifetime (Jones 2011). In fact, most doctors no longer use the term "fibrocystic breast disease" because the condition typically does not require urgent action (Alvero 2015; Jones 2011; Mayo Clinic 2013a).
Some types of fibrocystic breast changes are associated with a small increase in breast cancer risk, particularly when there is a family history of breast cancer. However, fibrocystic changes are often not associated with an increased risk of breast cancer (Tamimi 2010; Sugg 2014; Guray 2006). Importantly, women who do notice changes in their breast tissue should let their doctor know right away so breast cancer or another serious disease can be ruled out (Jones 2011; Alvero 2015).
Physicians typically use imaging tests followed by biopsy studies to evaluate breast masses for the presence of cancer. If changes in a woman's breast tissue are determined to be benign and do not cause symptoms, then no treatment is necessary. If breast changes cause mild-to-moderate pain or discomfort, then over-the-counter pain relievers such as acetaminophen and nonsteroidal anti-inflammatory drugs (NSAIDs) may help, but these drugs are not without side effects (ACR 2012). For women whose symptoms are more severe, drugs that alter hormonal activity may be used to relieve pain, but these may have side effects (Alvero 2015; Jones 2011; Sugg 2014). Less commonly, symptomatic breast changes may be due to an infection, in which case antibiotics can be used (Jones 2011).
Fortunately, there are several actions women can take on their own that may help ease symptoms caused by fibrocystic breast changes and reduce the incidence of these conditions. For example, increasing intake of dietary fiber is believed to decrease the incidence of benign breast conditions (Jones 2011). Several natural interventions may also be of benefit, including vitamin E, omega-3 fatty acids, plant lignans, and chasteberry (also known as Vitex agnus-castus) (Vaziri 2014; Jones 2011; Altern Med Rev 2009).
Hormonal imbalances are generally thought to underlie fibrocystic breast changes. Specifically, estrogen excess, inadequate progesterone, or abnormal metabolism of these hormones appear to contribute to benign changes in breast tissue (Jones 2011). Given the important role of hormones in fibrocystic breast changes, women are also encouraged to read the Female Hormone Restoration protocol.
3 Background
Structure and Function of the Breast
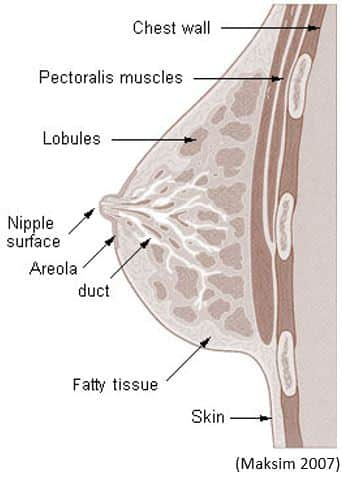 |
Breast tissue is composed of ducts, lobules, ligaments, connective tissue, blood and lymphatic vessels, lymph nodes, nerves, and fat (Mayo Clinic 2015a). Each female breast contains 10–15 ducts that begin within the breast and merge at the nipple. It is through these ducts that milk passes during lactation. For each duct, there is a lobule surrounded by fat cells. The lobule is the milk-producing structure in the breast (Johns Hopkins Medicine 2012; Neville 2014). The breast is supported by ligaments and bands of fibrous tissue that together determine the breast's shape and position (Prendergast 2013).
Breast lobules and ducts react to hormones to produce milk during lactation. The pituitary gland at the base of the brain releases prolactin and oxytocin, which stimulate milk production and release (Nussey 2001). However, breast tissue is also responsive to estrogen and progesterone (Mauvais-Jarvis 1986). All four of these hormones are important for the appropriate timing of lactation, suppressing ovulation during lactation, milk production and expression, and growth and maturation of breasts during development (Clevenger 1997; Jonas 2009; Bellmann 1976; Neville 2009).
Types of Fibrocystic Breast Abnormalities
Benign breast conditions are divided into three categories based on how the tissue extracted during a biopsy looks under a microscope (ie, histologically) (Dupont 1985; Tamimi 2010; Mayo Clinic 2013b; ACS 2015). The categories are:
- Non-proliferative (no increase in cell number or growth)
- Proliferative without atypia (overgrowth of normal-appearing cells lining breast lobules and ducts)
- Atypical hyperplasia (overgrowth of abnormal-appearing cells lining breast lobules and ducts)
These categories indicate risk of the abnormality becoming breast cancer (Schnitt 2003; Hartmann 2005; Dupont 1985; Guray 2006):
- Women with non-proliferative changes generally do not have increased breast cancer risk.
- Women whose benign breast abnormalities are proliferative without atypia have a 1.3- to 2-fold increased risk of breast cancer compared with women who have non-proliferative benign breast disorders.
- Women with atypical hyperplasia have a 4- to 13-fold increased risk of breast cancer compared with women who have non-proliferative changes.
- There are two types of atypical hyperplasia: ductal and lobular.
Table 1: Types of Benign Breast Disease
Category |
Condition |
Breast Cancer Risk |
Non-proliferative |
Simple cyst |
Generally not associated with breast cancer |
Complex cyst |
||
Papillary apocrine changes |
||
Epithelial-related calcifications |
||
Mild hyperplasia of the usual type |
||
Ductal ectasia |
||
Non-sclerosing adenosis |
||
Periductal fibrosis |
||
Proliferative without atypia |
Sclerosing adenosis |
Low (1.3- to 2-fold increased risk) |
Intraductal papilloma |
||
Fibroadenomas |
||
Ductal hyperplasia of the usual type |
||
Adenosis |
||
Radial scar |
||
Papillomatosis |
||
Atypical hyperplasia |
Ductal atypical hyperplasia |
Moderate (4- to 13-fold increased risk) |
Lobular atypical hyperplasia |
Other Breast Abnormalities
A variety of other breast abnormalities may cause signs and symptoms similar to those caused by fibrocystic changes.
Table 2: Other Breast Abnormalities that may Resemble Fibrocystic Changes
Abnormality |
Associated Breast Cancer Risk |
Characteristics |
Lipomas |
None |
Lipomas may be confused with other causes of fibrocystic changes; may require excisional biopsy to confirm the diagnosis. |
Fat Necrosis |
None |
Usually a result of trauma |
Hamartomas |
None |
Uncommon and painless |
Adenomas |
None |
Multiple subtypes with different characteristics |
Mastitis |
None |
May be confused with inflammatory breast cancer |
Apocrine metaplasia |
None |
Common finding in women over age 25 |
Complex fibroadenomas |
Low |
Refers to the presence of multiple types of abnormalities in addition to fibroadenoma |
Phyllodes tumor |
Can refer to both benign and malignant growths |
Rapid rate of growth |
The Cause of Fibrocystic Changes
The precise cause of fibrocystic changes is not known, but hormonal imbalances are strongly implicated as a contributing factor (Alvero 2015; Jones 2011). A relative deficiency of progesterone or excess of estrogen during the luteal phase of the menstrual cycle may lead to fibrocystic changes (Vorherr 1986; Horner 2000; Carbonaro 2012). The luteal phase occurs after ovulation, when an egg is released by an ovary; this phase lasts until the onset of the menstrual period. The luteal phase usually lasts 14 days (UCSF 2015). During the luteal phase, breast tissue may become tender and lumps may increase in size (Cleveland Clinic 2014).
Fibroadenomas, which are a type of fibrocystic change composed of fibrous and glandular tissue, are particularly sensitive to hormonal changes (Yu 2013; Greenberg 1998). In fact, these breast abnormalities can produce milk during pregnancy and they recede beginning in perimenopause as hormone levels decline. Therefore, women may be more likely to experience symptoms caused by a fibroadenoma during pregnancy and lactation (Yu 2013). Also, women who begin oral contraceptives before age 20 have an increased risk of developing fibroadenomas (Yu 1992; Estevao 2007; Guray 2006).
4 Risk Factors
Age
The incidence of benign breast abnormalities peak in women's 30s and 40s (Sugg 2014). This is in contrast to risk of breast cancer, which continues to increase after menopause (Guray 2006).
Alcohol Consumption
Alcohol intake during adolescence and early adulthood increases risk of proliferative benign breast conditions (Liu 2012; Berkey 2010).
Caffeine and Related Compounds
At one time, it was believed that methylxanthines—a class of naturally occurring stimulant molecules that includes caffeine and theobromine, a compound in cacao—aggravated symptoms of fibrocystic breasts, or caused fibrocystic abnormalities to increase in size. However, a rigorous analysis of studies on the subject failed to show a beneficial effect of methylxanthine avoidance on fibrocystic changes (Franco 2013; Horner 2000). Avoidance of methylxanthines is still sometimes recommended, but the benefit for women with fibrocystic changes is uncertain (Jones 2011; Alvero 2015; Sugg 2014).
