
Diverticulosis and Diverticular Disease
Diverticulosis and Diverticular Disease
Last Section Update: 01/2023
Contributor(s): Maureen Williams, ND
1 Overview
Summary and Quick Facts for Diverticulosis and Diverticular Disease
- The presence of small pouches or pockets in the wall of the large intestine is common with advancing age. These pockets are called diverticula, and most often form in the lower part of the large intestine, the colon.
- In this protocol you will learn about how diverticulosis and diverticular disease develop, and what factors are thought to increase risk of these conditions. You will also discover how new evidence is reshaping the treatment of these conditions.
- Targeted natural interventions including probiotics butyrate and fiber may help decrease symptoms and improve diverticular disease.
Diverticula are small pouches or pockets in the wall of the digestive system, most often the large intestine. When these pouches become inflamed, this characterizes diverticular disease. Diverticula are quite common in older individuals, and often do not cause symptoms.
Targeted natural interventions including probiotics, butyrate, and fiber may help decrease symptoms and improve diverticular disease.
Figure 1: The Spectrum of Conditions Associated with Diverticula

Signs and Symptoms
- Acute diverticulitis causes pain in the lower left abdomen that tends to worsen with movement.
Causes and Risk Factors
- Factors currently known to increase risk of diverticulosis include advancing age, obesity, and smoking.
- Factors known to increase risk of diverticulitis include low-fiber diet, sedentary lifestyle, obesity, smoking, alcohol consumption, and use of NSAIDs and pain relievers.
Diagnosis
- Since it is asymptomatic in most people, diverticulosis is usually found incidentally during an unrelated diagnostic or screening procedure.
- Computed tomography (CT) scan or abdominal ultrasound are the preferred diagnostic imaging modalities to establish a diagnosis of diverticular disease.
- Mild cases of uncomplicated diverticular disease may be confused with irritable bowel syndrome.
Conventional Treatment
- Asymptomatic diverticulosis does not require treatment.
- Conservative treatment for uncomplicated diverticulitis includes a liquid or low-residue diet and oral antibiotics.
- In complicated diverticulitis, hospitalization with intravenous fluids, antibiotics, or surgery may be required.
Novel and Emerging Strategies
- Fecal calprotectin, a non-invasive stool test, is under investigation as a biomarker that may help identify diverticular disease.
- An analysis of four randomized controlled trials found rifaximin (Xifaxan), an antibiotic with a favorable safety profile, plus fiber supplementation was associated with better symptom relief, fewer complications, and a better chance of being symptom-free after one year compared with fiber supplementation alone.
- A randomized controlled trial using mesalamine (Asacol) in patients with acute diverticulitis found the rate of complete response was significantly higher in patients receiving mesalamine versus placebo.
Dietary and Lifestyle Considerations
- Plant-based diets that are high in fiber may protect against diverticular disease.
- Contrary to popular belief, nut and popcorn consumption may reduce the risk of diverticulitis rather than increase it.
- Physical activity and maintaining a healthy weight may reduce the incidence of diverticular disease.
Note: A low-fiber diet is often recommended during the initial healing phase after an episode of acute diverticulitis. People recovering from an episode should ask their healthcare provider about consuming fiber.
Integrative Interventions
- Probiotics: By helping restore the balance of intestinal flora and reduce inflammation in the intestine, probiotic supplementation may be of benefit in both acute and chronic diverticular problems.
- Butyrate: In a randomized clinical trial of sodium butyrate in 52 people with diverticular disease, less than 7% of those in the butyrate group experienced diverticulitis symptoms compared with slightly more than 31% in the placebo group.
- Fiber: Gradually increasing fiber until consumption reaches 20–30 g of fiber daily has been recommended by some diverticular disease researchers. Supplemental fiber in a form like psyllium seed husk can help increase total daily fiber intake.
- Fish oil: Several university-associated medical centers recommend supplementing omega-3 fatty acids, including from fish oil, in diverticular disease, as these have anti-inflammatory activity.
- Curcumin: Studies in animal models have shown curcumin can inhibit tumor necrosis factor-alpha, one of the inflammatory chemical messengers associated with diverticular disease and acute diverticulitis.
2 Introduction
The presence of small pouches or pockets in the wall of the large intestine is common with advancing age. These pockets are called diverticula, and most often form in the lower part of the large intestine, the colon (NIDDK 2012; Mayo Clinic 2014a). In Western countries, more than half of people older than 70 have diverticula; and in the United States, colonic diverticula are present in about two-thirds of individuals over age 85 (Peery 2013; Ferri 2015).
Many long-held beliefs about diverticula and associated conditions have been challenged over the past several years. For example, it used to be thought that fragments of foods containing large fibrous particles, such as popcorn, nuts, seeds, and corn, could become trapped in diverticula and cause inflammation (Thaha 2015). However, a large study that monitored over 47 000 men for 18 years showed that eating these foods did not increase risk for diverticular inflammation; in fact, study participants who ate the most nuts and popcorn actually had a decreased risk of diverticular complications (Strate 2008).
Diverticula do not by themselves ordinarily cause symptoms (Boynton 2013; Sopena 2011). In fact, many people are not even aware they have diverticula until they are detected during a routine colonoscopy or other procedure (Strate, Modi 2012; Thaha 2015; Mosadeghi 2015). A person who has diverticula without inflammation or any associated symptoms is said to have diverticulosis, a term that simply denotes the presence of diverticula in the large intestine (NIDDK 2012).
Less commonly, however, diverticula do cause problems. A person who has symptoms associated with diverticula is said to have diverticular disease (Spiller 2015; Strate, Modi 2012; Aydin 2012; Peery 2013).
Inflammation of diverticula—called diverticulitis—is a form of diverticular disease that can cause symptoms ranging from mild abdominal pain and fever to potentially life-threatening hemorrhage (NIDDK 2012; Thaha 2015; Ferri 2015). Diverticulosis is thought to progress to diverticulitis in about 1‒4% of cases (Shahedi 2013).
For decades, the standard of care for diverticulitis emphasized hospitalization and treatment with antibiotics, and possibly invasive surgery. However, a growing body of evidence suggests this aggressive approach may not improve outcomes compared with a more conservative approach that emphasizes individualized evaluation and treatment, and the judicious use of antibiotics and minimally invasive surgical techniques. Additionally, emerging therapies such as probiotics, non-systemic antibiotics, and anti-inflammatory drugs are increasingly being studied for the treatment of diverticular disease (McDermott 2014; Turley 2013; Razik 2015; Kruse 2014; Regenbogen 2014; Morris 2014).
In this protocol you will learn about how diverticulosis and diverticular disease develop, and what factors are thought to increase risk of these conditions. You will also discover how new evidence is reshaping the treatment of these conditions. Several promising novel and emerging approaches to treating diverticular disease will be reviewed, and a number of integrative interventions such as probiotics, butyrate, and natural anti-inflammatory agents will be described as well.
3 Background
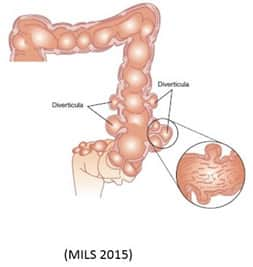
The colon wall is made up of several layers, including the mucosa, submucosa, and a muscular outer wall. The muscular layer itself has an inner and outer layer (Maykel 2004).
In the most common type of diverticula, the mucosa and submucosa are forced through weak areas in the muscular layer (Strate, Modi 2012; von Rahden 2012). Between 65% and 90% of colonic diverticula occur in the sigmoid colon, which is on the left side and close to the end of the digestive tract, with the remainder located in other regions (Maykel 2004; Bugiantella 2015).
Diverticula form as a result of a complex interaction of age, diet, and structural and functional changes in the nerves and muscles of the colon wall. These factors may contribute to weakness of and increased pressure on the colon wall (Strate, Modi 2012; von Rahden 2012; Bugiantella 2015; Humes 2014).
In 1‒4% of cases, diverticula become inflamed; this is known as diverticulitis (Shahedi 2013). It used to be thought that mechanical obstruction of diverticula by fecal matter or undigested food particles caused diverticular disease, but newer research suggests that changes in the microbial composition of the intestinal tract (which can create a pro-inflammatory environment) and changes in colon motility are important contributors (von Rahden 2012; Tursi 2012; Strate, Modi 2012; Peery 2013).
4 Signs and Symptoms
About 80‒85% of individuals with diverticulosis will never experience any symptoms; about 10‒15% will develop diverticular disease; and roughly 5% will have at least one episode of acute diverticulitis (Bugiantella 2015). For those who develop diverticular disease, symptoms can have a rapid, or acute, onset, or can be ongoing and chronic, and can vary in intensity from mild to severe (Sopena 2011; Boynton 2013).
Chronic Diverticular Disease
There are several different specific symptom patterns of chronic diverticular disease:
Symptomatic uncomplicated diverticular disease (SUDD). This condition is characterized by recurring or persistent lower left abdominal pain, bloating, and constipation or diarrhea, in the absence of diverticulitis. SUDD can resemble irritable bowel syndrome. Fever, elevated white blood cell count, and other signs of an infectious or inflammatory condition are not characteristic of SUDD (Tursi 2010).
