
Arthritis - Rheumatoid
Arthritis - Rheumatoid
Last Section Update: 03/2023
Contributor(s): Debra Gordon, MS; Shayna Sandhaus, PhD
Table of Contents
1 Overview
Summary and Quick Facts for Arthritis Rheumatoid
- Rheumatoid arthritis (RA) is a systemic inflammatory disease characterized by an autoimmune response that causes pain and disfigurement in peripheral joints. A dangerously underappreciated fact about RA is that it also significantly increases risk of cardiovascular disease.
- In this protocol, you will discover an advanced European drug delivery system that dramatically augments the efficacy and lessens the side effects of prednisone, a drug commonly used in the treatment of rheumatoid arthritis. You will also learn about oral tolerance – a unique, drug-free strategy that helps retrain the immune system to not attack the joints, as well as convenient blood tests and scientifically studied natural compounds that allow you to assess and target your cardiovascular risk.
- Too often, conventional treatment strategies yield only marginal relief and fall pitifully short of mitigating the systemic risks that threaten the longevity of RA patients. Initiating an aggressive cardiovascular risk reduction program should be as high a priority as relieving joint pain.
What is Rheumatoid Arthritis?
Rheumatoid arthritis (RA) is a systemic inflammatory disease that causes pain and disfigurement of peripheral joints. The disease may alternate between “flares” and periods of remission, but is generally progressive. Importantly, patients with RA are at a significantly higher risk of cardiovascular disease.
The disease is characterized by an autoimmune response that can damage joints and cause systemic inflammation. The inflammation is caused by the immune system mistakenly attacking the soft tissue in joints, causing damage and dysfunction.
Natural interventions like curcumin, Boswellia serrata extract, and white peony extract may help reduce inflammation and improve overall health in patients with RA.
What are the Signs and Symptoms of Rheumatoid Arthritis?
- Joint inflammation (swollen, warm, painful)—may be worse in the morning
- Fatigue
- Malaise
- Weight loss
- Damage to other areas of the body may occur as well. Some symptoms may include ulcers on the skin, coughing or shortness of breath, high cholesterol, and anemia.
What are the Conventional Medical Treatments for Rheumatoid Arthritis?
- Disease-modifying antirheumatic drugs (DMARDs) (eg, methotrexate and sulfasalazine)
- Glucocorticoids (eg, prednisone)
- Non-steroidal anti-inflammatory drugs (NSAIDs)
- Statins to prevent cardiovascular disease
What are Emerging Therapies for Rheumatoid Arthritis?
- Modified-release prednisone to improve on the action of conventional prednisone
- Stem cell treatment
- Bioidentical hormone replacement therapy
What Dietary and Lifestyle Changes Can Benefit Rheumatoid Arthritis?
- Avoid foods that cause sensitivities (elevated IgG antibodies)
- Exercise (dynamic aerobic exercise and/or strength training)
What Natural Interventions May Benefit Rheumatoid Arthritis?
- Undenatured type-II collagen. When immune cells encounter exposed joint collagen in RA patients, an autoimmune attack is launched, resulting in inflammation. Consuming undenatured type-II collagen may help the immune system develop “oral tolerance,” teaching the T cells to ignore collagen encountered in joints.
- Essential fatty acids. Omega-3 and certain omega-6 fatty acids are recommended for many RA patients because they can reduce inflammation and improve cardiovascular health. Fatty acids derived from fish oil have been shown to reduce RA pain and improve cholesterol and triglyceride levels.
- Vitamin D. Vitamin D plays an immunomodulatory role and can improve pain relief in RA patients taking DMARDs.
- Vitamin B6. Treatment with vitamin B6 reduced levels of pro-inflammatory cytokines in patients with RA. Patients with RA are also more likely to be deficient in vitamin B6.
- White peony extract. Multiple studies have shown that white peony extract has immunomodulatory, anti-inflammatory, and pain-relieving activity. The extract can reduce symptoms on its own and improve patient response to other treatments.
- Curcumin. Curcumin is a well-known anti-inflammatory compound. It has been shown to be as effective as an NSAID in treating RA-related activity.
- Boswellia serrata extract. The anti-inflammatory extract of the Boswellia sacra tree can improve joint flexion, reduce swelling, and prevent cartilage degradation in arthritic patients.
- Pomegranate. Pomegranates are rich in antioxidant polyphenols. Animal studies and small clinical trials have demonstrated pomegranate’s ability to help with arthritic pain and inflammation.
- Other plant extracts and compounds such as andrographis, green tea, ginger, and quercetin may help reduce inflammation as well.
- Supplemental forms of several endogenous compounds may be important for preventing inflammation and damage, including S-adenosyl-L-methionine (SAMe), glucosamine, and chondroitin sulfate.
2 Introduction
Rheumatoid arthritis (RA) is a systemic inflammatory disease characterized by an autoimmune response that causes pain and disfigurement in peripheral joints. A dangerously underappreciated fact about RA is that it also significantly increases risk of cardiovascular disease. Because systemic inflammation hastens the onset of most age-related diseases, individuals afflicted with RA have a nearly 40% increased risk of dying compared to healthy people (Khan 2010; Radovits 2010; Peters 2009).
Too often, conventional treatment strategies yield only marginal relief and fall pitifully short of mitigating the systemic risks that threaten the longevity of RA patients. Life Extension encourages both patients and physicians to view RA as a disease of the entire body, not just the joints. Initiating an aggressive cardiovascular risk reduction program should be as high a priority as relieving joint pain.
In this protocol, you will discover an advanced European drug delivery system that dramatically augments the efficacy and lessens the side effects of prednisone, a drug commonly used in the treatment of RA. You will also learn about oral tolerance – a unique, drug-free strategy that helps re-train the immune system to not attack the joints, as well as convenient blood tests and scientifically studied natural compounds that allow you to assess and target your cardiovascular risk.
3 Symptoms And Affected Tissues
The prominent feature of rheumatoid arthritis is joint inflammation. Affected joints are usually swollen, warm, painful and stiff. These symptoms typically worsen in the morning but, at least early in the disease process, can sometimes be eased by gentle movement. As the disease progresses, however, these symptoms often increase in severity until movement is severely impaired.
Inflammation associated with RA is systemic, meaning that it is not isolated to only those joints affected. RA tends to present symptoms in a symmetrical way. For example, if the joints of the right hand are inflamed, the joints of the left hand are likely to be inflamed as well (St. Clair 2004). While the hand and wrist joints are most often affected, other joints may be involved including those of the feet and ankles, knees, hips, elbows, shoulders, and the cervical spine (i.e., the neck) (Klippel 2010).
In general, the symptoms and severity of RA follow one of three patterns (Ruffing 2012):
- Spontaneous remission: The symptoms ultimately disappear, which occurs in less than 10% of patients with RA. This generally occurs only in patients whose blood tests are negative for a protein called rheumatoid factor (RF), an autoimmune mediator.
- Relapsing/remitting disease: The patient experiences periods of very severe symptoms called "flares", which are contrasted with episodes of mild or no symptoms. This pattern generally occurs early on in the course of the disease.
- Persistent and progressive disease: Disease activity gets progressively worse. However, flares and periods of remission are not as dramatic as relapsing/remitting disease. This is the most common course of disease.
During the course of the disease process, RA mediated inflammation can cause permanent damage to several tissues in the body, especially the joints (NIAMS 2009).
4 How Autoimmune Inflammation Destroys Joints
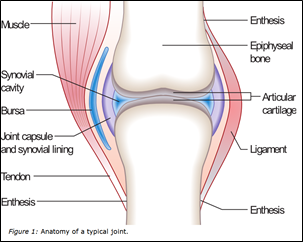
In RA, the immune system mistakenly attacks healthy cells and tissues – predominantly the synovium, the soft tissue between the articular capsule (joint capsule) and the joint cavity of synovial joints. This immune mediated assault leads to the development of pannus, a destructive fibrous tissue within affected joints that erodes cartilage and exacerbates joint dysfunction.
RA damage is engendered by multiple components of the immune system, including antibodies and killer T-cells.
Antibodies are proteins secreted by B-cells that normally recognize and bind to invading microbes such as bacteria and viruses. By attaching to the invading microbe, they activate other components of the immune system to launch an inflammatory response, which destroys the cells.
In RA, antibodies mistakenly recognize "self" cells as invaders. Once antibodies attach to synovial cells in the joint, they attract a variety of immune cells that launch a devastating inflammatory attack. The complex inflammatory process within joints is mediated in large by the cytokines tumor necrosis factor-alpha (TNF-α) and interleukin-6 (IL-6). The inflammatory damage is not limited to the synovium, but spills over to the chondrocytes (cartilage cells that cushion joints). This process raises the level of dangerous inflammatory compounds throughout the body, including C-reactive protein (CRP), which is a marker of inflammation and can be evaluated via a high-sensitivity CRP (hs-CRP) test.
Another kind of immune system cell that develops in the thymus and contributes to RA is the T-cell. One T-cell sub-type—the "killer" T-cell—can directly kill other cells. This is useful in eradicating invading microbes, but in the case of RA, killer T-cells contribute to tissue damage by directly damaging joints and other affected organs.
An important pathological feature of arthritis is the exposure of collagen as a result of cartilage deterioration. When a joint is sufficiently damaged, collagen (a protein component of cartilage) becomes exposed to circulating immune cells, which attack it. This process promotes further inflammatory joint destruction.
Under normal circumstances, joint tissue can repair itself. However, joints may become permanently weakened and deformed if inflammation is severe, chronic, and occurs over many years as with RA.
Inflammatory Damage Associated with Rheumatoid Arthritis Extends Beyond the Joints.
Once the immune system is activated against self-tissue, it sends inflammatory chemicals through the body resulting in widespread damage. For many patients it causes fatigue, malaise and unexplained weight loss.
Other areas targeted by the immune system in RA can include the skin, lungs, eyes, blood, nervous system, heart, and bones. Signs and symptoms may include (Klippel 2010; St. Clair 2004; Cush 2005):
- Skin: Nodules and ulcers on the surface of the skin occur in 50% of people with RA (Mikuls 2007).
- Lungs: RA may cause interstitial lung disease, resulting in a dry cough and shortness of breath that may worsen with physical activity; 20-30% of people with RA have some form of lung disease (Kahlenberg 2011).
- Eyes: Inflamed eyes are common and affect up to 25% of people with RA. Parts of the eye often targeted include the cornea, conjunctiva, and sclera (the white portion of the eye).
- Blood: Anemia and low iron levels often occur in RA and can cause fatigue, fast heartbeat, dizziness and pale skin.
- Nervous system: Degeneration of the cervical vertebrae of the spine can compress the spinal cord in the neck area, causing pain on top of that caused by synovitis (inflammation of the synovium).
