Life Extension Magazine®
High blood pressure, or hypertension, is a contributor to the development of atherosclerosis, stroke, kidney failure, dementia and heart disease.1-5
The root cause of high blood pressure in adults is often unclear.
Certain conditions, like diabetes, increase the chances of developing high blood pressure.
Unhealthy behaviors that put individuals at greater risk for developing high blood pressure include lack of physical activity and obesity.6,7
The medical profession is coming to the realization that magnesium deficiency is another risk factor.
A recent article published in the International Journal of Molecular Sciences provides an updated overview of the evidence linking hypertension—and the vascular diseases it causes—with magnesium deficiency.8
Magnesium deficiency is more common than most people realize. It has been estimated that 64% of all men and 67% of women in the U.S. have inadequate dietary intake of magnesium. More than 80% of people over the age of 71 have an inadequate dietary intake of magnesium.9
Low-cost magnesium supplements provide an easy and effective solution.
What you need to know
Most men and women in the United States are deficient in magnesium, and this deficiency is strongly correlated with hypertension. Multiple studies have shown that magnesium can help maintain a healthy blood pressure. This has been shown through its ability to increase production of prostaglandin E1, which is a vascular relaxant that also prevents clots from forming inside blood vessels.
Hypertension Causes Heart Disease
Heart disease is the leading cause of death in the U.S. and worldwide.1
There are many risk factors for heart disease, including elevated blood lipids, smoking, advancing age, obesity, and elevated blood glucose levels.1
Hypertension is one of the most prevalent risk factors.1 According the American Heart Association, an estimated 41.4% of Americans will have high blood pressure by 2030.10
Over time, high blood pressure inflicts damage on the blood vessels and heart, accelerating the development of coronary artery blockage and heart failure.8
Hypertension Caveats
For many aging individuals, blood pressure lowering medications are essential to bring blood pressure to optimal ranges of around 115/75 mmHg.
Beta-blocker drugs like carvedilol in the dose of 12.5 mg a day may be considered as a first choice to optimizing blood pressure.
Carvedilol and other beta-blockers have some interesting side benefits, such as reduced risk of certain cancers, reduced risk of sudden heart attack, and possible slowing of certain aging processes.
Since the early 1980s, Life Extension® has urged people to keep their systolic pressure below 120 mmHg. Back in those days, doctors did not usually start treating blood pressure until systolic pressure reached 160 mmHg. A consistent flow of published data supports the benefit of maintaining one’s blood pressure in the low normal ranges (around 115/75 mmHg).
An important caveat relates to older people with damaged vascular systems often caused by decades of chronic hypertension. The capillary beds of these individuals are sometimes so broken that a higher level of blood pressure may be required to sustain life, which is ironic since these higher blood pressure levels cause even more vascular damage.
A solution for people with chronic vascular insufficiencies (such as atherosclerosis and/or reduced brain-kidney blood flow) is to gradually reduce blood pressure and use nutrients, hormones and drugs that may help reverse arterial damage by improving endothelial (inner arterial wall) function.
How Low Magnesium Leads to Hypertension
Several conditions contribute to the development of high blood pressure, such as whether blood vessels are flexible (constricted or relaxed), stress responses, and structural changes in the blood vessels themselves.
Low magnesium levels impact all these conditions.
Blood Vessel Constriction
Magnesium keeps blood pressure down by aiding blood vessel relaxation and dilation.11-13
Magnesium is a cofactor, or “helper compound,” required for hundreds of reactions throughout the body. One of those reactions leads to the production of prostaglandin E1, an important vascular relaxant which also helps prevent clots from forming inside blood vessels.14
Magnesium also tempers the secretion of the hormone aldosterone, which causes the kidney to hold on to sodium and water. This can affect blood pressure.15-17
When there’s a deficiency of magnesium, blood vessels are chronically constricted and sodium and water are retained, resulting in hypertension.
