Life Extension Magazine®
The term “inflammation” is used in so many different ways that the role of chronic inflammation in accelerating degenerative processes remains largely overlooked.
Endless advertisements tout drugs (like ibuprofen) that temporarily relieve localized pain.
Other ads promote immune-modulating drugs that help suppress rheumatoid-like disease, but have deadly side effect risks.
Few realize that normal aging ignites low-level inflammation that causes or contributes to virtually every chronic disease.1-4
What you need to know
The Anti-Inflammatory Benefits of GLA
- GLA is an anti-inflammatory compound that is found in very small amounts in some leafy greens and nuts, while the pro-inflammatory fats linoleic acid and arachidonic acid are present in ample amounts in vegetable oils and chicken, and eggs and meat, respectively.
- Chronic inflammation throughout the body contributes to numerous diseases.
- Supplementing with GLA may reduce chronic low-grade inflammation and provide benefit to patients with rheumatoid arthritis, osteoporosis, cancer, atopic dermatitis, and acute respiratory
Most readers of Life Extension Magazine® take definitive steps to reduce their inflammatory burden. This includes avoiding toxic foods and supplementing with curcumin, fish oil, vitamin D, and other nutrients that have specific inflammation-reducing properties.
This article describes published scientific findings as to how gamma-linolenic acid (GLA) and healthier diets can suppress chronic inflammatory reactions that are a leading killer of aging Americans.
Inflammation seems to be the buzzword these days, and for good reason.
Chronic inflammation underlies major diseases of aging, from cancer and atherosclerosis, to arthritis and diabetes.5
Unhealthy dietary patterns contribute to today’s inflammation epidemic.6
Getting at root causes of chronic inflammatory disorders can play a major role in achieving maximum longevity and optimal healthspan.
Healthy fats such as gamma-linolenic acid (GLA) and omega-3s work by several pathways to reduce the dangers of inflammation throughout the body.
What is Inflammation?

When most people stub their toe or hit their elbow, they take an aspirin or ibuprofen to suppress the inflammation. These over-the-counter anti-inflammatory medications work by reducing pro-inflammatory substances.
Acute inflammation is beneficial, as it allows for the healing of a cut or wound, which, if left uncontrolled, could lead to infection or even death. Once inflammation is no longer necessary, the body has mechanisms that turn it off.
The body uses two particular fats to “turn on” and “turn off” inflammation:
An omega-6 fat called arachidonic acid forms necessary pro-inflammatory substances like prostaglandin E2.
Omega-3 fats produce anti-inflammatory substances that bring the overall state of inflammation into balance.
Consuming too many omega-6 fats—while not eating enough omega-3s—contributes to uncontrolled systemic inflammation, which can cause chronic degenerative illnesses associated with pathological aging.
One way the body controls inflammation is by balancing anti-inflammatory substances from omega-3s and pro-inflammatory substances from omega-6 fats.
Understanding Dietary Fats
For optimal health, we must ingest both omega-3 and omega-6 fats. While necessary in moderate amounts, most Americans overconsume omega-6-rich foods, while they underconsume foods that provide EPA and DHA.
Omega-6 fats are known for their pro-inflammatory properties.
But not all omega-6 fats are pro-inflammatory. Of particular interest is the omega-6 fat GLA (gamma-linolenic acid), which has remarkable anti-inflammation mechanisms.
GLA is found in trace amounts in some nuts and green leafy vegetables. The body can make small amounts of GLA from linoleic acid. As a result of this small amount of production by the body, GLA has been called a conditionally essential nutrient.7,8
What is the Ideal Dose of GLA?
The studies reported in this article describe effective daily doses of GLA of 360 mg, 450 mg, 480 mg, 540 mg, 1,130 mg, 2,000 mg and in one study extending up 2,800 mg.
Research that Life Extension® uncovered two decades ago indicates that if one supplements with omega-3-rich fish oil, then lower doses (400 mg) of GLA may be all that are needed.
Also, the addition of sesame lignans to a GLA formula can enhance its efficacy by guiding GLA down an anti-inflammatory pathway (see charts and descriptions on next two pages).
So most of you should consider initiating 400 mg of GLA with sesame lignans daily. If there are not noticeable improvements in a week or two, then slowly increase dose until desired results are obtained.
There is nothing wrong with starting off at higher doses, but for most readers of this magazine who supplement with omega-3s, lower doses of GLA (with sesame lignans) may be all that are needed.