- Heart: People with RA are at a two-fold greater risk of developing heart disease, thus contributing to the 40% greater mortality rate of people with RA compared to the general population (Radovits 2010; Peters 2009). Even early in the disease process, RA patients are prone to endothelial dysfunction due to increased circulating inflammatory molecules. Endothelial cells are the delicate cells lining the inside of blood vessels. Endothelial dysfunction is the initial stage of potentially fatal atherosclerotic vascular disease (Tanasescu 2009).
- Bones: People with RA have a significantly increased risk of bone fractures. Both the disease and medicine(s) used to treat RA (e.g., corticosteroids) can cause bone loss, which increases the risk of bone fractures (Spector 1993).
- Dyslipidemia: People who have RA are more likely to have dyslipidemia (elevated levels of cholesterol and triglycerides in blood) (Park 1999; Boers 2003). One study showed dyslipidemia 10 years before the development of RA (van Halm 2007). Therefore, it is important that people with both dyslipidemia and a family history of RA focus on prevention and monitor their health very closely. Dyslipidemia and endothelial dysfunction synergize to dramatically compromise the cardiovascular health of RA patients.
5 Diagnosis
The two important factors to consider when diagnosing RA are 1) whether inflammation is present, and 2) whether an autoimmune response is occurring. Inflammation can be measured with a variety of blood tests including hs-CRP (measures inflammation quantitatively) and an erythrocyte sedimentation rate (ESR) test (measures inflammation functionally) (St. Clair 2004).
To help determine if an autoimmune reaction is taking place, doctors often assess the levels of two proteins: rheumatoid factor (RF) and anti-citrullinated protein antibody (ACPA), sometimes referred to as anti-cyclic citrullinated protein (anti-CCP). Both RF and ACPA are autoantibodies involved in the immune attack against self-tissue in RA.
Table 1. Criteria for a definitive diagnosis of rheumatoid arthritis.> A definitive diagnosis requires confirming synovitis due to RA in at least one joint. Additionally, a total score ≥ 6 by adding the individual criterion scores below (Aletaha 2010; Pietschmann 2011).
| CRITERION | RANGE SCORE |
SCORE CALCULATION |
DEFINITION | TEST |
| Number and site of joints involved | 0-5 | Add one point for each joint involved. | "Involved" means a joint is inflamed. | Physical exam, patient report, and/or imaging of the joint |
Serologic abnormality (abnormal blood test results) |
0-3 | 0 = Normal 1 = Abnormalities are present at low levels 2 = Abnormalities are present at high levels |
The presence (high or low levels) or absence of either RF or ACPA; high score indicative of autoimmunity. | Blood test analyzed by laboratory |
| Elevated Acute-Phase Response | 0-1 | 0 = Test is negative 1 = Test is abnormal |
"Abnormal" means elevated CRP or high ESR; high scores indicate inflammation | Blood test analyzed by laboratory |
| Symptom Duration | 0-1 | 0 = Symptoms have persisted for less than 6 weeks 1 = Symptoms have persisted for 6 weeks or longer |
Symptoms that do not resolve within 6 weeks are indicative of RA. | Monitoring by doctor/patient report |
6 Conventional Medical Treatment of Rheumatoid Arthritis
The goal of RA treatment is to prevent and/or control joint damage, prevent loss of function, and decrease pain (American College of Rheumatology 2002). Early diagnosis and treatment is important for achieving the best possible outcome (Nell 2004; van Aken 2004).
To date, conventional medicine has relied on a mix of powerful pharmaceuticals designed to slow the disease process. While these drugs have been shown to provide relief for many patients, they may also cause side effects that can seriously reduce quality of life. Typically, treatment with one or more of the following types of prescription drugs begins as soon as the diagnosis is confirmed.
Disease-Modifying Antirheumatic Drugs (DMARDS)
DMARDSs decrease joint inflammation and slow the progression of joint damage (Ma 2010).
The two principle classes of DMARDs are conventional and biologic. Conventional DMARDs are chemically synthesized and suppress the immune system. Biologic DMARDs are genetically engineered to target specific molecules of the immune system.
Examples of conventional DMARDs include methotrexate, leflunomide, hydroxychloroquine, and sulfasalazine. Methotrexate (often the DMARD of choice used to treat established RA) is sometimes used in combination with other drugs, including other DMARDs to reduce disease activity as much as possible (Jurgens 2011).
Biologic DMARDs are newer than conventional DMARDs. They are considered second-line drugs after conventional DMARDS for the treatment of RA. Examples of biologic DMARDs include drugs that target TNF-α (a potent pro-inflammatory mediator produced in large amounts in RA). Some anti-TNF-α drugs include adalimumab, etanercept, and certolizumab pegol. Since TNF-α orchestrates the inflammatory network that drives so many disease processes, some DMARDs are being used experimentally for conditions in which autoimmunity is not a central feature. For example, entanercept (Enbrel®) is being explored as a potential therapeutic agent for Alzheimer's disease (Life Extension 2012).
Another commonly prescribed biologic DMARD targeting B-cells (the immune cell that produces antibodies) is rituximab. Rituximab has been shown to reduce RA related symptoms such as joint damage (Edwards 2004; Keystone 2009). Other biologic DMARDSs include abatacept, an inhibitor of T-cell activation and tocilizumab, an antibody against the IL-6 receptor (Tak 2011).
Glucocorticoids
Glucocorticoids suppress both inflammation and the activity of immune system cells. The most commonly used glucocorticoids today are prednisone and methylprednisolone (a more potent glucocorticoid than prednisone). When administered systemically, these drugs can be effective but can also cause side effects (e.g., osteoporosis, eye disease, insomnia, weight gain, and increased susceptibility to infection), which can dramatically impact quality of life (American College of Rheumatology 2002; Moreland 2002). Even though glucocorticoids can be injected directly into the affected joint, the benefits of this delivery method are temporary (American College of Rheumatology 2002).
Doctors often use prednisone as a "bridging" therapy after patients are diagnosed with RA. This regimen includes the use of prednisone for six to twelve months to allow DMARDs to take effect (St. Clair 2004; van Gestel 1995).
Non-Steroidal Anti-Inflammatory Drugs (NSAIDS)
NSAIDs inhibit inflammation and reduce pain. This class of drugs operates by inhibiting the pro-inflammatory enzymes cyclooxygenase-1 and -2 (COX-1 and COX-2). Both of the COX enzymes convert arachidonic acid (an omega-6 fatty acid) into pro-inflammatory prostaglandins, which contribute to swelling and pain.
Selective COX-2 inhibitors were revolutionary when introduced—but then grave side effects were discovered (St. Clair 2004; Trelle 2011). The NSAID rofecoxib (Vioxx®) after being prescribed to tens of thousands of RA patients was removed from the market in 2004 when it was shown to significantly increase risk of heart attack and stroke. Other COX-2 inhibitors such as valdecoxib (Bextra®) were voluntarily removed from the market after studies revealed similar risks. Years before the public learned about the dangers of Vioxx® and Bextra®, Life Extension warned its customers that taking these drugs would create lethal havoc in the body (Faloon 2001). Currently, only one COX-2 inhibitor—Celebrex®—is available on the U.S. market.
The remaining NSAIDs on the market inhibit both the COX-1 and COX-2 enzymes. Unfortunately, these can lead to gastrointestinal side effects such as pain and bleeding because COX-1 is important for proper functioning of the gastrointestinal mucosa.
Additional NSAIDs include aspirin, naproxen, ibuprofen, and acetaminophen. Aspirin inhibits the aggregation of platelets (the components of blood that "clump together" and form a blood clot) more so than other NSAIDs. Taking low-dose aspirin may be beneficial for those at a higher risk of cardiovascular disease (Pearson 2002). However, taking aspirin in combination with therapeutic doses of the common RA drug methotrexate may cause liver and kidney damage (Colebatch 2011).
Statins
Because the chief cause of mortality among people with RA is cardiovascular disease, keeping cholesterol levels within a healthy range is an important component of treatment. Statin drugs have been shown to effectively lower cholesterol levels up to 16% as well as significantly reduce cardiovascular events (e.g., heart attacks) in people with rheumatoid arthritis (Sheng 2011; Ridker 2009).
Although statins are widely prescribed, they have many potential side effects including a breakdown of muscle tissue. Statins are also known to cause depletion of coenzyme Q10, which is necessary for basic cell function. Patients taking statins should supplement with coenzyme Q10 to avoid depletion of this critical enzyme. Life Extension suggests that CoQ10 blood levels be kept in the range of 3 – 7 µg/mL.
Table 2. Types of conventional medicines used in the treatment of rheumatoid arthritis and their potential side effects (Kahlenberg 2011; American College of Rheumatology 2002; Ma 2010; Moreland 2002; Youssef 1997; McCormack 2011; Coblyn 2011).
| TYPE | DRUG | POTENTIAL SIDE EFFECTS |
| Conventional DMARDs | Hydroxychloroquine | Eye damage |
| Methotrexate | Liver/lung damage, decreased production of immune cells | |
| Leflunomide | Diarrhea, headache, hair loss, rash | |
| Sulfasalazine | Decreased production of immune cells | |
| Biologic DMARDs | Anti-TNF | Injection site reaction, rash, infection |
| Rituximab | Infusion reaction | |
| Abatacept | Infusion reaction, infection | |
| Anakinra | Injection site reaction, infections | |
| Tocilizumab | Low platelets and neutrophils, elevated cholesterol and triglycerides, infections | |
| Glucocorticoids | Prednisone | Difficulty sleeping, increased appetite, mood changes |
| Methyl-prednisolone | Difficulty sleeping, increased appetite, mood changes | |
| Cortisone | Difficulty sleeping, increased appetite, headache, sweating | |
| NSAIDs | Acetaminophen | Ulcers and bleeding in the GI tract; potential kidney toxicity |
| Aspirin | ||
| Ibuprofen | ||
| Naproxen | ||
| Coxibs (e.g., Celecoxib) |
Stem Cells – A Developing Strategy for RA Treatment
Stem cells are unique in that they can either divide and reproduce or differentiate into specialized cells. The therapeutic potential of stem cells is a very hot topic in clinical research today. For example, scientists are testing ways to induce a stem cell to turn into normal nerve cells, and then implanting them to replace dead cells in people who have been paralyzed.
Stem cells can be treated in the laboratory to develop into cartilage, bone, and muscle cells, all of which can be damaged through RA mediated inflammation (Dudics 2009; Duijnisveld 2011).
As of 2011, 89 people with RA have received therapeutic stem cell transplants in hopes of causing disease remission or at a minimum, improvement. One study analyzed the result of high-dose chemotherapy in combination with a stem cell transplant in 7 patients with RA. Assessment of disease activity indicated that 5 (71.4%) of the patients clinically responded to this treatment, meaning that symptoms improved. However, stem cell transplants are associated with a treatment related mortality (TRM) of approximately 5-10%. Therefore, this treatment is reserved for only the most severe cases (Tyndall 2011).