Stress Responses
Stress is a physiological risk factor that leads to elevated blood pressure.8
Sympathetic nervous system reflexes, often referred to as our “fight or flight” responses, cause the release of neurotransmitters and hormones known collectively as catecholamines. These compounds exert a powerful constricting effect on blood vessels, raising blood pressure.
In lab studies, magnesium was shown to reduce the amount of catecholamines released in response to stressors.15,18
A deficiency of magnesium lets stress responses run amok, leading to vascular constriction and resulting hypertension.
Blood Vessel Structure
Magnesium deficiency causes several changes that accelerate the aging and hardening of arteries.
It leads to low-grade inflammation and oxidative stress in blood vessel walls.19 Over time, this causes dysfunction of the blood vessel that results in arterial stiffness and, ultimately, atherosclerosis—which raises blood pressure.20
Low levels of magnesium also increase the “permeability” of the blood vessel lining, allowing more LDL (or “bad”) cholesterol to get into the vessel wall.21 This leads to an increase in the atherosclerotic plaque that narrows the blood vessel, which can result in heart disease.
Magnesium deficiency has also been tied to metabolic syndrome and type II diabetes, characterized by elevated blood glucose levels.22-25 This further contributes to blood-vessel wall damage and the progression of atherosclerosis.
What Human Studies Reveal

Numerous human clinical trials have found an association between magnesium and hypertension.26-28
These studies show that the lower the magnesium level in patients, the higher the systolic blood pressure.
Other studies, including a meta-analysis of trials that enrolled more than 2,000 subjects, have found that supplementation with magnesium reduces systolic and diastolic blood pressure in hypertensive patients.29
Human studies have also demonstrated an association between low magnesium and risk for cardiovascular events, including heart attack and stroke.9,12
A meta-analysis that looked at 5 studies with 58,750 participants found that there was a 9% reduction in risk for cardiovascular events with every 0.12 mg/dL increase in serum magnesium levels.9
Magnesium Intake and Blood Pressure Critical Factors for Success
Many factors conspire to create magnesium insufficiency in our bodies.
Some of these factors include poor dietary intake, accelerated loss from the body (impaired absorption, excessive urinary loss), alcohol intake, and some types of medications, especially drugs (both over-the-counter and prescription) for treatment of acid reflux (antacids, and other acid blockers like H2-receptor antagonists and proton pump inhibitors). Some blood pressure medications (especially diuretics) and even some types of antibiotics can contribute to inadequate magnesium status, too.
The good news is that in most cases, magnesium intake in the range of 500 to 1,000 mg per day may help reduce systolic blood pressure as much as 5 mmHg; however, not all data indicate success.30-33
The reason for this apparent inconsistency is because of a failure to adequately control for both sodium and potassium intake.
In fact, reducing sodium intake while also increasing both potassium and magnesium intake helps to optimize healthy blood pressure levels. Published research suggests that magnesium has a far greater beneficial impact on blood pressure reduction when combined with both an increase in potassium intake and a reduction in sodium intake.34,35
