Life Extension Magazine®
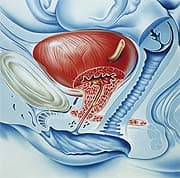
You may be surprised to learn that urinary tract infections (UTIs) are the most common form of bacterial infection, accounting for 7 million office visits, 1 million emergency room visits, and 100,000 hospitalizations each year, at an estimated annual cost of $1.6 billion to the American public.1 One third of all women will contract a UTI by the age of 24.1 Once a woman has contracted a UTI, her risk of recurrence is 20%.2 Conventional medicine typically calls for aggressive treatment with broad-spectrum antibiotics, including trimethoprim, cephalexin, or ciprofloxacin (Cipro®). The deleterious effects of these drugs on women’s health are notorious: fatigue, nausea, digestive distress, secondary infection, and the eventual evolution of resistant bacterial strains impervious to even the most powerful antibiotics. In a little-known development, new data have emerged on a low-cost, natural intervention that until recently was available only in Europe. This extract from the Hibiscus sabdariffa flower not only exerts direct antibacterial action against microorganisms that cause UTIs,3 but it has also been shown to suppress the fungus responsible for common yeast infestations. The natural compounds in hibiscus complement the already well-documented efficacy of cranberry.4,5 In women suffering from chronic UTIs (more than 8 infections per year), 200 mg of hibiscus per day reduced UTI recurrence by a remarkable 77%.6 In this article, you will discover exciting new research on the power of these natural, complementary agents and their unique ability to halt the painful cycle of UTIs. A Dangerous AfflictionThe female anatomy (with a shorter urethra) provides an easy route for harmful bacteria to migrate into the urinary tract.
In general, UTIs originate from the transfer of bacteria—most often Escherichia coli from the GI tract—from the anus to the urethra, where they attach to mucosal cells along the urinary tract, colonize, and proliferate. E. coli is the causal agent in 80-95% of acute, non-complicated UTIs. Staphylococcus saprophyticus accounts for most of the remainder. Harmful bacteria can travel up the urethra, take hold within the bladder, and ultimately ascend into the kidneys. Left unchecked, this can lead to a condition known as pyelonephritis, or kidney infection. Acute pyelonephritis is characterized by shaking chills, flank pain, high fever, and pain in the muscles and joints. Chronic pyelonephritis is a longstanding form of kidney inflammation with symptoms that may be so mild that they go unnoticed. This carries the risk that the infectious inflammatory disease may go undetected as it slowly progresses over many years, until there is enough deterioration to produce kidney failure. In severe cases, pyelonephritis may progress to sepsis (a potentially fatal, whole-body infection of the tissue and bloodstream). A vicious cycle of repeated infection may also take hold. Many women develop multiple UTIs annually. They are typically administered antibiotics with each infection. This may induce unwanted and potentially dangerous side effects, ranging from rash, nausea, dizziness, and the destruction of beneficial microflora in the body that leads to yeast infections (candidiasis). Disorders of the digestive tract, including diarrhea, colitis (inflammation of the colon), and abdominal pain are also commonplace. Women often require further medication to treat the secondary yeast infection that results from antibiotics; these anti-fungal medications may produce even more unwanted, detrimental side effects. The result is a taxing pharmaceutical onslaught that can take an enormous toll on women’s health and well being over time. So-called “superinfections” may even develop—powerfully resistant strains of bacteria that antibiotics are powerless to stop. For this reason, preventing the initial bacterial invasion of the urethra represents a crucial point of intervention in the progress of UTIs. By inhibiting bacterial adhesion to the urethral lining at this early stage, an infection cannot take root. Powerful Protection with ProanthocyanidinsCranberry is the best-known natural preventive option for frequent UTIs. It first emerged as an effective intervention for bladder and urinary tract health in the early twentieth century. Scientists speculated that the benzoic acid in cranberries was metabolized to hippuric acid and excreted in the urine, which prevented bacterial growth by creating an acidic environment in the bladder. Since then a wealth of clinical data have detailed the precise mechanism by which certain constituent components of the whole cranberry act to powerfully counter UTI onset.7-10 The most recent studies do not indicate a change in urine pH brought about by cranberries (meaning they do not acidify urine). Instead, cranberry’s antimicrobial action arises from a class of flavonoids called proanthocyanidins (PACs). In addition to exerting potent antioxidant effects, cranberry PACs block bacteria from taking hold of the cells lining the urinary tract. The surfaces of E. coli and many other bacteria are covered with motile, tendril-like structures called fimbriae. The fimbria acts as a kind of tentacle, enabling bacteria to “grab onto” other microorganisms, inanimate objects and—most importantly—host cells. A single bacterium may possess as many as 1,000 fimbriae. It is this feature that renders E. coli and other species endowed with fimbriae—including Staphylococcus saprophyticus, Salmonella, and Helicobacter pylori—especially virulent and infectious. They employ these structures to latch onto cells in the mucous membranes at multiple sites of the body and initiate a debilitating and potentially lethal proliferation. A 2009 study demonstrated conclusively that cranberry PACs provoke disabling alterations in the fimbriae and other surface properties of the E. coli bacterium, vastly diminishing its capacity to attach specifically to the surface of the cells lining the urinary tract.7