7 Rheumatoid Arthritis and the Gut: An Inflammatory Connection
Rheumatoid Arthritis patients display a greater propensity for food allergies and sensitivities, a link that evidence indicates may be more than coincidental (Hvatum 2006). In fact, studies suggest that reactions originating in the gut may fuel systemic inflammatory fires, thereby exacerbating RA symptoms. Support for this theory appeared in the peer-reviewed literature as early as the late 1940's (Zeller 1949).
Immunologic reactions to components of certain foods in many ways resemble the self-reactivity seen in RA and other autoimmune diseases; that is, the immune system mistakenly attacks non-pathogenic molecules. Therefore, it may be possible to calm the immune system by eliminating unnecessary molecular triggers found in certain foods. Studies have shown that RA patients produce significantly more intestinal antibodies against various foods than healthy controls (Hvatum 2006). In a 12-week clinical trial, adherence to an allergen-restricted or allergen-free diet corresponded with symptomatic improvement for a small number of subjects (van de Laar 1992). When allergens were reintroduced into their diets, symptoms reemerged. Vegetarian, vegan, and gluten-free diets have been linked to symptomatic relief in RA patients (Muller 2001; Hafstrom 2001). Interestingly, a recent review of genome-wide association studies revealed that people with celiac disease (characterized by gluten sensitivity) and those with RA shared genetic similarities (Zhernakova 2011).
Based on the connection between food and rheumatism, avoiding foods that result in elevated IgG antibodies in the blood may be an underappreciated method of relieving RA symptoms. Low-cost IgG blood testing allows RA patients to pinpoint potentially problematic foods and begin eating a diet that best suits their immunological profile.
Oral Tolerance and Undenatured Type-II Collagen
Immune system T-cells are tasked with recognizing and distinguishing between "self" and "foreign" molecules. They do this by responding to very specific molecular shapes and 3-dimensional structures (Bagchi 2002). If T-cells in the blood are simply exposed without any "training" to a previously unrecognized protein structure (such as those found in joint collagen), they react violently and trigger a massive inflammatory response to destroy the protein (Cremer 1998).
When scientists want to create an animal model of arthritis they inject collagen into their subjects, thereby sensitizing the T-cells in their blood to the collagen protein (Corthay 1998). Those circulating T-cells initiate inflammation in the animal's joints, which are rich in collagen.
With adequate preparation, T-cells can be "trained" to differentiate between friend and foe. One place this training happens is in the intestinal tract; specifically, the lower end of the small intestine, which is rich in collections of immune tissue called Peyer's patches. Peyer's patches contain T-cells, which become exposed to all sorts of molecular shapes that are natural components of the food we eat (Meyer 2000). In that fashion, we desensitize our immune systems and develop a natural tolerance to new foods without having constant allergic or inflammatory reactions.
By providing the correct 3-dimensional collagen to the digestive tract, we can "educate" our T-cells to ignore collagen when they encounter it in joints (Park 2009; Bagchi 2002). This phenomenon is dubbed oral tolerance to collagen.
Upon induction, oral tolerance to collagen suppresses joint inflammation, as has been demonstrated in numerous laboratory studies (Park 2009; Zhu 2007; Nagler-Anderson 1986). Oral administration of soluble type II collagen has even prevented experimentally induced arthritis by way of collagen injections (Min 2006; Nagler-Anderson 1986).
But not just any collagen will do. Typical commercial processing causes collagen to become denatured, uncoiling from its normal helical shape and losing its functional 3-dimensional structure. Denatured collagen has no beneficial effects on joint inflammation (Nagler-Anderson 1986).
A more natural form of collagen called undenatured type II collagen (UC-II®) has recently been developed (Zhao 2011). UC-II® retains its original 3-dimensional molecular structure, keeping it recognizable by T-cells in Peyer's patches. UC-II® is robust enough to survive the harsh conditions in the stomach and small intestine, arriving at Peyer's patches with its molecular structure intact (Bagchi 2002).
As mentioned previously, collagen exposure subsequent to joint deterioration is a key mechanism by which the immune system is driven to destroy joint tissue in arthritis. Therefore, retraining the immune system through induction of oral tolerance may be an effective means of easing the inflammatory rheumatic process.
8 Hormones and Rheumatoid Arthritis
The role of steroid hormones in autoimmunity is evidenced by differences between men and women in both immune function and incidence of autoimmune disease. For example, estrogen actions tend to be pro-inflammatory, while progesterone, androgens, and glucocorticoids are anti-inflammatory (Cutolo 2004). Studies have documented low progesterone levels in women with autoimmune diseases, suggesting that a relative imbalance in favor of estrogen may contribute to immune reactivity in some female patients (Shabanova 2008). In RA and other autoimmune diseases, estrogen levels appear to be driven too high by actions of inflammatory mediators like TNF-α and IL-6 (Cutolo 2006). In some studies, lower levels of testosterone have been observed in male patients with RA than in controls (Masi, 2006). Testosterone and progesterone functions to promote immune tolerance in males and females, respectively (Cutolo 2006). Therefore, ensuring adequate levels of progesterone to balance excess estrogen in women and sufficient levels of testosterone in men may modulate some underlying immunologic features of RA (Karlson 2009; Cutolo 2009). Medications used to treat RA symptoms have been shown to suppress sex hormone production as well, potentially compounding an existing hormone insufficiency or imbalance (Weitoft 2008).
While large-scale clinical trials have yet to evaluate the efficacy of bioidentical hormone replacement therapy in RA patients, Life Extension suggests that the potential for considerable benefit outweighs the minimal risk. Taking measures to achieve and maintain optimal levels of sex hormones may soon emerge as an effective strategy for the symptomatic management of RA. Those interested in reading more about natural bioidentical hormone replacement therapy should review the Male or Female Hormone Restoration protocols.
The role and therapeutic potential of the hormone dehydroepiandrosterone (DHEA) in male and female RA patients is supported by a broad base of evidence. Between ages 25 and 75, levels of the multifunctional hormone DHEA decrease by approximately 80% (Weiss 2011). Moreover, glucocorticoid therapy often employed in RA suppresses DHEA levels significantly (Yukioka 2006). The implications of low levels of DHEA may be considerable in RA, especially since DHEA counteracts the inflammatory cytokines TNF-α and IL-6 in the synovium. Conversely, local TNF-α suppresses DHEA levels in the synovium; thus, the relationship between the anti-inflammatory effects of DHEA and the pro-inflammatory effects of TNF-α are reciprocal in nature. In a one year, double-blinded, placebo controlled trial, 125 men and women aged 65 – 75 received 50 mg of DHEA daily. Treatment resulted in improved insulin sensitivity and lower levels of TNF-α and IL-6 in blood samples (Weiss 2011). These results were maintained during an additional year of open-label continuation.
9 Nutrients
Fatty Acids
Polyunsaturated fatty acids (PUFAs), primarily those derived from marine sources, have been recommended for RA patients for many years because of their ability to reduce inflammation and bolster cardiovascular health while helping soothe the overactive immune system (Goldberg 2007).
There are two main types of dietary PUFAs: omega-6 and omega-3. Both are important for health. However, it is especially important to maintain the correct ratio of omega-6 to omega-3 in the diet. Research has shown that the typical American diet is composed of an omega-6 to omega-3 ratio as high as 25:1 (Simopoulos 2011). The ideal ratio, however, is about 4:1, meaning very few people are getting enough omega-3 fatty acid relative to the amount of omega-6 (Holub 2002). A ratio so skewed toward omega-6 has the potential to be highly pro-inflammatory. Thus, it is essential for arthritis patients to get sufficient omega-3 fatty acids.
A number of trials have supported the benefit of RA patients consuming omega-3 fatty acids in the form of fish oil. These studies have shown that fish oil can help reduce the inflammation (Dawczynski 2011), pain and symptoms associated with RA. Eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA), typically derived from fish oil, have proven anti-inflammatory properties. The results of a study in which people with RA consumed 1,800 mg EPA and 900 mg DHA daily for three months indicated that these fatty acids are effective in controlling morning stiffness, whereas those who received the placebo experienced worsening symptoms (Kremer 1985).
Numerous clinical studies have supported the benefits of RA patients consuming fish oil (James 1997). In a study assessing joint tenderness and dose of NSAIDs required to control symptoms in people with well-established RA, those consuming fish oil experienced less joint pain and took lower doses of NSAIDs (James 2010). Data from a separate study indicated that consuming fish oil may complement the anti-inflammatory properties of acetaminophen (Caughey 2010). Consuming fish oil also significantly reduced TNF-α and other pro-inflammatory cytokines (Endres 1989). Fish oil significantly improved cholesterol and triglyceride levels in people with RA as well, mitigating cardiovascular risk (Olendzki 2011).
Krill oil is a marine oil whose properties differ slightly from those of fish oil. In an animal model, krill oil "significantly reduced arthritis scores and swelling" (Ierna 2010). In a separate study of krill oil combined with hyaluronic acid and astaxanthin—both of which target pro-inflammatory agents in the body—arthritis patients reported a 55% pain reduction in under three months; 63% of participants were entirely pain-free post-treatment (Valensa 2011).
Gamma-linolenic acid (GLA): GLA is a beneficial omega-6 fatty acid found in oils from several different plants. Its heart healthy effects are well documented. In a study in which RA patients consumed 1400 mg GLA daily, their RA symptoms were significantly reduced, including number and severity of tender joints and degree of swelling (Leventhal 1993). A thorough review of clinical trials found that whereas consuming 1,400 mg daily or more of GLA resulted in a significant improvement in RA related symptoms, lower doses (i.e., 500 mg daily) did not appear effective (Cameron 2009). Other studies have shown that the following GLA-rich oils may be beneficial in people with RA:
Blackcurrant seed oil (Ribes nigrum): A 24-week clinical trial involving people with RA compared the effects of blackcurrant oil to placebo and found that blackcurrant seed oil significantly improved RA related symptoms (Leventhal 1994).
Borage seed oil (Borago officinalis): Oil from the borage plant seed is rich in GLA. Borage seed oil was used as the source of GLA in the study testing the benefits of GLA in reducing RA symptoms (Leventhal 1993). Results from a comprehensive review indicate that borage seed oil is associated with improved clinical outcomes in people with RA (Macfarlane 2011).
A recent clinical study found that RA patients consuming borage seed oil had decreased levels of total cholesterol, LDL, triglycerides, and increased HDL levels (Olendski 2011). This effect is particularly beneficial for people with RA as they have a greater risk of heart disease than the general population (Radovits 2010; Peters 2009).