Magnesium competes with sodium for binding sites on vascular smooth muscle cells and binds to potassium in a cooperative manner, increases prostaglandin E, helps support endothelial-dependent vasodilation and reduces endothelial dysfunction.36-38
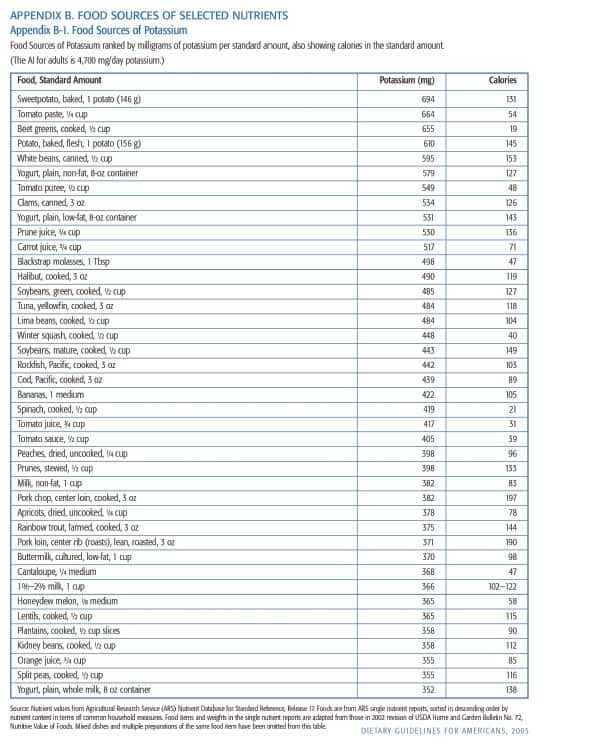
For optimal results, maximize blood pressure reduction with magnesium, between 500 and 1,000 mg daily from combined food sources (e.g. nuts, whole grains, beans) and dietary supplements. Obtain about 4,000 mg of potassium from dietary sources (leafy greens, potatoes, beans) and potassium supplements if needed. (Food sources of potassium are listed on next page.) Reduce sodium intake to less than 1,500 mg daily.39
Furthermore, in patients with pre-existing hypertension (high blood pressure), a comprehensive analytic review of 44 human studies of oral magnesium supplementation for hypertension showed that magnesium supplements enhanced the blood pressure-lowering effect of antihypertensive medications.27
In regard to the “ideal” or “best” form of magnesium for dietary supplementation, there are many factors to consider. In fact, the idea of a single “optimal” form of magnesium for supplementation is debatable. Instead, it is important to consider the reason for the supplement.
One approach for ideal magnesium supplementation is to use a 2-part supplement composed partly of magnesium citrate in a quick-release form and magnesium oxide in an extended-release form.
Magnesium oxide is highly concentrated, allowing a lot of magnesium to go into a relatively small pill. Because magnesium oxide is somewhat less bioavailable, it is ideal for an extended-release formulation, which gradually makes its way into the circulation.
Magnesium citrate, on the other hand, is less concentrated but is highly bioavailable, which allows for quick release of the mineral in a form that is readily absorbed. This kind of innovative combination provides extended magnesium benefits in a single supplement.
Summary
Magnesium is a mineral that is required for the healthy function of hundreds of enzymatic reactions in the body.
Magnesium deficiency is increasingly common. A recent review article reveals that low magnesium is a major contributor to the development of hypertension, which leads to atherosclerosis and heart disease.
Maintenance of normal magnesium levels helps keep blood pressure in the normal range and reduces the risk for cardiovascular disease, including the incidence of heart attack and stroke.
Supplementation with low-cost magnesium is recommended to treat deficiency and maintain optimal levels.
If you have any questions on the scientific content of this article, please call a Life Extension® Wellness Specialist at 1-866-864-3027.
References
- Available at: https://www.cdc.gov/heartdisease/facts.htm. Accessed January 28, 2019.
- Available at: https://www.heart.org/en/health-topics/cholesterol/about-cholesterol/atherosclerosis. Accessed January 28, 2019.
- Turin TC, Okamura T, Afzal AR, et al. Hypertension and lifetime risk of stroke. J Hypertens. 2016 Jan;34(1):116-22.
- Barri YM. Hypertension and kidney disease: a deadly connection. Curr Hypertens Rep. 2008 Feb;10(1):39-45.
- Kennelly SP, Lawlor BA, Kenny RA. Blood pressure and dementia - a comprehensive review. Ther Adv Neurol Disord. 2009 Jul;2(4):241-60.
- Available at: https://www.cdc.gov/dhdsp/data_statistics/fact_sheets/fs_bloodpressure.htm. Accessed January 28, 2018.
- Available at: https://www.webmd.com/hypertension-high-blood-pressure/guide/blood-pressure-causes. Accessed January 28, 2019.