5 Signs and Symptoms
Breast Pain
Tenderness, fullness, and pain that wax and wane throughout the menstrual cycle are characteristic symptoms of fibrocystic changes. The pain of fibrocystic changes may be experienced as dull, throbbing, or burning. It is often present in both breasts and is usually not localized, and may radiate to the arm or armpit. The pain can range from mild to severe, and when cyclical is generally worse before the menstrual period and relieved within a few days of the onset of menses (Vaidyanathan 2002; Sugg 2014; Jones 2011).
Lumps
Breast lumps are another characteristic sign of fibrocystic changes. The breast lumps associated with fibrocystic changes often become progressively more tender and are usually present symmetrically in both breasts, though they may be felt in one specific location or on only one side. The lumpiness is often felt in the upper outer part of the breast, though this also happens to be a common location of breast cancer tumors. Growth and regression of benign breast lumps are more likely to be cyclical in younger women. When a single mass is prominent it is called a "dominant mass," and will ordinarily require more detailed medical evaluation to rule out other conditions, including cancer (Jones 2011; Sugg 2014; Vaidyanathan 2002).
Benign breast lumps are usually mobile, which means they can be moved about freely. The lumps may also increase in size prior to menstruation. A breast cancer tumor, on the other hand, is usually fixed and immobile because it forms many attachments to the surrounding tissues (Sharma 2010; CGRDU 2005; Sugg 2014).
Nipple Discharge
In benign breast disease, as many as 15% of women have nipple discharge, whereas nipple discharge is present in only 2.5–3.0% of breast cancer cases. Even when nipple discharge is considered suspicious, only 5% of these cases are actually cancer. Nipple discharge associated with fibrocystic changes occurs only when the nipples are compressed and is often present on both sides. Discharge that occurs spontaneously, without compression, is potentially a sign of a serious condition and should be evaluated promptly; the same is true for bloody or watery discharge or discharge that is present in large amounts. Nipple discharge associated with benign breast diseases tend to be present in only small amounts, and can be clear, white, milky, gray, yellow, or even black or dark green. The discharge may come from one or both breasts (Jones 2011; Sugg 2014; Vaidyanathan 2002).
6 Diagnosis
Fibrocystic changes occur in at least half of women and are uncommonly associated with the development of breast cancer. However, the primary importance of diagnosing benign breast disease is to rule out more serious conditions, including breast cancer (Sugg 2014; Alvero 2015; Jones 2011; Vaidyanathan 2002).
Unfortunately, benign breast conditions are often misdiagnosed since each woman’s breast anatomy is different and mammography cannot identify all structures with complete precision. Thus, a woman with a benign breast lump may need other diagnostic procedures potentially including ultrasound, aspiration, and biopsy to exclude malignancy (Amin 2013; Miltenburg 2008; Jones 2011). Thyroid hormone irregularities, particularly hypothyroidism, should also be ruled out in women with fibrocystic breast conditions, as low thyroid function may be related to fibrocystic changes and the progression of breast cancer (Stoddard 2008; Patrick 2008; Smyth 2003).
Manual Breast Examination
A clinical manual breast exam (performed by a doctor) is often an early step in assessing breast symptoms. This exam involves palpating the breasts for lumps, and determining if discharge can be expressed. However, a manual breast examination will rarely be able to detect early-stage breast cancer and cannot be used in isolation to clearly differentiate among different benign breast disorders (Miltenburg 2008; Onstad 2013).
Women may perform breast self-exams to detect changes in their breasts. Fibrocystic breast tissue may feel thick, lumpy, or rope-like in texture, and the lump(s) are mobile and do not feel stuck to surrounding tissue. Lumps caused by fibrocystic breast conditions may become larger before each menstrual period and shrink after the menstrual period is over. Breast pain may occur in both breasts, and this pain may fluctuate throughout the menstrual cycle or remain constant. The most important consideration for women who examine their own breasts is to take note of changes in appearance or texture of breast tissue and to promptly report those changes to their health care provider, who can advise whether additional evaluation is necessary (NLM 2013; Scott-Conner 2015; NBCF 2012; Mayo Clinic 2013a).
Ultrasound
Ultrasound is often the only imaging study used to evaluate breast lumps in younger women. Ultrasound does not expose the patient to radiation. Instead, ultrasound uses sound waves to investigate the anatomy of the breast (Jones 2011; Miltenburg 2008; Gucalp 2014; NLM 2014).
Mammogram
A mammogram is an x-ray–based imaging procedure of the breasts. There are two types of mammogram: screening and diagnostic. Screening mammograms are performed on women with no signs or symptoms of abnormalities, and are meant to detect early-stage breast cancer. Diagnostic mammograms are used in women who have signs and symptoms of breast abnormalities in order to help differentiate cancer from benign conditions such as fibrocystic changes (NCI 2014). As a tool for detecting cancer, mammography is most useful in postmenopausal women. Younger women and those taking hormone replacement therapy often have dense breast tissue, which makes mammogram images less helpful. By themselves, mammograms do not identify all cases of cancer: follow-up of all imaging studies by means of cyst aspiration or biopsy is usually necessary for conclusive diagnosis (Miltenburg 2008; Evans 2002; Jones 2011; Onstad 2013).
One downside of mammograms is they expose women to a small amount of radiation (Jones 2011). Although not appropriate for all women, alternatives to mammography are available. Women interested in reading about breast cancer screening using mammography alternatives can refer to the Life Extension magazine article Breast Cancer Screening Alternatives.
Breast Imaging Reporting and Data System (BI-RADS) Physicians use a system called BI-RADS (Breast Imaging Reporting and Data System) to classify breast abnormalities. The BI-RADS score can provide an estimate of breast cancer risk and also guide further management. The BI-RADS system is applicable to both ultrasound and mammogram (Kim 2008; NCI 2014). The BI-RADS system classifies a breast nodule according to six features (Heinig 2008). Based on these six features, the radiologist provides a BI-RADS score from 0 to 6, with a higher score denoting a higher risk that the mass is cancerous, and a score of 6 indicating biopsy-proven cancer. Table 3: BI-RADS Scoring
|
Breast Biopsy
In women who receive a BI-RADS score of 4 or 5 after mammography or ultrasonography, a breast biopsy is often required (Eberl 2006; Kennedy 2011). There are several forms of breast biopsy available:
Fine needle aspiration. Fine needle aspiration is the least invasive type of breast tissue biopsy (Wesola 2013). In this procedure, the physician inserts a narrow gauge needle into the breast, removing a small sample of cells for analysis. Fine needle aspiration has a very low rate of complications and is associated with minimal discomfort. However, it requires a high degree of expertise on the part of the physician performing the procedure (Ljung 2001; Breastcancer.org 2015; Kaur 2007) and has become less favored than core needle biopsy in many breast cancer centers (Zervoudis 2014).
Core needle biopsy. A core needle biopsy is more invasive than fine needle aspiration and is associated with greater discomfort, though it has a low rate of complications. Some researchers prefer core needle biopsy, and it may be a more reliable method for distinguishing between in situ and invasive breast cancer compared to fine needle aspiration (Zervoudis 2014; Verkooijen 2002). Core needle biopsy is usually the first biopsy procedure used to evaluate breast lumps that cannot be easily palpated manually (Willems 2012; Al-Sobhi 1999; Verkooijen 2002).
Image-guided biopsy. If a mass that needs to be biopsied cannot be easily observed or localized, then the physician performing the biopsy may use imaging techniques to help guide the needle. A biopsy guided by mammography is called a stereotactic biopsy, and ultrasound imaging can be used to perform an ultrasound-guided biopsy (Huang 2014; BreastCancer.org 2015).
Surgical biopsy techniques. In cases where fine needle aspiration or core needle biopsy are inconclusive or provide results that are suspicious for cancer, incisional biopsy or excisional biopsy may be indicated (ACS 2014).
- In incisional biopsy, a physician uses manual instruments to cut through the skin and remove a piece of the suspicious tissue for examination. This procedure may be performed under sedation (BreastCancer.org 2015).
- Excisional biopsy is a surgical procedure performed under local anesthesia in which the entire area of suspicious tissue is removed. This procedure may be performed under sedation (ACS 2014; BreastCancer.org 2015).
7 Conventional Treatment
Acetaminophen and NSAIDs
Acetaminophen or a nonsteroidal anti-inflammatory drug (NSAID) such as ibuprofen or naproxen are often considered first-line treatment for breast pain (Jones 2011; Sugg 2014; Kosir 2013). While these over-the-counter medications are usually effective at temporarily relieving mild-to-moderate breast pain, long-term, chronic use is associated with potentially severe side effects. For example, chronic NSAID use can cause gastrointestinal bleeding (Seager 2001; O'Neil 2012) and can damage the liver and kidney (Bessone 2010; Plantinga 2011).