Evening primrose oil (Oenothera biennis): A review showed that primrose oil effectively reduced RA symptoms (Cameron 2011). In one study, people with RA taking daily NSAID therapy consumed either 6 g per day of evening primrose oil or placebo. Those receiving daily doses of evening primrose oil experienced less morning stiffness after 3 months and less pain after 6 months (Brzeski 1991).
Vitamins
Vitamin K: Vitamin K, an antioxidant and anti-inflammatory agent that plays a role in bone metabolism and blood coagulation, is actually a group of closely related compounds that includes vitamin K1 (phylloquinone) and vitamin K2 (menaquinone). Vitamin K1 is more abundantly found in foods but is less bioactive than vitamin K2, which has a number of different subtypes. Menaquinone-4 (MK-4) and menaquinone-7 (MK-7) are the most important forms of vitamin K2. Menaquinones are mainly found in animal organs, such as the liver, or in bacterially fermented foods, such as soy, yogurt, and cheese (Grober 2014).
Animal research indicates oral supplementation with vitamin K plays a role in the expression of genes involved in the inflammatory pathways (Ohsaki 2006). A one-year study in over 500 elderly individuals found that dietary phylloquinone intake was associated with an improvement in markers related to insulin resistance and chronic inflammatory diseases (Juanola-Falgarona 2013). Cellular and animal research indicates that MK-4 inhibited the proliferation of rheumatoid synovial cells and inhibited collagen-induced arthritis in rats (Okamoto 2007).
In a cross-sectional study of 158 female RA patients not on warfarin or teriparatide, 70 individuals were treated with 45 mg/day of vitamin K2. The treatment group exhibited lower levels of inflammatory markers, including CRP, compared with the group that received no treatment. In addition, a longitudinal component of this study examined 52 patients who took vitamin K along with their medications for three months. These patients showed statistically significant decreases in serum CRP (Ebina 2013).
In a randomized controlled trial of 84 subjects being treated for RA, the group receiving 100 µg/day of MK-7 had reduced inflammatory markers compared with the control group. MK-7 has a longer half-life and is more bioavailable than MK-4 (Rheaume-Bleue 2015). Vitamin K vitamers have the potential to combat inflammation and improve joint health, although further research is warranted.
Vitamin D, which is synthesized when the skin comes into contact with ultra-violet light, plays an important immunomodulatory role and appears to appreciably ease RA symptoms. The results of a randomized clinical trial showed that RA patients taking a low dose of 1-25 dihydroxyvitamin D along with their disease modifying antirheumatic drug (DMARD) therapy had significantly greater pain relief at 3 months compared with the group receiving DMARDs only (Gopinath 2011). Alarmingly, a recent Swiss trial found that 86% of 272 RA patients had deficient or insufficient levels of vitamin D (Stoll 2011).
The vitamin D receptor (VDR), which binds vitamin D is located on the surface of immune cells. Because immune cells play an important role in promoting inflammation in RA, it seems logical that vitamin D would also have a role in RA mediated inflammation. Indeed, a recent study found that the VDR is important in limiting the inflammatory tendency of immune cells in a mouse model of RA (Zwerina 2011).
However, vitamin D does more than just arrest damaging immune cells; it also supercharges protective immune cells.
T-reg cells are specialized components of the immune system that help keep immunity balanced. If too few T-reg cells are present, the immune system becomes overactive as in autoimmune diseases like RA. Vitamin D increases the number of protective T-reg cells, restoring equilibrium to an overactive immune system (Cooney 2011).
Vitamin B6: The prevalence of vitamin B6 deficiency is elevated in people with RA. This deficiency has been associated with more severe symptoms (Chiang 2003). A study found that treatment with 100mg daily of vitamin B6 reduced blood levels of TNF-α and other pro-inflammatory cytokines in people with RA (Huang 2010).
Folate: A folate deficiency is particularly common in people RA being treated with methotrexate, as this drug depletes folate (Whittle 2004). Therefore, folate supplementation may be beneficial for people with RA.
Plants and Plant-derived Compounds
Andrographis: Andrographolides, components extracted from the plant Andrographis paniculata, inhibit activity of the pro-inflammatory compound known as inducible nitric oxide synthase (iNOS). This helps exert a powerful anti-inflammatory effect (Chiou 2000). Readers who are familiar with the vascular benefits of eNOS (endothelial NOS) should note that unlike eNOS, iNOS is pro-inflammatory and often involved in disease states where it is desirable to inhibit its actions.
Andrographolides suppress production of the pro-inflammatory cytokines TNF-alpha and prostaglandin E2 (PGE-2), preventing their gene expression at multiple levels (Liu 2007(a,b)). By doing so they downregulate the chemical signaling pathways that cells use to "tell" each other to initiate the inflammatory response, which plays a key role in rheumatoid arthritis (Liu 2008).
Scientific analysis has further revealed that andrographolides operate "upstream" within the process of the inflammatory cascade by blocking the effects of the pro-inflammatory transcription factor nuclear factor-kappaB (NF-kB) (Bao 2009).
NF-kB is found in almost all human cells. It plays a key role in cellular responses to stress, cytokines, free radicals, oxidized low-density lipoprotein (LDL), and bacterial or viral pathogens. Accordingly, its central role as a first-responder to oxidative damage, infection, and toxin-induced stress links it to inflammation, cancer, and chronic disease (Ahn 2005). NF-kB tightly regulates virtually all factors that are downstream in the inflammatory cascade, including cytokines known as interleukins, hormones known as prostaglandins, and TNF-alpha.
By blocking NF-kB, andrographolides inhibit production of a host of inflammatory mediators in one simple step (Chao 2009). As demonstrated in animal studies, they also permit normal activity of vital immune surveillance cells as they simultaneously suppress over-active inflammatory cells (Naik 2009).
This is a critical feature that distinguishes andrographolides from most anti-rheumatic drugs (DMARDS). Whereas andrographolides suppress inflammatory immune factors, DMARDs can suppress immune function in general resulting in an increased risk of infection (Manganelli 1993).
Curcumin: Curcumin is an antioxidant compound found in the spice turmeric and has potent anti-inflammatory and immunomodulatory properties. One laboratory based study showed that curcumin reduces synovial inflammation (Jackson 2006). Specifically, this study demonstrated that exposing inflamed synovial cells to curcumin not only reduced the inflammatory state of these cells, but suppressed the production of pro-inflammatory proteins and the activation of cells with inflammatory properties.
Curcumin also helps protect cartilage from inflammation mediated destruction. A meta-analysis sought to examine the body of evidence concerning the effect of curcumin on chondrocytes, the cells that make up cartilage. The researchers concluded that curcumin not only helps prevent the degradation of cartilage induced by certain inflammatory proteins in the joint (Henrotin 2010), but it also helps promote cartilage regeneration (Buhrmann 2010).
Curcumin may also help lower the dose of methotrexate required for therapeutic effects and drug-related liver toxicity. One study found that administering curcumin along with a very low, sub-therapeutic dose of methotrexate in a mouse model of arthritis effectively treated the inflammation while reducing the level of drug-induced liver damage (Banji 2011). If as effective in humans, taking curcumin along with methotrexate would enable people with RA to take lower doses of methotrexate, thereby decreasing their risk of liver toxicity.
One small (18 people) but well-designed study found that consuming curcumin resulted in improved ambulation (increase in time) as well as a significant reduction in joint swelling and morning stiffness (Deodhar 1980). These results were corroborated by a larger clinical trial in which 45 RA patients were randomized to receive 50 mg of diclofenac sodium, 500 mg of a highly absorbable form of curcumin, or both for 8 weeks. In this trial, curcumin alone and in combination with diclofenac sodium proved to be at least as effective as diclofenac sodium alone in easing RA disease activity, as measured by multiple standardized assessments. In addition, curcumin alone powerfully suppressed CRP (a marker of inflammation in the blood) by 52% from baseline, while diclofenac sodium alone only decreased CRP by 1.5%. The investigators of this trial remarked that "Taken together, our present results provide a clear proof-of-principle for the superiority of curcumin, and the lack of any synergistic or additive efficacy when used in conjunction with diclofenac strongly favours the safe and effective application of curcumin alone in clinical settings for the management of rheumatoid arthritis, and other proinflammatory diseases including cancer in the future" (Chandran 2012).
Quercetin: Quercetin is a flavonoid compound rich in fruits and vegetables -- especially apples, citrus fruits, parsley, sage and onions. Quercetin strongly inhibits multiple components of the inflammatory process, including the COX enzymes that are targeted by NSAIDs (Lee 2010). Laboratory experiments with synovial cells have shown that although quercetin does not have an effect on the production of pro-inflammatory proteins, it directly reduces inflammation in the synovium as well as the activation of pro-inflammatory cells (Jackson 2006).
A recent proof-of-concept study demonstrated decreased inflammation by utilizing bioengineering techniques to increase the bioavailability of quercetin in a rat model of RA. The investigators loaded quercetin into microspheres and delivered the microsphere-quercetin combination directly into the joint (Natarajan 2011). The microspheres enabled the quercetin to be released consistently over 30 days. Although additional human trials are needed, the data thus far supports an anti-inflammatory role for quercetin in RA.
Boswellia serrata extract: Resin from the Boswellia serrata plant contains an anti-inflammatory compound called 3-acetyl-11-keto-β-boswellic acid (AKBA). Boswellia serrata extract also contains high levels of boswellic acids, which are potent inhibitors of 5-lipoxygenase (5-LOX), an enzyme that produces inflammatory leukotrienes. Boswellia serrata extract may also have inhibitory effects on pro-inflammatory proteins such as TNF-α (Ammon 2006). Extracts of Boswellia have been shown to improve arthritic symptoms and reduce inflammatory activity and markers in animal models of rheumatoid arthritis (Banji 2022; Kumar 2019). And Boswellia has historically been used in Ayurvedic medicine for inflammatory, painful conditions like rheumatoid arthritis (Sethi 2022).
One placebo-controlled clinical study in 260 participants with rheumatoid arthritis found that Boswellia extract effectively improved symptoms like joint swelling, pain, and stiffness; it also improved erythrocyte sedimentation rate, suggesting an improvement in inflammation (Etzel 1996). Another placebo-controlled study in 182 patients with rheumatoid arthritis found that 16 weeks of treatment with a combination of Ayurvedic plant extracts (including Boswellia) led to improvement in joint swelling compared with placebo (Chopra 2000).
Pomegranate: Pomegranates contain a high concentration of polyphenols, which are compounds with strong antioxidant properties. Pomegranate seeds are either eaten in their natural form or processed to produce pomegranate juice. Alternatively, the active compounds can be extracted from the rest of the fruit's components.
One study tested the severity of inflammation and incidence of arthritis in mice fed a pomegranate extract in addition to their food. The mice in the pomegranate fed group had a lower incidence of arthritis, and those who did get arthritis developed it later than normal (i.e., delayed disease) as well as having reduced joint inflammation and damage (Shukla 2008).