Rheumatoid Arthritis
Patients with rheumatoid arthritis have inflamed, swollen, and painful joints due to an overactive immune system. Evidence suggests that the anti-inflammatory effects of GLA can provide benefit to those with this disease.
One study found that supplementing rheumatoid arthritis patients with borage oil (providing 1.4 grams of GLA daily) for six months significantly improved joint tenderness, swelling, and pain.9
Another study in rheumatoid arthritis patients found meaningful improvements in over 75% of participants when given 2.8 grams of GLA a day for 12 months.10
A third study in rheumatoid arthritis patients found that supplementation with 2 grams of GLA/day for six months improved joint tenderness.11
Finally, a study in rheumatoid arthritis patients found that those who were given 540 mg of GLA/day or 450 mg GLA/day plus 240 mg EPA had significant subjective improvement in their disease state and a significant reduction in the use of NSAIDs (anti-inflammatory pain relievers). Moreover, once the patients were switched over to placebo they had a relapse in their disease state.
The authors concluded that GLA and the combination of GLA/fish oil, “…produce a subjective improvement and allow some patients to reduce or stop treatment with NSAIDs.”12
This study indicates that supplementation with GLA and fish oil containing EPA/DHA may be particularly beneficial in those suffering from rheumatoid arthritis.
Risk Factors for GLA Deficiency
 |
- Formula feeding
- Insulin resistance
- Advanced age
- Smoking
- Consumption of alcohol, refined sugars, trans fats, and partially hydrogenated oils
- Deficiency in magnesium and zinc
- Deficiency in vitamins B3, B6, C, and E
Bone Health
It is estimated that 200 million people worldwide suffer from osteoporosis.13 Osteoporosis primarily affects the elderly, including 30% of postmenopausal women in the United States and Europe.13
Supplementation of GLA and EPA can improve bone health by enhancing calcium absorption and deposition of calcium into bones.
In one clinical study, 65 elderly women with a history of a diet low in calcium were assigned to receive either a combination of GLA plus EPA or a coconut oil placebo for 18 months. In addition, all participants received a calcium supplement.
The supplement combination, GLA/EPA plus calcium, increased the bone mineral density of the femur (the long, thick bone in the thigh) and helped maintain mineral density in the lumbar spine compared to the placebo group. In contrast, women who took the placebo plus calcium lost mineral density in the lumbar spine.14
This suggests that the correct fats serve as beneficial signaling molecules to help properly orchestrate what happens to vitamins and minerals in your body, including your bones.
Increasing and maintaining bone strength is important over time because our body’s capacity to heal declines with age.
Supplementing daily with GLA and omega-3s may improve bone health in the elderly.14
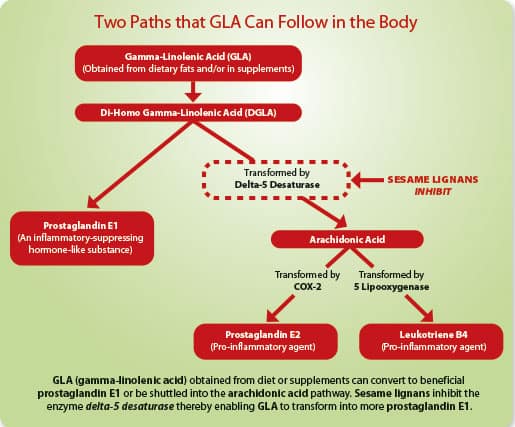
How Sesame Helps Optimize GLA
Gamma-Linolenic Acid (GLA) reduces inflammation by converting to prostaglandin E1 in the body.36-39
If GLA goes down the wrong pathway and excessively converts to arachidonic acid, then greater levels of inflammation may occur.
Sesame lignans suppress the enzyme that causes GLA to excessively convert into arachidonic acid.37
By blocking the delta-5 desaturase enzyme with sesame lignans, more GLA can be converted to beneficial prostaglandin E1, which helps suppress inflammatory reactions.36-39
Eczema
Atopic dermatitis, also called eczema, is a common condition, particularly in children.
Symptoms may include red, itchy, scaly rashes and vary in location depending on age (scalp, forehead, and face, including cheeks). While conventional treatments include topical creams and steroids as well as oral antihistamines, these treat symptoms rather than the root of the problem.