Topical application of NSAID preparations directly to the breasts has proven effective for relief of both cyclical and non-cyclical breast pain. Importantly, unlike oral NSAIDs or acetaminophen, topical NSAIDs do not carry systemic risks to the gastrointestinal tract, liver, or kidneys (Qureshi 2005; Colak 2003; Kataria 2014). Professional medical societies have recommended topical NSAIDs for the treatment of breast pain (mastalgia), and some sources consider topical NSAIDs first-line treatment for mastalgia (Olawaiye 2005; Sugg 2014). Localized skin reactions are possible with topical NSAIDs (Klinge 2013).
Hormone-Related Treatments
For persistent, severe breast pain, medications that influence hormones may be recommended (Sugg 2014).
Oral contraceptives. Combined oral contraceptives (estrogen and progesterone) are sometimes recommended to help reduce symptoms of fibrocystic breasts, and are believed to work by supplying controlled amounts of estrogen and progesterone (Jones 2011). However, clinical trials of combined oral contraceptives for fibrocystic breast changes have yielded mixed results (Leonardi 1997; Carbonaro 2012).
Cabergoline. Cabergoline (Dostinex) is a drug that activates certain receptors for the neurotransmitter dopamine in the brain. One effect of this medication is the suppression of prolactin production in the pituitary gland (NIH 2012). Studies have shown that cabergoline helps reduce breast pain and other symptoms associated with fibrocystic breast changes (Aydin 2010; Castillo-Huerta 2013). It is not entirely clear why reducing prolactin levels helps treat fibrocystic changes, though sex hormone influence on the action of the pituitary gland may contribute (Srivastava 2007; Peters 1984). Another drug that functions similarly to cabergoline is called bromocriptine (Parlodel, Cycloset). Although there is some evidence that bromocriptine might help reduce symptoms caused by fibrocystic changes, cabergoline has been shown to perform better and cause fewer side effects in some studies (Aydin 2010; Castillo-Huerta 2013). Nevertheless, both of these drugs can cause serious side effects, such as intense nausea and neurological, psychological, and vascular problems (Mayo Clinic 2015b; Jones 2011; Onstad 2013).
Tamoxifen. When fibrocystic changes result in severe and chronic pain, physicians may prescribe a powerful drug called tamoxifen (Nolvadex, Soltamox) (Srivastava 2007; Jones 2011). Tamoxifen is best known as a treatment used in conjunction with chemotherapy for certain breast cancers. The usage of tamoxifen for breast pain is considered off label and should be supervised by a specialist (EBCTCG 2005; Jones 2011). Tamoxifen is effective for treatment of fibrocystic changes but has a significant side effect profile and is not often prescribed for this condition (Vaidyanathan 2002; Onstad 2013; Alvero 2015).
Danazol. Danazol (Danocrine) is currently the only drug approved by the Food and Drug Administration (FDA) for the treatment of breast pain, and in this capacity is used at a low dose, continuously for 3–6 months (Jones 2011). Danazol acts upon the pituitary gland in a way that suppresses estrogen and progesterone, and favors a masculine hormonal pattern (Beaumont 2002; NLM 2015). Sources differ regarding the effectiveness of danazol, but are in agreement that its serious side effect profile often makes it poorly tolerated (Alvero 2015; Onstad 2013; Goyal 2011). Among danazol’s side effects are masculinization symptoms (deepening of the voice, acne, abnormal hair growth patterns), vision problems, liver and lung problems, joint pain, irregular periods, and heart attack (NHS 2015).
8 Novel and Emerging Strategies
Ormeloxifene (Centchroman)
Ormeloxifene, also known as centchroman, belongs to a class of drugs known as selective estrogen receptor modulators (SERMs). Ormeloxifene is a nonsteroidal compound that is manufactured and currently available in India as an oral contraceptive; some research on the drug is ongoing in the United States (de Barros 2015). A paper published in 2015 reported on a trial that compared ormeloxifene to tamoxifen for the treatment of breast pain. The effectiveness of the two medications after 12 weeks was similar, though side effects such as dizziness, menstrual irregularities and development of ovarian cysts were greater in the ormeloxifene group (Jain 2015). A three-month randomized controlled trial in 121 women aged 20–50 compared 30 mg ormeloxifene twice per week to placebo for the treatment of breast pain and lumps. Compared with placebo, both breast pain and breast lumps were significantly reduced by ormeloxifene treatment (Kumar 2013).
In another trial ormeloxifene significantly reduced breast pain to a greater degree than danazol; nearly 90% of women had relief in the ormeloxifene group, while 69% taking danazol experienced pain relief (Tejwani 2011). In another study, 86% of women taking ormeloxifene for 24 weeks had complete resolution of breast pain (Sharma 2012).
As some researchers have expressed concern with ormeloxifene’s side-effect profile (Jain 2015), women interested in this drug should consult closely with their health care provider to weigh the risks and benefits.
Near-Infrared Imaging with Contrast
The primary concern in the assessment of breast symptoms is to correctly differentiate between benign breast changes and serious breast diseases such as breast cancer. An experimental procedure, near-infrared imaging with the use of contrast, has shown an ability to increase diagnostic accuracy when combined with mammography and ultrasound. Multiple studies have shown that cancerous breast tissue tends to absorb more contrast media than benign tissue. This difference can be detected using a scanner that detects near-infrared energy. Preliminary evidence is promising, but this innovative diagnostic approach is still in development. Like other imaging methods, this approach is minimally invasive, though the contrast material must be injected into a vein (Hawrysz 2000; Poellinger 2012). More research is needed to determine the true utility of near-infrared imaging in detecting fibrocystic changes and differentiating them from breast cancer.
9 Dietary and Lifestyle Considerations
Dietary factors appear to play an important role in the development of both benign fibrocystic changes and breast cancer, and specific components of a healthy diet may significantly reduce the risk of developing fibrocystic changes and benign breast disease (Frazier 2013; Baer 2003; Berkey 2013; Su 2010). For instance, dietary fiber improves estrogen metabolism, and diets high in fiber have been associated with reduced incidence of some benign breast disorders (Jones 2011).
A study in 675 women with benign breast conditions, compared to 1070 healthy controls, found that greater consumption of fruits and vegetables decreased the risk of proliferative fibrocystic breast conditions and breast cancer. This effect was most clear when comparing the one-quarter of women with proliferative breast conditions or breast cancer who ate the most fruits and vegetables to controls (Li 2005). A similar finding on the importance of diet came from a study that compared 121 women with benign breast disease to 121 women with non-breast related conditions. This study found that several dietary components were associated with significantly reduced odds of benign breast disease. Higher citrus fruit consumption was associated with 57% reduced odds, and higher non-citrus fruit with 65% reduced odds (Galvan-Portillo 2002).
Several studies have shown that women who consume more vegetable fats, vegetable protein, fiber, and nuts, and less animal fat, red meat, and alcohol are less likely to develop fibrocystic and benign breast changes later in life. Studies have yet to determine if adult women who adopt this dietary approach are at reduced risk of fibrocystic changes, but this strategy, as reflected in a Mediterranean dietary pattern, has been shown to reduce breast cancer risk in adult women. Thus, a fiber-rich, plant-based diet high in healthy fats from sources such as olive oil and fish, and low in red meat, is a reasonable preventive strategy (Frazier 2013; Baer 2003; Berkey 2012; Berkey 2013; Su 2010; Kakkoura 2015; Castello 2014; de Lorgeril 2014; Escrich 2011).
10 Nutrients
Chasteberry (Vitex agnus-castus)
Chasteberry, also known as Vitex agnus-castus, is commonly used for breast pain in Europe (van Die 2013), and the German Commission E (a regulatory body that oversees dietary supplements in Germany) supports the use of Vitex agnus-castus for the treatment of breast tenderness, especially premenstrually (Altern Med Rev 2009).
In a randomized controlled trial in 97 women with cyclical breast pain, daily dosing with a solution containing about 32.4 mg of chasteberry extract significantly reduced breast pain compared with placebo. The improvement was observed over two menstrual cycles, and half of the patients receiving chasteberry extract reported that they were free from severe pain after the second treatment cycle, with some women reporting that pain relief was noticeable beginning with the first cycle (Halaska 1999). Chasteberry is believed to exert its effect through inhibition of excessive release of the hormone prolactin by means of activity at dopamine receptors in the pituitary gland (Carmichael 2008; Wuttke 2003). This mechanism of action is similar to that of the drug bromocriptine. According to a rigorous review of the literature, chasteberry benefits other conditions influenced by hormonal fluctuations, including premenstrual syndrome, and menstrual cycle irregularities (van Die 2013; Altern Med Rev 2009).