In a recent pilot study testing the efficacy of pomegranate extract in 6 people with RA, it was reported that the people consuming the extract had significantly fewer tender joints (Balbir-Gurman 2011). Expanding the sample size of patients studied will determine if these effects are broadly applicable.
Green tea: The active ingredient in green tea is epigallocatechin 3-gallate (EGCG), which has been tested extensively for its health promoting properties. EGCG has been shown to have significant anti-inflammatory and antioxidant effects as well as helping to optimize the lipid profile (Ahmed 2010).
Pre-clinical studies indicate that green tea may be effective in reducing inflammation in the joints of people with RA. For example, supplementing drinking water with green tea significantly reduced the severity of arthritis in a rat model of RA (Kim 2008). It was even effective in preventing the onset of arthritis in a mouse model of RA (Haqqi 1999).
Ginger: Ginger, the underground stem of the Zingiber officinale plant, has potent anti-inflammatory and antioxidant properties (Grzanna 2005). Ginger directly suppresses inflammation by inhibiting pro-inflammatory enzymes and blocking the production of pro-inflammatory proteins (Nievergelt 2011). Furthermore, several investigators have reported that consuming ginger significantly prevented the onset of arthritis in rodent models of RA (Funk 2009; Ramadan 2011; Fouda 2009).
Nigella sativa seeds: These seeds are commonly called "black cumin" or "black caraway." Investigators have shown that consuming thymoquinone, the active compound of the seed oil, inhibited inflammation and prevented arthritis in a rat model of RA (Tekeoglu 2007).
A recent study compared the symptoms of RA patients receiving 500 mg of Nigella sativa oil twice daily for one month with those receiving placebo capsules. Remarkably, up to 40% (which varied approximately 10% based upon the disease activity scale used to assess symptoms) of people receiving Nigella sativa seed oil experienced an improvement in RA symptoms (Gheita 2011).
Beta-sitosterol and beta-sistosterol glucoside: As suggested by some preliminary research, a proprietary 99:1 mixture of beta-sistosterol (BSS) and beta-sitosterol glucoside (BSSG) called Moducare® may modulate immunity in RA. In laboratory experiments a BSS/BSSG blend has demonstrated an ability to balance immune cell function under varying conditions (Ju 2004; Anonymous 2001). Two small pilot studies in human subjects have corroborated the in vitro data. In the first study, 17 ultra-marathon runners were given either the BSS/BSSG mixture or a placebo. After the race, when immune function is normally drastically altered, researchers assessed parameters of inflammation in both groups. In the group taking the BSS/BSSG mixture, it was noted that levels of immune cells rose while inflammatory mediators in the blood declined, suggesting that the mixture primed the immune system for defense while simultaneously suppressing excess inflammation (Bouic 1999). In the second trial, 18 patients with active RA took the either the BSS/BSSG mixture or placebo for 24 weeks. The mixture lead to significant improvements compared to placebo in all of the following: measurable tender joint count, patient's assessment of pain, patient's global assessment of disease activity, and physician's global assessment of pain. Furthermore, erythrocyte sedimentation rate (ESR), an assessment of the inflammatory tendency of blood, decreased by 56% (Louw 2002).
White peony extract: White peony (Paeonia lactiflora) root is a traditional Chinese medicinal herb that contains bioactive compounds called glucosides. A water and alcohol extract of the peony root, known as total glucosides of peony, has more than 15 identified compounds. The most active and abundant of these is paeoniflorin, which represents more than 90% of the total glucosides of peony (Feng 2016; He 2011). A number of studies have shown paeoniflorin and total glucosides of peony have immunomodulatory, anti-inflammatory, and pain-relieving properties, and provide support for peony’s historical use in the treatment of autoimmune conditions in general and rheumatoid arthritis in particular (Feng 2016; Zhang 2012; Lindler 2020). In 1998, the State Food and Drug Administration of China approved total glucosides of peony for the treatment of rheumatoid arthritis (He 2011).
In a meta-analysis of eight randomized controlled trials involving 522 participants with rheumatoid arthritis, total glucosides of peony combined with methotrexate had better therapeutic efficacy than methotrexate alone, including a greater decrease in ESR and swollen joint count. Additionally, fewer adverse events were reported in the combination group than methotrexate alone (Feng 2018).
In a controlled trial, 450 people with rheumatoid arthritis were treated for 12 weeks with either 1.8 grams of total glucosides of peony daily or 10 mg of methotrexate weekly, an immunosuppressive anti-rheumatic medication (Gold Standard 2016). A therapeutic response was achieved in about 72% of the peony-treated group. These results were later confirmed in a more advanced clinical trial in over 1,000 people with rheumatoid arthritis (He 2011). Several clinical trials have studied the effect of total glucosides of peony in combination with methotrexate or leflunomide, another anti-rheumatic medication, and found that peony extract can protect against the liver toxicity of methotrexate and improve response to treatment compared with the medications alone (Chen, Li 2013; Du 2005; Wang 2007; Xiang 2015; Zhao 2006; Liu 2021).
Other clinical studies have found that total glucosides of peony may also be helpful in other types of autoimmune arthritis, including juvenile idiopathic arthritis and psoriatic arthritis (Cai 2016; Wang 2014).
Studies using animal models of inflammatory arthritis also demonstrated the anti-inflammatory and anti-rheumatic potential of total glucosides of peony (Zheng 2007; Liu 2010; Lin 2012; Jia 2014). In one study, treatment with total glucosides of peony inhibited inflammatory cytokine production by joint cells and prevented bone destruction around affected joints (Wei 2013).
Laboratory and animal investigations into the actions of total glucosides of peony indicate that in conditions of immune overactivation, total glucosides of peony modulates immunological system activity (He 2011). In animal models of rheumatoid arthritis, paeoniflorin alone has demonstrated similar immune-modulating effects (Zhang 2015; Zhai 2016; Chen, Guo 2013).
Endogenous Compounds
SAMe: S-adenosyl-L-methionine (SAMe) is a natural compound in the body that is necessary for many different physiological processes. SAMe has been shown to improve symptoms of osteoarthritis, liver disease, and even depression. Although most scientific research has focused on osteoarthritis, the mechanisms for SAMe suggest a role in RA. SAMe supports the production of the structural components of cartilage, which can be destroyed by the chronic inflammation of RA. The anti-inflammatory properties of SAMe suggest a supportive role for this compound in RA patients (Talbott 2007).
A comprehensive review of several individual clinical studies found that SAMe relieved pain and improved joint function in people with osteoarthritis (Rutjes 2009). In fact, SAMe had similar analgesic and function improving effects as treatment with NSAIDs, but without the adverse effects (Soeken 2002).
The common RA medicine methotrexate has been shown to inhibit cell signaling through the SAMe pathway (Nesher 1996). Therefore, the cells in joint tissue may not process SAMe normally. This laboratory study suggests that people treated with methotrexate may benefit from SAMe supplementation.
Glucosamine: This compound is a precursor to glycosaminoglycans, components of larger molecules – proteoglycans – which are incorporated into cartilage. Proteoglycans are critical for healthy cartilage and proper cushioning of the joint because they draw water into the joint, acting as a lubricant. In addition, glucosamine seems to have some anti-inflammatory properties (Talbott 2007).
Glucosamine has been shown to suppress production of the pro-inflammatory cytokine IL-8 in cells of the synovium (Hua 207). Another study found that glucosamine was effective in significantly reducing RA symptoms despite no detectable differences in conventional markers of inflammation such as CRP (Nakamura 2007).
Chondroitin sulfate: This compound is a structural component of cartilage. When taken as a supplement, it helps fight inflammation and supports the rebuilding of cartilage (Talbott 2007). Chondroitin sulfate may be healthy for the heart as well. An animal model of atherosclerosis and chronic arthritis found that chondroitin sulfate prevented atherosclerotic lesions from developing (Martinez-Calatrava 2010). This data, although very preliminary, raises the possibility that chondroitin sulfate may help fight the systemic inflammation present in RA that leads to joint and heart disease.
Exercise
As with other rheumatic diseases, exercise is a critical component of maintaining muscle mass, supporting a healthy heart, and preventing joint damage as much as possible. Various types of exercises are beneficial for people with RA.
Aerobic exercise: Several studies have demonstrated that dynamic aerobic exercises such as swimming, walking, and bike riding not only improve overall health and quality of life in patients with RA but also reduce pain. Another benefit of dynamic exercise is the improvement in cardiovascular health, which is especially important for people with RA (Cooney 2011). To date, no studies have reported that dynamic exercise has deleterious effects on disease activity or joint function (Van den Ende 1998; Cairns 2009). Even high-intensity exercise has not been shown to lead to increased inflammation or joint damage (Plasqui 2008).
Strength training: Strength training (e.g., weight lifting) involves applying resistance to various muscle groups to improve muscle strength. Similar to dynamic exercise, strength training reduced pain and improved function in people with RA (Flint-Wagner 2009).
Disclaimer and Safety Information
This information (and any accompanying material) is not intended to replace the attention or advice of a physician or other qualified health care professional. Anyone who wishes to embark on any dietary, drug, exercise, or other lifestyle change intended to prevent or treat a specific disease or condition should first consult with and seek clearance from a physician or other qualified health care professional. Pregnant women in particular should seek the advice of a physician before using any protocol listed on this website. The protocols described on this website are for adults only, unless otherwise specified. Product labels may contain important safety information and the most recent product information provided by the product manufacturers should be carefully reviewed prior to use to verify the dose, administration, and contraindications. National, state, and local laws may vary regarding the use and application of many of the therapies discussed. The reader assumes the risk of any injuries. The authors and publishers, their affiliates and assigns are not liable for any injury and/or damage to persons arising from this protocol and expressly disclaim responsibility for any adverse effects resulting from the use of the information contained herein.
The protocols raise many issues that are subject to change as new data emerge. None of our suggested protocol regimens can guarantee health benefits. Life Extension has not performed independent verification of the data contained in the referenced materials, and expressly disclaims responsibility for any error in the literature.
[Anonymous] Monograph. Plant sterols and sterolins. Altern Med Rev. 2001 Apr;6(2):203-6.
Ahmed S. Green tea polyphenol epigallocatechin 3-gallate in arthritis: progress and promise. Arthritis Res Ther, 2010. 12(2):208.
Ahn KS, Aggarwal BB. Transcription Factor NF-{kappa}B: A sensor for smoke and stress signals. Ann N Y Acad Sci. 2005 Nov;1056:218-33.
Aletaha D, et al. 2010 Rheumatoid arthritis classification criteria: an American College of Rheumatology/European League Against Rheumatism collaborative initiative. Arthritis Rheum, 2010. 62(9):2569-81.
American College of Rheumatology Subcommittee on Rheumatic Arthritis Guidelines (2002), Guidelines for the management of rheumatoid arthritis: 2002 Update. Arthritis Rheum, 2002. 46(2):328-46.
