Life Extension Magazine®
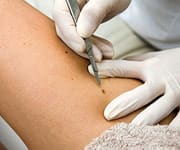
One American dies every hour from melanoma.1 Incidences of this deadly skin cancer are on the increase. Although no cure exists for advanced melanoma, virtually 100% of its victims can be saved if the malignancy is caught early.2 The problem is that dermatologists cannot accurately diagnose a melanoma based on a visual examination alone. A biopsy is needed to definitely ascertain if a skin lesion is a melanoma. Biopsies require expenditure of money and time, along with some minor trauma. Patients and dermatologists have to make decisions as to whether a particular skin lesion warrants a biopsy. In a clinical trial involving 23 dermatologists around the US, a hand-held non-invasive scanning device called MelaFind® was tested on suspicious lesions. Its accuracy in detecting melanoma was 98%—which equaled or bested the top doctors in avoiding unnecessary biopsies.3 MelaFind® was submitted for FDA approval in June 2009. Despite clinical trial results documenting its unprecedented (98%) ability to detect early stage melanoma, the FDA refused to approve it and insisted on further review.4,5 FDA's Lethal IllogicAccording to bureaucratic illogic, the FDA was concerned that non-dermatologists might use MelaFind® to screen for melanoma, even though the company promised to only sell it to dermatologists. Since the FDA cannot regulate doctors, the agency felt that the best way of keeping MelaFind® out of the hands of non-dermatologists was to not approve it at all. The FDA expressed other concerns such as its misuse by dermatologists. This is rather bizarre since dermatologists are the most highly trained in our society to diagnose and treat skin diseases, yet the FDA did not want them to use this new device that was 98% accurate in diagnosing melanoma.6,7 The Real World of Medical Practice
FDA bureaucrats live in a cave when it comes to the intricacies and expenses involved in the real-world medical setting. Hurried people too often ignore suspicious skin lesions until it's too late. Patients often go to their primary care doctor when it comes to suspicious skin lesions. More enlightened individuals visit a dermatologist. Either way, medical efficiency comes into play when deciding whether a suspicious lesion should be biopsied or merely kept an eye on. A dermatologist charges for each biopsy, and there is a separate expense for the pathology lab. Return visits are often needed. All this adds up to medical costs that MelaFind® could otherwise render far more efficient. MelaFind® is not 100% accurate. That means it may miss a few (2%) suspicious lesions that a dermatologist would then have to decide warranted a biopsy nonetheless. The FDA is using this as another reason not to approve it. Using this logic, MRI and ultrasound testing would never have been approved because these are not 100% reliable diagnostic tools either. If ever approved, MelaFind® will provide doctors with an efficient method to detect early stage melanoma. According to some dermatologists, it has the potential to "save many lives."8 There were 68,130 new cases of melanoma in 2010 and 8,700 deaths.9 These numbers show that melanoma can be easily cured—if caught in the early stages before it infiltrates and metastasizes. We at Life Extension® envision a day when devices like MelaFind® will be used in large screening campaigns where early stage melanomas can be easily detected and removed. None of this will happen as long as the FDA is allowed to erect bureaucratic barriers that suppress this kind of medical innovation. FDA Approves Expensive Melanoma DrugCynical individuals might question the timing of the FDA's denial of MelaFind®, a device that could spare thousands of agonizing deaths from metastatic melanoma. Just a few weeks after saying no to MelaFind®, the FDA approved a new drug by pharmaceutical giant Bristol-Meyers Squibb to treat advanced melanoma trademarked Yervoy™.10 In a study involving 676 patients with advanced melanoma, those receiving Yervoy™ survived for 10 months compared to 6.4 months for those who did not receive it. Fourteen patients died from side effects caused by Yervoy™.11 The FDA hailed this as a breakthrough and granted approval for widely spread melanoma. Shares of Bristol-Meyers Squibb surged as analysts predicted a $1.7 billion blockbuster.12 The reason so much money will be made is that it will cost each patient an astounding $120,000 for the four-course treatment.4 For what used to be the price of a nice home, one with terminal melanoma can buy an extra 108 days of life. The average cost per day of added life will be over $1,000—further exacerbating today's health care cost crisis! The generic name for Yervoy™ is ipilimumab. If you ever wonder why you cannot pronounce the names of new compounds (like ipilimumab), it is because pharmaceutical companies intentionally create names that no one can readily comprehend. Pharmaceutical companies do this to make it harder for future generic drug makers to enter the market with lower-cost versions, since virtually no one can pronounce the generic name.