A randomized trial compared chasteberry extract and bromocriptine in the treatment of 40 women with cyclical breast pain and 40 women with mildly elevated prolactin secretion. Prolactin secretion and breast pain were significantly reduced by both treatments. The authors pointed out that the necessity of long-term treatment of breast pain makes tolerability and low toxicity a priority, so patients are more likely to adhere to treatment with chasteberry extract (Kilicdag 2004).
Lignans, Flaxseed, and Enterolactones
Lignans are polyphenolic compounds present in a variety of plant foods, with high concentrations found in flaxseeds and sesame seeds, as well as in certain plant extracts such as Norway spruce (Pandey 2009; Willför 2003; Liu 2006). Plant lignans are converted by intestinal bacteria to the biologically active “mammalian lignans” such as enterolactone (Lampe 2003; Liu 2006; Higdon 2010). Enterolactones have been shown to concentrate in breast cyst tissue and potentially mitigate breast cancer risk in certain patients (Boccardo 2003). Both lignans and enterolactones have been studied in pre-clinical settings and observational studies, and found to have substantial anticancer activity. This quality is particularly evident in protection from breast cancer abnormalities, and in an association with reduced breast cancer risk (Fabian 2010; Thompson 1996; Guglielmini 2012; Suzuki 2008; Boccardo 2004).
Enterolactones appear to have aromatase-inhibiting activity (Adlercreutz 1993; Lu 2012). Aromatase is the enzyme responsible for creating estrogen from precursor compounds (Bulun 2005). This property could account for the ability of enterolactones to protect against breast cancer and benign breast changes (Su 2010). Tamoxifen is one of the few drugs used to treat fibrocystic changes and severe breast pain, but is associated with significant side effects. Since fibrocystic changes are known to be closely associated with female sex steroids, and possibly with estrogen excess, dietary and supplemental lignans may be one of the more promising approaches to managing benign breast changes (Sugg 2014; Jones 2011; Vaziri 2014).
A population-based study compared the diets of 121 women with benign breast disease and 121 control women. Women who consumed the most food sources of lignans were 52% less likely to have benign breast changes than those with the lowest consumption of these foods (Galvan-Portillo 2002).
In a randomized controlled trial, 56 women with severe cyclical breast pain were given a 25 g flaxseed-containing muffin daily, while 60 women received a placebo muffin. The treatment phase of the trial lasted three months, during which the women assessed breast pain, swelling and lumpiness each cycle, as well as daily breast pain. Median reduction of pain score was significantly greater in the flaxseed group compared to placebo at the end of three cycles. There were no significant side effects. Lignans measured in urine increased in the flaxseed group (Goss 2000).
A randomized trial in 181 women with cyclical breast pain assigned participants to receive either 30 g flaxseed per day in specially prepared bread; plain bread without flaxseed; or a capsule containing a modest amount of the omega-3 fatty acids eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA). The intervention lasted for two menstrual cycles. The severity of breast pain was significantly reduced by about 56% in the flaxseed group, 17% in the plain bread group, and about 42% in the omega-3 group (Vaziri 2014).
Two professional organizations endorse flaxseed consumption for the treatment of benign breast conditions. The Society of Obstetricians and Gynecologists of Canada recommends flaxseed as first-line treatment for cyclical breast pain (Rosolowich 2006), and the Canadian Cancer Society recommends consumption of flaxseed for fibrocystic breast changes (CCS 2015).
Vitamin E
Vitamin E was shown to be effective in reducing the most severe premenstrual breast pain, and showed a trend towards overall reduction of cyclical breast pain, in a trial that compared vitamin E, evening primrose oil, a combination of the two, and placebo (Pruthi 2010). Another study compared women with existing proliferative abnormalities to women with non-proliferative conditions or women who did not require a breast biopsy. This study found that women with the highest serum concentration of alpha- and gamma-tocopherol, two forms of vitamin E, showed a trend towards lower risk of both proliferative disease without atypia and breast cancer. Women with the highest consumption of vitamin E from food had a significantly lower risk of breast cancer, and a similar trend was present for those with the highest consumption of vitamin E from both supplements and food (London 1992). A dietary study among girls found that those who consumed the most vitamin E during adolescence had a significant 21% lower risk of proliferative benign changes as adults compared with those who consumed the least vitamin E (Baer 2003).
Evening Primrose Oil and Gamma-Linolenic Acid
Evening primrose oil may relieve breast pain (Vaidyanathan 2002; Kosir 2013). Gamma-linolenic acid (GLA), which is believed to be the active constituent of evening primrose oil, may also be useful in this context (Sugg 2014). It is important to note that up to four months of treatment with evening primrose oil may be necessary for breast pain relief (Onstad 2013).
A randomized controlled trial compared six months of 3 g evening primrose oil, 1200 IU vitamin E, a combination of the two, or placebo each day in 41 women with premenstrual breast pain. All three treatments reduced the most severe pain, with the clearest effect for evening primrose oil alone; there was a trend for all three treatments to reduce the incidence of cyclical breast pain (Pruthi 2010).
Iodine
Iodine may be necessary for normal function of breast tissue, and iodine deficiency has been shown, in preclinical and clinical trials, to be related to precancerous and cancerous changes in breast tissue (Eskin 1977; Patrick 2008). In rodents, dietary restriction of iodine creates a syndrome very similar to fibrocystic changes (Krouse 1979), and in another study, supplementing rodents with iodine was shown to suppress breast tumor growth (Funahashi 1996). Lower incidence of benign breast disease occurs in Japanese women, and some researchers hypothesize that this may be related to greater iodine intake in this population, via consumption of seaweed (Cann 2000).
A review of three clinical studies found that treating women who had fibrocystic breast changes with iodide or iodine led to clinical improvement in about 70% of cases. Side effects of iodine treatment, which included changes in thyroid hormone levels, acne, headaches, thinning hair, and others, occurred in about 11% of subjects in one of the studies (Ghent 1993).
Omega-3 Fatty Acids
Supplementation with the beneficial omega-3 fatty acids eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA) may effectively reduce cyclical breast pain and lower the risk of fibrocystic breast changes.
A randomized trial gave one group of women with cyclical breast pain a daily omega-3 supplement containing 180 mg EPA and 120 mg DHA. In this group, pain intensity was significantly reduced by about 42% after two cycles among women who received the omega-3 supplement, while women who did not receive the omega-3 supplement experienced a reduction of only about 17% (Vaziri 2014).
In another study, women with the highest EPA concentration in their red blood cells had a 62% lower risk of developing fibroadenoma compared with women with the lowest EPA concentrations (Dijkstra 2010). Similar research found that women with the highest red blood cell EPA concentration had a 67% lower risk of non-proliferative fibrocystic changes than women with the lowest red blood cell omega-3 concentrations (Shannon 2009).
Vitamin D
Vitamin D deficiency is strongly linked to breast cancer risk and may be associated with fibrocystic changes. A study that compared vitamin D levels in women with no breast lumps, fibrocystic changes, or breast cancer found that severe vitamin D deficiency (blood levels of less than 12.5 ng/mL) increased the risk for breast cancer by threefold. Importantly, women with fibrocystic changes had vitamin D levels higher than women with breast cancer but lower than healthy controls (Alipour 2014). One trial found that women who consumed more than 533 IU vitamin D per day from diet and supplements showed a trend towards lower incidence of proliferative benign breast changes (Rohan 2008). A survey in 682 women with proliferative breast changes found that those in the highest one-fifth of vitamin D intake during adolescence had a 21% lower risk of proliferative benign changes compared with women whose intake was in the lowest one-fifth as adolescents (Su 2012).
Indole-3-Carbinol and Diindolylmethane
Indole-3-carbinol (I3C) and diindolylmethane (DIM) are related molecules found in cabbage family vegetables such as broccoli, kale, and cauliflower. I3C is metabolized in the body to form DIM, a biologically active compound. I3C and DIM can modulate estrogen receptor activation and estrogen metabolism, properties that may help counter the known role of estrogen excess in fibrocystic changes (Weng 2008; Higdon 2008). Neither I3C nor DIM have been studied in clinical settings in the treatment or prevention of fibrocystic changes; however, rats treated with dietary I3C showed a reduction in the incidence of fibroadenomas (Kojima 1994). More studies are needed before conclusions can be reached about the role of I3C and DIM in the treatment of fibrocystic changes (Weng 2008).
Resveratrol
A study in which higher consumption of fruits and vegetables significantly decreased the risk of proliferative fibrocystic breast conditions and breast cancer also found that higher consumption of grapes was especially associated with a lower risk of proliferative fibrocystic breast conditions and breast cancer. The authors of this study pointed out that resveratrol, a natural polyphenolic compound present in grapes and related foods, has powerful anticancer effects (Li 2005; Vang 2011).