One of the underlying causes of atopic dermatitis in infants may be insufficient delta-6-desaturase activity, the enzyme responsible for converting linoleic acid to GLA. Patients with atopic dermatitis or eczema have low levels of GLA but adequate levels of linoleic acid, suggesting impaired conversion of linoleic acid to GLA.15
Additionally, many infant formulas, unlike breast milk, are low in GLA. Thus, formula-fed infants in particular are at risk of GLA deficiency and may benefit from GLA supplementation.16
Numerous studies show that GLA is helpful for patients with atopic dermatitis and eczema.17-25 A meta-analysis of 26 clinical studies in 1,207 patients established that GLA is beneficial for itch/pruritus, crusting, edema, and redness.26
Painkiller Drug Price Jumps Astronomically
In the latest example of out-of-control drug costs, a manufacturer has increased the price of a painkiller to 22 times its original 2013 cost, bringing it to an astounding $2,979 per bottle.*
The Irish company Horizon Pharma’s incredible price-hike of Vimovo is particularly notable because the drug is comprised of naproxen and esomeprazole, two medications that are available separately for much less—about $36 total.
Horizon Pharma insists that the nearly three-grand wholesale price is not passed down to consumers, who usually pay a fraction of that amount. But critics say it exemplifies a wasteful, complicated system that leads to generally higher sick care insurance costs.
In reaction to the hike, Express Scripts and CVS Caremark—pharmacy benefit managers which negotiate with drug manufacturers on behalf of employers and health insurers—initially put Vimovo on their list of excluded drugs. Horizon responded by setting up rebate deals that lower the cost.
Critics say side agreements, confidential rebates and murky deal-making between drug makers, insurers and pharmacy benefit managers make it very difficult to figure out just who is financially benefiting from jacked-up drug prices.
“There is no transparency,” says Annabel Samimy, a Stifel Financial analyst. “It’s a big black box.”
Editor’s Note: Horizon claims that Vimovo, while made up of naproxen and esomeprazole, is more than just a combination of the two much-cheaper drugs because it is a “special formulation.”
*Available at: https://tinyurl.com/ybbsauwt. Accessed on March 1, 2018.
Diabetic Neuropathy
Damage to the eyes, kidneys, and peripheral nerves are a common consequence of diabetes. These diabetic microvascular complications may be related to an impairment of delta-6 desaturase, the enzyme that converts linoleic acid to GLA.
Loss of delta-6 desaturase activity is a key factor in aging.27
In animal studies, the combination of GLA and EPA can prevent and may even reverse diabetic neuropathy.28 This may be due to an increase in myelin sheath formation and improved nerve-conduction velocities.
In humans, a randomized trial of 22 diabetic patients with peripheral neuropathy was conducted using 360 mg of GLA a day. After six months, there were clinical improvements in neuropathy symptom scores, whereas those in the placebo group remained unchanged or deteriorated.29
A larger, randomized, double-blind trial, the Gamma-Linolenic Acid Multicenter Trial Group, compared placebo to GLA (480 mg/day) in 111 patients with mild diabetic neuropathy for one year. People in the GLA-supplemented group showed favorable results compared to placebo based on 16 parameters tested.30
Acute Respiratory Distress and Asthma
Critically ill patients with acute respiratory distress syndrome caused by sepsis/pneumonia, trauma, or aspiration injury improved when given tube-feeding nutrition that combined GLA, EPA, and antioxidants. This study noted a reduction in the requirement for ventilation, length of intensive care-unit stay, and reduced organ failure.31
Low (750 mg/day GLA + 500 mg/day EPA) and high dose (1,130 mg/day GLA + 750 mg/day EPA) supplementation with GLA plus EPA has been found to benefit mild-to-moderate asthmatics, improving quality of life and decreasing the reliance on rescue medications.32
Cancer
Breast cancer patients (34 women with nonmetastatic breast cancer and four with metastatic) were supplemented with GLA (2.8 grams/day) plus 20 mg tamoxifen or tamoxifen alone. In the GLA plus tamoxifen group, there was a faster response to treatment and a greater estrogen-receptor fall compared to those taking tamoxifen alone.33
Another study evaluated nine patients with grade four recurrent cerebral glioma, an advanced form of brain cancer. After surgery, radiation, or chemotherapy, a small amount of GLA was delivered directly (by injection) into the brain or the tumor itself for seven consecutive days.