Segmental colitis associated with diverticulitis (SCAD). SCAD is thought to occur in about 0.3‒1.3% of people with diverticulosis, and appears to be similar to inflammatory bowel disease. The symptoms most commonly associated with SCAD are rectal bleeding, diarrhea, and abdominal pain; fever and elevated white blood cell count do not usually occur with this condition (Mann 2012).
Chronic diverticulitis. Chronic diverticulitis is characterized by mild and persistent diverticular inflammation that may cause abdominal pain but usually does not cause fever (Sheiman 2008).
Acute Diverticular Disease
The characteristic symptom of acute diverticulitis is pain in the lower left abdomen that tends to worsen with movement; pain may also be right-sided or originate in other parts of the abdomen. Fever, usually below 102°F, is another common symptom. Other possible symptoms include abdominal bloating, lack of appetite, nausea (generally without vomiting), constipation or diarrhea, and painful urination. In severe acute diverticulitis, the abdomen may become stiff and rigid (Wilkins 2013; Medina-Fernandez 2015).
An episode of acute diverticulitis may become a medical emergency necessitating surgical intervention if complications arise. Potential complications include bleeding, abscess, fistula, perforation, or obstruction (Schaffzin 2004; Köckerling 2015).
Figure 1: The Spectrum of Conditions Associated with Diverticula (Collins 2015; Strate 2012)
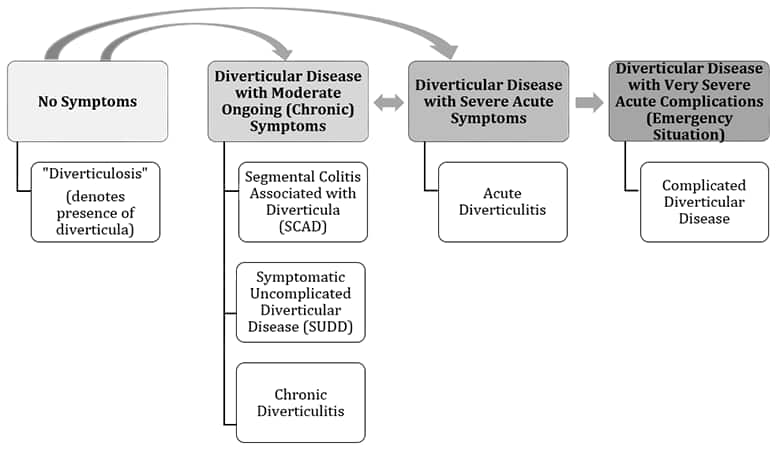
|
Distinguishing Symptomatic Uncomplicated Diverticular Disease from Irritable Bowel Syndrome Symptomatic uncomplicated diverticular disease (SUDD) may be confused with irritable bowel syndrome (IBS) due to the overlap in their hallmark symptoms: abdominal discomfort or pain and disturbance in bowel habits (Spiller 2012). It can also be difficult to distinguish these conditions because they appear to co-occur in many people (Jung 2010; Yamada 2014). What’s more, researchers speculate that a bout of acute diverticulitis may trigger colonic sensory and motor nerve damage, changes in bacterial ecology, and mucosal inflammation, resulting in a set of chronic abdominal and digestive symptoms sometimes referred to as “post-diverticulitis IBS.” One study found that people with a history of diverticulitis were 4.6 times more likely to receive a diagnosis of IBS during a nine-year period than people without a history of diverticulitis (Strate, Modi 2012). A correct diagnosis is critical in these cases, since surgery may be a reasonable choice for someone with recurrent acute diverticulitis but is likely to yield poor results in IBS (Spiller 2014). It appears that the pattern of abdominal pain may be helpful in distinguishing SUDD from IBS. In one study, 72 people with colonoscopy-confirmed diverticulosis and suffering from abdominal pain were given a preliminary diagnosis of either SUDD or IBS-like symptoms, based on the location and duration of their pain; those with lower left-sided abdominal pain lasting more than 24 hours met the diagnostic criteria for SUDD, and those with pain in other parts of their abdomen were considered to have IBS-like symptoms. Researchers then found that no one in the IBS-like symptom group, and 64% of those in the SUDD group, had elevated fecal calprotectin, a marker of intestinal inflammation, thereby showing that moderate-to-severe lower left-sided pain lasting more than 24 hours is correlated with diverticular disease (Tursi 2015). |
5 Causes and Risk Factors
Diverticulosis
Factors currently known to increase risk of diverticulosis include advancing age, obesity (especially central or visceral obesity), and smoking (Comstock 2014; Nagata 2014; Spiller 2015; Medina-Fernandez 2015; Nagata 2013).
Diverticular Disease
Several factors increase the risk of progression from diverticulosis to diverticular disease (Peery 2013; von Rahden 2012):
Low-fiber diet. In a study of 47 033 healthy adults followed for an average of 11.6 years, those with the highest dietary fiber intake (>25 g daily) were 41% less likely to be hospitalized for diverticular disease compared with those with the lowest intake (<14 g daily) (Crowe 2011). A four-year study in over 43 000 participants found that those with the highest intake of insoluble fiber had an approximately 40% lower risk of diverticular disease (Aldoori 1998).
Sedentary lifestyle. Several studies have found that increased physical activity appears to be protective against diverticular disease (Aldoori, Giovannucci, Rimm, Ascherio 1995; Williams 2009).
Obesity. Most studies show that higher body mass index, obesity, and abdominal obesity increase the risk of diverticular disease and its complications (Spiller 2015; Bose 2013; Dobbins 2006; Strate, Liu, Aldoori, Syngal 2009; Sorser 2009).
Smoking. Most studies suggest smokers are at increased risk of complications of diverticular disease, particularly perforation, but also abscess and hospitalization (Turunen 2010; Papagrigoriadis 1999; Collins 2015; Hjern 2011; Aldoori, Giovannucci, Rimm, Wing 1995).
Alcohol. Research into alcohol consumption and risk of diverticular disease has been inconclusive (Aldoori 2002; Strate 2012), though a study that included 23 people under age 50 found that in that age group, chronic alcohol consumption was associated with greater than three-fold higher odds of having an episode of acute diverticulitis (Pisanu 2013).
Non-steroidal anti-inflammatory drugs (NSAIDs), pain relievers, and steroids. The use of aspirin and other NSAIDs such as ibuprofen; opioid pain relievers such as codeine; and corticosteroids, especially inhaled steroids used to treat asthma, appear to increase the risk of diverticulitis and its complications (Hjern 2015; Kvasnovsky 2014; Strate 2011).
6 Diagnosis
Diverticulosis
Diverticulosis is usually found incidentally during an unrelated diagnostic or screening procedure (Sopena 2011). In fact, asymptomatic diverticulosis is the most common finding on routine cancer-screening colonoscopy (Shahedi 2013).
Diverticular Disease
Diverticular disease, including acute diverticulitis, can often be diagnosed on the basis of the patient’s signs and symptoms, including physical exam findings, medical history, and laboratory testing. In approximately one-third of cases, diagnostic imaging is necessary to make a diagnosis (Andeweg 2014; Bugiantella 2015).
Several abdominal and pelvic ailments must be ruled out to diagnose diverticular disease. These include appendicitis, bowel obstruction, colon cancer, ectopic pregnancy, gastroenteritis, inflammatory bowel disease, irritable bowel syndrome, kidney stones, diseases of the ovaries, pancreatitis, and urinary tract infection (Wilkins 2013). Computed tomography (CT) scan or abdominal ultrasound are the preferred diagnostic imaging modalities, when necessary, to establish a diagnosis of diverticular disease (Aydin 2012; Andeweg 2014).
Due to the risk of pain or complications, colonoscopy cannot be performed during an episode of diverticular disease or acute diverticulitis. However, it may be recommended four to six weeks after an acute episode has resolved, particularly in cases with complications or after a first episode of acute diverticulitis to rule out an underlying cancer (Bugiantella 2015; Wilkins 2013). Nevertheless, there is increasing evidence that CT imaging used in the initial assessment is adequate to identify cancer, leading some researchers to recommend against additional colonoscopies beyond the regular colon cancer screening schedule (Medina-Fernandez 2015).
While uncomplicated diverticular disease is not associated with changes in blood test parameters, acute diverticulitis may cause blood test abnormalities including:
- High white blood cell count (leukocytosis). A high number of white blood cells is seen in about 55% of cases of acute diverticulitis (Wilkins 2013) and indicates active infection or inflammation (Asadollahi 2011).
- Elevated C-reactive protein. C-reactive protein is a marker of inflammation. High levels (>50 mg/L) are frequently seen in people with acute diverticulitis, and very high levels (>200 mg/L) may be a sign of perforation (Wilkins 2013).
- Anemia. Anemia may develop due to bleeding of diverticula, especially in elderly patients (Lizardi-Cervera 2008).
7 Conventional Treatment
Diverticulosis
Asymptomatic diverticulosis does not require treatment (Telem 2009; Sopena 2011). However, several preventive measures may reduce the risk that diverticulosis will progress to diverticular disease. These include eating a diet high in fiber and low in animal-based foods; getting adequate physical activity; not smoking; restricting alcohol intake; limiting use of non-steroidal anti-inflammatory drugs, steroids, and opiate painkillers; and maintaining a healthy weight (Strate 2012; Bugiantella 2015).