The reason that Yervoy™ (ipilimumab) is expected to sell so well is that current FDA-approved therapies have not been shown to substantially extend survival, but the FDA allowed them to be used for decades anyway. We are not against the FDA's approval of Yervoy™ as it may prove to work better when treating less advanced melanoma. What bothers us are the bureaucratic barriers. They are so cumbersome that few new therapies ever get approved. This enables companies to charge extortionist prices for the few that receive the FDA's coveted anointment. FDA Fails to Approve Effective Lymphoma DrugEach year about 65,000 Americans are diagnosed with non-Hodgkin lymphoma.13 It is estimated to have killed over 20,000 in the US in 2010.14 Jackie Kennedy Onassis died from non-Hodgkin lymphoma at the age of 64.15 Non-Hodgkin lymphoma is one of the few cancers where establishment medicine can brag about treatment breakthroughs. Over the past 50 years, survival rates have more than doubled.16 Often overlooked are long-term side effects like cumulative heart muscle damage that precludes long-term use of certain conventional treatments.17 Lymphoma patients who fail treatment with FDA-approved chemotherapy have a life expectancy measured in weeks or months. A next-generation compound called pixantrone is designed to be less toxic and more effective than current anthracycline chemo drugs. It has successfully gone through phase I and phase II human clinical trials. In 2004, a randomized phase III trial mandated by the FDA was initiated. Pixantrone was administered to non-Hodgkin lymphoma patients who had already failed conventional therapy. The control group received whatever their oncologist thought would work best for them. In these extremely difficult-to-treat lymphoma patients, 20% of those receiving pixantrone showed a complete response, compared to only 6% receiving conventional care.18 A follow-up analysis of the data showed 24% of patients attaining complete response status as opposed to 7% in the standard group.19 These are unprecedented findings! A complete response is not a cure, but it can buy a patient precious time in remission and the opportunity to identify potential curative therapies. Despite almost four years of phase III clinical studies showing that pixantrone works three times better than what's available today, the FDA declined to approve it. In an FDA briefing as to why pixantrone was not approved, the FDA stated:
The "Special Protocol Assessment" is an agreement between the FDA and a drug maker regarding how a clinical study should be done.21 It originally envisioned enrolling 320 patients over a 36-month time period. For various reasons, it took 45 months to recruit 140 patients.22 This is not unusual as some 60% of phase III studies do not meet patient recruitment objectives, but nonetheless generate statistically significant data that are used to approve a new drug. Pixatrone Not Owned by Big PharmaUnlike Bristol-Meyers Squibb, which had the wherewithal to fund a huge clinical study and whose stock soared in response to the FDA's approval of Yervoy™,23 the maker of pixantrone's auditors handed management a notice that the company (Cell Therapeutics) may not be able to continue as a going concern in response to the FDA's refusal to approve their drug.24,25 Cell Therapeutics' initial challenge in enrolling enough study subjects was convincing oncologists and hematologists that pixantrone might work. Patient incentive to participate was minimized because the FDA mandated that only 50% of the study subjects would receive the promising drug (pixantrone). Despite these limitations, Cell Therapeutics believes it generated statistically significant data and has taken the unusual step of appealing the FDA's denial of pixantrone. The reason appeals are seldom filed is fear of FDA retaliation on future drug applications. In the case of Cell Therapeutics, which is not part of Big Pharma, it may have little to risk in asking for a common-sense review of the impressive data it generated in terminally ill lymphoma patients. The inability of Cell Thera-peutics to adhere to the FDA's impossible-to-achieve dictates is an example of a federal agency that went out of its way to railroad a promising cancer therapy.
|