Ammon HP. Boswellic acids in chronic inflammatory diseases. Planta Med, 2006. 72(12):1100-16.
Balbir-Gurman A, et al. Consumption of pomegranate decreases serum oxidative stress and reduces disease activity in patients with active rheumatoid arthritis: a pilot study. Isr Med Assoc J, 2011. 13(8):474-9.
Banji D, et al. Synergistic activity of curcumin with methotrexate in ameliorating Freund's Complete Adjuvant induced arthritis with reduced hepatotoxicity in experimental animals. Eur J Pharmacol, 2011. 668(1-2):293-8.
Banji D, Banji OJF, Rashida S, Alshahrani S, Alqahtani SS. Bioavailability, anti-inflammatory and anti-arthritic effect of Acetyl Keto Boswellic acid and its combination with methotrexate in an arthritic animal model. Journal of ethnopharmacology. Jun 28 2022;292:115200. doi:10.1016/j.jep.2022.115200. https://pubmed.ncbi.nlm.nih.gov/35306043/
Bao Z, Guan S, Cheng C, et al. A novel antiinflammatory role for andrographolide in asthma via inhibition of the nuclear factor-kappaB pathway. Am J Respir Crit Care Med. 2009 Apr 15;179(8):657-65.
Boers M, et al. Influence of glucocorticoids and disease activity on total and high density lipoprotein cholesterol in patients with rheumatoid arthritis. Ann Rheum Dis, 2003. 62(9):842-5.
Bouic P, et al. The effects of B-sitosterol (BSS) and B-sitosterol glucoside (BSSG) mixture on selected immune parameters of marathon runners: inhibition of post marathon immune suppression and inflammation. Int J Sports Med. 1999 May;20(4):258-62.
Brzeski M, Madhok R, Capell HA. Evening primrose oil in patients with rheumatoid arthritis and side-effects of non-steroidal anti-inflammatory drugs. Br J Rheumatol, 1991. 30(5):370-2.
Buhrmann C, et al. Curcumin mediated suppression of nuclear factor-kappaB promotes chondrogenic differentiation of mesenchymal stem cells in a high-density co-culture microenvironment. Arthritis Res Ther, 2010. 12(4):R127.
Buttgereit F, et al. Targeting pathophysiological rhythms: prednisone chronotherapy shows sustained efficacy in rheumatoid arthritis. Ann Rheum Dis. 2010 Jul;69(7):1275-80. Epub 2010 Jun 11.
Buttgereit F. How should impaired morning function in rheumatoid arthritis be treated? Scand J Rheumatol Suppl. 2011;125:28-39.
Cai Y, Yuan Q, Xu K, et al. Assessment of the Therapeutic Effect of Total Glucosides of Peony for Juvenile Idiopathic Arthritis: A Systematic Review and Meta-Analysis. Evidence-based complementary and alternative medicine: eCAM.2016;2016:8292486.
Cairns AP and McVeigh JG. A systematic review of the effects of dynamic exercise in rheumatoid arthritis. Rheumatol Int, 2009. 30(2):147-58.
Cameron M, et al. Evidence of effectiveness of herbal medicinal products in the treatment of arthritis. Part 2: Rheumatoid arthritis. Phytother Res, 2009. 23(12):1647-62.
Cameron M, Gagnier JJ, Chrubasik S. Herbal therapy for treating rheumatoid arthritis. Cochrane Database Syst Rev, 2011(2):CD002948.
Caughey GE, et al. Fish oil supplementation increases the cyclooxygenase inhibitory activity of paracetamol in rheumatoid arthritis patients. Complement Ther Med, 2010. 18(3-4):171-4.
Chandran B and Goel A. A Randomized, Pilot Study to Assess the Efficacy and Safety of Curcumin in Patients with Active Rheumatoid Arthritis. Published online 9 MAR 2012.
Chao WW, Kuo YH, Hsieh SL, Lin BF. Inhibitory effects of ethyl acetate extract of Andrographis paniculata on NF-{kappa}B trans-activation activity and LPS-induced acute inflammation in mice. Evid Based Complement Alternat Med. 2009 Sep 10.
Chen T, Guo ZP, Wang L, et al. Paeoniflorin suppresses vascular damage and the expression of E-selectin and ICAM-1 in a mouse model of cutaneous Arthus reaction. Experimental dermatology. Jul 2013;22(7):453-457.
Chen Z, Li XP, Li ZJ, Xu L, Li XM. Reduced hepatotoxicity by total glucosides of paeony in combination treatment with leflunomide and methotrexate for patients with active rheumatoid arthritis. International immunopharmacology.Mar 2013;15(3):474-477.
Chiang EP, et al. Abnormal vitamin B(6) status is associated with severity of symptoms in patients with rheumatoid arthritis. Am J Med, 2003. 114(4):283-7.
Chiou WF, Chen CF, Lin JJ. Mechanisms of suppression of inducible nitric oxide synthase (iNOS) expression in RAW 264.7 cells by andrographolide. Br J Pharmacol. 2000 Apr;129(8):1553-60.
Chopra A, Lavin P, Patwardhan B, Chitre D. Randomized double blind trial of an ayurvedic plant derived formulation for treatment of rheumatoid arthritis. The Journal of rheumatology. Jun 2000;27(6):1365-72. https://pubmed.ncbi.nlm.nih.gov/10852255/
Coblyn JS and Brigham and Women's Hospital. Brigham and Women's experts' approach to rheumatology2011, Sudbury, Mass.: Jones and Bartlett. xi, 236.
Colebatch AN, Marks JL, Edwards CJ. Safety of non-steroidal anti-inflammatory drugs, including aspirin and paracetamol (acetaminophen) in people receiving methotrexate for inflammatory arthritis (rheumatoid arthritis, ankylosing spondylitis, psoriatic arthritis, other spondyloarthritis). Cochrane Database Syst Rev, 2011. 11: CD008872.
Cooney JK, et al. Benefits of exercise in rheumatoid arthritis. J Aging Res, 2011. 2011: Article ID 681640. doi: 10.4061/2011/681640.
Cush JJ and Kavanaugh A. Rheumatoid arthritis: early diagnosis and treatment. 1st ed. 2005, West Islip, NY: Professional Communications. p.320.
Cutolo M, et al. Estrogens and autoimmune diseases. Ann N Y Acad Sci. 2006 Nov;1089:538-47.
Cutolo M, et al. Sex hormones influence on the immune system: basic and clinical aspects in autoimmunity. Lupus. 2004;13(9):635-8.
Cutolo M. Androgens in rheumatoid arthritis: when are they effectors? Arthritis Res Ther. 2009;11(5):126. Epub 2009 Sep 22.
Cutolo M. Rheumatoid arthritis: circadian and circannual rhythms in RA. Nat Rev Rheumatol. 2011 Aug 2;7(9):500-2. doi: 10.1038/nrrheum.2011.115.
Dawczynski C, et al. Incorporation of n-3 PUFA and gamma-linolenic acid in blood lipids and red blood cell lipids together with their influence on disease activity in patients with chronic inflammatory arthritis--a randomized controlled human intervention trial. Lipids in health and disease, 2011. 10:130.
Deodhar SD, Sethi R, Srimal RC. Preliminary study on antirheumatic activity of curcumin (diferuloyl methane). Indian J Med Res, 1980. 71:632-4.
Du JH, Dong BD. [Comparative study on clinical efficacy of using methotrexate singly or combined with total glucosides of Paeony in treating rheumatoid arthritis]. Zhongguo Zhong xi yi jie he za zhi Zhongguo Zhongxiyi jiehe zazhi = Chinese journal of integrated traditional and Western medicine / Zhongguo Zhong xi yi jie he xue hui, Zhongguo Zhong yi yan jiu yuan zhu ban.Jun 2005;25(6):540-542.
Dudics V, et al. Chondrogenic potential of mesenchymal stem cells from patients with rheumatoid arthritis and osteoarthritis: measurements in a microculture system. Cells Tissues Organs, 2009. 189(5):307-16.
Duijnisveld BJ, et al. Regenerative potential of human muscle stem cells in chronic inflammation. Arthritis Res Ther, 2011. 13(6):R207.
Ebina K, Shi K, Hirao M, et al. Vitamin K2 administration is associated with decreased disease activity in patients with rheumatoid arthritis. Mod Rheumatol. 2013;23(5):1001-7.
Edwards JC, et al. Efficacy of β-cell-targeted therapy with rituximab in patients with rheumatoid arthritis. N Engl J Med, 2004. 350(25):2572-81.
Endres S, et al. The effect of dietary supplementation with n-3 polyunsaturated fatty acids on the synthesis of interleukin-1 and tumor necrosis factor by mononuclear cells. N Engl J Med, 1989. 320(5):265-71.
Etzel R. Special extract of BOSWELLIA serrata (H 15) in the treatment of rheumatoid arthritis. Phytomedicine. May 1996;3(1):91-4. doi:10.1016/s0944-7113(96)80019-5. https://pubmed.ncbi.nlm.nih.gov/23194870/
Faloon W. "ARTHRITIS UPDATE: Drugs That Inhibit COX-2 May Cause Tissue Damage" Life Extension magazine, 1/2001.
Feng Z, Xu J, He G, Cao M, Duan L, Chen L, Wu Z. The Efficacy and Safety of the Combination of Total Glucosides of Peony and Leflunomide for the Treatment of Rheumatoid Arthritis: A Systemic Review and Meta-Analysis. Evidence-based complementary and alternative medicine: eCAM. 2016;2016:9852793.
Feng Z-T, Xu J, He G-C, Cai S-J, Li J, Mei Z-G. A systemic review and meta-analysis of the clinical efficacy and safety of total glucosides of peony combined with methotrexate in rheumatoid arthritis. Clinical rheumatology. 2018;37(1):35-42. doi:10.1007/s10067-017-3770-y
FDA Import Refusal Report. Available at http://www.accessdata.fda.gov/scripts/importrefusals/ir_detail.cfm?EntryId=UPS-2301487-7&DocId=1&LineId=1&SfxId= Accessed 2/8/2012.
Flint-Wagner HG, et al. Assessment of a sixteen-week training program on strength, pain, and function in rheumatoid arthritis patients. J Clin Rheumatol, 2009. 15(4):165-71.
Fouda AM and Berika MY. Evaluation of the effect of hydroalcoholic extract of Zingiber officinale rhizomes in rat collagen-induced arthritis. Basic Clin Pharmacol Toxicol, 2009. 104(3):262-71.
Funk JL, et al. Comparative effects of two gingerol-containing Zingiber officinale extracts on experimental rheumatoid arthritis. J Nat Prod, 2009. 72(3):403-7.
Gheita TA and Kenawy SA. Effectiveness of Nigella sativa Oil in the Management of Rheumatoid Arthritis Patients: A Placebo Controlled Study. Phytother Res, 2011.