Disclaimer and Safety Information
This information (and any accompanying material) is not intended to replace the attention or advice of a physician or other qualified health care professional. Anyone who wishes to embark on any dietary, drug, exercise, or other lifestyle change intended to prevent or treat a specific disease or condition should first consult with and seek clearance from a physician or other qualified health care professional. Pregnant women in particular should seek the advice of a physician before using any protocol listed on this website. The protocols described on this website are for adults only, unless otherwise specified. Product labels may contain important safety information and the most recent product information provided by the product manufacturers should be carefully reviewed prior to use to verify the dose, administration, and contraindications. National, state, and local laws may vary regarding the use and application of many of the therapies discussed. The reader assumes the risk of any injuries. The authors and publishers, their affiliates and assigns are not liable for any injury and/or damage to persons arising from this protocol and expressly disclaim responsibility for any adverse effects resulting from the use of the information contained herein.
The protocols raise many issues that are subject to change as new data emerge. None of our suggested protocol regimens can guarantee health benefits. Life Extension has not performed independent verification of the data contained in the referenced materials, and expressly disclaims responsibility for any error in the literature.
ACR. American College of Rheumatology. NSAIDs: Nonsteroidal Anti-inflammatory Drugs. Available at: http://www.rheumatology.org/practice/clinical/patients/medications/nsaids.asp. Last updated 8/2012. Accessed 3/6/2015.
ACS. American Cancer Society. Ductal or lobular hyperplasia. Available at: http://www.cancer.org/healthy/findcancerearly/womenshealth/non-cancerousbreastconditions/non-cancerous-breast-conditions-hyperplasia . Last updated 5/1/2015. Accessed 5/4/2015.
ACS. American Cancer Society. Types of biopsy procedures. http://www.cancer.org/treatment/understandingyourdiagnosis/examsandtestdescriptions/forwomenfacingabreastbiopsy/breast-biopsy-biopsy-types. Last updated 7/21/2014 . Accessed 12/19/2014.
Adlercreutz H, Bannwart C, Wähälä K, Mäkelä T, Brunow G, Hase T, ... Vickery LE. Inhibition of human aromatase by mammalian lignans and isoflavonoid phytoestrogens. The Journal of steroid biochemistry and molecular biology. 2// 1993;44(2):147-153.
Alipour S, Hadji M, Hosseini L, Omranipour R, Saberi A, Seifollahi A, ... Shirzad N. Levels of serum 25-hydroxy-vitamin d in benign and malignant breast masses. Asian Pacific journal of cancer prevention : APJCP. 2014;15(1):129-132.
Al-Sobhi SS, Helvie MA, Pass HA, Chang AE. Extent of lumpectomy for breast cancer after diagnosis by stereotactic core versus wire localization biopsy. Annals of surgical oncology. Jun 1999;6(4):330-335.
Altern Med Rev. Vitex agnus-castus. Monograph. Alternative medicine review : a journal of clinical therapeutic. Mar 2009;14(1):67-71.
Alvero R. Ferri's Clinical Advisor. Fibrocystic Breast Disease. Available at: www.clinicalkey.com. Copyight 2015 by Mosby, an imprint of Elsevier, Inc. Accessed 10/14/2014.
Amin AL, Purdy AC, Mattingly JD, Kong AL, Termuhlen PM. Benign breast disease. The Surgical clinics of North America. Apr 2013;93(2):299-308.
Aydin Y, Atis A, Kaleli S, Uludag S, Goker N. Cabergoline versus bromocriptine for symptomatic treatment of premenstrual mastalgia: a randomised, open-label study. European journal of obstetrics, gynecology, and reproductive biology. Jun 2010;150(2):203-206.
Baer HJ, Schnitt SJ, Connolly JL, Byrne C, Cho E, Willett WC, Colditz GA. Adolescent diet and incidence of proliferative benign breast disease. Cancer epidemiology, biomarkers & prevention : a publication of the American Association for Cancer Research, cosponsored by the American Society of Preventive Oncology. Nov 2003;12(11 Pt 1):1159-1167.
Beaumont H, Augood C, Duckitt K, Lethaby A. Danazol for heavy menstrual bleeding. The Cochrane database of systematic reviews. 2002(2):Cd001017.
Bellmann O. [Hormonal regulation of lactation (author's transl)]. Klinische Padiatrie. Sep 1976;188(5):385-395.
Berkey CS, Tamimi RM, Rosner B, Frazier AL, Colditz GA. Young women with family history of breast cancer and their risk factors for benign breast disease. Cancer. Jun 1 2012;118(11):2796-2803.
Berkey CS, Willett WC, Frazier AL, Rosner B, Tamimi RM, Rockett HR, Colditz GA. Prospective study of adolescent alcohol consumption and risk of benign breast disease in young women. Pediatrics. May 2010;125(5):e1081-1087.
Berkey CS, Willett WC, Tamimi RM, Rosner B, Frazier AL, Colditz GA. Vegetable protein and vegetable fat intakes in pre-adolescent and adolescent girls, and risk for benign breast disease in young women. Breast cancer research and treatment. 2013;141(2):299-306.
Bessone F. Non-steroidal anti-inflammatory drugs: What is the actual risk of liver damage? World J Gastroenterol. 2010;16(45):5651-61.
Boccardo F, Lunardi G, Guglielmini P, Parodi M, Murialdo R, Schettini G, Rubagotti A. Serum enterolactone levels and the risk of breast cancer in women with palpable cysts. European journal of cancer (Oxford, England : 1990). Jan 2004;40(1):84-89.
Boccardo F, Lunardi GL, Petti AR, Rubagotti A. Enterolactone in breast cyst fluid: correlation with EGF and breast cancer risk. Breast cancer research and treatment. May 2003;79(1):17-23.
BreastCancer.org. Symptoms & Diagnosis page. Biopsy. Available at: http://www.breastcancer.org/symptoms/testing/types/biopsy. Last updated 1/14/2015. Accessed 2/18/2015.
Bulun SE, Lin Z, Imir G, Amin S, Demura M, Yilmaz B, ... Deb S. Regulation of Aromatase Expression in Estrogen-Responsive Breast and Uterine Disease: From Bench to Treatment. Pharmacological Reviews. September 1, 2005 2005;57(3):359-383.
Cann SA, van Netten JP, van Netten C. Hypothesis: iodine, selenium and the development of breast cancer. Cancer causes & control : CCC. Feb 2000;11(2):121-127.
Carbonaro A, Ciotta L, Stracquadanio M, Formuso C, Giunta M, Agati A, ... Chammas F. Oral contraception and benign breast diseases. American Journal of Nursing. 2012;1(1):1-4.
Carmichael AR. Can Vitex Agnus Castus be Used for the Treatment of Mastalgia? What is the Current Evidence? Evidence-based complementary and alternative medicine : eCAM. Sep 2008;5(3):247-250.
Castello A, Pollan M, Buijsse B, Ruiz A, Casas AM, Baena-Canada JM, ... Martin M. Spanish Mediterranean diet and other dietary patterns and breast cancer risk: case-control EpiGEICAM study. British journal of cancer. Sep 23 2014;111(7):1454-1462.
Castillo-Huerta E, Garibay-Valencia M, Mirabent-Gonzalez F. [Clinical comparision of alpha dihydroergocryptine against cabergoline in the treatment of the fibrocystic mastopathy]. Ginecologia y obstetricia de Mexico. Jul 2013;81(7):370-376.
CCS. Canadian Cancer Society. Cancer Information page. Breast cancer: Fibrocystic breast changes. Available at: http://www.cancer.ca/en/cancer-information/cancer-type/breast/breast-cancer/benign-conditions/fibrocystic-changes/?region=on . Accessed 2/19/2015.
CGRDU. Clinical Governance Research and Development Unit. NICE Clinical Guidelines, No. 27. Referral Guidelines for Suspected Cancer in Adults and Children. Section 12: Breast Cancer. London: Royal College of General Practiioners (UK). 2005. <http://www.ncbi.nlm.nih.gov/books/NBK45764/>.
Cleveland Clinic. Understanding Benign Breast Disease. 2014. Available at: http://my.clevelandclinic.org/health/diseases_conditions/hic_Breast_Cancer_An_Overview/hic_The_Diagnosis_is_Breast_Cancer/hic_Understanding_Benign_Breast_Disease
Clevenger CV, Plank TL. Prolactin as an autocrine/paracrine factor in breast tissue. Journal of mammary gland biology and neoplasia. Jan 1997;2(1):59-68.
