Life Extension Magazine®
It can happen without warning: you slip in the shower and hit your head, a car swerves and hits you, a small stroke occurs and suddenly you can't speak, your mobility is limited, and your world shrinks. These are real-life examples of the often intractable effects of traumatic brain injury or TBI. And thanks to the groundbreaking work of Dr. Mark L. Gordon and a handful of forward-looking physicians, there's new hope for the 1.7 million Americans afflicted with this condition. Using cutting-edge hormone replacement techniques, Gordon and his colleagues are helping to change the way we think about traumatic brain injuries, their symptoms - and how to treat them effectively. In his clinical practice, Dr. Gordon is developing new protocols that may revolutionize the devastating impact of traumatic brain injuries. One of the biggest patient populations in need of urgent care are the soldiers returning from the battlefields of Iraq and Afghanistan. Our story begins with them. Starting with Soldiers
Traumatic brain injury (TBI) is often referred to as the "signature wound" of both the Iraq and Afghanistan wars. Traumatic brain injury occurs when a sudden trauma to the head disrupts brain function. In both these wars, however, even close proximity to the force of an explosion can be just as devastating. Most of the reported traumatic brain injury among Operation Enduring Freedom and Operation Iraqi Freedom veterans has been traced to improvised explosive devices, or IEDs. "Traumatic brain injury can be caused by a direct impact, or by acceleration alone," explains Dr. Mark L. Gordon, interventional endocrinologist and traumatic brain injury treatment specialist at Millennium Health Centers in Los Angeles. "Brain trauma also causes secondary injury, which takes place in the minutes and days following the injury," he adds. "These processes include alterations in cerebral blood flow and increased pressure within the skull, contributing substantially to damage from the initial injury." Gordon says traumatic brain injury can cause a host of physical, cognitive, emotional, and behavioral effects, some of which can be difficult to detect. Symptoms can appear immediately or weeks to years following the injury. "Insidious traumatic brain injury can be difficult to detect," Gordon says. "Localized damage to the frontal and occipital lobes occurs when the brain collides with the skull. Increasingly, we are discovering that traumatic brain injury is also a causative factor for accelerated hormonal deficiencies." These deficiencies, says Gordon, can cause a host of psychological, physiological, and physical manifestations, including depression, outbursts of anger, anxiety, mood swings, memory loss, inability to concentrate, learning disabilities, sleep deprivation, increased risk for heart attacks, strokes, high blood pressure, diabetes, loss of libido, menstrual irregularities, premature menopause, obesity, loss of lean body mass, muscular weakness, and a number of other medically documented conditions. What's more, Gordon points out that veterans suffering from these forms of psychological damage due to traumatic brain injury are frequently misdiagnosed and have their injury erroneously downgraded to post-traumatic stress disorder (PTSD). Moreover, especially in mild traumatic brain injury cases, symptoms at the initial time of injury may go unrecognized or unnoticed, but patients will still develop hormone deficiencies. Unfortunately, the government is slow to accept the link between traumatic brain injury and hormonal deficiencies. Dr. Gordon's Epiphany
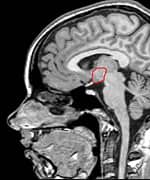
By sheer serendipity, many years ago Dr. Gordon provided care for a young man with a history of numerous sports-related head injuries, whose parents were themselves patients at the clinic. The young man's symptoms long outlasted the immediate effects of his acute injury and included loss of concentration, memory, mental energy, focus, and physical well-being, often accompanied by loss of lean muscle mass and an increase in body fat. The parents, familiar with the effects of hormonal imbalances, naturally assumed that their son's problems might reflect an endocrine problem of his own. And indeed, many of his symptoms resembled those of adult patients with so-called hypopituitarism, or loss of pituitary gland function. The pituitary gland is located at the base of the brain and is sometimes called the "master" gland of the endocrine system, because it controls the functions of the other hormone- secreting glands. Gordon, who is nothing if not intellectually curious, hit the books. What he found was startling and life-changing, for himself as a clinician, for his young patient, and now for scores of additional victims of traumatic brain injury. Symptoms of Traumatic Brain Injury Mimic Pituitary DysfunctionDr. Gordon found a wealth of published literature suggesting that traumatic brain injury causes pituitary dysfunction, confirming his initial hunch.1 Although the figures vary between studies, at least 50% (and up to 76%) of traumatic brain injury victims show some loss of pituitary hormone function immediately after the brain injury.2-4 In general, the more severe the original brain injury, the more profound the hormonal deficits, although hormone deficiency or insufficiency (levels in the low "normal" range) are seen even in patients with mild traumatic brain injury.5-9 And while about 58% of patients recover their normal pituitary function within one year of their head injury, a shocking 52% develop new pituitary hormone deficiencies after one year. 10,11 Those deficits include reductions in many different pituitary hormones, including those that regulate the thyroid gland, the adrenal glands (that produce cortisol, DHEA, and other vital hormones), the gonads (where estrogen and testosterone are produced), and growth hormone.3,4,12,13 The severity of the hormone deficiencies correlates strongly with the kinds of symptoms Dr. Gordon was seeing in his patient. For example, patients with growth hormone deficiency or insufficiency had significantly worse disability rating scores, greater rates of depression, worse quality of life, lower energy, greater fatigue, and poorer emotional well-being, compared to brain injury patients with normal hormonal levels.14,15 Dr. Gordon's hunch was borne out: patients with traumatic brain injury often have pituitary hormone deficiencies or insufficiencies, especially in growth hormone. And those defects are closely associated with the persistent neurological, psychological, and emotional deficits that are so tragically common in survivors of traumatic brain injury. And where are you most likely to find a high concentration of survivors of traumatic brain injury? The United States military.