Uncomplicated Diverticulitis
Traditionally, uncomplicated diverticulitis has been treated with broad-spectrum antibiotics and a liquid diet (Ferri 2015). However, the use of antibiotics in uncomplicated or mild diverticulitis has recently been called into question because new evidence suggests they may be unnecessary (de Korte 2011; Hjern 2007; Collins 2015). There is an emerging consensus in the scientific literature that treating mild uncomplicated diverticulitis with antibiotics has no benefit in terms of speeding recovery or preventing complications and recurrences (de Korte 2011; Hjern 2007; Collins 2015; Wilkins 2013).
Recommendations for conservative treatment usually include outpatient management with a liquid or low-residue diet (ie, low in fiber and other foods that increase bowel activity such as dairy), sometimes called bowel rest, and oral antibiotics if symptoms persist but do not worsen over three days (Wilkins 2013; Thaha 2015; Ferri 2015). Surgery is rarely considered necessary for uncomplicated diverticulitis; it is reserved for cases that do not respond to medical management, based on individualized risk analysis (Humes 2014; Wilkins 2013).
In light of new evidence and the evolving model of diverticular disease as an inflammatory condition associated with a disturbed bowel flora, newer treatments are increasingly being used in mild and uncomplicated cases and to prevent recurrence (Humes 2014). These therapies, including non-systemically absorbed antibiotics and probiotics, are described in the Novel and Emerging Therapies and Integrative Interventions sections of this protocol.
Complicated Diverticulitis
In complicated diverticulitis, hospitalization with intravenous fluids and antibiotics may be required. A localized abscess may be drained using CT-guided percutaneous drainage. Diagnostic imaging is recommended to assess severity and identify complications, which could include abscess, perforation, fistula, or stricture (Wilkins 2013).
Surgery is usually reserved for those with abscesses, perforations, fistulas, obstructions, or multiple recurrences, and those who do not respond to appropriate medical treatment. Abdominal surgery can be performed either laparoscopically or as traditional open surgery. Bowel resection may be performed, though more conservative methods such as laparoscopic intraperitoneal lavage (washing) and percutaneous drainage are increasingly favored, especially for low-grade abscesses. These less-invasive procedures result in shorter hospitalizations, fewer complications, and better in-hospital survival (Franklin 2008; Wilkins 2013; Ferri 2015; Morris 2014; Medina-Fernandez 2015).
8 Novel and Emerging Strategies
Fecal Calprotectin Testing
Calprotectin is a protein released from white blood cells during inflammation. Fecal calprotectin, a non-invasive stool test, is under investigation as a biomarker that may help identify diverticular disease. Fecal calprotectin can distinguish inflammatory bowel diseases, such as Crohn’s or ulcerative colitis, from functional disorders such as irritable bowel syndrome (IBS). Fecal calprotectin is also being investigated as a biomarker for colorectal cancer and as a clinical tool in patients with inflammatory bowel disease to identify risk of relapse (Burri 2014; Henderson 2014; Fengming 2014).
Two studies have found that fecal calprotectin is higher in active diverticular disease than in healthy individuals and those with IBS. In asymptomatic diverticulosis, however, fecal calprotectin was not elevated; and in segmental colitis associated with diverticula (SCAD) it was higher than in other types of diverticular disease. In these studies, treatment of uncomplicated acute diverticulitis and symptomatic uncomplicated diverticular disease (SUDD) reduced fecal calprotectin to normal levels (Tursi 2009; Tursi 2011).
Persistently high fecal calprotectin may indicate a high risk of recurrence. In one study, 54 people were followed for an average of 20 months after a bout of acute uncomplicated diverticulitis; seven of the eight people who had a recurrence during the study had elevated fecal calprotectin, while only one person who experienced a recurrence had normal fecal calprotectin (Tursi, Elisei, Picchio 2014).
Taken together, these preliminary findings suggest fecal calprotectin may distinguish diverticular disease from IBS; help monitor severity of diverticulitis and response to treatment; and predict risk of disease recurrence (Tursi, Elisei 2015; Tursi 2009; Erbayrak 2009).
Rifaximin
Rifaximin (Xifaxan) is an antibiotic that is poorly absorbed into the bloodstream and so has a favorable safety profile (Gold Standard 2014). Rifaximin targets the microbial community in the gut and has been studied for the treatment of SUDD (Sopena 2011; Strate, Modi 2012). A comprehensive literature review analyzed four randomized controlled trials that compared treatment of SUDD using fiber supplementation plus seven days per month of rifaximin with fiber supplementation alone. This analysis found that rifaximin was associated with better symptom relief, fewer complications, and a better chance of being symptom-free after one year (Bianchi 2011).
An interesting study in 40 patients with uncomplicated diverticular disease found that rifaximin treatment reduced the interaction of gut bacteria with specialized receptors on immune cells, called toll-like receptors, which are involved in the induction of the inflammatory immune response to microorganisms. This study showed that rifaximin reduced the activation of toll-like receptors, thereby reducing gut inflammation. These findings prompted the researchers who conducted the study to postulate that rifaximin might have anti-inflammatory activity in the gut lining, as well as systemic immune-modulating effects, through its impact on pathogenic microbes residing in the gut (Cianci 2014).
Mesalamine
Mesalamine (also called mesalazine) (Asacol) belongs to a class of medications that contain 5-aminosalicylic acid (5-ASA), which have anti-inflammatory and free radical-scavenging effects. Medications in this drug class are used in the treatment of inflammatory bowel disease (CCFA 2013; Tursi 2014; Thaha 2015). Mesalamine has also been studied in diverticular disease (Thaha 2015; Collins 2015; Morris 2014). One rigorous review of the scientific literature examined six randomized controlled trials of 5-ASA medications for uncomplicated diverticulitis in a total of 818 patients, and found that these medications led to significantly better outcomes than placebo (Gatta 2010).
A randomized controlled trial in 117 patients who had acute diverticulitis found that the rate of complete response, in which patients became asymptomatic, was significantly higher in patients receiving mesalamine than in those who received placebo (Stollman 2013). Additional rigorous studies are needed to clarify the role of mesalamine in the treatment of diverticular disease.
9 Dietary and Lifestyle Considerations
Plant-Based, Fiber-Rich Diet
Plant-based diets that are high in fiber may protect against diverticular disease. The study of fiber as it relates to diverticular disease often focuses on fiber’s role in promoting bowel regularity (Collins 2015). However, fiber may also influence the risk of diverticular disease via its role as a prebiotic, meaning it provides fuel for beneficial probiotic organisms. Also, fiber promotes the formation of short-chain fatty acids, notably butyrate, which are essential for colonic health. In fact, butyrate has been studied as a treatment for diverticular disease (Slavin 2013; Krokowicz, Stojcev 2014).
In a study that monitored over 47 000 men and women for an average of 11.6 years, vegetarians had a 31% lower risk and vegans had a 72% lower risk of diverticular disease compared with meat eaters. This study also noted a link between increased dietary fiber and lower risk of diverticular disease in both meat eaters and non-meat eaters (Crowe 2011). And in a study in more than 43 000 people, the risk of symptomatic diverticular disease was reduced by 45% in those with the highest intake of insoluble fiber, compared with those who had the lowest intake (Aldoori 1998).
Some, though not all, trials have found a beneficial effect of a high-fiber diet or fiber supplements on diverticular disease symptoms (Unlu 2012), and many practice guidelines call for a high fiber intake or fiber supplementation for the prevention and treatment of symptomatic diverticular disease (Cuomo 2014; Andersen 2012; Thaha 2015).
Note: A low-fiber, low-residue diet is often recommended during the initial healing phase after an episode of acute diverticulitis (Mayo Clinic 2014b; Saul 2015; Thaha 2015). People recovering from an episode of acute diverticulitis should ask their healthcare provider about consuming fiber.
Nuts, Corn, and Popcorn
Historically, diverticular disease management has included the avoidance of foods with large indigestible pieces such as nuts, seeds, corn, and popcorn. The belief behind this recommendation was that fragments of these foods could become trapped in diverticula and cause inflammation and infection. However, a study in over 47 000 American male health professionals found no association between consumption of these foods and diverticulitis risk. In fact, this study found that men who ate nuts or popcorn two or more times per week had 20% and 28% reduced risk of diverticulitis, respectively, compared with men who ate those foods less than once per month (Strate 2008).
Physical Activity and Weight Management
Physical activity and maintaining a healthy weight may reduce the incidence of diverticular disease and its complications. In an 18-year study in over 47 000 American male health professionals, those who reported exercising the most were 25% less likely to develop diverticular disease and 46% less likely to have diverticular bleeding than those who reported exercising the least. Vigorous activity was especially correlated with a significantly lower risk of diverticular disease and bleeding (Strate, Liu, Aldoori, Giovannucci 2009). A study in over 36 500 women found that those who reported low levels of exercise—30 minutes or less per day—had a 53% higher risk of diverticular disease compared with women who exercised more than 30 minutes per day (Hjern 2012). Another study that followed more than 10 000 joggers aged 50 or older for 7.7 years found that more running was associated with less diverticular disease, and more vigorous and longer runs were more protective (Williams 2009).