Colak T, Ipek T, Kanik A, Ogetman Z, Aydin S. Efficacy of topical nonsteroidal antiinflammatory drugs in mastalgia treatment. Journal of the American College of Surgeons. Apr 2003;196(4):525-530.
de Barros A. UTHSC Professor Receives Grant To Study Ormeloxifene As Prostate Cancer Treatment. Prostate Cancer News Today webpage. Available at: http://prostatecancernewstoday.com/2014/11/19/uthsc-professor-receives-grant-study-ormeloxifene-prostate-cancer-treatment/ . Accessed 5/14/2015.
de Lorgeril M, Salen P. Do statins increase and Mediterranean diet decrease the risk of breast cancer? BMC medicine. 2014;12:94.
Dijkstra SC, Lampe JW, Ray RM, Brown R, Wu C, Li W, ... Thomas DB. Biomarkers of dietary exposure are associated with lower risk of breast fibroadenomas in Chinese women. The Journal of nutrition. Jul 2010;140(7):1302-1310.
Dupont WD, Page DL. Risk factors for breast cancer in women with proliferative breast disease. The New England journal of medicine. Jan 17 1985;312(3):146-151.
EBCTCG (Early Breast Cancer Trialists’ Collaborative Group). Effects of chemotherapy and hormonal therapy for early breast cancer on recurrence and 15-year survival: an overview of the randomised trials. Lancet. 2005;365(9472):1687-1717.
Eberl MM, Fox CH, Edge SB, Carter CA, Mahoney MC. BI-RADS classification for management of abnormal mammograms. Journal of the American Board of Family Medicine : JABFM. Mar-Apr 2006;19(2):161-164.
Escrich E, Moral R, Solanas M. Olive oil, an essential component of the Mediterranean diet, and breast cancer. Public health nutrition. Dec 2011;14(12a):2323-2332.
Eskin BA. Iodine and mammary cancer. Advances in experimental medicine and biology. 1977;91:293-304.
Estevao RA, Nazario AC, Baracat EC. Effect of oral contraceptive with and without associated estriol on ultrasound measurements of breast fibroadenoma: randomized clinical trial. Sao Paulo medical journal = Revista paulista de medicina. Sep 6 2007;125(5):275-280.
Evans A. Hormone replacement therapy and mammographic screening. Clinical radiology. Jul 2002;57(7):563-564.
Fabian CJ, Kimler BF, Zalles CM, Klemp JR, Petroff BK, Khan QJ, ... Johnson KA. Reduction in Ki-67 in benign breast tissue of high-risk women with the lignan secoisolariciresinol diglycoside. Cancer prevention research (Philadelphia, Pa.). Oct 2010;3(10):1342-1350.
Franco R, Onatibia-Astibia A, Martinez-Pinilla E. Health benefits of methylxanthines in cacao and chocolate. Nutrients. Oct 2013;5(10):4159-4173.
Frazier AL, Rosenberg SM. Preadolescent and adolescent risk factors for benign breast disease. The Journal of adolescent health : official publication of the Society for Adolescent Medicine. May 2013;52(5 Suppl):S36-40.
Funahashi H, Imai T, Tanaka Y, Tobinaga J, Wada M, Morita T, ... Takagi H. Suppressive effect of iodine on DMBA-induced breast tumor growth in the rat. Journal of surgical oncology. Mar 1996;61(3):209-213.
Galvan-Portillo M, Torres-Sanchez L, Lopez-Carrillo L. Dietary and reproductive factors associated with benign breast disease in Mexican women. Nutrition and cancer. 2002;43(2):133-140.
Ghent WR, Eskin BA, Low DA, Hill LP. Iodine replacement in fibrocystic disease of the breast. Canadian journal of surgery. Journal canadien de chirurgie. Oct 1993;36(5):453-460.
Goss P, Li T, Theriault M, Pinto S, Thompson L. Effects of dietary flaxseed in women with cyclical mastalgia. Breast Cancer Research and Treatment; 2000.
Goyal A. Breast pain. Clin Evid (Online). 2011;2011.
Greenberg R, Skornick Y, Kaplan O. Management of breast fibroadenomas. Journal of general internal medicine. Sep 1998;13(9):640-645.
Gucalp A, Gupta GP, Pilewskie ML, Sutton EJ, Norton L. Advances in managing breast cancer: a clinical update. F1000prime reports. 2014;6:66.
Guglielmini P, Rubagotti A, Boccardo F. Serum enterolactone levels and mortality outcome in women with early breast cancer: a retrospective cohort study. Breast cancer research and treatment. Apr 2012;132(2):661-668.
Guray M, Sahin AA. Benign breast diseases: classification, diagnosis, and management. The oncologist. May 2006;11(5):435-449.
Halaska M, Beles P, Gorkow C, Sieder C. Treatment of cyclical mastalgia with a solution containing a Vitex agnus castus extract: results of a placebo-controlled double-blind study. Breast (Edinburgh, Scotland). Aug 1999;8(4):175-181.
Hartmann LC, Sellers TA, Frost MH, Lingle WL, Degnim AC, Ghosh K, ... Visscher DW. Benign breast disease and the risk of breast cancer. The New England journal of medicine. Jul 21 2005;353(3):229-237.
Hawrysz DJ, Sevick-Muraca EM. Developments toward diagnostic breast cancer imaging using near-infrared optical measurements and fluorescent contrast agents. Neoplasia (New York, N.Y.). Sep-Oct 2000;2(5):388-417.
Heinig J, Witteler R, Schmitz R, Kiesel L, Steinhard J. Accuracy of classification of breast ultrasound findings based on criteria used for BI-RADS. Ultrasound in obstetrics & gynecology : the official journal of the International Society of Ultrasound in Obstetrics and Gynecology. Sep 2008;32(4):573-578.
Higdon J, Drake V, Williams D. Oregon State University: Data on file. Accessed 6/12/2015.
Higdon J, Drake VJ, Lampe JW. Oregon State University: Data on file.
Horner NK, Lampe JW. Potential mechanisms of diet therapy for fibrocystic breast conditions show inadequate evidence of effectiveness. Journal of the American Dietetic Association. Nov 2000;100(11):1368-1380.
Huang ML, Adrada BE, Candelaria R, Thames D, Dawson D, Yang WT. Stereotactic breast biopsy: pitfalls and pearls. Techniques in vascular and interventional radiology. Mar 2014;17(1):32-39.
Jain BK, Bansal A, Choudhary D, Garg PK, Mohanty D. Centchroman vs tamoxifen for regression of mastalgia: A randomized controlled trial. International journal of surgery (London, England). Mar 2015;15:11-16.
Johns Hopkins Medicine. Anatomy and Physiology of the Breast. 2012; http://pathology.jhu.edu/breast/anatomy.php.
Jonas K, Johansson LM, Nissen E, Ejdeback M, Ransjo-Arvidson AB, Uvnas-Moberg K. Effects of intrapartum oxytocin administration and epidural analgesia on the concentration of plasma oxytocin and prolactin, in response to suckling during the second day postpartum. Breastfeeding medicine : the official journal of the Academy of Breastfeeding Medicine. Jun 2009;4(2):71-82.
Jones R, Scherger JE, Murray JL, Danasas GT, deMarco BJ. First Consult. Fibrocystic breast changes. Available at: www.clinicalkey.com. Last updated 3/13/2011. Accessed 10/14/2014.
Kakkoura MG, Demetriou CA, Loizidou MA, Loucaides G, Neophytou I, Marcou Y, ... Kyriacou K. Single-nucleotide polymorphisms in one-carbon metabolism genes, Mediterranean diet and breast cancer risk: a case-control study in the Greek-Cypriot female population. Genes & nutrition. Mar 2015;10(2):453.
Kataria K, Dhar A, Srivastava A, Kumar S, Goyal A. A systematic review of current understanding and management of mastalgia. The Indian journal of surgery. Jun 2014;76(3):217-222.
Kaur G, Sivakumar S. Comparison of unsatisfactory aspirates in fine needle aspiration performed by surgical medical officers and pathologists. Journal of Cytology. 2007;24(2):82-84.
Kennedy G, Markert M, Alexander JR, Avisar E. Predictive value of BI-RADS classification for breast imaging in women under age 50. Breast cancer research and treatment. Dec 2011;130(3):819-823.
Kilicdag E, Tarim E, Bagis T, Erkanli S, Aslan E, Ozsahin K, Kuscu E. Fructus agni casti and bromocriptine for treatment of hyperprolactinemia and mastalgia. International Journal of Gynecology & Obstetrics. 2004;85(3):292-293.
Kim EK, Ko KH, Oh KK, Kwak JY, You JK, Kim MJ, Park BW. Clinical application of the BI-RADS final assessment to breast sonography in conjunction with mammography. AJR. American journal of roentgenology. May 2008;190(5):1209-1215.
Klinge SA, Sawyer GA. Effectiveness and safety of topical versus oral nonsteroidal anti-inflammatory drugs: a comprehensive review. The Physician and sportsmedicine. May 2013;41(2):64-74.
