Life Extension Magazine®

The federal government has a problem. It is obligated to pay the sick-care expenses of a surging population that is living years beyond original expectations.
The result of Americans surviving longer is that government medical insurance programs are descending into insolvency.
One way to reduce outlays is to deceive the public with misleading propaganda that urges citizens to neglect their health.
If this charade succeeds, tens of millions will die prematurely, thus sparing Medicare and other programs the expense of fulfilling their obligations to aging Americans. There’s no question about it, premature death is cost effective for the government.
Government has a big advantage. Their deceptive reports receive widespread media coverage, which leads most consumers to believe them.
Life Extension® is on the opposing side. We strive to keep our members alive far beyond any expectation. Our 33-year track record documents that we are decades ahead of government-sanctioned medicine, yet the media ignores our science-based positions.
As a reader of this publication, you get to learn what our government is seeking to censor.
In 1941, the Japanese bombed Pearl Harbor. The ensuing World War caused the deaths of over 405,000 Americans.1
A more significant event occurred in 1941 from a loss-of-life standpoint. That year, a study was published in the journal Cancer Research showing greater cancer mortality in people living at higher latitudes—where there is less sunlight exposure.2
Instead of acting to save lives, this finding was overlooked by government-sanctioned medicine until 2006, when the Journal of the National Cancer Institute published results from a huge population study showing lower cancer deaths in response to higher vitamin D blood levels.3 Compared to 25-hydroxyvitamin D blood levels of 20 (ng/mL), this study’s analysis indicated those with a reading of 50 (ng/mL) would have a 51% reduction in total incidences of cancer.3
The Journal of the National Cancer Institute study authors concluded that to increase 25-hydroxyvitamin D from a low of 20 to a higher 50 ng/mL—about 4,500 IU a day of vitamin D supplementation would be necessary.3
Move forward to year 2012 and another government-sponsored program (United States Preventive Services Task Force) issued a carefully crafted press release to imply there is no benefit to supplementing with vitamin D (or calcium). This led newspapers like the Washington Post to run the headline:
“Task Force Recommends Against Vitamin D, Calcium Supplements”4
These kinds of misleading headlines were repeated in the worldwide media.5-9
What the “Task Force” Really Stated

The United States Preventive Services Task Force evaluated 137 published studies about vitamin D and concluded what most Life Extension members already know, i.e. low-dose vitamin D (400 IU/day) has no benefit in preventing fractures or cancer.10
To reiterate this point, the Task Force reviewed the published data and came to the conclusion that women should not take low doses of vitamin D to prevent fracture or for any other benefit.
The Task Force is correct! This was documented by the 2006 study published in the Journal of the National Cancer Institute showing that it would require 4,500 IU a day of vitamin D to reduce incidences of cancer by 51%.3
The Task Force also stated that 1,000 mg a day of calcium (calcium carbonate) plus 400 IU of vitamin D does not prevent bone fractures. This was long ago known to nutritional experts who understand that osteoporosis prevention requires supplementation with nutrients such as vitamin K11-15 and magnesium,16-20 along with maintenance of a youthful hormone balance21-23 and resistance exercises.24-27
Omissions and Lies
Instead of recommending that effective doses (over 4,000 IU/day) of vitamin D be taken along with other critical nutrients and hormones, the United States Preventive Services Task Force concluded that people should not take any vitamin D or calcium.
The Task Force went further and noted a small risk in kidney stones in women taking calcium and vitamin D supplements. This contradicts other studies showing calcium supplements reduce kidney stone risk28-30 and that magnesium and potassium intake prevents kidney stone formation by 85%!31-33
The most outrageous lie was a Task Force statement that most people can achieve sufficient doses of vitamin D and calcium with a healthy diet. The truth is that the only way to achieve optimal vitamin D levels without supplements is significant sun exposure. There is no healthy diet that comes close to providing over 4,000 IU of vitamin D each day. This blatant lie deceives consumers into believing they will obtain enough vitamin D if they eat healthy.
This is one reason why we refer to the United States Preventive Services Task Force as a "Federal Death Panel." Their recommendation to not take any vitamin D, because low-dose vitamin D is ineffective, will condemn millions of Americans to needlessly die of cancer if the truth remains suppressed.
Clarifying “Low-Dose”
Some people find it difficult to understand why something as effective as vitamin D does not show some benefit even with low doses (compared to no dose).
The harsh reality is that to protect against cancer and other diseases, the body has to maintain a minimum blood level of around 50 (ng/mL) of 25-hydroxyvitamin D.34 Blood levels below 50 ng/mL mean different cells are viciously competing for an insufficientamount of vitamin D.35 In this lethal scenario, many cells are inevitably deprived of enough vitamin D to maintain healthy division patterns.36
According to the 2006 mega-study published in the Journal of the National Cancer Institute, if one were to ingest 400 IU of vitamin D a day, the increase in 25-hydroxyvitamin D blood levels would be a tiny 2.6 ng/mL.3 This is in keeping with an early report showing for each 1,000 IU of vitamin D3 that is supplemented, 25-hydroxyvitamin D blood levels will increase by 7 ng/mL.37
A typical aging person who does not take vitamins will have 25-hydroxyvitamin D levels around 20 (ng/mL). So boosting it to 22.6 ng/mL by taking a 400 IU vitamin D supplement does not come close to achieving conventional medicine’s minimum blood level of 32 ng/mL, let alone optimal ranges of over 50 ng/mL.
If one supplements with 5,000 IU of vitamin D each day, they can increase 25-hydroxyvitamin D from 20 to around 55 ng/mL, which is the protective blood level enjoyed by youngsters playing each day in the summer sun. (Children should not play in the sun without sunscreen.)
It is important to note that there is a huge individual variation in one’s response to vitamin D dosing, meaning some people only need around 3,000 IU/day while others need over 10,000 IU/day to achieve optimal status. That is why Life Extension added the 25-hydroxyvitamin D test to its Male and Female Blood Panels last year. I have learned through personal communication from Stephen B. Strum, MD, FACP, that the average vitamin D3 dose needed by adult men in a prostate cancer practice to achieve a 25-hydroxyvitamin D level of 60 ng/mL is 8,000 IU/day.
To use an analogy as to why low-dose vitamin D is worthless (which is what the Task Force was really saying), pretend you wake New Year’s Day with a splitting headache from excess drinking the night before. If you take 400 mg of ibuprofen, your headache may disappear. If you only take 40 mg of ibuprofen, you are unlikely to feel any relief. If a clinical study is done using 40 mg of ibuprofen to relieve headaches, the results will show there is no difference between placebo and 40 mg of ibuprofen. That does not mean ibuprofen is ineffective, it just means that ten times more is needed. In medicine, this is called a dose-response relationship, and it applies to virtually every nutrient, hormone, and prescription drug.
The United States Preventive Services Task Force cited data from studies showing doses as low as 400 IU/day of vitamin D do not prevent bone fracture or cancer as a basis to advise aging Americans to not take any vitamin D (or calcium). This is clearly an absurd recommendation since hard-core scientific data show ten times more vitamin D (over 4,000 IU/day) is required to provide expected benefits.38-41
Cancer Risk Reduction in Response to Higher Vitamin D Status
| CANCER PRIMARY SITE | RISK REDUCTION WITH INCREASED VITAMIN D LEVELS |
| Breast43 | 50% |
| Colon44,45 | 50% |
| Prostate46,47 | 49% |
| Ovary48 | 36% |
Vitamin D Levels in Supplement Users
Life Extension was the first to discover that most supplement users have insufficient vitamin D levels unless they take around 5,000 IU of vitamin D each day. Insufficient is defined as blood levels of 25-hydroxyvitamin D under 50 ng/mL.