The Combat Connection"When you have 360,000-plus GIs coming back from war with traumatic brain injury, it gets expensive," he says. "Especially when you have to start addressing hormone deficiencies." In 2006, the army's surgeon general established the Traumatic Brain Injury Task Force to establish a clear picture of the processes and research involved with helping traumatic brain injury–affected service members transition to civilian life. The task force was designed to assess how the army addressed aspects of traumatic brain injury care, and made recommendations for improvement. But Gordon believes the bottom line is that a task force can do little if the military doesn't want to pay for treatment. Gordon explains that conventional medical dosage for testosterone is at 200-300 milligrams per week, which he has shown is far too high! "For example, a typical 25-35 year old male naturally generates 4-10 milligrams per day, or 60 milligrams per week. Using supraphysiological dosages of testosterone (as military doctors are doing) can have significant side-effects if not monitored closely. We can achieve similar benefits at one-quarter the dose without the risk factors." While Gordon admits that interventional endocrinology may not be for everyone, patients like soldiers will eagerly seek it out when traditional doctors have hit a wall and are unable to fix ongoing issues. Recently, he spoke with a military veteran in North Carolina who described the sheer difficulty of getting anything done through the military. "Part of the reason," Gordon explains, "is because the military and doctors see testosterone as a ‘bodybuilder drug,' rather than a natural substance produced in our bodies. It makes no sense why they can readily accept insulin use for diabetes, but not testosterone. They are both natural hormones, flowing naturally through our bodies."
|
Growth Hormone: A Critical PlayerGrowth hormone is the most common hormone deficiency or insufficiency in patients with traumatic brain injury at any level of severity.16-19 Deficiencies in this hormone are especially marked in patients with moderate to severe traumatic brain injury.20 Brain-injured patients with growth hormone deficiency experience rapid weight gain and have substantially lower levels of other hormones as well.17,19 Low growth hormone levels are also associated with excessive anxiety and depression and poor physical health and quality of life.15,21 Finally, brain-injured patients with growth hormone deficiency show greater deficits in attention, executive functioning, memory, and emotion than those with normal growth hormone levels.22 Growth hormone is an intriguing hormone, and we are learning more about it each year. In children, it is responsible for regulating linear growth, ultimately determining adult height and body proportions. But growth hormone has many other remarkable functions throughout the body and into adulthood. It is neuroprotective, increasing survival of damaged nerve cells and promoting regeneration of nerve tissue.23-25 Growth hormone also increases the number of receptors for other hormones in tissues throughout the body; this has the effect of increasing the body's sensitivity to those hormones' actions, helping to overcome the effects of their deficiencies.26-29 Like all hormones, growth hormone acts by binding to specific cell-surface receptors. Receptors for growth hormone are found throughout the brain, and they are especially densely distributed in brain regions responsible for learning and memory.30,31 That may explain why declining growth hormone levels are associated with poorer cognitive function. Growth hormone levels fall with age and are especially low in Alzheimer's disease.32-36 As Dr. Gordon points out, it is therefore not surprising that traumatic brain injury patients often show symptoms identical to the cognitive decline and memory loss we see with aging and Alzheimer's disease. In essence, a brain-injured patient with low growth hormone levels undergoes accelerated cognitive aging. Hope for Traumatic Brain Injury Patients at Millennium Health Centers
Dr. Gordon was struck by the obvious paradox: although there is copious evidence that patients with traumatic brain injury suffer from hypothalamic-pituitary hormonal imbalances, and ample expert recommendations for rigorous hormone testing, few physicians were bothering to test their brain-injured patients.2230,37 Worse, despite compelling studies showing the benefits of hormone replacement, virtually no physician was offering such therapy in the United States. Dr. Gordon decided to act. Over the course of several years, he has developed a panel of comprehensive hormone testing for survivors of traumatic brain injury (Table 1). Gordon's clinic, Millennium Health Centers, provides primary, or direct, testing to determine how well the hypothalamic-pituitary system is functioning, and also secondary testing, which determines how the target endocrine glands themselves are affected (Table 2). In his practice, Dr. Gordon obtains a complete history and performs a detailed physical examination on each brain-injured patient and correlates those findings with their lab results. From this information he is able to create a treatment protocol for individualized hormone replacement. Dr. Gordon uses physiologic dosing, not megadoses, of each hormone. His goal is to restore hormone levels to the middle of the optimum range, but he works each patient up to that level slowly, monitoring their cognitive and physical functions monthly.