This process, known as bacteriostasis, prevents harmful bacteria from colonizing the urinary tract. Instead, they are flushed from the urethra during the natural voiding process. The bacteriostatic effect of cranberry and its extracts has been well documented.11,12 Just 400-500 mg of cranberry extract has been shown to deprive deleterious microbes of their ability to attach to the mucous membrane and colonize the urinary tract.4,5 In examination of women plagued with recurrent bladder infections (6 or more in the prior year), cranberry extract (200 mg twice daily) completely eliminated UTI incidence. Women who continued cranberry supplementation remained infection-free during the next two years.5 Similar benefits were also revealed in a study of children with chronic UTIs.13 Cranberry beverages can also be effective. In one study, occurrence of UTIs was slashed by half in women consuming cranberry juice (250 mL, or about 8 ounces) three times daily and in women consuming cranberry extract twice daily.14 Recent clinical data further indicate that cranberries may also prevent UTIs in adult women at high risk for urinary infections. Researchers have recorded that older women who consumed 300 mL (about 10 ounces) of a cranberry beverage daily experienced only 42% of the risk of UTI of women who consumed a placebo.15 Women who fall prey to the vicious cycle of chronic UTIs may wind up on low-dose antibiotics for months—or even years. The good news is that this may not be necessary. In 2009, a group of researchers compared antibiotics head-to-head with daily supplements of cranberry extract in women suffering from recurrent infection.16 Cranberry (500 mg) and antibiotics (100 mg trimethoprin) were shown to be almost equally effective in preventing UTIs. Although cranberry was slightly outperformed, it posed none of the many dangers of antibiotics. A further and often overlooked advantage of cranberry extract is cost. In a novel cost effectiveness study, researchers from the University of British Columbia calculated that the amount needed to obtain cranberry’s full bacteriostatic benefit would cost less than half as much in extract form compared to juice.14 Cranberry must be taken daily to prevent UTIs, requiring at least 16 ounces of unsweetened, 100% cranberry juice every day. Low cost one-per-day extracts are also available.
| |||||
A Potent New UTI InterventionNative to Africa and Asia, Hibiscus sabdariffa has been used in some cultures to support bladder and kidney health. Traditional African practitioners use tea brewed from hibiscus calyxes (the green floral envelope of the blossom) as an acidic and anti-bacterial, both to acidify and deodorize urine and protect against UTIs and kidney stone formation. Hibiscus boasts a range of powerful compounds that prevent E. coli from adhering to the urinary tract and bladder wall linings. Both the flower and calyx are abundant in bacteriostatic polyphenols, including flavonoids, sambubiosides, and proanthocyanidins. In particular, the flavonoid gossypetin (3,5,7,8,3,’ 4’-hexahydroxy flavone) found in hibiscus has been identified as a distinct antimicrobial compound with powerful effects.3 Together these natural agents have been shown to inhibit the activity of a host of microbes responsible for UTIs, including E. coli, Staphylococcus aureus, and Pseudomonas aeruginosa. In fact, hibiscus’s mode of prophylaxis (prevention) and high concentration of bacteriostatic compounds may exert bacteriocidal (bacteria-killing) effects comparable to the antibiotic chloramphenicol—with none of the risks. In a double-blind, placebo-controlled, clinical trial, women taking hibiscus experienced a 77% reduction in UTIs.6 Sixty-one women participated in the 6-month study, and 59 women completed the entire study. All of them had a history of frequent UTIs (more than four per year, including one or more in the three months prior to the start of the study). The women were randomly assigned to one of three groups receiving a daily dose of 200 mg of hibiscus extract standardized to 90% polyphenols; 200 mg of hibiscus extract standardized to 60% polyphenols; or placebo. Compared to the control group, women taking the hibiscus concentrations experienced a 77% decrease in infections, as well as overall improvement in urinary comfort. In 2009, a group of researchers compared antibiotics head-to-head with daily supplements of cranberry extract in women suffering from recurrent infection.16 Cranberry (500 mg) and antibiotics (100 mg trimethoprin) were shown to be almost equally effective in preventing UTIs. According to in vitro research, hibiscus also reduces contamination of both E. coli and Candida albicans, the fungus responsible for yeast infections.3,17,18 The antimicrobial effect was found to be immediate and complete after only one day. In addition, when hibiscus was compared to cranberry in vitro, the hibiscus had a stronger antimicrobial effect, particularly against Candida albicans.19 Hibiscus’s bacteriostatic/bacteriocidal compounds are excreted through urine in high concentrations, enabling them to reach the bladder and urinary tract intact, where they disable infectious bacteria.20 Summary