In 2009, Life Extension conducted the largest survey of supplement users in history and found 85% had insufficient vitamin D blood levels based on 25-hydroxyvitamin D readings of 50 ng/mL or less.42 These findings motivated health conscious consumers to increase their intake of this inexpensive nutrient.
The result is that most enlightened supplement users now have optimal vitamin D blood status, based on Life Extension’s ongoing review of the thousands of 25-hydroxyvitamin D blood tests our members take.
When we see a 25-hydroxyvitamin D reading over 100 ng/mL (which is rare), we contact the member and advise they reduce their vitamin D intake.
Ideal 25-hydroxyvitamin D ranges are probably between 50-80 ng/mL. Yet based on the deceptive Task Force recommendations, average consumers have been misled into thinking they should take no vitamin D or calcium.
To reiterate, both sides agree there is no proven efficacy with low-dose vitamin D. By deceiving the public into thinking they should not take any vitamin D, the United States Preventive Services Task Force is functioning as a Federal Death Panel.
Watch Prostate Cancer Death Rates Soar
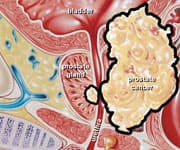
Life Extension is on the front lines helping people afflicted with metastatic cancer to find therapies overlooked by their oncologist. In too many cases, advanced-stage cancers fail to respond to treatment, or a tumor that goes into remission rapidly recurs. If these metastatic cancers were detected earlier, the probability of cure would have been significantly greater.
The most common cancer striking men has a blood marker that can enable very early detection, thereby enabling curative therapies to be employed before metastasis strikes. The name of this blood marker is PSA (prostate-specific antigen) and it has spared tens of thousands of men, from young men in their forties to those sixty and beyond, agonizing deaths from metastatic prostate cancer.
The problem is that most urologists and oncologists are not properly interpreting PSA results, nor are they efficiently implementing further diagnostic and treatment protocols. The unfortunate outcome is that too many aging men are being subjected to needless and incompetently administered procedures that sometimes result in unnecessary suffering and premature death.
Instead of recommending that medical professionals upgrade their protocols to deliver state-of-the-art technology, the United States Preventive Services Task Force suggests that aging men not undergo PSA screening—at all!49
The media ran this Federal Death Panel recommendation as headline news. The result is that prostate cancer will once again be diagnosed at an advanced stage, when there is bulky disease and a small chance of curative therapy. Men will see their physicians as they did in the pre-PSA era, prior to 1987, with presenting clinical findings such as:
A. Inability to urinate due to prostate cancer obstructing the urethra as it passes through the prostate gland.
B. Pain in the bones or fracture of bones such as the femur or humerus or vertebral bodies of the spine due to bone metastases from prostate cancer.
C. Spinal cord compression due to encroachment by prostate cancer that traveled to bone or lymph node and then invaded and compressed the spinal cord.
D. Nerve root pain if prostate cancer compresses a major nerve as it leaves the spinal cord.
E. Symptoms of uremia (a toxic condition involving accumulation of metabolic waste products in the blood stream) due to lymph node compression of the ureters caused by prostate cancer that has spread to the lymphatics. (Ureters are tubes that drain urine from kidneys to the bladder.)
What Can Happen When PSA Screening is Not Performed
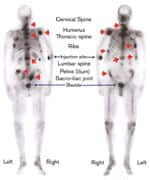
This is a radioisotope bone scan of a man presenting with advanced prostate cancer showing metastatic lesions that have invaded bone. Black areas represent uptake of a radioisotope tracer at sites of bone metastases. These metastases involve the spine, ribs, pelvis, and right shoulder. Metastatic lesions at these sites can result in increased fracture risk and spinal cord compression among other problems.
Source: A Primer on Prostate Cancer: The Empowered Patient’s Guide by Stephen B. Strum, MD, FACP, and Donna Pogliano.
Doctors Don’t Know That Cancer Cells Use PSA
PSA is not just a marker of prostate disease. It functions as an enzyme to break down natural barriers that surround cells. Cancer cells spew out PSA that digests the protective extracellular matrix (tissues surrounding cells). PSA thus contributes to the ability of cancer cells to escape the prostate and metastasize to distant sites within the body.
By lowering PSA levels, men can diminish the ability of cancer cells in their prostate gland to break down the healthy tissues that help contain them.
Our understanding that cancer cells utilize PSA’s enzymatic protease digestion to escape confinement provides persuasive evidence for keeping PSA levels low to prevent frank prostate cancer from developing, or markedly slow it down.
Hidden Dangers of PSA
PSA may contribute to prostate cancer progression and the ability of these cancer cells to escape the prostate and metastasize to distant sites within the body. We can no longer think of PSA as merely a blood marker reflecting prostate health.
In fact, many, if not all, of the biomarkers (like PSA) used in tracking a wide array of cancers may have specific cancer-facilitating functions. Therefore, in men with prostate cancer, and perhaps even in those trying to prevent the emergence of prostate cancer, taking steps to keep PSA levels low may reduce one’s risk of developing this illness or having it progress to a clinically symptomatic condition.
The easiest way to reduce PSA is to inhibit the enzyme 5-alpha reductase, which transforms testosterone into the more androgenic dihydrotestosterone (DHT). DHT has a growth-promoting effect on prostate cells that is 2.4 to 10 times greater than that of testosterone.58,59
In a study of 4,325 men with benign prostate enlargement who were randomly selected to receive either Avodart® (0.5 mg/day) or placebo, those receiving Avodart® had a cumulative incidence of prostate cancer of 1.2% compared to 2.5% for the placebo group at 27 months of follow-up. This equates with a 52% reduction in prostate cancer in the Avodart® group.60
In another study using finasteride (Proscar®), 18,882 men aged 55 or older (with normal digital rectal examination results and a PSA level of 3.0 ng/mL or lower) were randomly assigned treatment with Proscar® (5 mg/day) or placebo for seven years. Prostate cancer was detected in 803 of the 4,368 men in the Proscar® group and 1,147 of the 4,692 men in the placebo group, for a 24.8% reduction in prevalence over seven years. High-grade cancers were noted in 6.4% of Proscar®-treated patients compared to 5.1% of men receiving placebo.61 (Proscar® suppresses only type two 5-alpha reductase, whereas Avodart® blocks both type one and type two 5-alpha reductase. Avodart® thus appears to be the better drug.)
Aging men should consider having their blood tested for DHT. If DHT levels are elevated, Avodart® drug therapy appears to be safe and effective not only for improving urinary flow symptoms, but more importantly, for potentially reducing prostate cancer risk. Avodart® appears to accomplish these effects by reducing the growth-promoting effects of DHT on prostatic tissue, while decreasing the cancer-inducing properties of PSA by reducing PSA synthesis in the prostate gland.