Also, excess weight, especially when carried around the abdomen, appears to be a risk factor for diverticular disease and its complications. A study in over 47 000 male US health professionals found that, compared with normal-weight men, obese men had a greater than 1.7-fold higher risk of diverticulitis and a 3.1-fold higher risk of diverticular bleeding; men with the largest waist circumference, compared with those with the lowest, had a greater than 1.5-fold higher risk of diverticulitis and greater than 1.9-fold higher risk of diverticular bleeding (Strate, Liu, Aldoori, Syngal 2009). Another study in women found that overweight and obese women had a 29% and 33% increased risk, respectively, of diverticular disease compared with normal-weight women; and obese women had double the risk for complicated diverticular disease (Hjern 2012).
10 Nutrients
Fiber Supplements
Several trials of high fiber diets and various forms of fiber supplements have shown benefit in terms of pain reduction and overall improvement in patients with diverticular disease (Hobson 2004; Unlu 2012).
Consumption of 20–30 g of fiber daily has been recommended by some diverticular disease researchers. Supplemental fiber in the form of agents like psyllium seed husk and ground flaxseed can help increase total daily fiber intake. Patients with diverticular disease who begin fiber supplementation or a program of increased dietary fiber should do so gradually, over a period of weeks, and simultaneously increase their fluid intake. This is because increasing one’s fiber intake too rapidly can cause symptoms of digestive upset such as gas and bloating. Also, for those recovering from a bout of acute diverticulitis, a low-fiber diet may be advised; people in this situation should talk with their healthcare provider before increasing fiber in their diet, including supplemental fiber (Saul 2015; Thaha 2015; Slavin 2013; Wick 2012).
Probiotics
Probiotics are living microorganisms that, when ingested in adequate amounts, have positive effects on health. In addition to supporting the functions of a healthy gut microbiome, such as inhibiting intestinal colonization by harmful microorganisms, aiding digestion, strengthening gut barrier function, and promoting normal gut motility, probiotics also appear to help regulate immune function and suppress inflammation (Ren 2022; Piccioni 2021).
Diverticular disease is increasingly being recognized as an inflammatory disorder that may be related to a disturbed intestinal microbial ecosystem, known as “dysbiosis” (Tursi 2022). By helping restore the balance of intestinal flora and reduce inflammation in the colon, probiotics may be of benefit in both acute and chronic diverticular problems (Piccioni 2021).
In general, probiotics containing Lactobacillus species have been found to reduce symptoms like bloating and abdominal pain in individuals with SUDD (Piccioni 2021). Results from two open-label studies suggest a probiotic containing L. casei DG (also known as L. paracasei CNCM I 1572) (Bretto 2022) may help reduce symptoms and prevent recurrence of acute diverticulitis in people with SUDD. The effect of this probiotic was comparable to mesalamine in both studies; however, the combination of mesalamine plus L. casei DG appeared to perform slightly better than either alone (Tursi 2006; Tursi 2008). A randomized controlled trial in 210 subjects with SUDD appeared to confirm these findings. This trial compared L. casei DG, at a dose of 24 billion CFUs once daily, and mesalamine, together and separately, with placebo. Cyclic schedules of 10 days per month were used for all interventions. After one year, both the probiotic and mesalamine were found to be more effective than placebo for maintaining remission, but the combination of probiotics plus mesalamine appeared to work better than either alone (Tursi 2013).
In an open-label trial, a combination of probiotics (375,000 CFUs L. acidophilus 145; 390 million CFUs L. helveticus ATC 15009; and 1.5 billion CFUs Bifidobacterium species 420) in a phytoextract-enriched medium was found to be effective for preventing disease recurrence in people with SUDD (Lamiki 2010). In another trial that included 45 participants with SUDD, a high-fiber diet supplemented with the probiotic L. paracasei B21060, at a dose of 5 billion CFUs plus 2,443 mg of prebiotic compounds per day, was compared to a high-fiber diet alone. After three and six months of treatment, abdominal pain was significantly improved in both groups, while bloating improved significantly only in the probiotic/prebiotic group (Lahner 2012). Another study in 50 participants diagnosed with SUDD compared a high-fiber diet alone to a high-fiber diet plus either low-dose (12.5 billion CFUs twice daily) or high-dose (25 billion CFUs twice daily) L. paracasei F19. Both of the diet plus probiotic groups had reduced bloating and fewer episodes of persistent abdominal pain compared with the diet only group (Annibale 2011).
Other probiotic species, such as L. reuteri (aka Limosilactobacillus reuteri), have demonstrated beneficial effects in patients with acute uncomplicated diverticulitis (Piccioni 2021). In a double-blind, randomized, placebo-controlled trial that included 88 patients with acute uncomplicated diverticulitis, treatment with antibiotic therapy plus L. reuteri 4659 (500 million CFUs two times per day) for 10 days reduced pain and lowered levels of C-reactive protein (a marker of inflammation) more than antibiotics plus placebo (Petruzziello, Migneco 2019). A mixture of three probiotic strains (6 billion CFUs B. lactis LA 304; 28 billion CFUs L. salivarius LA 302; and 6 billion CFUs L. acidophilus LA 201) twice daily for 10 days alongside standard antibiotic therapy was compared with antibiotic therapy alone in a randomized controlled trial that included 84 participants with acute uncomplicated diverticulitis. Those who received the probiotic mixture had greater reductions in abdominal pain and inflammation (Petruzziello, Marannino 2019). In a randomized controlled trial in which antibiotics were not used, 119 acute uncomplicated diverticulitis patients received either 500 million CFUs L. reuteri ATCC PTA 4659 or placebo twice daily, along with fluids and bowel rest, for 10 days. At the end of the trial, the probiotic group had lower levels of blood C-reactive protein and fecal calprotectin, as well as shorter hospital stays compared with placebo (Ojetti 2022).
Butyrate
Butyrate is a short-chain fatty acid produced in humans by intestinal bacteria that digest and metabolize fiber. Butyrate is critical to colonic mucosal health; is the preferred fuel of the cells that line the interior of the colon; helps maintain the intestinal barrier; has anti-inflammatory and anti-cancer effects; and helps regulate colonic motility (Slavin 2013; Leonel 2012; Sossai 2012).
In a randomized clinical trial of sodium butyrate in 52 people with diverticular disease, subjects received either a twice daily dose of 150 mg of oral microencapsulated sodium butyrate or placebo. After one year, just 7% of those in the butyrate group experienced diverticulitis symptoms compared with 31% in the placebo group (Krokowicz, Stojcev 2014).
A preclinical trial studied the effect of calcium butyrate introduced directly into the colon of rodents in an induced model of inflammatory bowel disease (IBD). Calcium butyrate completely prevented the weight loss typical of rats with induced colitis and significantly reduced the tissue damage and fluid accumulation of colitis, by 48% and 22.7%, respectively. In a laboratory component of this study, calcium butyrate also exhibited antitumor effects (Celasco 2014).
Clinical studies have shown that butyrate, in the form of sodium butyrate, reduced the frequency of symptoms of irritable bowel syndrome and eased traveler’s diarrhea (Banasiewicz 2013; Krokowicz, Kaczmarek 2014). It has been proposed that supplemental butyrate may be beneficial in IBD as well as colorectal cancer and certain metabolic diseases (Sossai 2012).
Anti-inflammatory Agents
Natural anti-inflammatory compounds may counteract some of the inflammatory processes that contribute to diverticular disease. These include the omega-3 fatty acids from fish, eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA); curcumin from the turmeric plant, Curcuma longa; and Boswellia serrata extract. Clinical trials to evaluate the specific effect of these natural anti-inflammatory agents in diverticular disease are still needed.
Omega-3 fatty acids. EPA and DHA have been extensively studied for their general anti-inflammatory activity, and many studies have demonstrated that omega-3 fats are beneficial in IBD (Farrukh 2014). Low levels of omega-3 fats have been found in patients with IBD, and almost all trials using fish oil supplements have demonstrated a beneficial effect, with the best results in ulcerative colitis (Farrukh 2014; Siguel 1996).
Emerging evidence suggests an overlap between the inflammation that characterizes chronic diverticular disease and that of IBD (Peppercorn 2004; Strate, Modi 2012). For this reason, treatments that are of benefit in IBD are worthy of consideration in diverticular disease. Several university-associated medical centers recommend supplementing omega-3 fatty acids, including from fish oil, in diverticular disease, in doses ranging from 1–5.5 g per day (UMMC 2013; PSH 2015; LHMC 2015).
Curcumin. Curcumin is an anti-inflammatory compound from the culinary and medicinal herb turmeric (Curcuma longa) (Iqbal 2003). Preclinical studies suggest curcumin may be of benefit in inflammatory bowel disease including ulcerative colitis. Studies in animal models of IBD have shown that curcumin can inhibit tumor necrosis factor-alpha, one of the inflammatory chemical messengers associated with diverticular disease and acute diverticulitis (Tursi, Elisei 2012; Tursi, Elisei, Giorgetti 2014). Early research suggests curcumin is safe and effective at preventing relapse when used with anti-inflammatory drugs to manage IBD (Baliga 2012).