Gold Standard. Drug Monograph. Methotrexate. www.clinicalkey.com. Last updated 2016. Accessed 10/7/2016.
Goldberg RJ and Katz J. A meta-analysis of the analgesic effects of omega-3 polyunsaturated fatty acid supplementation for inflammatory joint pain. Pain, 2007. 129(1-2):210-23.
Gopinath K and Danda D. Supplementation of 1,25 dihydroxy vitamin D3 in patients with treatment naive early rheumatoid arthritis: a randomised controlled trial. Int J Rheum Dis, 2011. 14(4):332-9.
Grober U, Reichrath J, Holick M, et al. Vitamin K: an old vitamin in a new perspective. Dermatoendocrinol. 2014;6(1):e968490.
Grzanna R, Lindmark L, Frondoza CG. Ginger--an herbal medicinal product with broad anti-inflammatory actions. J Med Food, 2005. 8(2):125-32.
Haqqi TM, et al. Prevention of collagen-induced arthritis in mice by a polyphenolic fraction from green tea. Proc Natl Acad Sci U S A, 1999. 96(8):4524-9.
He DY, Dai SM. Anti-inflammatory and immunomodulatory effects of paeonia lactiflora pall., a traditional chinese herbal medicine. Frontiers in pharmacology.2011;2:10.
Henrotin Y, et al. Biological actions of curcumin on articular chondrocytes. Osteoarthritis Cartilage, 2010. 18(2):141-9.
Holub BJ. Clinical nutrition: 4. Omega-3 fatty acids in cardiovascular care. CMAJ : Canadian Medical Association journal = journal de l'Association medicale canadienne, 2002. 166(5):608-15.
Hua J, et al. Evaluation of the suppressive actions of glucosamine on the interleukin-1beta-mediated activation of synoviocytes. Inflamm Res, 2007. 56(10):432-8.
Huang SC, et al. Vitamin B(6) supplementation improves pro-inflammatory responses in patients with rheumatoid arthritis. Eur J Clin Nutr, 2010. 64(9):1007-13.
Ierna M, et al. Supplementation of diet with krill oil protects against experimental rheumatoid arthritis. BMC musculoskeletal disorders, 2010. 11:136.
Jackson JK, et al. The antioxidants curcumin and quercetin inhibit inflammatory processes associated with arthritis. Inflamm Res, 2006. 55(4):168-75.
James M, Proudman S, Cleland L. Fish oil and rheumatoid arthritis: past, present and future. Proc Nutr Soc, 2010. 69(3):316-23.
James MJ and Cleland LG, Dietary n-3 fatty acids and therapy for rheumatoid arthritis. Semin Arthritis Rheum, 1997. 27(2):85-97.
Jia XY, Chang Y, Sun XJ, et al. Total glucosides of paeony inhibit the proliferation of fibroblast-like synoviocytes through the regulation of G proteins in rats with collagen-induced arthritis. International immunopharmacology.Jan 2014;18(1):1-6.
Juanola-Falgarona M, Salas-Salvado J, Estruch R, et al. Association between dietary phylloquinone intake and peripheral metabolic risk markers related to insulin resistance and diabetes in elderly subjects at high cardiovascular risk. Cardiovasc Diabetol. 2013;12(7).
Ju YH, et al. beta-Sitosterol, beta-Sitosterol Glucoside, and a Mixture of beta-Sitosterol and beta-Sitosterol Glucoside Modulate the Growth of Estrogen-Responsive Breast Cancer Cells In Vitro and in Ovariectomized Athymic Mice. J Nutr. 2004 May;134(5):1145-51.
Jurgens MS, Jacobs JW, and Bijlsma JW. The use of conventional disease-modifying anti-rheumatic drugs in established RA. Best Pract Res Clin Rheumatol, 2011. 25(4):523-33.
Kahlenberg JM and Fox DA. Advances in the medical treatment of rheumatoid arthritis. Hand Clin, 2011. 27(1):11-20.
Karlson EW, et al. A prospective study of androgen levels, hormone-related genes and risk of rheumatoid arthritis. Arthritis Res Ther. 2009;11(3):R97. Epub 2009 Jun 25.
Keystone E, et al. Rituximab inhibits structural joint damage in patients with rheumatoid arthritis with an inadequate response to tumour necrosis factor inhibitor therapies. Ann Rheum Dis, 2009. 68(2):216-21.
Khan F, et al. The role of endothelial function and its assessment in rheumatoid arthritis. Nat Rev Rheumatol. 2010 May;6(5):253-61. Epub 2010 Mar 30.
Kim HR, et al. Green tea protects rats against autoimmune arthritis by modulating disease-related immune events. J Nutr, 2008. 138(11):2111-6.
Klippel, JH. The pocket primer on the rheumatic diseases. 2nd ed2010, Atlanta, GA: Arthritis Foundation. p.242.
Kremer JM, et al. Effects of manipulation of dietary fatty acids on clinical manifestations of rheumatoid arthritis. Lancet, 1985. 1(8422):184-7.
Kumar R, Singh S, Saksena AK, Pal R, Jaiswal R, Kumar R. Effect of Boswellia Serrata Extract on Acute Inflammatory Parameters and Tumor Necrosis Factor-α in Complete Freund's Adjuvant-Induced Animal Model of Rheumatoid Arthritis. Int J Appl Basic Med Res. Apr-Jun 2019;9(2):100-106. doi:10.4103/ijabmr.IJABMR_248_18. https://pubmed.ncbi.nlm.nih.gov/31041173/
Lee JH and Kim GH. Evaluation of antioxidant and inhibitory activities for different subclasses flavonoids on enzymes for rheumatoid arthritis. J Food Sci, 2010. 75(7):H212-7.
Leventhal LJ, Boyce EG, Zurier RB. Treatment of rheumatoid arthritis with gammalinolenic acid. Ann Intern Med, 1993. 119(9):867-73.
Leventhal LJ, Boyce EG, Zurier RB. Treatment of rheumatoid arthritis with blackcurrant seed oil. Br J Rheumatol, 1994. 33(9):847-52.
Life Extension. Available at: http://www.lifeextension.com/HealthWellness/ClinicalResearch/StudyDetails.aspx?study=CL025 Accessed 2/10/2012.
Lin J, Xiao L, Ouyang G, et al. Total glucosides of paeony inhibits Th1/Th17 cells via decreasing dendritic cells activation in rheumatoid arthritis. Cell Immunol.Dec 2012;280(2):156-163.
Lindler BN, Long KE, Taylor NA, Lei W. Use of Herbal Medications for Treatment of Osteoarthritis and Rheumatoid Arthritis. Medicines (Basel, Switzerland). Oct 28 2020;7(11)doi:10.3390/medicines7110067
Liu B, Meng X, Ma Y, et al. Clinical safety of total glucosides of paeony adjuvant therapy for rheumatoid arthritis treatment: a systematic review and meta-analysis. BMC Complement Med Ther. Mar 26 2021;21(1):102. doi:10.1186/s12906-021-03252-y
Liu GL, Li YC, Shen YJ. [Inhibitory effect of total glucosides of paeonia on the NF-kappaB/p65 protein expression in paws of RA rats]. Xi bao yu fen zi mian yi xue za zhi = Chinese journal of cellular and molecular immunology.Nov 2010;26(11):1082-1084.
Liu J, Wang ZT, Ge BX. Andrograpanin, isolated from Andrographis paniculata, exhibits anti-inflammatory property in lipopolysaccharide-induced macrophage cells through down-regulating the p38 MAPKs signaling pathways. Int Immunopharmacol. 2008 Jul;8(7):951-8.
Liu J, Wang ZT, Ji LL, Ge BX. Inhibitory effects of neoandrographolide on nitric oxide and prostaglandin E2 production in LPS-stimulated murine macrophage. Mol Cell Biochem. 2007 Apr;298(1-2):49-57.
Liu J, Wang ZT, Ji LL. In vivo and in vitro anti-inflammatory activities of neoandrographolide. Am J Chin Med. 2007;35(2):317-28.
Louw I, et al. A pilot study of the clinical effects of a mixture of beta-sitosterol and beta-sitosterol glucoside in active rheumatoid arthritis (RA). Am J Clin Nutr 2002 75: 2 339S-439S [abstract 40].
Ma MH, Kingsley GH, and Scott DL. A systematic comparison of combination DMARD therapy and tumour necrosis inhibitor therapy with methotrexate in patients with early rheumatoid arthritis. Rheumatology (Oxford), 2010. 49(1):91-8.
Macfarlane GJ, et al. Evidence for the efficacy of complementary and alternative medicines in the management of rheumatoid arthritis: a systematic review. Rheumatology (Oxford), 2011. 50(9):1672-83.
Manganelli P and Rioda WT. [Weekly low-dose methotrexate in rheumatoid arthritis. Review of the literature]. Minerva medica, 1993. 84(10):541-52.
Martinez-Calatrava MJ, Largo R, Herrero-Beaumont G. Improvement of experimental accelerated atherosclerosis by chondroitin sulphate. Osteoarthritis Cartilage, 2010. 18 Suppl 1:S12-6.
Masi AT, et al. Sex hormones and risks of rheumatoid arthritis and developmental or environmental influences. Ann N Y Acad Sci. 2006 Jun;1069:223-35.
McCormack PL. Celecoxib: a review of its use for symptomatic relief in the treatment of osteoarthritis, rheumatoid arthritis and ankylosing spondylitis. Drugs, 2011. 71(18): 2457-89.
Mikuls TR, et al. The association of race and ethnicity with disease expression in male US veterans with rheumatoid arthritis. J Rheumatol, 2007. 34(7):1480-4.
Moreland LW and O'Dell JR. Glucocorticoids and rheumatoid arthritis: back to the future? Arthritis Rheum, 2002. 46(10):2553-63.
Naik SR, Hule A. Evaluation of immunomodulatory activity of an extract of andrographolides from Andographis paniculata. Planta Med. 2009 Jun;75(8):785-91.
Nakamura H, et al. Effects of glucosamine administration on patients with rheumatoid arthritis. Rheumatol Int, 2007. 27(3):213-8.
Natarajan V, et al. Formulation and evaluation of quercetin polycaprolactone microspheres for the treatment of rheumatoid arthritis. J Pharm Sci, 2011. 100(1):195-205.
Nell VP, et al. Benefit of very early referral and very early therapy with disease-modifying anti-rheumatic drugs in patients with early rheumatoid arthritis. Rheumatology (Oxford), 2004. 43(7):906-14.
Nesher G, Osborn TG, Moore TL. In vitro effects of methotrexate on polyamine levels in lymphocytes from rheumatoid arthritis patients. Clin Exp Rheumatol, 1996. 14(4):395-9.