Avodart® does have several downsides. At more than $4 per capsule, it is expensive. Moreover, a small percentage of men who use it have sexual dysfunction problems such as decreased libido (3%), impotence (5%), and ejaculation disorders (1%). The frequency of these side effects reportedly decline after six months of continued use of Avodart®.62 Fortunately, Avodart® is approved by the FDA to treat urinary symptoms related to benign prostate enlargement, so it is covered by most insurance plans.
Easy Ways to Reduce PSA
We all know that if artery-clogging LDL is elevated, it can be reduced by lifestyle changes, nutrients, and drugs. Overlooked is the fact that elevated PSA can also be reduced in many men.
What this means is that PSA testing can enable men to identify prostate disease at an early stage when it might be reversible.
While conventional reference ranges state that PSA levels under 4.0 ng/mL are normal, we at Life Extension view any reading over 1.0 ng/mL with suspicion. We know that PSA readings over 1.0 ng/mL can indicate unhealthy activity, such as prostatitis, benign prostate hypertrophy, or prostate cancer.50,51
Rather than watching PSA readings gradually elevate, there are interventions that reduce and/or stabilize the production of PSA, and thus shut down a mechanism used by cancer cells to escape confinement within the prostate gland.
Life Extension suggests that men with PSA readings over 1.0 ng/mL initiate steps to reduce levels of this tissue-destroying enzyme. Dietary changes and nutritional supplements may be tried first, but drugs like dutasteride (Avodart®) are recommended to quickly reduce PSA, shrink prostate gland size (to reduce urinary difficulties), and to reduce prostate cancer risk.52
Avodart® can slash PSA readings by nearly 60%.53 Critics of Avodart® mistakenly view this as bad because they think it may mask underlying prostate cancer. If properly used, Avodart®, along with dietary changes and nutrient supplements can markedly reduce the chances that isolated malignant cells in the prostate gland will mature into full-blown prostate cancer.
Proper use of Avodart® should also include testing free testosterone blood levels to ensure an aging man is not suffering a testosterone deficiency. When an aging man deficient in testosterone takes a drug like Avodart® that reduces dihydrotestosterone, the result can be increased risk of heart failure.54 The solution is to restore natural testosterone levels to a youthful range for systemic benefits and then initiate Avodart® (0.5 mg daily) to protect against benign prostate enlargement and prostate cancer.
We at Life Extension are well aware that it is quite normal for men over age 50 to have PSA readings between 1.1 and 2.4. It is also “normal” for men over age 50 to get up frequently at night to urinate and for these same men to develop some stage of prostate cancer.
Our argument is that when a blood test shows a PSA reading over 1.0, this should be greeted as a friendly warning to initiate definitive steps to reduce it. In the process of reducing PSA by making healthier lifestyle choices and achieving youthful hormone balance, men should see a reduction in nighttime urinary frequency, along with reduction in risk for virtually all degenerative disease. That’s quite a benefit in return for taking steps to reduce just one blood marker, i.e. PSA!
Analogies to Testing Cardiac Risk Factors
The medical establishment supports blood testing to identify risk factors that predispose people to vascular disease. When blood test results show elevated LDL, triglycerides, or glucose, steps are taken to lower these artery-blocking factors and thus slash coronary artery disease risk.
The same can be done when a blood test reveals PSA over 1.0 ng/mL. Interventions can be readily employed to lower PSA and thus reduce prostate disease risk.
Just imagine that a blood test reveals your triglycerides or glucose are high. Instead of lowering these risk factors, what if doctors instead performed invasive diagnostic techniques and even needless surgeries—as is done far too often today in response to an elevated PSA reading. If this type of medical mismanagement were done in the cardiovascular arena, the United States Preventive Services Task Force would likely recommend against glucose and triglyceride blood testing since too many false positives were occurring, resulting in expensive and side effect-prone procedures. What few doctors know today is that a rising PSA can sometimes be reversed without causing serious side effects. Since the United States Preventive Services Task Force had no idea that PSA itself contributes to carcinogenesis and that PSA is often controllable, they issued a blanket warning that all healthy men should avoid PSA screening. The lunacy of this archaic view is further exposed when one realizes how many different ways PSA levels can be controlled.
Staggering Statistics on Prostate Cancer
Prostate cells are very prone to gene mutation.55 Autopsy evidence indicates that prostate cancer is histologically evident in up to 34% of men aged 40-49 and up to 80% of men aged 80 and older.56,57 Most men, however, never progress to clinically diagnosed disease, indicating the presence of control mechanisms that keep prostate cancer cell colonies small and thus controlled.
There is an increasing understanding of mechanisms involving gene regulation processes that enable cells to divide out of control and eventually form a prostate tumor. These new findings make it more important than ever for men to monitor their PSA blood levels to detect prostate cancer at its earliest stages.
Boron Reduces PSA…Protects against Prostate Cancer
PSA and IGF-1 function as active growth factors in the prostate gland.63-66
In mice, boron protects against the ability of PSA to degrade extracellular matrix and reduces expression of IGF-1 in prostate tumors.67
One animal study showed that in response to both low- and high-dose boron supplements, PSA levels plummeted 87% on average, while tumor size declined 31.5% on average.67 Another study showed that boron inhibited proliferation of androgen-dependent and androgen-independent prostate cancer cell lines in a dose-dependent manner.68
A report from UCLA showed that men with the highest dietary boron intake reduced their prostate cancer risk by 54% compared to men with the lowest boron intake!69 While the authors noted that the observed association should be interpreted with caution because of the small case sample size and the nature of the cross-sectional study design, clearly these findings deserve further investigation.
If laboratory studies can be replicated in human patients, boron at doses ranging from 6 to 15 mg a day may become an effective and low-cost adjuvant therapy. Most Life Extension members already take 3-9 mg of boron contained in various multi-nutrient formulas.
Green Tea May Block PSA’s Detrimental Effects

The MEDIOCRE doctor attends to impending sickness;
The INFERIOR doctor treats actual sickness.
--Chinese Proverb
There may be another way to protect the prostate gland against its own PSA. Since consuming green tea has been reported to lower the risk of prostate cancer, scientists investigated the effects of the green tea flavonoid epigallocatechin gallate (EGCG) on the expression and activity of PSA by prostate cancer cells.
EGCG was shown to restrain PSA expression. In addition, EGCG inhibited tumor-promoting activities such as degradation of type IV collagen. EGCG’s beneficial effects were at blood levels close to those measured in serum following ingestion of green tea.70 The study authors proposed that green tea extract may be a natural inhibitor of prostate carcinoma aggressiveness.
Newer studies are uncovering additional mechanisms by which green tea protects against prostate cancer.71-73 Spurred by these anti-cancer effects, doctors at Louisiana State University gave prostate cancer patients 1,300 mg of green tea extracts (mostly EGCG) prior to the time of radical prostectomy. Their findings showed significant reductions in PSA and other tumor promoters such as vascular endothelial growth factor. These findings led the doctors to conclude that there is a potential role for green tea extracts in the treatment and prevention of prostate cancer.74
The PSA Controversy
In May 2012 the United States Preventive Services Task Force (USPSTF) proclaimed that regular PSA testing should not be used as a screening tool for prostate cancer based upon their analysis.49
There were several problems with the USPSTF analysis. The report de-emphasized a major, high quality trial that showed robust mortality benefits by including in their analysis trials of poor/ lesser quality that did not show mortality benefits. This statistical manipulation diluted the over-all statistical effect of the higher quality trial on mortality (benefit) in their analysis.