"Science now has the ability to map the entire brain, and we now know exactly where growth hormone works on mood, which pathways it uses," says Dr. Gordon. "The military is simply not prepared to go to the depths that we have in the private sector." Patients typically respond within weeks to the Millennium approach. And the responses tend to be dramatic. Gordon recalls one case in particular, of a woman who had been involved in a "T-bone" car crash - a notoriously deadly situation in which the victim's vehicle is hit full-force from the side. The patient was left with multiple neurological deficits. She spoke with a stutter and needed to keep one hand on the wall as she walked in order to maintain her balance. She had substantial memory impairment as well. After a series of blood tests, Dr. Gordon began administering small doses of the hormones that were deficient in this patient's case. She soon showed encouraging progress, with diminished speech and balance impairment. Gordon recalls with obvious delight, "One day about six months later, I got a phone call from a woman who said, in a perfectly normal voice, ‘Hi, this is your patient Nancy.' I told her to stop joking and asked who it was. ‘I'm your patient, Nancy, the one with the bad stutter. I woke up this morning, and this is how I was able to speak. I just wanted to let you know.'" Nancy's case, though dramatic, is far from unique. Since that time, Dr. Gordon has treated scores of other patients with similar outcomes, which is why military veterans coming to him are in good hands: he has obtained a grant from Access Medical Laboratories in Jupiter, Florida, which currently covers the cost of testing veterans with traumatic brain injury. "They've arranged for a phlebotomy company to go to the veterans' homes and draw blood. Lab tests use a spectrum that goes way beyond typical blood tests, providing a bigger database." Any treatment starts with baseline hormone testing of testosterone, growth hormone, thyroid, and cortisol.
His work is attracting international attention, and he has been invited to lecture on his hormone-balancing approach at prestigious conferences around the world. Dr. Gordon is actively recruiting other physicians to learn from him so that they can apply his techniques in their own practices. SummaryTraumatic brain injury leaves millions of survivors with substantial impairments in physical, emotional, cognitive, and behavioral consequences each year. Despite high-tech diagnostic and treatment protocols, mainstream medicine has managed to do little to overcome these long-term pathologies. The recent discovery that traumatic brain injury, by damaging the brain's hypothalamus, triggers dysfunction of the pituitary gland, led Dr. Mark Gordon on a mission to identify and treat the resulting hormonal deficiencies in his patients with traumatic brain injury. Restoring hormone levels to their optimal, pre-injury and youthful levels results in remarkable recovery of many of the impaired functions. Patients with traumatic brain injury, or their family members, may visit Millennium's website at www.TBImedlegal.com, or call 818-990-1166 in order to set up initial lab testing. Information at the website also lets patients know what a typical course of treatment involves. If you are a veteran of the Gulf War, Iraq, or Afghanistan, The Millennium Health Centers has a limited grant from Access Medical Laboratories of Florida that will pay for your TBI Hormone Panel. In California, Dr. Gordon offers the same TBI Hormone Panel to law enforcement officers injured on the job. We care for those who take care of us! If you have any questions on the scientific content of this article, please call a Life Extension® Wellness Specialist at 1-866-864-3027. Editor's NoteScience continues to evolve, and new research is published daily. As such, we have a more recent article on this topic: Neurosteroidal Treatment for Traumatic Brain Injury
|
|||||||||||||||||||||||||||||||||||||||||||
| References | |||||||||||||||||||||||||||||||||||||||||||
|
|||||||||||||||||||||||||||||||||||||||||||