Boswellia extract. Resin from the Boswellia serrata tree contains a powerful anti-inflammatory compound called acetyl-11-keto-β-boswellic acid, or AKBA (Siddiqui 2011). One randomized controlled trial found that Boswellia extract was as effective as mesalamine at improving symptoms of Crohn’s disease with far fewer side effects (Gerhardt 2001). In another trial, Boswellia extract was compared to the medication sulfasalazine (Azulfidine) in 30 patients with chronic colitis. Seventy percent of those treated with Boswellia extract entered remission compared to only 40% in the sulfasalazine group (Gupta 2001). This confirmed an earlier report of Boswellia’s efficacy in the treatment of ulcerative colitis (Gupta 1997). In a preclinical model of intestinal inflammation, both Boswellia extract and pure AKBA protected against oxidative damage and prevented inflammatory, structural, and functional changes in cells of the intestinal lining that were exposed to inflammatory stimuli (Catanzaro 2015). An improved extract, called AprèsFlex, or Aflapin, which combines AKBA with other non-volatile Boswellia oils, has demonstrated improved anti-inflammatory activity at a lower concentration when compared to other preparations standardized to the same percentage of AKBA (Sengupta 2011).
Additional Support
L-glutamine . The amino acid L-glutamine is an important energy source for cells that line the intestinal mucosa (Peng 2004; Fleming 1997). L-glutamine has been extensively studied for its ability to preserve structural and functional health of the intestine, and to promote intestinal recovery during and after injury or stress, such as occurs in infection or surgery. Animal and laboratory studies show the potential for L-glutamine, by protecting cells from inflammatory damage, to be a useful therapeutic for IBD (Xue 2011). Because of the relationship between chronic mucosal inflammation and diverticular disease, and the frank tissue injury that occurs with acute diverticulitis, L-glutamine may also be helpful in treating these conditions; however, clinical studies are needed to clarify the therapeutic role of L-glutamine in diverticular disease.
Mucilaginous herbs. Mucilages are complex sugars found in many plants that form a thick, gel-like film when mixed with water (Watts 2012). Psyllium seed husk (Plantago psyllium), flaxseed (Linum usitatissimum), and the medicinal plants slippery elm (Ulmus fulva) and licorice (Glycyrrhiza glabra) contain mucilage (Saeedi 2010; Dugani 2008; Gill 1946; Shenefelt 2011; Alok 2014).
When ingested, mucilages are believed to form a barrier or lining on the intestinal mucosa, protecting against infection and injury, soothing irritation, and promoting tissue healing (Pengelly 2006). Slippery elm bark, for example, has demonstrated anti-inflammatory effects in laboratory studies, and appears to protect against mucosal hypersensitivity in animal studies, while deglycyrrhizinated licorice (DGL) has demonstrated an ability to help heal peptic ulcers (Langmead 2002; Watts 2012). These protective properties of mucilaginous herbs may play a role in helping soothe and heal irritated or inflamed tissues lining the digestive tract in diverticular disease; however, clinical trials demonstrating such beneficial effects are needed.
|
Readers of this protocol should also review the Inflammatory Bowel Disease protocol, which describes several nutrients with anti-inflammatory activity that may be of benefit in conditions involving intestinal inflammation. Although the nutrients described in the Inflammatory Bowel Disease protocol may not have been directly studied in people with diverticular disease, the emergence of inflammation as an important mediator of diverticular problems suggests that supplementation with nutrients possessing anti-inflammatory properties may be helpful. |
Disclaimer and Safety Information
This information (and any accompanying material) is not intended to replace the attention or advice of a physician or other qualified health care professional. Anyone who wishes to embark on any dietary, drug, exercise, or other lifestyle change intended to prevent or treat a specific disease or condition should first consult with and seek clearance from a physician or other qualified health care professional. Pregnant women in particular should seek the advice of a physician before using any protocol listed on this website. The protocols described on this website are for adults only, unless otherwise specified. Product labels may contain important safety information and the most recent product information provided by the product manufacturers should be carefully reviewed prior to use to verify the dose, administration, and contraindications. National, state, and local laws may vary regarding the use and application of many of the therapies discussed. The reader assumes the risk of any injuries. The authors and publishers, their affiliates and assigns are not liable for any injury and/or damage to persons arising from this protocol and expressly disclaim responsibility for any adverse effects resulting from the use of the information contained herein.
The protocols raise many issues that are subject to change as new data emerge. None of our suggested protocol regimens can guarantee health benefits. Life Extension has not performed independent verification of the data contained in the referenced materials, and expressly disclaims responsibility for any error in the literature.
References
Aldoori W, Ryan-Harshman M. Preventing diverticular disease. Review of recent evidence on high-fibre diets. Canadian family physician Medecin de famille canadien. Oct 2002;48:1632-1637.
Aldoori WH, Giovannucci EL, Rimm EB, Ascherio A, Stampfer MJ, Colditz GA, . . . Willett WC. Prospective study of physical activity and the risk of symptomatic diverticular disease in men. Gut. Feb 1995;36(2):276-282.
Aldoori WH, Giovannucci EL, Rimm EB, Wing AL, Trichopoulos DV, Willett WC. A prospective study of alcohol, smoking, caffeine, and the risk of symptomatic diverticular disease in men. Annals of epidemiology. May 1995;5(3):221-228.
Aldoori WH, Giovannucci EL, Rockett HR, Sampson L, Rimm EB, Willett WC. A prospective study of dietary fiber types and symptomatic diverticular disease in men. The Journal of nutrition. Apr 1998;128(4):714-719.
Alok S, Jain SK, Verma A, Kumar M, Mahor A, Sabharwal M. Herbal antioxidant in clinical practice: a review. Asian Pac J Trop Biomed. Jan 2014;4(1):78-84.
Andersen JC, Bundgaard L, Elbrond H, Laurberg S, Walker LR, Stovring J. Danish national guidelines for treatment of diverticular disease. Danish medical journal. May 2012;59(5):C4453.
Andeweg CS, Wegdam JA, Groenewoud J, van der Wilt GJ, van Goor H, Bleichrodt RP. Toward an evidence-based step-up approach in diagnosing diverticulitis. Scandinavian journal of gastroenterology. Jul 2014;49(7):775-784.
Annibale B, Maconi G, Lahner E, De Giorgi F, Cuomo R. Efficacy of Lactobacillus paracasei sub. paracasei F19 on abdominal symptoms in patients with symptomatic uncomplicated diverticular disease: a pilot study. Minerva gastroenterologica e dietologica. Mar 2011;57(1):13-22.
Asadollahi K, Hastings IM, Beeching NJ, Gill GV, Asadollahi P. Leukocytosis as an alarming sign for mortality in patients hospitalized in general wards. Iranian journal of medical sciences. Mar 2011;36(1):45-49.
Aydin N, Lauer GM, Pollak RF. First Consult. Diverticular disease. Available at: www.clinicalkey.com. Last updated 5/1/2012. Accessed 2/20/2015.
Baliga MS, Joseph N, Venkataranganna MV, Saxena A, Ponemone V, Fayad R. Curcumin, an active component of turmeric in the prevention and treatment of ulcerative colitis: preclinical and clinical observations. Food & function. Nov 2012;3(11):1109-1117.
Banasiewicz T, Krokowicz L, Stojcev Z, Kaczmarek BF, Kaczmarek E, Maik J, . . . Drews M. Microencapsulated sodium butyrate reduces the frequency of abdominal pain in patients with irritable bowel syndrome. Colorectal disease : the official journal of the Association of Coloproctology of Great Britain and Ireland. Feb 2013;15(2):204-209.
Bianchi M, Festa V, Moretti A, Ciaco A, Mangone M, Tornatore V, . . . Koch M. Meta-analysis: long-term therapy with rifaximin in the management of uncomplicated diverticular disease. Alimentary pharmacology & therapeutics. Apr 2011;33(8):902-910.
Bose KP, Khorshidi I, Southern WN, Brandt LJ. The impact of ethnicity and obesity on the course of colonic diverticulitis. Journal of clinical gastroenterology. Feb 2013;47(2):160-164.
Boynton W, Floch M. New strategies for the management of diverticular disease: insights for the clinician. Therapeutic advances in gastroenterology. May 2013;6(3):205-213.
Bretto E, D'Amico F, Fiore W, Tursi A, Danese S. Lactobacillus paracasei CNCM I 1572: A Promising Candidate for Management of Colonic Diverticular Disease. J Clin Med. Mar 30 2022;11(7)doi:10.3390/jcm11071916
Bugiantella W, Rondelli F, Longaroni M, Mariani E, Sanguinetti A, Avenia N. Left colon acute diverticulitis: An update on diagnosis, treatment and prevention. International journal of surgery (London, England). Jan 2015;13c:157-164.
Burri E, Beglinger C. The use of fecal calprotectin as a biomarker in gastrointestinal disease. Expert review of gastroenterology & hepatology. Feb 2014;8(2):197-210.
Catanzaro D, Rancan S, Orso G, et al. Boswellia serrata Preserves Intestinal Epithelial Barrier from Oxidative and Inflammatory Damage. PLoS One. 2015;10(5):e0125375.