This high quality trial was the European Randomized Study of Screening for Prostate Cancer (ERSPC), which randomized 182, 000 men aged 50 to 74 from 7 countries to PSA testing every 2 to 7 years (depending on center and year) or to usual care. An analysis of 162, 243 men aged 55 to 69 found that screening was associated with a 20% reduction in prostate cancer-specific mortality.103
After publication of the main ERSPC results, a participating center (Göteborg, Sweden) reported their results separately. This site determined that a PSA screening threshold of 2.5 to 3.0 ng/mL every 2 years in 20 ,000 men aged 50 to 64 years decreased risk for prostate cancer-specific mortality by 44% after a median of 14 years.104 This finding helps corroborate Life Extension’s long standing position that a PSA reading over 2.4 ng/mL should be viewed with suspicion, as opposed to standard reference ranges that state that PSA reading up to 4.0 ng/mL is normal.
Poor-quality trials included by the USPSTF in their analysis statistically diluted the beneficial effect observed in the higher quality ERSPC trial in their over-all assessment. Several lesser/poor quality trials found no difference between screening-invited and control groups in prostate cancer-specific mortality risk.105,106 Major methodological flaws in these trials included failure to adequately control for randomization and/or poor allocation blinding, poor attempts to capture lost data points, etc. One trial used by the USPSTF even used an exorbitantly high PSA cut point – 10 ng/mL, as a screening threshold.105
By including trials that erroneously classified high PSA readings (ranging from 2.5 to 10 ng/mL) as not being suspicious, is it any wonder that the USPSTF report concluded that PSA testing does not protect men against death from cancer? Said differently, some of the data reviewed by the USPSTF did not recognize that PSA readings over 2.4 ng/mL were indicative of possible prostate malignancy. The inevitable results were that men who could have received early treatment did not because their physicians failed to screen for prostate cancer even when PSA readings ranged from 2.5 to as high as 10 ng/mL.
Life Extension advocates the use of PSA screening to prevent prostate cancer deaths, with an important caveat– PSA results should be tracked and monitored over time (i.e., PSA velocity) with less emphasis being placed on individual test results.
Life Extension has examined this issue in detail. For more information please see the Life Extension magazine multi-part series entitled "The PSA Controversy" that appeared in the December 2012 issue.
Treating Advanced Prostate Cancer with Lycopene
In a study of twenty patients with metastatic hormone-refractory prostate cancer, each patient received 10 mg a day of lycopene for three months. No other treatment was given. One patient achieved a complete response, defined as a reduction of PSA (to under 4 ng/mL) and the absence of any sign of the disease for eight weeks. Six patients (30%) had a partial response, defined as a 50% reduction in PSA and alleviation of other symptoms such as bone pain if present. The disease remained stable in 10 patients (50%) and progressed in three (15%). A remarkable 63% (10 of 16) with bone pain were able to reduce their daily use of pain-suppressing drugs. The study concluded:
“Lycopene therapy appears to be effective and safe in the treatment of hormone-refractory prostate cancer.”75
In another study, 54 metastatic prostate cancer patients were castrated and half of them were given 2 mg of lycopene twice daily. Castration (removal of the testes) reduces testosterone levels and is a treatment for those with androgen-dependent prostate cancer. After six months, PSA declined significantly in both groups, but more so in the group receiving lycopene. After two years, 40% of the castrated group reduced their PSA level to less than 4 ng/mL, compared to 78% in the lycopene group. Bone scans showed that twice as many patients in the lycopene-plus-castration group attained a complete response compared to the castration-only men.
The author concluded:
“Adding lycopene to orchidectomy (castration) produced a more reliable and consistent decrease in serum PSA level; it not only shrinks the primary tumor but also diminishes the secondary tumors, providing better relief from bone pain and lower urinary tract symptoms, and improving survival compared with orchidectomy alone.”76
What is impressive about these two studies is that only small doses of lycopene (4-10 mg/day) were used. That low doses of lycopene produced such favorable results in these late-stage prostate cancer patients is quite remarkable and worthy of further study.
The Optimal PSA Range Controversy
Many men have noticed that there are several “optimal” ranges for PSA, making it confusing for those who are trying to maintain superior prostate health.
Most mainstream labs (e.g. LabCorp & Quest) currently use a reference range of 4.0 ng/mL or less on PSA blood test results and most doctors don’t get too concerned until the PSA is above that level. 107,108
Studies done on healthy young men with normal prostate glands, as assessed by clinical exam of the prostate, report a range of 0-2.6 ng/mL as normal.50 Some doctors use a more stringent range of 2.5 to 3.0 ng/mL or less as an optimal PSA range.51
Other doctors prefer to use age adjusted ranges that increase as a man ages. Typically in this scenario a man younger than 50 should have a PSA 2.5 ng/mL or less while a PSA up to even 6.5 ng/mL is considered normal for a man in his seventies. Another take on this age adjusted approach is looking at cutoff levels where the sensitivity and specificity of the PSA test is maximized for different age groups.
Doctors using this approach may use a PSA range of 2.0 ng/mL or less for men less than 50 years old, 3.0 ng/mL or less for those aged 50-59, 4.0 ng/mL or less for ages 60-69, and 7.0 ng/mL or less for men over age 70.109
Life Extension suggests that the most stringent approach is to consider a PSA above 1.0 ng/mL as the earliest possible warning sign that changes may be occurring and those interested in superior prostate health should engage in methods to reduce it. This is not to say someone with a PSA of 2.0 ng/mL has prostate cancer, prostatitis, or BPH. It may indicate a normal prostate or it could be the earliest warning sign of small cellular changes occurring in the prostate.
It is also important to note that PSA readings should be confirmed with repeat testing and one of the most important aspects of PSA testing is getting a baseline value and looking for changes over time. Doctors especially look at the doubling time for PSA as well as the PSA velocity combined with symptoms and results of the prostate exam to further assess prostate health.110
Federal Death Panel Advises All Men to Avoid PSA Testing
PSA testing alerts aging men that they have a prostate problem. A wide range of safe approaches can be utilized to attempt to bring PSA to optimal ranges of under 1.1.
By recommending that aging men avoid PSA testing, the United States Preventive Services Task Force is condemning a huge segment of the aging population to develop painful metastatic prostate cancer that is considered virtually incurable.
Equally important, and perhaps more important, the Task Force recommendations would exclude the use of PSA testing as a key biologic marker for prostate health. PSA values above the threshold of 1.0 ng/mL inform the medical team of disease processes affecting the prostate that may involve prostatic hyperplasia (BPH), prostatitis and/or prostate cancer. Such processes can be evaluated with various medical testing and changes in the patient’s environment (external and internal) can alter the course of these diseases and change the entire course of health of that individual. This is medicine at its best—it is preventative medicine, and it is far more compassionate than treating advanced diseases that remain subclinical for many years prior to overt manifestation.
My Personal Triumph Using PSA Testing
I was traveling to meet a new oncology group near the end of April 2003 when I called Life Extension’s Blood Lab to see if my most recent test results were ready. I asked Life Extension to fax these results to my hotel. What came out of that fax machine was beyond shocking. My PSA had shot up to 1.4 ng/mL—it had always been below 1.0 ng/mL. (See copy of lab reports above and below.)