NIAMS. Rheumatoid Arthritis. 2009 December 9, 2011]; Available from: http://www.niams.nih.gov/Health_Info/Rheumatic_Disease/default.asp.
Nievergelt A, et al. Ginger phenylpropanoids inhibit IL-1beta and prostanoid secretion and disrupt arachidonate-phospholipid remodeling by targeting phospholipases A2. J Immunol, 2011. 187(8):4140-50.
Ohsaki Y, Shirakawa H, Hiwatashi K, et al.Vitamin K Suppresses Lipopolysaccharide-Induced Inflammation in the Rat. Bioscience, Biotechnology, and Biochemistry. 2006;70(4):926-932.
Okamoto H, Shidara K, Hoshi D, et al. Anti-arthritis effects of vitamin K(2) (menaquinone-4)--a new potential therapeutic strategy for rheumatoid arthritis. The FEBS J. 2007;274(17):4588-94.
Olendzki BC, et al. Treatment of rheumatoid arthritis with marine and botanical oils: influence on serum lipids. Evid Based Complement Alternat Med, 2011. 2011: Article ID 827286. doi: 10.1155/2011/827286.
Park YB, et al. Lipid profiles in untreated patients with rheumatoid arthritis. J Rheumatol, 1999. 26(8):1701-4.
Pearson TA, et al. AHA Guidelines for Primary Prevention of Cardiovascular Disease and Stroke: 2002 Update: Consensus Panel Guide to Comprehensive Risk Reduction for Adult Patients Without Coronary or Other Atherosclerotic Vascular Diseases. American Heart Association Science Advisory and Coordinating Committee. Circulation, 2002. 106(3):388-91.
Peters MJ, et al. Does rheumatoid arthritis equal diabetes mellitus as an independent risk factor for cardiovascular disease? A prospective study. Arthritis Rheum, 2009. 61(11): 1571-9.
Pietschmann P. Principles of osteoimmunology: molecular mechanisms and clinical applications 2011, New York: Springer.
Plasqui G. The role of physical activity in rheumatoid arthritis. Physiol Behav, 2008. 94(2):270-5.
Radovits BJ, et al. Excess mortality emerges after 10 years in an inception cohort of early rheumatoid arthritis. Arthritis Care Res (Hoboken), 2010. 62(3):362-70.
Ramadan G, Al-Kahtani MA, El-Sayed WM. Anti-inflammatory and anti-oxidant properties of Curcuma longa (turmeric) versus Zingiber officinale (ginger) rhizomes in rat adjuvant-induced arthritis. Inflammation, 2011. 34(4):291-301.
Rheaume-Bleue K. Choosing the Right Vitamin K2: Menaquinone-4 vs Menaquinone-7: Clinical considerations of different forms of vitamin K2. Natural Medicine Journal. 2015;7(10).
Ridker PM and Solomon DH. Should patients with rheumatoid arthritis receive statin therapy? Arthritis Rheum, 2009. 60(5):1205-9.
Ruffing V and Bingham III CO. Rheumatoid Arthritis Clinical Presentation. Accessed 3/20/12. Available from: http://www.hopkins-arthritis.org/arthritis-info/rheumatoid-arthritis/rheum_clin_pres.html.
Rutjes AW, et al. S-Adenosylmethionine for osteoarthritis of the knee or hip. Cochrane Database Syst Rev, 2009(4):CD007321.
Sethi V, Garg M, Herve M, Mobasheri A. Potential complementary and/or synergistic effects of curcumin and boswellic acids for management of osteoarthritis. Therapeutic advances in musculoskeletal disease. 2022;14:1759720x221124545. doi:10.1177/1759720x221124545. https://pubmed.ncbi.nlm.nih.gov/36171802/
Shabanova SS, et al. Ovarian function and disease activity in patients with systemic lupus erythematosus. Clin Exp Rheumatol. 2008 May-Jun;26(3):436-41.
Sheng X, et al. Effectiveness of Statins on Total Cholesterol and Cardiovascular Disease and All-cause Mortality in Osteoarthritis and Rheumatoid Arthritis. J Rheumatol, 2011.
Shukla M, et al. Consumption of hydrolyzable tannins-rich pomegranate extract suppresses inflammation and joint damage in rheumatoid arthritis. Nutrition, 2008. 24(7-8):733-43.
Simopoulos AP. Evolutionary aspects of diet: the omega-6/omega-3 ratio and the brain. Mol Neurobiol. 2011 Oct;44(2):203-15. Epub 2011 Jan 29.
Soeken KL, et al. Safety and efficacy of S-adenosylmethionine (SAMe) for osteoarthritis. J Fam Pract, 2002. 51(5):425-30.
Spector TD, et al. Risk of vertebral fracture in women with rheumatoid arthritis. BMJ, 1993. 306(6877):558.
St. Clair EW, Pisetsky DS, and Haynes BJ. Rheumatoid arthritis 2004, Philadelphia: Lippincott Williams & Wilkins. xiv, p.555.
Stoll D, et al. High prevalence of hypovitaminosis D in a Swiss rheumatology outpatient population. Swiss Med Wkly. 2011 May 27;141:w13196. doi: 10.4414/smw.2011.13196.
Straub RH, et al. Circadian rhythms in rheumatoid arthritis: implications for pathophysiology and therapeutic management. Arthritis Rheum. 2007 Feb;56(2):399-408.
Tak PP and Kalden JR. Advances in rheumatology: new targeted therapeutics. Arthritis Res Ther, 2011. 13 Suppl 1:S5.
Talbott SM and Hughes K. The health professional's guide to dietary supplements2007, Philadelphia: Lippincott Williams & Wilkins. xx, p.444.
Tanasescu C, et al. Endothelial dysfunction in inflammatory rheumatic diseases. Rom J Intern Med. 2009;47(2):103-8.
Tekeoglu I, et al. Effects of thymoquinone (volatile oil of black cumin) on rheumatoid arthritis in rat models. Phytother Res. 2007 Sep;21(9):895-7.
Trelle S, et al. Cardiovascular safety of non-steroidal anti-inflammatory drugs: network meta-analysis. BMJ, 2011. 342:c7086.
Tyndall A. Successes and failures of stem cell transplantation in autoimmune diseases. Hematology Am Soc Hematol Educ Program, 2011. 2011:280-4.
Valensa. FlexPro MD Clinical Trial Overview and Results. (Data on File.) 2011
van Aken J, et al. Radiological outcome after four years of early versus delayed treatment strategy in patients with recent onset rheumatoid arthritis. Ann Rheum Dis, 2004. 63(3):274-9.
Van den Ende CH, et al. Dynamic exercise therapy in rheumatoid arthritis: a systematic review. Br J Rheumatol, 1998. 37(6):677-87.
van Gestel AM, et al. Oral steroids as bridge therapy in rheumatoid arthritis patients starting with parenteral gold. A randomized double-blind placebo-controlled trial. Br J Rheumatol, 1995. 34(4):347-51.
van Halm VP, et al. Lipids and inflammation: serial measurements of the lipid profile of blood donors who later developed rheumatoid arthritis. Ann Rheum Dis, 2007. 66(2): 184-8.
Wang Y, Xing HY. [Clinical observation on effect of total glucosides of paeony combined with methotrexate on rheumatoid arthritis]. Zhongguo Zhong xi yi jie he za zhi Zhongguo Zhongxiyi jiehe zazhi = Chinese journal of integrated traditional and Western medicine / Zhongguo Zhong xi yi jie he xue hui, Zhongguo Zhong yi yan jiu yuan zhu ban.Sep 2007;27(9):839-840.
Wang YN, Zhang Y, Wang Y, Zhu DX, Xu LQ, Fang H, Wu W. The beneficial effect of total glucosides of paeony on psoriatic arthritis links to circulating Tregs and Th1 cell function. Phytotherapy research: PTR.Mar 2014;28(3):372-381.
Wei CC, You FT, Mei LY, Jian S, Qiang CY. Total glucosides of paeony prevents juxta-articular bone loss in experimental arthritis. BMC complementary and alternative medicine. 2013;13:186.
Weiss EP, et al. droepiandrosterone (DHEA) replacement decreases insulin resistance and lowers inflammatory cytokines in aging humans. Aging (Albany NY). 2011 May;3(5):533-42.
Weitoft T, et al. Serum levels of sex steroid hormones and matrix metalloproteinases after intra-articular glucocorticoid treatment in female patients with rheumatoid arthritis. Ann Rheum Dis. 2008 Mar;67(3):422-4. Epub 2007 Sep 18.
Whittle SL and Hughes RA. Folate supplementation and methotrexate treatment in rheumatoid arthritis: a review. Rheumatology (Oxford), 2004. 43(3):267-71.
Youssef PP, et al. Effects of pulse methylprednisolone on inflammatory mediators in peripheral blood, synovial fluid, and synovial membrane in rheumatoid arthritis. Arthritis Rheum, 1997. 40(8):1400-8.
Yukioka M, et al. Adrenocorticotropic hormone and dehydroepiandrosterone sulfate levels of rheumatoid arthritis patients treated with glucocorticoids. Mod Rheumatol. 2006;16(1):30-5.
Xiang N, Li XM, Zhang MJ, et al. Total glucosides of paeony can reduce the hepatotoxicity caused by Methotrexate and Leflunomide combination treatment of active rheumatoid arthritis. International immunopharmacology.Sep 2015;28(1):802-807.
Zhai T, Sun Y, Li H, et al. Unique immunomodulatory effect of paeoniflorin on type I and II macrophages activities. Journal of pharmacological sciences.Mar 2016;130(3):143-150.
Zhang J, Li H, Huo R, et al. Paeoniflorin selectively inhibits LPS-provoked B-cell function. Journal of pharmacological sciences.May 2015;128(1):8-16.
Zhang W, Dai SM. Mechanisms involved in the therapeutic effects of Paeonia lactiflora Pallas in rheumatoid arthritis. International immunopharmacology.Sep 2012;14(1):27-31.
Zhao YX, Liu Y. [Clinical observation on effects of leflunomid and total glucosides of paeony on rheumatoid arthritis]. Zhongguo Zhong xi yi jie he za zhi Zhongguo Zhongxiyi jiehe zazhi = Chinese journal of integrated traditional and Western medicine / Zhongguo Zhong xi yi jie he xue hui, Zhongguo Zhong yi yan jiu yuan zhu ban.Apr 2006;26(4):355-357.
Zheng YQ, Wei W, Zhu L, Liu JX. Effects and mechanisms of Paeoniflorin, a bioactive glucoside from paeony root, on adjuvant arthritis in rats. Inflammation research: official journal of the European Histamine Research Society ... [et al.].May 2007;56(5):182-188.
Zwerina K, et al. Vitamin D receptor regulates TNF-mediated arthritis. Ann Rheum Dis, 2011. 70(6):1122-9.