Kojima T, Tanaka T, Mori H. Chemoprevention of spontaneous endometrial cancer in female Donryu rats by dietary indole-3-carbinol. Cancer research. Mar 15 1994;54(6):1446-1449.
Kosir MA. The Merck Manual Professional Edition. Breast Disorders. Mastalgia (Breast Pain). Available at: http://www.merckmanuals.com/professional/gynecology_and_obstetrics/breast_disorders/mastalgia_breast_pain.html. Last updated 9/2013. Accessed 3/17/2015.
Krouse TB, Eskin BA, Mobini J. Age-related changes resembling fibrocystic disease in iodine-blocked rat breasts. Archives of pathology & laboratory medicine. Nov 1979;103(12):631-634.
Kumar S, Rai R, Agarwal GG, Dwivedi V, Kumar S, Das V. A randomized, double-blind, placebo-controlled trial of ormeloxifene in breast pain and nodularity. The National medical journal of India. Mar-Apr 2013;26(2):69-74.
Lampe JW. Isoflavonoid and lignan phytoestrogens as dietary biomarkers. The Journal of nutrition. Mar 2003;133 Suppl 3:956s-964s.
Lanng C, Eriksen BO, Hoffmann J. Lipoma of the breast: a diagnostic dilemma. Breast (Edinburgh, Scotland). Oct 2004;13(5):408-411.
Leonardi M. [Hormonal contraception and benign breast disease. Evaluation of a treatment protocol for chronic mastopathy with mastalgia]. Minerva ginecologica. Jun 1997;49(6):271-276.
Li W, Ray RM, Lampe JW, Lin MG, Gao DL, Wu C, ... Thomas DB. Dietary and other risk factors in women having fibrocystic breast conditions with and without concurrent breast cancer: a nested case-control study in Shanghai, China. International journal of cancer. Journal international du cancer. Jul 20 2005;115(6):981-993.
Liu Y, Tamimi RM, Berkey CS, Willett WC, Collins LC, Schnitt SJ, ... Colditz GA. Intakes of alcohol and folate during adolescence and risk of proliferative benign breast disease. Pediatrics. May 2012;129(5):e1192-1198.
Liu Z, Saarinen NM, Thompson LU. Sesamin Is One of the Major Precursors of Mammalian Lignans in Sesame Seed (Sesamum indicum) as Observed In Vitro and in Rats. The Journal of nutrition. 2006;136(4):906-912.
Ljung BM, Drejet A, Chiampi N, Jeffrey J, Goodson WH, 3rd, Chew K, ... Miller TR. Diagnostic accuracy of fine-needle aspiration biopsy is determined by physician training in sampling technique. Cancer. Aug 25 2001;93(4):263-268.
London SJ, Stein EA, Henderson IC, Stampfer MJ, Wood WC, Remine S, ... Willett WC. Carotenoids, retinol, and vitamin E and risk of proliferative benign breast disease and breast cancer. Cancer causes & control : CCC. Nov 1992;3(6):503-512.
Lu WJ, Xu C, Pei Z, Mayhoub AS, Cushman M, Flockhart DA. The tamoxifen metabolite norendoxifen is a potent and selective inhibitor of aromatase (CYP19) and a potential lead compound for novel therapeutic agents. Breast cancer research and treatment. May 2012;133(1):99-109.
Maksim. Wikimedia Commons. Illu breast anatomy. Available at: http://commons.wikimedia.org/wiki/File:Illu_breast_anatomy.jpg. Last updated 7/7/2014. Accessed 3/12/2015.
Mauvais-Jarvis P, Kuttenn F, Gompel A. Antiestrogen action of progesterone in breast tissue. Breast cancer research and treatment. 1986;8(3):179-188.
Mayo Clinic. Diseases and Conditions page. Fibrocystic breasts. Complications. Available at: http://www.mayoclinic.org/diseases-conditions/fibrocystic-breasts/basics/complications/con-20034681 . 3/8/2013b. Accessed 5/4/2015.
Mayo Clinic. Diseases and Conditions page. Fibrocystic breasts. Definition. Available at: http://www.mayoclinic.org/diseases-conditions/fibrocystic-breasts/basics/definition/con-20034681. 3/8/2013a. Accessed 4/7/2015.
Mayo Clinic. Patient Care & Health Info page. Slide show: Female breast anatomy. Available at: http://www.mayoclinic.org/healthy-living/womens-health/multimedia/breast-cancer-early-stage/sls-20076628 . Accessed 2/18/2015a.
Mayo Clinic. Cabergoline (Oral Route). Side Effects. Available at: http://www.mayoclinic.org/drugs-supplements/cabergoline-oral-route/side-effects/drg-20062485 . Last updated 4/1/2015b. Accessed 6/12/2015.
Miltenburg DM, Speights VO, Jr. Benign breast disease. Obstetrics and gynecology clinics of North America. Jun 2008;35(2):285-300, ix.
NBCF. National Breast Cancer Foundation, Inc. Breast Self-Exam. Available at: http://www.nationalbreastcancer.org/breast-self-exam. Copyright 2012. Accessed 4/7/2015.
NCI. National Cancer Institute. Mammograms. http://www.cancer.gov/cancertopics/factsheet/detection/mammograms. 3/25/2014. Accessed 12/22/2014.
Neville MC. Classic studies of mammary development and milk secretion: 1945 - 1980. Journal of mammary gland biology and neoplasia. Sep 2009;14(3):193-197.
Neville MC. Milk Secretion: An Overview. http://mammary.nih.gov/reviews/lactation/Neville001/. Accessed 11/11/2014.
NHS. National Health Service. Side effects page. Danazol (Danazol 100 mg capsules). Available at: http://www.nhs.uk/Medicine-Guides/Pages/MedicineSideEffects.aspx?condition=Fibrocystic%20breast%20disease&medicine=Danazol. Accessed 2/18/2015. 2015.
NIH. U.S. National Library of Medicine. MedlinePlus. Cabergoline. Available at: http://www.nlm.nih.gov/medlineplus/druginfo/meds/a612020.html. Last updated 8/15/2012. Accessed 6/12/2015.
NLM. U.S. National Library of Medicine. PubChem. Compound Summary for CID 28417. danazol. Available at: http://pubchem.ncbi.nlm.nih.gov/compound/danazol#section=Top. Accessed 3/9/2015.
NLM. U.S. National Library of Medicine. PubMed Health. Breast Cancer Treatment (PDQ®). Available at: http://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0032825/#CDR0000062955__140. Last updated 11/25/2014. Accessed 3/6/2015.
NLM. U.S. National Library of Medicine. MedlinePlus. Fibrocystic breast disease. http://www.nlm.nih.gov/medlineplus/ency/article/000912.htm. Last updated 11/15/2013 . Accessed 11/10/2014.
Nussey S, Whitehead S. Chapter 7: The pituitary gland. In: Endocrinology: An Integrated Approach. Oxford: BIOS Scientific Publishers; 2001. <http://www.ncbi.nlm.nih.gov/books/NBK27/>.
Olawaiye A, Withiam-Leitch M, Danakas G, Kahn K. Mastalgia: a review of management. The Journal of reproductive medicine. Dec 2005;50(12):933-939.
O'Neil CK, Hanlon JT, Marcum ZA. Adverse effects of analgesics commonly used by older adults with osteoarthritis: focus on non-opioid and opioid analgesics. The American journal of geriatric pharmacotherapy. Dec 2012;10(6):331-342.
Onstad M, Stuckey A. Benign breast disorders. Obstetrics and gynecology clinics of North America. Sep 2013;40(3):459-473.
Pandey KB, Rizvi SI. Plant polyphenols as dietary antioxidants in human health and disease. Oxidative medicine and cellular longevity. Nov-Dec 2009;2(5):270-278.
Parker SJ, Harries SA. Phyllodes tumours. Postgraduate medical journal. Jul 2001;77(909):428-435.
Patrick L. Iodine: deficiency and therapeutic considerations. Alternative medicine review : a journal of clinical therapeutic. Jun 2008;13(2):116-127.
Peters F, Schuth W, Scheurich B, Breckwoldt M. Serum prolactin levels in patients with fibrocystic breast disease. Obstetrics and gynecology. Sep 1984;64(3):381-385.
Plantinga L, Grubbs V, Sarkar U, Hsu CY, Hedgeman E, Robinson B, ... Powe N. Nonsteroidal anti-inflammatory drug use among persons with chronic kidney disease in the United States. Annals of family medicine. Sep-Oct 2011;9(5):423-430.
Poellinger A. Near-infrared imaging of breast cancer using optical contrast agents. Journal of biophotonics. Nov 2012;5(11-12):815-826.
Prendergast P. Anatomy of the Breast. In: Shiffman MA, Di Giuseppe A, eds. Cosmetic Surgery: Springer Berlin Heidelberg; 2013:47-55.