My reaction was a controlled panic. As far as I was concerned, there were early-stage tumor cells lurking in my prostate gland that had to be eradicated. I’d seen too many cases where PSA jumps to 1.4 ng/mL and quickly moves up to the danger ranges (above 2.4 ng/mL).
All plans were cancelled that night as I searched computer databases to identify every single nutrient and lifestyle change that had ever been shown to reduce PSA levels. I noted each nutrient, extrapolated a human equivalent dose, and then took a quadruple-amount of almost every anti-cancer ingredient. Just some of the quadruple-dose nutrients I took included:
- Milk thistle extract77-79
- Green tea extract (decaffeinated)80-85
- Curcumin86,87
- Vitamin D88-91
- Cruciferous vegetable extracts (like I3C)92-94
- Gamma tocopherol95-98
- Genistein (soy) extract99,100
I made sure to take the prescription drug metformin101,102 on a consistent basis, slashed my consumption of red meat, and vowed to stay on this ultra-high dose regimen until there was a reversal of my PSA. As members have seen from the blood tests I have previously posted, my PSA has been around 0.5 ng/mL for the past several years---a more than 60% reduction compared to nine years ago (when I was younger).
I am convinced that had I not had regular PSA blood tests and used the findings to radically alter my dietary choices and nutrient-drug intake that I would be dealing with serious prostate issues now that I have turned age 58. In fact, at my age, prostate problems are normal.
In the December 2012 issue of Life Extension Magazine®, there was an article about a prostate cancer patient who used even more aggressive strategies to reverse his PSA and keep his cancer stable without resorting to toxic radiation or mutilating surgeries. If this patient had not discovered he had a prostate problem early on (via PSA testing) and treated it aggressively with non-toxic therapies, he might not be alive today.
As you can see from my most recent blood test, my PSA dropped to 0.4 ng/mL in 2013 from 1.4 ng/mL in 2003. If I had not checked my PSA regularly, I might very well have prostate cancer now. It does run in my family.
Government Wants You to Die Sooner!
The demarcation line between the pro-longevity principles of Life Extension and the pro-death edicts of the federal government grow wider each year. As a Life Extension member, you not only gain access to novel ways of living longer, but you learn the “other side” of the story about proven disease-reduction methods that our government is trying to censor.
Your support has enabled us to expand our four-decade campaign against the blatantly unscientific propaganda spewed by government-sponsored “task forces” that recommend against vitamin D supplements and PSA screening.
Deaths from prostate cancer have been in decline as more men find out they have prostate cancer and cure it before it spreads outside the prostate gland. We refer to the United States Preventive Services Task Force as a Federal Death Panel because their recommendation to avoid PSA testing will cause the needless deaths of tens of thousands of men—young men, middle aged, and older.
To make matters worse, this same Federal Death Panel proclaims that since low-dose vitamin D confers zero benefits, no one should take any vitamin D. Since higher-dose vitamin D may slash cancer incidences by over 50%,3 these misguided policy statements will create an epidemic of cancer in aging humans if the truth is suppressed.
Based on an overwhelming volume of peer-reviewed published science, virtually every American should be taking around 5,000 IU each day of vitamin D. Men over age 40 should have their PSA checked annually.
Annual Blood Test Super Sale
In 1996, we initiated a low-cost service whereby members could request their own blood tests.
Once a year, the price of the comprehensive Male or Female Blood Test Panel is sharply discounted so that members can ascertain their disease risk status and initiate preemptive measures before acute illness strikes.
The Male and Female Panels include the 25-hydroxyvitamin D test to ensure the proper dose of vitamin D is being taken to achieve optimal levels. The Male Panel includes the PSA test to assess the health of the prostate gland.
This year we are able to add the hemoglobin A1C test to the Male and Female Panels at no extra charge. Hemoglobin A1C is a measure of long term glucose control. It is more accurate than fasting glucose alone in detecting diabetic and pre-diabetic problems.
The retail price for the many individual tests included Male or Female Blood Test Panels can be astoundingly high, but Life Extension members obtain them for only $199 during the annual Blood Test Super Sale.
Upon receiving your order, we send your requisition out immediately. You can walk in for your blood draw at a time during normal business hours that is convenient to you. The next page describes the many unique tests that are included in Life Extension’s Male or Female Blood Test Panels.
To order the Male or Female Blood Test Panel at these once-a-year discounted prices, call 1-800-208-3444 (24 hours/day).
For longer life,
William Faloon
Male and Female Blood Test Panels
Unlike commercial blood tests that evaluate only a few disease risk factors, Life Extension’s Male and Female Blood Test. Panels measure a wide range of blood markers that predispose people to common age-related disorders. This year we are able to add the hemoglobin A1c test to the Male and Female Panels at no additional cost. Hemoglobin A1c is a measurement of long-term glucose control. Just look at the huge number of parameters included in the Male and Female Blood Test Panels:
| MALE PANEL | FEMALE PANEL |
Lipid ProfileTotal Cholesterol Cardiac MarkersC-Reactive Protein (high sensitivity) HormonesFree and Total Testosterone Metabolic ProfileGlucose Complete Blood Count (CBC)Red Blood Cell count including: hemoglobin, hematocrit, MCV, MCH, MCHC, RDW Cancer MarkerPSA (Prostate Specific Antigen) |
Lipid ProfileTotal Cholesterol Cardiac MarkersC-Reactive Protein (high sensitivity) HormonesProgesterone Metabolic ProfileGlucose Complete Blood Count (CBC)Red Blood Cell count including: hemoglobin, hematocrit, MCV, MCH, MCHC, RDW
|
Non-member retail price: $481 • Special Member Discount Price: $199. Blood Test Super Sale — April 1 through June 3, 2013.
To obtain these comprehensive Male or Female Panels at these low prices, call 1-800-208-3444 to order your requisition forms.
Then—at your convenience—you can visit one of the blood-drawing facilities provided by LabCorp in your area.
(Restrictions apply in NY, NJ, RI, MA, MD)
References
- Available at: http://www.abmc.gov/search/wwii.php. Accessed February 1, 2013.
- Available at: http://cancerres.aacrjournals.org/content/1/3/191.full.pdf+html. Accessed January 9, 2013.
- Giovannucci E, Liu Y, Rimm EB, et al. Prospective study of predictors of vitamin D status and cancer incidence and mortality in men. J Natl Cancer Inst. 2006 Apr 5;98(7):451-9.
- Available at: http://www.washingtonpost.com/blogs/the-checkup/post/uspstf-recommends-against-vitamin-d-calcium-supplements/2012/06/13/gjqatlngbv_blog.html. Accessed January 11, 2013.
- Available at: http://www.nytimes.com/2012/06/13/health/calcium-and-vitamin-d-ineffective-for-fractures-us-preventive-services-task-force-says.html. Accessed January 11, 2013.
- Available at: http://www.reuters.com/article/2012/06/12/us-vitamind-breaks-idusbre85b12220120612. Accessed January 11, 2013.