CCFA. Crohn’s & Colitis Foundation of America. Aminosalicylates. Available at: http://www.ccfa.org/assets/pdfs/aminosalicylates.pdf. 10/2013. Accessed 5/6/2015.
Celasco G, Moro L, Aiello C, Mangano K, Milasi A, Quattrocchi C, R DIM. Calcium butyrate: Anti-inflammatory effect on experimental colitis in rats and antitumor properties. Biomed Rep. Jul 2014;2(4):559-563.
Cianci R, Frosali S, Pagliari D, Cesaro P, Petruzziello L, Casciano F, . . . Pandolfi F. Uncomplicated diverticular disease: innate and adaptive immunity in human gut mucosa before and after rifaximin. J Immunol Res. 2014;2014:696812.
Collins D, Winter DC. Modern concepts in diverticular disease. Journal of clinical gastroenterology. May-Jun 2015;49(5):358-369.
Comstock SS, Lewis MM, Pathak DR, Hortos K, Kovan B, Fenton JI. Cross-sectional analysis of obesity and serum analytes in males identifies sRAGE as a novel biomarker inversely associated with diverticulosis. PloS one. 2014;9(4):e95232.
Crowe FL, Appleby PN, Allen NE, Key TJ. Diet and risk of diverticular disease in Oxford cohort of European Prospective Investigation into Cancer and Nutrition (EPIC): prospective study of British vegetarians and non-vegetarians. BMJ (Clinical research ed.). 2011;343:d4131.
Cuomo R, Barbara G, Pace F, Annese V, Bassotti G, Binda GA, . . . Annibale B. Italian consensus conference for colonic diverticulosis and diverticular disease. United European Gastroenterol J. Oct 2014;2(5):413-442.
de Korte N, Unlu C, Boermeester MA, Cuesta MA, Vrouenreats BC, Stockmann HB. Use of antibiotics in uncomplicated diverticulitis. The British journal of surgery. Jun 2011;98(6):761-767.
Dobbins C, Defontgalland D, Duthie G, Wattchow DA. The relationship of obesity to the complications of diverticular disease. Colorectal disease : the official journal of the Association of Coloproctology of Great Britain and Ireland. Jan 2006;8(1):37-40.
Dugani A, Auzzi A, Naas F, Megwez S. Effects of the oil and mucilage from flaxseed (linum usitatissimum) on gastric lesions induced by ethanol in rats. The Libyan journal of medicine. 2008;3(4):166-169.
Erbayrak M, Turkay C, Eraslan E, Cetinkaya H, Kasapoglu B, Bektas M. The role of fecal calprotectin in investigating inflammatory bowel diseases. Clinics (Sao Paulo, Brazil). May 2009;64(5):421-425.
Farrukh A, Mayberry JF. Is there a role for fish oil in inflammatory bowel disease? World journal of clinical cases. Jul 16 2014;2(7):250-252.
Fengming Y, Jianbing W. Biomarkers of inflammatory bowel disease. Disease markers. 2014;2014:710915.
Ferri FF. Ferri's Clinical Advisor. Diverticular Disease (Diverticulosis, Diverticulitis). Available at: www.clinicalkey.com. 2015. Accessed 2/20/2015.
Fleming SE, Zambell KL, Fitch MD. Glucose and glutamine provide similar proportions of energy to mucosal cells of rat small intestine. The American journal of physiology. Oct 1997;273(4 Pt 1):G968-978.
Franklin ME, Jr., Portillo G, Trevino JM, Gonzalez JJ, Glass JL. Long-term experience with the laparoscopic approach to perforated diverticulitis plus generalized peritonitis. World journal of surgery. Jul 2008;32(7):1507-1511.
Gatta L, Vakil N, Vaira D, Pilotto A, Curlo M, Comparato G, . . . Di Mario F. Efficacy of 5-ASA in the treatment of colonic diverticular disease. Journal of clinical gastroenterology. Feb 2010;44(2):113-119.
Gerhardt H, Seifert F, Buvari P, et al. [Therapy of active Crohn disease and Boswellia serrata extract H 15]. Z Gastroenterol. 2001;39(1):11-7.
Gill RE, Hirst EL, Jones JK. Constitution of the mucilage from the bark of Ulmus fulva (slippery elm mucilage); the sugars formed in the hydrolysis of the methylated mucilage. Journal of the Chemical Society. Nov 1946:1025-1029.
Gold Standard. Drug Monograph: Rifaximin. Available at: www.clinicalkey.com. Last updated 4/14/2014. Accessed 5/28/2015.
Gupta I, Parihar A, Malhotra P, et al. Effects of Boswellia serrata gum resin in patients with ulcerative colitis. Eur J Med Res. 1997;2(1):37-43.
Gupta I, Parihar A, Malhotra P, et al. Effects of gum resin of Boswellia serrata in patients with chronic colitis. Planta Med. 2001;67(5):391-5.
Henderson P, Anderson NH, Wilson DC. The diagnostic accuracy of fecal calprotectin during the investigation of suspected pediatric inflammatory bowel disease: a systematic review and meta-analysis. Am J Gastroenterol. May 2014;109(5):637-645.
Hjern F, Josephson T, Altman D, Holmstrom B, Mellgren A, Pollack J, Johansson C. Conservative treatment of acute colonic diverticulitis: are antibiotics always mandatory? Scandinavian journal of gastroenterology. Jan 2007;42(1):41-47.
Hjern F, Mahmood MW, Abraham-Nordling M, Wolk A, Hakansson N. Cohort study of corticosteroid use and risk of hospital admission for diverticular disease. The British journal of surgery. Jan 2015;102(1):119-124.
Hjern F, Wolk A, Hakansson N. Obesity, physical inactivity, and colonic diverticular disease requiring hospitalization in women: a prospective cohort study. Am J Gastroenterol. Feb 2012;107(2):296-302.
Hjern F, Wolk A, Hakansson N. Smoking and the risk of diverticular disease in women. The British journal of surgery. Jul 2011;98(7):997-1002.
Hobson KG, Roberts PL. Etiology and pathophysiology of diverticular disease. Clinics in colon and rectal surgery. Aug 2004;17(3):147-153.
Humes DJ, Spiller RC. Review article: The pathogenesis and management of acute colonic diverticulitis. Alimentary pharmacology & therapeutics. Feb 2014;39(4):359-370.
Iqbal M, Sharma SD, Okazaki Y, Fujisawa M, Okada S. Dietary supplementation of curcumin enhances antioxidant and phase II metabolizing enzymes in ddY male mice: possible role in protection against chemical carcinogenesis and toxicity. Pharmacology & toxicology. Jan 2003;92(1):33-38.
Jung HK, Choung RS, Locke GR, 3rd, Schleck CD, Zinsmeister AR, Talley NJ. Diarrhea-predominant irritable bowel syndrome is associated with diverticular disease: a population-based study. Am J Gastroenterol. Mar 2010;105(3):652-661.
Köckerling F. Emergency Surgery for Acute Complicated Diverticulitis. Viszeralmedizin. 2015;31(2):107-110.
Krokowicz L, Kaczmarek BF, Krokowicz P, Stojcev Z, Mackiewicz J, Walkowiak J, . . . Banasiewicz T. Sodium butyrate and short chain fatty acids in prevention of travellers' diarrhoea: a randomized prospective study. Travel Med Infect Dis. Mar-Apr 2014;12(2):183-188.
Krokowicz L, Stojcev Z, Kaczmarek BF, Kociemba W, Kaczmarek E, Walkowiak J, . . . Banasiewicz T. Microencapsulated sodium butyrate administered to patients with diverticulosis decreases incidence of diverticulitis--a prospective randomized study. International journal of colorectal disease. Mar 2014;29(3):387-393.
Kruse E, Leifeld L. [Prevention and conservative therapy of diverticular disease]. Der Chirurg; Zeitschrift fur alle Gebiete der operativen Medizen. Apr 2014;85(4):299-303.
Kvasnovsky CL, Papagrigoriadis S, Bjarnason I. Increased diverticular complications with nonsteriodal anti-inflammatory drugs and other medications: a systematic review and meta-analysis. Colorectal disease : the official journal of the Association of Coloproctology of Great Britain and Ireland. Jun 2014;16(6):O189-196.
Lahner E, Esposito G, Zullo A, Hassan C, Cannaviello C, Paolo MC, . . . Annibale B. High-fibre diet and Lactobacillus paracasei B21060 in symptomatic uncomplicated diverticular disease. World journal of gastroenterology : WJG. Nov 7 2012;18(41):5918-5924.
Lamiki P, Tsuchiya J, Pathak S, Okura R, Solimene U, Jain S, . . . Marotta F. Probiotics in diverticular disease of the colon: an open label study. Journal of gastrointestinal and liver diseases : JGLD. Mar 2010;19(1):31-36.
Langmead L, Dawson C, Hawkins C, Banna N, Loo S, Rampton DS. Antioxidant effects of herbal therapies used by patients with inflammatory bowel disease: an in vitro study. Alimentary pharmacology & therapeutics. Feb 2002;16(2):197-205.
Leonel AJ, Alvarez-Leite JI. Butyrate: implications for intestinal function. Current opinion in clinical nutrition and metabolic care. Sep 2012;15(5):474-479.