Computed tomography and magnetic resonance imaging showed regression of the brain tumors. The authors concluded that “…GLA is a safe antitumor agent and higher doses of GLA should be investigated in future studies.”34
Placement of GLA (1.0-2.5 mg/ml) directly into the bladder through a catheter (intravesical) was tested in a phase II trial in patients with recurrent, superficial bladder cancer, which is found on the surface of the inside lining of the bladder. A single placement of 50 ml of the intravesical GLA retained for one hour resulted in tumor shrinkage in 43% of the patients.35
The authors concluded that intravesical GLA was safe and well-tolerated and had significant cytotoxic effects against early bladder cancer.
Oral supplementation of GLA or injecting GLA directly into cancerous areas may improve treatment of breast cancer as well as brain and recurrent superficial bladder cancers. These types of treatments require further investigation and larger studies.
Summary
GLA deficiency can be caused by aging, hyperinsulinemia, and a Western diet, which leads to chronic low-grade inflammation and a host of chronic diseases.
Supplementing with anti-inflammatory GLA may provide benefits to patients with rheumatoid arthritis, osteoporosis, cancer, eczema, acute respiratory distress, asthma, and common degenerative disorders.
If you have any questions on the scientific content of this article, please call a Life Extension® Wellness Specialist at 1-866-864-3027.
References
- Xia S, Zhang X, Zheng S, et al. An Update on Inflamm-Aging: Mechanisms, Prevention, and Treatment. J Immunol Res. 2016;2016:8426874.
- Franceschi C, Campisi J. Chronic inflammation (inflammaging) and its potential contribution to age-associated diseases. J Gerontol A Biol Sci Med Sci. 2014;69 Suppl 1:S4-9.
- Franceschi C, Valensin S, Lescai F, et al. Neuroinflammation and the genetics of Alzheimer’s disease: the search for a pro-inflammatory phenotype. Aging (Milano). 2001;13(3):163-70
- .Lencel P, Magne D. Inflammaging: the driving force in osteoporosis? Med Hypotheses. 2011;76(3):317-21.
- Chung HY, Cesari M, Anton S, et al. Molecular inflammation: underpinnings of aging and age-related diseases. Ageing Res Rev. 2009;8(1):18-30.
- Seaman DR. The diet-induced proinflammatory state: a cause of chronic pain and other degenerative diseases? J Manipulative Physiol Ther. 2002;25(3):168-79.
- Gamma-linolenic acid (GLA). Monograph. Altern Med Rev. 2004;9(1):70-8.
- Kapoor R, Huang YS. Gamma linolenic acid: an antiinflammatory omega-6 fatty acid. Curr Pharm Biotechnol. 2006;7(6):531-4.
- Leventhal LJ, Boyce EG, Zurier RB. Treatment of rheumatoid arthritis with gammalinolenic acid. Ann Intern Med. 1993;119(9):867-73.
- Zurier RB, Rossetti RG, Jacobson EW, et al. gamma-Linolenic acid treatment of rheumatoid arthritis. A randomized, placebo-controlled trial. Arthritis Rheum. 1996;39(11):1808-17.
- Leventhal LJ, Boyce EG, Zurier RB. Treatment of rheumatoid arthritis with blackcurrant seed oil. Br J Rheumatol. 1994;33(9):847-52.
- Belch JJ, Ansell D, Madhok R, et al. Effects of altering dietary essential fatty acids on requirements for non-steroidal anti-inflammatory drugs in patients with rheumatoid arthritis: a double blind placebo controlled study. Ann Rheum Dis. 1988;47(2):96-104.
- Available at: https://www.iofbonehealth.org/epidemiology. Accessed June 5, 2018.
- Kruger MC, Coetzer H, de Winter R, et al. Calcium, gamma-linolenic acid and eicosapentaenoic acid supplementation in senile osteoporosis. Aging (Milano). 1998;10(5):385-94.
- Horrobin DF. Fatty acid metabolism in health and disease: the role of delta-6-desaturase. Am J Clin Nutr. 1993;57(5 Suppl):732S-6S; discussion 6S-7S.
- Horrobin DF. Nutritional and medical importance of gamma-linolenic acid. Prog Lipid Res. 1992;31(2):163-94.
- Lovell CR, Burton JL, Horrobin DF. Treatment of atopic eczema with evening primrose oil. Lancet. 1981;1(8214):278.
- Wright S, Burton JL. Oral evening-primrose-seed oil improves atopic eczema. Lancet. 1982;2(8308):1120-2.
- Schalin-Karrila M, Mattila L, Jansen CT, et al. Evening primrose oil in the treatment of atopic eczema: effect on clinical status, plasma phospholipid fatty acids and circulating blood prostaglandins. Br J Dermatol. 1987;117(1):11-9.