- Available at: http://www.cbsnews.com/8301-504763_162-57451854-10391704/panel-postmenopausal-women-shouldnt-take-vitamin-d-calcium-supplements-to-prevent-fractures. Accessed January 11, 2013.
- Available at: http://www.usatoday.com/news/health/story/2012-06-07/panel-vitamin-d-recommendations/55549414/1. Accessed January 11, 2013.
- Available at: http://www.npr.org/blogs/health/2012/06/12/154840966/panel-questions-benefits-of-vitamin-d-supplements. Accessed January 11, 2013.
- Available at: http://www.uspreventiveservicestaskforce.org/uspstf12/vitamind/vitdart.htm. Accessed February 4, 2013.
- Plaza SM, Lamson DW. Vitamin K2 in bone metabolism and osteoporosis. Altern Med Rev. 2005 Mar;10(1):24-35.
- Booth SL, Broe KE, Gagnon DR, et al. Vitamin K intake and bone mineral density in women and men. Am J Clin Nutr. 2003 Feb;77(2):512-6.
- Iwamoto J, Takeda T, Sato Y. Menatetrenone (vitamin K2) and bone quality in the treatment of postmenopausal osteoporosis. Nutr Rev. 2006 Dec;64(12):509-17.
- Shiraki M, Shiraki Y, Aoki C, Miura M. Vitamin K2 (menatetrenone) effectively prevents fractures and sustains lumbar bone mineral density in osteoporosis. J Bone Miner Res. 2000 Mar;15(3):515-21.
- Yamaguchi M, Weitzmann MN. Vitamin K2 stimulates osteoblastogenesis and suppresses osteoclastogenesis by suppressing NF-kappaB activation. Int J Mol Med. 2011 Jan;27(1):3-14.
- Ishimi Y. Nutrition and bone health. Magnesium and bone. Clin Calcium. 2010 May;20(5):762-7.
- Matsuzaki H. Prevention of osteoporosis by foods and dietary supplements. Magnesium and bone metabolism. Clin Calcium. 2006 Oct;16(10):1655-60.
- Ryder KM, Shorr RI, Bush AJ, et al. Magnesium intake from food and supplements is associated with bone mineral density in healthy older white subjects. J Am Geriatr Soc. 2005 Nov;53(11):1875-80.
- Tucker KL, Hannan MT, Chen H, Cupples LA, Wilson PW, Kiel DP. Potassium, magnesium, and fruit and vegetable intakes are associated with greater bone mineral density in elderly men and women. Am J Clin Nutr. 1999 Apr;69(4):727-36.
- Aydin H, Deyneli O, Yavuz D, et al. Short-term oral magnesium supplementation suppresses bone turnover in postmenopausal osteoporotic women. Biol Trace Elem Res. 2010 Feb;133(2):136-43.
- Gennari L, Merlotti D, Martini G,et al. Longitudinal association between sex hormone levels, bone loss, and bone turnover in elderly men. J Ciin Endocrinol Metab. 2003 Nov;88(11):5327-33.
- Duan Y, Seeman E. Bone fragility in Asian and Caucasian men. Ann Acad Med Singapore. 2002 Jan;31(1):54-66.
- Clarke BL, Khosla S. Female reproductive system and bone. Arch Biochem Biophys. 2010 Nov 1;503(1):118-28.
- Borer KT. Physical activity in the prevention and amelioration of osteoporosis in women : interaction of mechanical, hormonal and dietary factors. Sports Med. 2005;35(9):779-830.
- Guadalupe-Grau A, Fuentes T, Guerra B, Calbet JA. Exercise and bone mass in adults. Sports Med. 2009;39(6):439-68.
- Marcus R. Role of exercise in preventing and treating osteoporosis. Rheum Dis Clin North Am. 2001 Feb;27(1):131-41, vi.
- Available at: http://www.nof.org/articles/238. Accessed January 11, 2013.
- Williams CP, Child DF, Hudson PR, et al. Why oral calcium supplements may reduce renal stone disease: report of a clinical pilot study. J Clin Pathol. 2001 Jan;54(1):54-62.
- Heaney RP. Calcium supplementation and incident kidney stone risk: a systematic review. J Am Coll Nutr. 2008 Oct;27(5):519-27.
- Candelas G, Martinez-Lopez JA, Rosario MP, Carmona L, Loza E. Calcium supplementation and kidney stone risk in osteoporosis: a systematic literature review. Clin Exp Rheumatol 2012 Nov-Dec;30(6):954-61.
- Ettinger B, Pak CY, Citron JT, Thomas C, Adams-Huet B, Vangessel A. Potassium-magnesium citrate is an effective prophylaxis against recurrent calcium oxalate nephrolithiasis. J Urol. 1997 Dec;158(6):2069-73.
- Jaipakdee S, Prasongwatana V, Premgamone A, et al. The effects of potassium and magnesium supplementations on urinary risk factors of renal stone patients. J Med Assoc Thai. 2004 Mar;87(3):255-63.
- Taylor EN, Fung TT, Curhan GC. DASH-style diet associates with reduced risk for kidney stones. J Am Soc Nephrol. 2009 Oct;20(10):2253-9.
- Mohr SB, Gorham ED, Alcaraz JE, et al. Serum 25-hydroxyvitamin D and prevention of breast cancer: pooled analysis. Anticancer Res. 2011 Sep;31(9):2939-48.
- Timpini A, Pini L, Tantucci C, Cossi S, Grassi V. Vitamin D and health status in elderly. Intern Emerg Med. 2011 Feb;6(1):11-21.
- Nair-Shalliker V, Fenech M, Forder PM, Clements MS, Armstrong BK. Sunlight and vitamin D affect DNA damage, cell division and cell death in human lymphocytes: a cross-sectional study in South Australia. Mutagenesis 2012 Sep;27(5):609-14.
- Heaney RP, Davies KM, Chen TC, Holick MF, Barger-Lux MJ. Human serum 25-hydroxycholecalciferol response to extended oral dosing with cholecalciferol. Am J Clin Nutr. 2003 Jan;77(1):204-10.
- Available at: http://onlinelibrary.wiley.com/doi/10.1002/jbmr.328/pdf. Accessed January 11, 2013.
- Garland CF, French CB, Baggerly LL, Heaney RP. Vitamin D supplement doses and serum 25-hydroxyvitamin D in the range associated with cancer prevention. Anticancer Res. 2011 Feb;31(2):607-11.
- Available at: http://health.usnews.com/health-news/diet-fitness/diabetes/articles/2011/02/27/higher-vitamin-d-intake-could-cut-cancer-risk. Accessed January 11, 2013.
- Available at: http://articles.mercola.com/sites/articles/archive/2013/01/05/vitamin-d-health-benefits.aspx. Accessed January 11, 2013.
- Available at: https://www.lifeextension.com/magazine/mag2010/jan2010_Startling-Findings-About-Vitamin-D-Levels-in-Life-Extension-Members_01.htm. Accessed January 11, 2013.
- Garland CF, Gorham ED, Mohr SB, et al. Vitamin D and prevention of breast cancer: pooled analysis. J Steroid Biochem Mol Biol. 2007 Mar;103(3-5):708-11.
- Gorham ED, Garland CF, Garland FC, et al. Vitamin D and prevention of colorectal cancer. J Steroid Biochem Mol Biol. 2005 Oct;97(1-2):179-94.