Pruthi S, Wahner-Roedler DL, Torkelson CJ, Cha SS, Thicke LS, Hazelton JH, Bauer BA. Vitamin E and evening primrose oil for management of cyclical mastalgia: a randomized pilot study. Alternative medicine review : a journal of clinical therapeutic. Apr 2010;15(1):59-67.
Qureshi S, Sultan N. Topical nonsteroidal anti-inflammatory drugs versus oil of evening primrose in the treatment of mastalgia. The surgeon : journal of the Royal Colleges of Surgeons of Edinburgh and Ireland. Feb 2005;3(1):7-10.
Rohan TE, Negassa A, Caan B, Chlebowski RT, Curb JD, Ginsberg M, ... Page DL. Low-fat dietary pattern and risk of benign proliferative breast disease: a randomized, controlled dietary modification trial. Cancer prevention research (Philadelphia, Pa.). 2008;1(4):275-284.
Rosa M. "Inflammatory" changes in breast: how to provide a better care to our patients. Archives of gynecology and obstetrics. May 2010;281(5):901-905.
Rosolowich V, Saettler E, and Szuck B. SOGC Clinical Practice Guidelines, No. 170. Mastalgia. Available at: http://www.jogc.com/abstracts/full/200601_SOGCClinicalPracticeGuidelines_1.pdf . Jan 2006.
Schnitt SJ. Benign breast disease and breast cancer risk: morphology and beyond. The American journal of surgical pathology. Jun 2003;27(6):836-841.
Scott-Conner C. UI Health Care. Health Library page. FAQ: Fibrocystic Breast Disease. Available at: http://www.uihealthcare.org/fibrocystic-breast-disease-frequently-asked-questions/. Copyright 2015. Accessed 4/7/2015.
Seager JM, Hawkey CJ. ABC of the upper gastrointestinal tract: Indigestion and non-steroidal anti-inflammatory drugs. BMJ (Clinical research ed.). Nov 24 2001;323(7323):1236-1239.
Shannon J, King IB, Lampe JW, Gao DL, Ray RM, Lin MG, ... Thomas DB. Erythrocyte fatty acids and risk of proliferative and nonproliferative fibrocystic disease in women in Shanghai, China. The American journal of clinical nutrition. Jan 2009;89(1):265-276.
Sharma GN, Dave R, Sanadya J, Sharma P, Sharma KK. Various types and management of breast cancer: an overview. Journal of advanced pharmaceutical technology & research. Apr 2010;1(2):109-126.
Sharma N, Gupta A, Jha PK, Rajput P. Mastalgia cured! Randomized trial comparing centchroman to evening primrose oil. The breast journal. Sep 2012;18(5):509-510.
Smyth PP. The thyroid, iodine and breast cancer. Breast cancer research : BCR. 2003;5(5):235-238.
Srivastava A, Mansel RE, Arvind N, Prasad K, Dhar A, Chabra A. Evidence-based management of Mastalgia: a meta-analysis of randomised trials. Breast (Edinburgh, Scotland). Oct 2007;16(5):503-512.
Stoddard FR, 2nd, Brooks AD, Eskin BA, Johannes GJ. Iodine alters gene expression in the MCF7 breast cancer cell line: evidence for an anti-estrogen effect of iodine. International journal of medical sciences. 2008;5(4):189-196.
Su X, Colditz GA, Collins LC, Baer HJ, Sampson LA, Willett WC, ... Tamimi RM. Adolescent intakes of vitamin D and calcium and incidence of proliferative benign breast disease. Breast cancer research and treatment. Jul 2012;134(2):783-791.
Su X, Tamimi RM, Collins LC, Baer HJ, Cho E, Sampson L, ... Colditz GA. Intake of fiber and nuts during adolescence and incidence of proliferative benign breast disease. Cancer causes & control : CCC. Jul 2010;21(7):1033-1046.
Sugg S, Lizarraga I, Colwick SE. ePocrates. Fibrocystic breasts. Available at: https://online.epocrates.com/noFrame/showPage.do?method=diseases&MonographId=1003. Last updated 5/13/2014. Accessed 10/16/2014.
Suzuki R, Rylander-Rudqvist T, Saji S, Bergkvist L, Adlercreutz H, Wolk A. Dietary lignans and postmenopausal breast cancer risk by oestrogen receptor status: a prospective cohort study of Swedish women. British journal of cancer. Feb 12 2008;98(3):636-640.
Tamimi RM, Rosner B, Colditz GA. Evaluation of a breast cancer risk prediction model expanded to include category of prior benign breast disease lesion. Cancer. Nov 1 2010;116(21):4944-4953.
Tejwani PL, Srivastava A, Nerkar H, Dhar A, Hari S, Thulkar S, ... Kumar S. Centchroman regresses mastalgia: a randomized comparison with danazol. The Indian journal of surgery. Jun 2011;73(3):199-205.
Thompson LU, Seidl MM, Rickard SE, Orcheson LJ, Fong HH. Antitumorigenic effect of a mammalian lignan precursor from flaxseed. Nutrition and cancer. 1996;26(2):159-165.
UCSF. University of California San Francisco. Patient Education page. The Menstrual Cycle. 2015. Available at: http://www.ucsfhealth.org/education/the_menstrual_cycle/.
Vaidyanathan L, Barnard K, Elnicki DM. Benign breast disease: when to treat, when to reassure, when to refer. Cleveland Clinic journal of medicine. May 2002;69(5):425-432.
van Die MD, Burger HG, Teede HJ, Bone KM. Vitex agnus-castus extracts for female reproductive disorders: a systematic review of clinical trials. Planta medica. May 2013;79(7):562-575.
Vang O, Ahmad N, Baile CA, Baur JA, Brown K, Csiszar A, ... Wu JM. What is new for an old molecule? Systematic review and recommendations on the use of resveratrol. PloS one. 2011;6(6):e19881.
Vaziri F, Zamani Lari M, Samsami Dehaghani A, Salehi M, Sadeghpour H, Akbarzadeh M, Zare N. Comparing the effects of dietary flaxseed and omega-3 Fatty acids supplement on cyclical mastalgia in Iranian women: a randomized clinical trial. International journal of family medicine. 2014;2014:174532.
Verkooijen HM. Diagnostic accuracy of stereotactic large-core needle biopsy for nonpalpable breast disease: results of a multicenter prospective study with 95% surgical confirmation. International journal of cancer. Journal international du cancer. Jun 20 2002;99(6):853-859.
Visscher DW, Nassar A, Degnim AC, Frost MH, Vierkant RA, Frank RD, ... Hartmann LC. Sclerosing adenosis and risk of breast cancer. Breast cancer research and treatment. Feb 2014;144(1):205-212.
Vorherr H. Fibrocystic breast disease: pathophysiology, pathomorphology, clinical picture, and management. American journal of obstetrics and gynecology. Jan 1986;154(1):161-179.
Wells CA, El-Ayat GA. Non-operative breast pathology: apocrine lesions. Journal of clinical pathology. Dec 2007;60(12):1313-1320.
Weng JR, Tsai CH, Kulp SK, Chen CS. Indole-3-carbinol as a chemopreventive and anti-cancer agent. Cancer letters. Apr 18 2008;262(2):153-163.
Wesola M, Jelen M. The diagnostic efficiency of fine needle aspiration biopsy in breast cancers - review. Advances in clinical and experimental medicine : official organ Wroclaw Medical University. Nov-Dec 2013;22(6):887-892.
Willems SM, van Deurzen CH, van Diest PJ. Diagnosis of breast lesions: fine-needle aspiration cytology or core needle biopsy? A review. Journal of clinical pathology. Apr 2012;65(4):287-292.
Willför S, Hemming J, Reunanen M, Eckerman C, Holmbom B. Lignans and Lipophilic Extractives in Norway Spruce Knots and Stemwood. Holzforschung. 2003;57(1):27-36.
Wuttke W, Jarry H, Christoffel V, Spengler B, Seidlova-Wuttke D. Chaste tree (Vitex agnus-castus)--pharmacology and clinical indications. Phytomedicine : international journal of phytotherapy and phytopharmacology. May 2003;10(4):348-357.
Yu H, Rohan TE, Cook MG, Howe GR, Miller AB. Risk factors for fibroadenoma: a case-control study in Australia. American journal of epidemiology. Feb 1 1992;135(3):247-258.
Yu JH, Kim MJ, Cho H, Liu HJ, Han SJ, Ahn TG. Breast diseases during pregnancy and lactation. Obstetrics & gynecology science. May 2013;56(3):143-159.
Zervoudis S, Iatrakis G, Tomara E, Bothou A, Papadopoulos G, Tsakiris G. Main controversies in breast cancer. World journal of clinical oncology. Aug 10 2014;5(3):359-373.