- Senapati S, Banerjee S, Gangopadhyay DN. Evening primrose oil is effective in atopic dermatitis: a randomized placebo-controlled trial. Indian J Dermatol Venereol Leprol. 2008;74(5):447-52.
- Hederos CA, Berg A. Epogam evening primrose oil treatment in atopic dermatitis and asthma. Arch Dis Child. 1996;75(6):494-7.
- Guenther L, Wexler D. Efamol in the treatment of atopic dermatitis. J Am Acad Dermatol. 1987;17(5 Pt 1):860.
- Morse PF, Horrobin DF, Manku MS, et al. Meta-analysis of placebo-controlled studies of the efficacy of Epogam in the treatment of atopic eczema. Relationship between plasma essential fatty acid changes and clinical response. Br J Dermatol. 1989;121(1):75-90.
- Bordoni A, Biagi PL, Masi M, et al. Evening primrose oil (Efamol) in the treatment of children with atopic eczema. Drugs Exp Clin Res. 1988;14(4):291-7.
- Biagi PL, Bordoni A, Masi M, et al. A long-term study on the use of evening primrose oil (Efamol) in atopic children. Drugs Exp Clin Res. 1988;14(4):285-90.
- Morse NL, Clough PM. A meta-analysis of randomized, placebo-controlled clinical trials of Efamol evening primrose oil in atopic eczema. Where do we go from here in light of more recent discoveries? Curr Pharm Biotechnol. 2006;7(6):503-24.
- Horrobin DF. Loss of delta-6-desaturase activity as a key factor in aging. Med Hypotheses. 1981;7(9):1211-20.
- Julu PO. Essential fatty acids prevent slowed nerve conduction in streptozotocin diabetic rats. J Diabet Complications. 1988;2(4):185-8.
- Jamal GA, Carmichael H. The effect of gamma-linolenic acid on human diabetic peripheral neuropathy: a double-blind placebo-controlled trial. Diabet Med. 1990;7(4):319-23.
- Keen H, Payan J, Allawi J, et al. Treatment of diabetic neuropathy with gamma-linolenic acid. The gamma-Linolenic Acid Multicenter Trial Group. Diabetes Care. 1993;16(1):8-15.
- Gadek JE, DeMichele SJ, Karlstad MD, et al. Effect of enteral feeding with eicosapentaenoic acid, gamma-linolenic acid, and antioxidants in patients with acute respiratory distress syndrome. Enteral Nutrition in ARDS Study Group. Crit Care Med. 1999;27(8):1409-20.
- Surette ME, Stull D, Lindemann J. The impact of a medical food containing gammalinolenic and eicosapentaenoic acids on asthma management and the quality of life of adult asthma patients. Curr Med Res Opin. 2008;24(2):559-67.
- Kenny FS, Pinder SE, Ellis IO, et al. Gamma linolenic acid with tamoxifen as primary therapy in breast cancer. Int J Cancer. 2000;85(5):643-8.
- Bakshi A, Mukherjee D, Bakshi A, et al. Gamma-linolenic acid therapy of human gliomas. Nutrition. 2003;19(4):305-9.
- Harris NM, Crook TJ, Dyer JP, et al. Intravesical meglumine gamma-linolenic acid in superficial bladder cancer: an efficacy study. Eur Urol. 2002;42(1):39-42.
- Akimoto K, Kitagawa Y, Akamatsu T, et al. Protective effects of sesamin against liver damage caused by alcohol or carbon tetrachloride in rodents. Ann Nutr Metab. 1993;37(4):218-24.
- Chavali SR, Zhong WW, Forse RA. Dietary alpha-linolenic acid increases TNF-alpha, and decreases IL-6, IL-10 in response to LPS: effects of sesamin on the delta-5 desaturation of omega6 and omega3 fatty acids in mice. Prostaglandins Leukot Essent Fatty Acids. 1998;58(3):185-91.
- Fujiyama-Fujiwara Y, Umeda-Sawada R, Kuzuyama M, et al. Effects of Sesamin on the Fatty Acid Composition of the Liver of Rats Fed N-6 and N-3 Fatty Acid-Rich Diet. Journal of Nutritional Science and Vitaminology. 1995;41(2):217-25.
- Shimizu S, Akimoto K, Shinmen Y, et al. Sesamin is a potent and specific inhibitor of delta 5 desaturase in polyunsaturated fatty acid biosynthesis. Lipids. 1991;26(7):512-6.