- Feskanich D, Ma J, Fuchs CS, et al. Plasma vitamin D metabolites and risk of colorectal cancer in women. Cancer Epidemiol Biomarkers Prev. 2004 Sep;13(9):1502-8.
- Marshall DT, Savage SJ, Garrett-Mayer E, et al. Vitamin D3 supplementation at 4000 international units per day for one year results in a decrease of positive cores at repeat biopsy in subjects with low-risk prostate cancer under active surveillance. J Clin Endocrinol Metab. 2012 Jul;97(7):2315-24.
- John EM, Schwartz GG, Koo J, Van Den BD, Ingles SA. Sun exposure, vitamin D receptor gene polymorphisms, and risk of advanced prostate cancer. Cancer Res. 2005 Jun 15;65(12):5470-9.
- Tworoger SS, Lee IM, Buring JE, Rosner B, Hollis BW, Hankinson SE. Plasma 25-hydroxyvitamin D and 1,25-dihydroxyvitamin D and risk of incident ovarian cancer. Cancer Epidemiol Biomarkers Prev. 2007 Apr;16(4):783-8.
- Moyer VA, U.S. Preventive Services Task Force. Screening for prostate cancer: U.S. Preventive Services Task Force recommendation statement. Ann Intern Med. 2012 Jul 17;157(2):120-34.
- Glenski WJ, Klee GG, Bergstralh EJ, Oesterling JE. Prostate-specific antigen: establishment of the reference range for the clinically normal prostate gland and the effect of digital rectal examination, ejaculation, and time on serum concentrations. Prostate. 1992;21(2):99-110.
- Available at: http://www.cancer.gov/newscenter/qa/2009/plcoprostateresultsqa. Accessed January 11, 2013.
- Andriole GL, Marberger M, Roehrborn CG. Clinical usefulness of serum prostate specific antigen for the detection of prostate cancer is preserved in men receiving the dual 5alpha-reductase inhibitor dutasteride. J Urol. 2006 May;175(5):1657-62.
- Andriole GL, Humphrey P, Ray P, et al. Effect of the dual 5alpha-reductase inhibitor dutasteride on markers of tumor regression in prostate cancer. J Urol. 2004 Sep;172(3):915-9.
- Andriole GL, Bostwick DG, Brawley OW, et al. Effect of dutasteride on the risk of prostate cancer. N Engl J Med. 2010 Apr 1;362(13):1192-202.
- Kashuba VI, Pavlova TV, Grigorieva EV, et al. High mutability of the tumor suppressor genes RASSF1 and RBSP3 (CTDSPL) in cancer. PLoS One. 2009 May 29;4(5):e5231.
- Available at: http://www.cancerscreening.nhs.uk/prostate/prostate-booklet-text.pdf. Accessed February 4, 2013.
- Sakr WA, Haas GP, Cassin BF, Pontes JE, Crissman JD. The frequency of carcinoma and intraepithelial neoplasia of the prostate in young male patients. J Urol. 1993 Aug;150(2 Pt 1):379-85.
- Deslypere JP, Young M, Wilson JD, McPhaul MJ. Testosterone and 5 alpha-dihydrotestosterone interact differently with the androgen receptor to enhance transcription of the MMTV-CAT reporter gene. Mol Cell Endocrinol. 1992 Oct;88(1-3):15-22.
- Wright AS, Thomas LN, Douglas RC, Lazier CB, Rittmaster RS. Relative potency of testosterone and dihydrotestosterone in preventing atrophy and apoptosis in the prostate of the castrated rat. J Clin Invest. 1996 Dec 1;98(11):2558-63.
- Andriole GL, Roehrborn C, Schulman C, et al. Effect of dutasteride on the detection of prostate cancer in men with benign prostatic hyperplasia. Urology. 2004 Sep;64(3):537-41.
- Thompson IM, Goodman PJ, Tangen CM, et al. The influence of finasteride on the development of prostate cancer. N Engl J Med. 2003 Jul 17;349(3):215-24.
- Available at: http://www.drugs.com/sfx/avodart-side-effects.html. Accessed January 11, 2013.
- Djavan B, Bursa B, Seit z C, et al. Insulin-like growth factor 1 (IGF-1), IGF-1 density, and IGF-1/PSA ratio for prostate cancer detection. Urology. 1999;54:603-6.
- Wolk A, Mantzoros CS , Andersson SO, et al. Insulin-like growth factor 1 and prostate cancer risk: a population-based, case-control study . J Nat l Cancer Inst. 1998;90:911-15.
- Mantzoro s CS , Tzono u A, Signorello LB , et al. Insulin-like growth factor 1 in relation to prostate cancer and benign pro-static hyperplasia. Br J Cancer. 1997;76:1115-18.
- Cohen P, Peehl DM, Graves HC, Rosenfeld RG. Biological effects of prostate specific antigen as an insulin-like growth factor binding protein-3 protease. J Endocrinol. 1994 Sep;142(3):407-15.
- Gallardo-Williams MT, Chapin RE, King PE, et al. Boron supplementation inhibits the growth and local expression of IGF-1 in human prostate adenocarcinoma (LNCaP) tumors in nude mice. Toxicol Pathol. 2004 Jan;32(1):73-8.
- Barranco WT, Eckhert CD. Boric acid inhibits human prostate cancer cell proliferation. Cancer Lett. 2004 Dec 8;216(1):21-9.
- Cui Y, Winton MI, Zhang ZF, et al. Dietary boron intake and prostate cancer risk. Oncol Rep. 2004 Apr;11(4):887-92.
- Pezzato E, Sartor L, Dell’Aica I, et al. Prostate carcinoma and green tea: PSA-triggered basement membrane degradation and MMP-2 activation are inhibited by (-) epigallocatechin-3-gallate. Int J Cancer. 2004 Dec 10;112(5):787-92.
- Siddiqui IA, Malik A, Adhami VM, et al. Green tea polyphenol EGCG sensitizes human prostate carcinoma LNCaP cells to TRAIL-mediated apoptosis and synergistically inhibits biomarkers associated with angiogenesis and metastasis. Oncogene. 2008 Mar 27;27(14):2055-63.
- McCarthy S, Caporali A, Enkemann S, et al. Green tea catechins suppress the DNA synthesis marker MCM7 in the TRAMP model of prostate cancer. Mol Oncol. 2007 Sep;1(2):196-204.
- Adhami VM, Siddiqui IA, Ahmad N, Gupta S, Mukhtar H. Oral consumption of green tea polyphenols inhibits insulin-like growth factor-I-induced signaling in an autochthonous mouse model of prostate cancer. Cancer Res. 2004 Dec 1;64(23):8715-22.
- McLarty J, Bigelow RL, Smith M, Elmajian D, Ankem M, Cardelli JA. Tea polyphenols decrease serum levels of prostate-specific antigen, hepatocyte growth factor, and vascular endothelial growth factor in prostate cancer patients and inhibit production of hepatocyte growth factor and vascular endothelial growth factor in vitro. Cancer Prev Res. (Phila). 2009 Jul;2(7):673-82.
- Ansari MS, Gupta NP. Lycopene: a novel drug therapy in hormone refractory metastatic prostate cancer. Urol Oncol. 2004 Sep;22(5):415-20.