LHMC. Lahey Hospital & Medical Center. Fish Oil. Available at: https://lahey.org/Departments_and_Locations/Departments/Colon_and_Rectal_Surgery/Ebsco_Content/Diverticular_Disease/Diverticulitis.aspx?chunkiid=21684. Copyright 2015 EBSCO Publishing. Accessed 5/8/2015.
Lizardi-Cervera J, Vazquez-Elizondo G, Becerra-Laparra I, Chavez-Tapia N, Noriega-Iriondo MF, Uribe M. [Comparative study of the clinical presentation and complications of acute colonic diverticulitis in patients older and younger than 65 years.]. Revista de gastroenterologia de Mexico. 2008;73(3):153-158.
Mann NS, Hoda KK. Segmental colitis associated with diverticulosis: systematic evaluation of 486 cases with meta-analysis. Hepato-gastroenterology. Oct 2012;59(119):2119-2121.
Maykel JA, Opelka FG. Colonic diverticulosis and diverticular hemorrhage. Clinics in colon and rectal surgery. Aug 2004;17(3):195-204.
Mayo Clinic. Patient Care & Health Info page. Diseases and Conditions. Diverticulitis. Definition. Available at: http://www.mayoclinic.org/diseases-conditions/diverticulitis/basics/definition/con-20033495. 8/7/2014a. Accessed 5/26/2015.
Mayo Clinic. Patient Care & Health Info page. Nutrition and healthy eating. Diverticulitis diet. Available at: http://www.mayoclinic.org/healthy-lifestyle/nutrition-and-healthy-eating/in-depth/diverticulitis-diet/art-20048499. 4/13/2014b. Accessed 5/6/2015.
McDermott FD, Collins D, Heeney A, Winter DC. Minimally invasive and surgical management strategies tailored to the severity of acute diverticulitis. The British journal of surgery. Jan 2014;101(1):e90-99.
Medina-Fernandez FJ, Diaz-Jimenez N, Gallardo-Herrera AB, Gomez-Luque I, Garcilazo-Arsimendi DJ, Gomez-Barbadillo J. New trends in the management of diverticulitis and colonic diverticular disease. Revista espanola de enfermedades digestivas : organo oficial de la Sociedad Espanola de Patologia Digestiva. Mar 2015;107(3):162-170.
Morris AM, Regenbogen SE, Hardiman KM, Hendren S. Sigmoid diverticulitis: a systematic review. JAMA : the journal of the American Medical Association. Jan 15 2014;311(3):287-297.
Mosadeghi S, Bhuket T, Stollman N. Diverticular disease: evolving concepts in classification, presentation, and management. Current opinion in gastroenterology. Jan 2015;31(1):50-55.
Nagata N, Niikura R, Shimbo T, Kishida Y, Sekine K, Tanaka S, . . . Uemura N. Alcohol and smoking affect risk of uncomplicated colonic diverticulosis in Japan. PloS one. 2013;8(12):e81137.
Nagata N, Sakamoto K, Arai T, Niikura R, Shimbo T, Shinozaki M, . . . Uemura N. Visceral Abdominal Obesity Measured by Computed Tomography is Associated With Increased Risk of Colonic Diverticulosis. Journal of clinical gastroenterology. Nov 19 2014.
NIDDK. National Institute of Diabetes and Digestive and Kidney Diseases. What I need to know about Diverticular Disease. Available at: http://www.niddk.nih.gov/health-information/health-topics/digestive-diseases/diverticular-disease/Pages/ez.aspx . Last updated 5/10/2012. Accessed 4/8/2015.
Ojetti V, Saviano A, Brigida M, et al. Randomized control trial on the efficacy of Limosilactobacillus reuteri ATCC PTA 4659 in reducing inflammatory markers in acute uncomplicated diverticulitis. European journal of gastroenterology & hepatology. May 1 2022;34(5):496-502. doi:10.1097/meg.0000000000002342
Papagrigoriadis S, Macey L, Bourantas N, Rennie JA. Smoking may be associated with complications in diverticular disease. The British journal of surgery. Jul 1999;86(7):923-926.
Peery AF, Sandler RS. Diverticular disease: reconsidering conventional wisdom. Clinical gastroenterology and hepatology : the official clinical practice journal of the American Gastroenterological Association. Dec 2013;11(12):1532-1537.
Peng X, Yan H, You Z, Wang P, Wang S. Effects of enteral supplementation with glutamine granules on intestinal mucosal barrier function in severe burned patients. Burns : journal of the International Society for Burn Injuries. Mar 2004;30(2):135-139.
Pengelly A. The Constituents of Medicinal Plants: An Introduction to the Chemistry and Therapeutics of Herbal Medicine, 2nd edition. Sydney, NSW, Australia: Allen and Unwin. 2006.
Peppercorn MA. The overlap of inflammatory bowel disease and diverticular disease. Journal of clinical gastroenterology. May-Jun 2004;38(5 Suppl 1):S8-10.
Petruzziello C, Marannino M, Migneco A, et al. The efficacy of a mix of three probiotic strains in reducing abdominal pain and inflammatory biomarkers in acute uncomplicated diverticulitis. European review for medical and pharmacological sciences. Oct 2019;23(20):9126-9133. doi:10.26355/eurrev_201910_19316
Petruzziello C, Migneco A, Cardone S, et al. Supplementation with Lactobacillus reuteri ATCC PTA 4659 in patients affected by acute uncomplicated diverticulitis: a randomized double-blind placebo controlled trial. International journal of colorectal disease. Jun 2019;34(6):1087-1094. doi:10.1007/s00384-019-03295-1
Piccioni A, Franza L, Brigida M, et al. Gut Microbiota and Acute Diverticulitis: Role of Probiotics in Management of This Delicate Pathophysiological Balance. J Pers Med. Apr 14 2021;11(4)doi:10.3390/jpm11040298
Piccioni A, Franza L, Vaccaro V, et al. Microbiota and Probiotics: The Role of Limosilactobacillus Reuteri in Diverticulitis. Medicina (Kaunas, Lithuania). Aug 5 2021;57(8)doi:10.3390/medicina57080802Pisanu A, Vacca V, Reccia I, Podda M, Uccheddu A. Acute diverticulitis in the young: the same disease in a different patient. Gastroenterology research and practice. 2013;2013:867961.
PSH. Penn State Hershey. Health Information Library. Diverticular disease. Available at: http://pennstatehershey.adam.com/content.aspx?productId=107&pid=33&gid=000051. 3/25/2015. Accessed 5/8/2015.
Razik R, Nguyen GC. Diverticular Disease: Changing Epidemiology and Management. Drugs & aging. Apr 18 2015.
Regenbogen SE, Hardiman KM, Hendren S, Morris AM. Surgery for diverticulitis in the 21st century: a systematic review. JAMA surgery. Mar 2014;149(3):292-303.
Ren Z, Hong Y, Huo Y, et al. Prospects of Probiotic Adjuvant Drugs in Clinical Treatment. Nutrients. Nov 9 2022;14(22)doi:10.3390/nu14224723
Saeedi M, Morteza-Semnani K, Ansoroudi F, Fallah S, Amin G. Evaluation of binding properties of Plantago psyllium seed mucilage. Acta pharmaceutica (Zagreb, Croatia). Sep 2010;60(3):339-348.
Saul N. Ask the Expert topics. page. Copyright 2015 National Women's Health Resource Center. Available at: http://www.healthywomen.org/content/ask-expert/1572/caffeine-and-diverticulitis. Accessed 5/6/2015.
Schaffzin DM, Wong WD. Nonoperative management of complicated diverticular disease. Clinics in colon and rectal surgery. Aug 2004;17(3):169-176.
Sengupta K, Kolla JN, Krishnaraju AV, et al. Cellular and molecular mechanisms of anti-inflammatory effect of Aflapin: a novel Boswellia serrata extract. Mol Cell Biochem. 2011;354(1-2):189-97.
Shahedi K, Fuller G, Bolus R, Cohen E, Vu M, Shah R, . . . Spiegel B. Long-term risk of acute diverticulitis among patients with incidental diverticulosis found during colonoscopy. Clinical gastroenterology and hepatology : the official clinical practice journal of the American Gastroenterological Association. Dec 2013;11(12):1609-1613.
Sheiman L, Levine MS, Levin AA, Hogan J, Rubesin SE, Furth EE, Laufer I. Chronic diverticulitis: clinical, radiographic, and pathologic findings. AJR. American journal of roentgenology. Aug 2008;191(2):522-528.
Shenefelt PD, Benzie IFF, Wachtel-Galor S (eds.). Chapter 18: Herbal Treatment for Dermatologic Disorders. In: Herbal Medicine: Biomolecular and Clinical Aspects. 2nd edition. Copyright 2011 CRC Press. <http://www.ncbi.nlm.nih.gov/books/NBK92761/>.
Siddiqui MZ. Boswellia Serrata, A Potential Antiinflammatory Agent: An Overview. Indian J Pharm Sci. 2011;73(3):255-261.
Siguel EN, Lerman RH. Prevalence of essential fatty acid deficiency in patients with chronic gastrointestinal disorders. Metabolism: clinical and experimental. Jan 1996;45(1):12-23.