Urinary tract infections (UTIs) are the most common form of bacterial infection, accounting for 7 million office visits, 1 million emergency room visits, and 100,000 hospitalizations each year, with an estimated cost of $1.6 billion annually. One third of all women will contract a UTI by the age of 24. Once a woman has contracted a UTI, her risk of recurrence is 20%. The proanthocyanidins in cranberry effectively prevent UTIs by blocking E. coli from adhering to the urinary tract and bladder. Cranberry is especially effective for women who endure numerous UTIs annually. Studies show that cranberry extract in pill form is more economical than drinking large quantities of 100% cranberry juice. Like cranberry, extract of Hibiscus sabdariffa prevents bacteria that cause UTIs from adhering to the linings of the urinary tract and bladder wall and may also possess bacteriocidal effects. Abundant in polyphenolic compounds, hibiscus may exhibit bacteriocidal (bacteria-killing) properties comparable to the antibiotic chloramphenicol—without the antibiotic’s side effect profile. When compared to cranberry in vitro, hibiscus had a stronger antimicrobial effect, particularly against Candida albicans. If you have any questions on the scientific content of this article, please call a Life Extension® Health Advisor at 1-866-864-3027. Victoria Dolby Toews, MPH has been a health journalist since 1993; her latest book is The Green Tea Book, second edition (Penguin, 2007). | ||
| References | ||
| 1. Foxman B. Epidemiology of urinary tract infections: incidence, morbidity, and economic costs. Am J Med. 2002 Jul 8;113 Suppl 1A:5S-13S. 2. Available at: http://kidney.niddk.nih.gov/Kudiseases/pubs/utiadult/#risk. Accessed January 18, 2010. 3. Mounnissamy VM, Kavimani S, Gunasegaran R. Antibacterial activity of gossypetin isolated from hibiscus sabdariffa. The Antiseptic. 2002 Mar; 99(3): 81-2. 4. Hess MJ, Hess PE, Sullivan MR, Nee M, Yalla SV. Evaluation of cranberry tablets for the prevention of urinary tract infections in spinal cord injured patients with neurogenic bladder. Spinal Cord. 2008 Sep;46(9):622–6. 5. Bailey DT, Dalton C, Joseph Daugherty F, et al. Can a concentrated cranberry extract prevent recurrent urinary tract infections in women? A pilot study. Phytomedicine 2007;14(4):237-41. 6. Allaert F. Double-blind, placebo-controlled study of Hibiscus sabdariffa L extract in the prevention of recurrent cystitis in women. Poster presented at the Federative Pelviperineal Diagnostics and Procedures Meeting: Convergences in Pelviperineal Pain. Nantes, France: December 16-18, 2009. 7. Pinzón-Arango PA, Liu Y, Camesano TA. Role of cranberry on bacterial adhesion forces and implications for Escherichia coli-uroepithelial cell attachment. J Med Food. 2009 Apr;12(2):259-70. 8. Jass J, Reid G. Effect of cranberry drink on bacterial adhesion in vitro and vaginal microbiota in healthy females. Can J Urol. 2009 Dec;16(6):4901-7. 9. Lee YL, Owens J, Thrupp L, Cesario TC. Does cranberry juice have antibacterial activity? JAMA. 2000 Apr 5;283(13):1691. 10. Howell MB. Bioactive compounds in cranberries and their role in prevention of urinary tract infections. Mol Nutr Food Res. 2007 Jun;51(6):732-7. 11. Stothers L. A randomized placebo controlled trial to evaluate naturopathic cranberry products as prophylaxis against urinary tract infection in women. Presented at: American Urological Association 2001 Annual Meeting; June 2-7, 2001; Anaheim, CA; Publ ID:318. 12. Kontiokari T, Sundqvist K, Nuutinen M, et al. Randomised trial of cranberry-lingonberry juice and Lactobacillus GG drink for the prevention of urinary tract infections in women. BMJ. 2001 Jun 30;322(7302):1571. 13. Ferrara P, Romaniello L, Vitelli O, et al. Cranberry juice for the prevention of recurrent urinary tract infections: a randomized controlled trial in children. Scand J Urol Nephrol. 2009;43(5):369-72. 14. Stothers L. A randomized trial to evaluate effectiveness and cost effectiveness of naturopathic cranberry products as prophylaxis against urinary tract infection in women. Can J Urol. 2002 Jun;9(3):1558-62. 15. Avorn J, Monane M, Gurwitz JH, Glynn RJ, Choodnovskiy I, Lipsitz LA. Reduction of bacteriuria and pyuria after ingestion of cranberry juice. JAMA. 1994 Mar 9;27(10):751-4. 16. McMurdo ME, Argo I, Phillips G, Daly F, Davey P. Cranberry or trimethoprim for the prevention of recurrent urinary tract infections? A randomized controlled trial in older women. J Antimicrob Chemother. 2009 Feb;63(2):389-95. 17. Ali BH, Al Wabel N, Blunden G. Phytochemical, pharmacological and toxicological aspects of Hibiscus sabdariffa L.: a review. Phytother Res. 2005 May;19(5):369-75. 18. Rukayadi Y, Shim JS, Hwang JK. Screening of Thai medicinal plants for anticandidal activity. Mycoses. 2008 Jul;51(4):308-12. 19. Burgundy Botanical Extracts. Data on file. 20. Frank T, Janssen M, Netzel M, et al. Pharmacokinetics of anthocyanidin-3-glycosides following consumption of Hibiscus sabdariffa L. extract. J Clin Pharmacol. 2005 Feb;45(2):203-10. |