- Ansari MS, Gupta NP. A comparison of lycopene and orchidectomy vs orchidectomy alone in the management of advanced prostate cancer. BJU Int. 2003 Sep;92(4):375-8.
- Davis-Searles PR, Nakanishi Y, Kim NC, et al. Milk thistle and prostate cancer: differential effects of pure flavonolignans from Silybum marianum on antiproliferative end points in human prostate carcinoma cells. Cancer Res. 2005 May 15;65(10):4448-57.
- Zi X, Agarwal R. Silibinin decreases prostate-specific antigen with cell growth inhibition via G1 arrest, leading to differentiation of prostate carcinoma cells: implications for prostate cancer intervention. Proc Natl Acad Sci USA. 1999 Jun 22;96(13):7490-5.
- Singh RP, Agarwal R. A cancer chemopreventive agent silibinin, targets mitogenic and survival signaling in prostate cancer. Mutat Res. 2004 Nov 2;555(1-2):21-32.
- Moyers SB, Kumar NB. Green tea polyphenols and cancer chemoprevention: multiples mechanisms and endpoints for phase II trials. Nutr Rev. 2004 May;62(5)204-11.
- Kim HS, Kim MH, Jeong M, et al. EGCG blocks tumor promoter-induced MMP-9 expression via suppression of MAPK and AP-1 activiation in human gastric AGS cells. Anticancer Res. 2004 Mar-Apr;24(2B):747-53.
- Pillai SP, Mitscher LA, Menon SR, et al. Antimutagenic/antioxidant activity of green tea components and related compounds. J Environ Pathol Toxicol Oncol. 1999;18(3):147-58.
- Khan N, Mukhtar H. Multitargeted therapy of cancer by green tea polyphenols. Cancer Lett. 2008 Oct 8;269(2):269-80.
- Siddiqui IA, Shukla Y, Adhami VM, et al. Suppression of NFkappaB and its regulated gene products by oral administration of green tea polyphenols in an autochthonous mouse prostate cancer model. Pharm Res. 2008 Sep;25(9):2135-42.
- Yang CS, Wang X. Green tea and cancer prevention. Nutr Cancer. 2010;62(7):931-7.
- Reuter S, Eifes S, Dicato M, Aggarwal BB, Diederich M. Modulation of anti-apoptotic and survival pathways by curcumin as a strategy to induce apoptosis in cancer cells. Biochem Pharmacol. 2008 Dec 1;76(11):1340-51.
- Agrawal DK, Mishra PK. Curcumin and its analogues: potential anticancer agents. Med Res Rev. 2010 Sep;30(5):818-60.
- Vijayakumar S, Mehta RR, Boerner PS, Packianathan S, Mehta RG. Clinical trials involving vitamin D analogs in prostate cancer. Cancer J. 2005 Sep-Oct;11(5):362-73.
- Lou YR, Qiao S, Talonpoika R, Syvala H, Tuohimaa P. The role of Vitamin D3 metabolism in prostate cancer. J Steroid Biochem Mol Biol. 2004 Nov;92(4):317-25.
- John EM, Schwartz GG, Koo J, Van Den BD, Ingles SA. Sun exposure, vitamin D receptor gene polymorphisms, and risk of advanced prostate cancer. Cancer Res. 2005 Jun 15;65(12):5470-9.
- Woo TC, Choo R, Jamieson M, Chander S, Vieth R. Pilot study: potential role of vitamin D (Cholecalciferol) in patients with PSA relapse after definitive therapy. Nutr Cancer. 2005;51(1):32-6.
- Sarkar FH, Li Y. Indole-3-carbinol and prostate cancer. J Nutr. 2004 Dec;134(12 Suppl):3493S-8S.
- Garikapaty VP, Ashok BT, Chen YG, et al. Anti-carcinogenic and anti-metastatic properties of indole-3-carbinol in prostate cancer. Oncol Rep. 2005 Jan;13(1):89-93.
- Nachshon-Kedmi M, Yannai S, Haj A, Fares FA. Indole-3-carbinol and 3,3’-diindolylmethane induce apoptosis in human prostate cancer cells. Food Chem Toxicol. 2003 Jun;41(6):745-52.
- Helzlsouer KJ, Huang HY, Alberg AJ, et al. Association between alpha-tocopherol, gamma-tocopherol, selenium, and subsequent prostate cancer. J Natl Cancer Inst. 2000 Dec 20;92(24):2018-23.
- Campbell SE, Musich PR, Whaley SG, et al. Gamma tocopherol upregulates the expression of 15-S-HETE and induces growth arrest through a PPAR gamma-dependent mechanism in PC-3 human prostate cancer cells. Nutr Cancer. 2009;61(5):649-62.
- Jiang Q, Wong J, Fyrst H, Saba JD, Ames BN. Gamma-tocopherol or combinations of vitamin E forms induce cell death in human prostate cancer cells by interrupting sphingolipid synthesis. Proc Natl Acad Sci U S A. 2004 Dec 21;101(51):17825-30.
- Spaccarotella KJ, Kris-Etherton PM, Stone WL, et al. The effect of walnut intake on factors related to prostate and vascular health in older men. Nutr J. 2008 May 2;7:13.
- Adjakly M, Ngollo M, Boiteux JP, Bignon YJ, Guy L, Bernard-Gallon D. Genistein and daidzein: different molecular effects on prostate cancer. Anticancer Res 2013 Jan;33(1):39-44.
- Guo Y, Wang S, Hoot DR, Clinton SK. Suppression of VEGF-mediated autocrine and paracrine interactions between prostate cancer cells and vascular endothelial cells by soy isoflavones. J Nutr Biochem. 2007 Jun;18(6):408-17.
- Ben Sahra I, Laurent K, Giuliano S, et al. Targeting cancer cell metabolism: the combination of metformin and 2-deoxyglucose induces p53-dependent apoptosis in prostate cancer cells. Cancer Res. 2010 Mar 15;70(6):2465-75.
- Wright JL, Stanford JL. Metformin use and prostate cancer in Caucasian men: results from a population-based case-control study. Cancer Causes Control. 2009 Nov;20(9):1617-22.
- Schröder FH, Hugosson J, Roobol MJ, et al. Screening and prostate-cancer mortality in a randomized European study. N Engl J Med. 2009 Mar 26;360(13):1320-8.
- Hugosson J, Carlsson S, Aus G, et al. Mortality results from the Göteborg randomised population-based prostate-cancer screening trial. Lancet Oncol. 2010 Aug;11(8):725-32.
- Kjellman A, Akre O, Norming U, Törnblom M, Gustafsson O. 15-year followup of a population based prostate cancer screening study. J Urol. 2009;181:1615-21.
- Sandblom G, Varenhorst E, Rosell J, Löfman O, Carlsson P. Randomised prostate cancer screening trial: 20 year follow-up. BMJ. 2011;342:d1539.
- Available at: https://www.labcorp.com. Accessed February 7, 2013.
- Available at: http://www.questdiagnostics.com/testcenter/testdetail.action?ntc=5363. Accessed February 7, 2013.
- Available at: http://archive.is/bm3a. Accessed March 18, 2013.
- Available at: http://www.asco.org/ascov2/meetings/abstracts?&vmview=abst_detail_view&confid=54&abstractid=20081. Accessed February 7, 2013.