Slavin J. Fiber and Prebiotics: Mechanisms and Health Benefits. Nutrients. 2013;5(4):1417-1435.
Sopena F, Lanas A. Management of colonic diverticular disease with poorly absorbed antibiotics and other therapies. Therapeutic advances in gastroenterology. Nov 2011;4(6):365-374.
Sorser SA, Hazan TB, Piper M, Maas LC. Obesity and complicated diverticular disease: is there an association? Southern medical journal. Apr 2009;102(4):350-353.
Sossai P. Butyric acid: what is the future for this old substance? Swiss medical weekly. 2012;142:w13596.
Spiller R. Editorial: new thoughts on the association between diverticulosis and irritable bowel syndrome. Am J Gastroenterol. Dec 2014;109(12):1906-1908.
Spiller R. Is it diverticular disease or is it irritable bowel syndrome? Digestive diseases (Basel, Switzerland). 2012;30(1):64-69.
Spiller RC. Changing views on diverticular disease: impact of aging, obesity, diet, and microbiota. Neurogastroenterology and motility : the official journal of the European Gastrointestinal Motility Society. Mar 2015;27(3):305-312.
Stollman N, Magowan S, Shanahan F, Quigley EM. A randomized controlled study of mesalamine after acute diverticulitis: results of the DIVA trial. Journal of clinical gastroenterology. Aug 2013;47(7):621-629.
Strate LL, Liu YL, Aldoori WH, Giovannucci EL. Physical activity decreases diverticular complications. Am J Gastroenterol. May 2009;104(5):1221-1230.
Strate LL, Liu YL, Aldoori WH, Syngal S, Giovannucci EL. Obesity increases the risks of diverticulitis and diverticular bleeding. Gastroenterology. Jan 2009;136(1):115-122.e111.
Strate LL, Liu YL, Huang ES, Giovannucci EL, Chan AT. Use of aspirin or nonsteroidal anti-inflammatory drugs increases risk for diverticulitis and diverticular bleeding. Gastroenterology. May 2011;140(5):1427-1433.
Strate LL, Liu YL, Syngal S, Aldoori WH, Giovannucci EL. Nut, corn, and popcorn consumption and the incidence of diverticular disease. JAMA : the journal of the American Medical Association. Aug 27 2008;300(8):907-914.
Strate LL, Modi R, Cohen E, Spiegel BM. Diverticular disease as a chronic illness: evolving epidemiologic and clinical insights. Am J Gastroenterol. Oct 2012;107(10):1486-1493.
Strate LL. Lifestyle factors and the course of diverticular disease. Digestive diseases (Basel, Switzerland). 2012;30(1):35-45.
Telem DA, Buch KE, Nguyen SQ, Chin EH, Weber KJ, Divino CM. Current recommendations on diagnosis and management of right-sided diverticulitis. Gastroenterology research and practice. 2009;2009:359485.
Thaha MA, Williams NS. ePocrates. Diverticular disease. Available at: https://online.epocrates.com/noFrame/showPage?method=diseases&MonographId=16. Last updated 1/5/2015. Accessed 2/20/2015.
Turley RS, Mantyh CR, Migaly J. Minimally invasive surgery for diverticulitis. Techniques in coloproctology. Feb 2013;17 Suppl 1:S11-22.
Tursi A, Brandimarte G, Elisei W, Giorgetti GM, Inchingolo CD, Aiello F. Faecal calprotectin in colonic diverticular disease: a case-control study. International journal of colorectal disease. Jan 2009;24(1):49-55.
Tursi A, Brandimarte G, Elisei W, Picchio M, Forti G, Pianese G, . . . Danese S. Randomised clinical trial: mesalazine and/or probiotics in maintaining remission of symptomatic uncomplicated diverticular disease--a double-blind, randomised, placebo-controlled study. Alimentary pharmacology & therapeutics. Oct 2013;38(7):741-751.
Tursi A, Brandimarte G, Giorgetti GM, Elisei W. Mesalazine and/or Lactobacillus casei in maintaining long-term remission of symptomatic uncomplicated diverticular disease of the colon. Hepato-gastroenterology. May-Jun 2008;55(84):916-920.
Tursi A, Brandimarte G, Giorgetti GM, Elisei W. Mesalazine and/or Lactobacillus casei in preventing recurrence of symptomatic uncomplicated diverticular disease of the colon: a prospective, randomized, open-label study. Journal of clinical gastroenterology. Apr 2006;40(4):312-316.
Tursi A, Elisei W, Brandimarte G, Giorgetti GM, Inchingolo CD, Nenna R, . . . Ierardi E. Mucosal expression of basic fibroblastic growth factor, Syndecan 1 and tumor necrosis factor-alpha in diverticular disease of the colon: a case-control study. Neurogastroenterology and motility : the official journal of the European Gastrointestinal Motility Society. Sep 2012;24(9):836-e396.
Tursi A, Elisei W, Giorgetti G, Aiello F, Brandimarte G. Role of fecal calprotectin in the diagnosis and treatment of segmental colitis associated with diverticulosis. Minerva gastroenterologica e dietologica. Sep 2011;57(3):247-255.
Tursi A, Elisei W, Giorgetti GM, Inchingolo CD, Nenna R, Picchio M, . . . Brandimarte G. Expression of basic fibroblastic growth factor, syndecan 1 and tumour necrosis factor alpha in resected acute colonic diverticulitis. Colorectal disease : the official journal of the Association of Coloproctology of Great Britain and Ireland. Mar 2014;16(3):O98-103.
Tursi A, Elisei W, Picchio M, Brandimarte G. Increased faecal calprotectin predicts recurrence of colonic diverticulitis. International journal of colorectal disease. Aug 2014;29(8):931-935.
Tursi A, Elisei W, Picchio M, Giorgetti GM, Brandimarte G. Moderate to Severe and Prolonged Left Lower-abdominal Pain is the Best Symptom Characterizing Symptomatic Uncomplicated Diverticular Disease of the Colon: A Comparison With Fecal Calprotectin in Clinical Setting. Journal of clinical gastroenterology. Mar 2015;49(3):218-221.
Tursi A. Advances in the management of colonic diverticulitis. CMAJ : Canadian Medical Association journal = journal de l'Association medicale canadienne. Sep 18 2012;184(13):1470-1476.
Tursi A. Diverticular disease of the colon and irritable bowel syndrome: it is time to differentiate. Am J Gastroenterol. May 2015;110(5):774-775.
Tursi A. Diverticular disease: A therapeutic overview. World journal of gastrointestinal pharmacology and therapeutics. Feb 6 2010;1(1):27-35.
Tursi A. New physiopathological and therapeutic approaches to diverticular disease: an update. Expert opinion on pharmacotherapy. May 2014;15(7):1005-1017.
Tursi A, Papa V, Lopetuso LR, Settanni CR, Gasbarrini A, Papa A. Microbiota Composition in Diverticular Disease: Implications for Therapy. International journal of molecular sciences. Nov 26 2022;23(23)doi:10.3390/ijms232314799
Turunen P, Wikstrom H, Carpelan-Holmstrom M, Kairaluoma P, Kruuna O, Scheinin T. Smoking increases the incidence of complicated diverticular disease of the sigmoid colon. Scandinavian journal of surgery : SJS : official organ for the Finnish Surgical Society and the Scandinavian Surgical Society. 2010;99(1):14-17.
UMMC. University of Maryland Medical Center. Medical Reference Guide: Complementary and Alternative Medicine Guide: Condition: Diverticular Disease. Available at http://umm.edu/health/medical/altmed/condition/diverticular-disease. Last udated 07/01/2013. Accessed 03/23/2015.
Unlu C, Daniels L, Vrouenraets BC, Boermeester MA. A systematic review of high-fibre dietary therapy in diverticular disease. International journal of colorectal disease. Apr 2012;27(4):419-427.
von Rahden BH, Germer CT. Pathogenesis of colonic diverticular disease. Langenbeck's archives of surgery / Deutsche Gesellschaft fur Chirurgie. Oct 2012;397(7):1025-1033.
Watts CR. Slippery Elm, its biochemistry and use as a complementary and alternative treatment for laryngeal irritation. Journal of Investigational Biochemistry. 2012;1(1):17-23.
Wick JY. Diverticular disease: eat your fiber! The Consultant pharmacist : the journal of the American Society of Consultant Pharmacists. Sep 2012;27(9):613-618.
Wilkins T, Embry K, George R. Diagnosis and management of acute diverticulitis. American family physician. May 1 2013;87(9):612-620.
Williams PT. Incident diverticular disease is inversely related to vigorous physical activity. Medicine and science in sports and exercise. May 2009;41(5):1042-1047.
Xue H, Sufit AJ, Wischmeyer PE. Glutamine therapy improves outcome of in vitro and in vivo experimental colitis models. JPEN. Journal of parenteral and enteral nutrition. Mar 2011;35(2):188-197.
Yamada E, Inamori M, Uchida E, Tanida E, Izumi M, Takeshita K, . . . Nakajima A. Association between the location of diverticular disease and the irritable bowel syndrome: a multicenter study in Japan. Am J Gastroenterol. Dec 2014;109(12):1900-1905.