- Kostov K, Halacheva L. Role of Magnesium Deficiency in Promoting Atherosclerosis, Endothelial Dysfunction, and Arterial Stiffening as Risk Factors for Hypertension. Int J Mol Sci. 2018 Jun 11;19(6).
- Qu X, Jin F, Hao Y, et al. Magnesium and the risk of cardiovascular events: a meta-analysis of prospective cohort studies. PLoS One. 2013;8(3):e57720.
- Benjamin EJ, Virani SS, Callaway CW, et al. Heart Disease and Stroke Statistics-2018 Update: A Report From the American Heart Association. Circulation. 2018 Mar 20;137(12):e67-e492.
- Cunha AR, Medeiros F, Umbelino B, et al. Altered vascular structure and wave reflection in hypertensive women with low magnesium levels. J Am Soc Hypertens. 2013 Sep-Oct;7(5):344-52.
- Grober U, Schmidt J, Kisters K. Magnesium in Prevention and Therapy. Nutrients. 2015 Sep 23;7(9):8199-226.
- Landau R, Scott JA, Smiley RM. Magnesium-induced vasodilation in the dorsal hand vein. BJOG. 2004 May;111(5): 446-51.
- Houston M. The role of magnesium in hypertension and cardiovascular disease. J Clin Hypertens (Greenwich). 2011 Nov;13(11):843-7.
- Belin RJ, He K. Magnesium physiology and pathogenic mechanisms that contribute to the development of the metabolic syndrome. Magnes Res. 2007 Jun;20(2):107-29.
- Swaminathan R. Magnesium metabolism and its disorders. Clin Biochem Rev. 2003 May;24(2):47-66.
- Laurant P, Dalle M, Berthelot A, et al. Time-course of the change in blood pressure level in magnesium-deficient Wistar rats. Br J Nutr. 1999 Sep;82(3):243-51.
- Douglas WW, Rubin RP. The mechanism of catecholamine release from the adrenal medulla and the role of calcium in stimulus-secretion coupling. J Physiol. 1963 Jul;167(2):288-310.
- Barbagallo M, Belvedere M, Dominguez LJ. Magnesium homeostasis and aging. Magnes Res. 2009 Dec;22(4):235-46.
- Harvey A, Montezano AC, Lopes RA, et al. Vascular Fibrosis in Aging and Hypertension: Molecular Mechanisms and Clinical Implications. Can J Cardiol. 2016 May;32(5):659-68.
- Maier JA. Endothelial cells and magnesium: implications in atherosclerosis. Clin Sci (Lond). 2012 May;122(9): 397-407.
- Barbagallo M, Dominguez LJ. Magnesium metabolism in type 2 diabetes mellitus, metabolic syndrome and insulin resistance. Arch Biochem Biophys. 2007 Feb 1;458(1):40-7.
- Barbagallo M, Dominguez LJ. Magnesium and the cardiometabolic syndrome. Curr Nutr Rep. 2012;1(2):100-8.
- Chaudhary DP, Sharma R, Bansal DD. Implications of magnesium deficiency in type 2 diabetes: a review. Biol Trace Elem Res. 2010 May;134(2):119-29.
- Geiger H, Wanner C. Magnesium in disease. Clin Kidney J. 2012 Feb;5(Suppl 1):i25-i38.
- Ma J, Folsom AR, Melnick SL, et al. Associations of serum and dietary magnesium with cardiovascular disease, hypertension, diabetes, insulin, and carotid arterial wall thickness: the ARIC study. Atherosclerosis Risk in Communities Study. J Clin Epidemiol. 1995 Jul;48(7):927-40.
- Rosanoff A. Magnesium supplements may enhance the effect of antihypertensive medications in stage 1 hypertensive subjects. Magnes Res. 2010 Mar;23 (1):27-40.
- Whang R, Chrysant S, Dillard B, et al. Hypomagnesemia and hypokalemia in 1,000 treated ambulatory hypertensive patients. J Am Coll Nutr. 1982;1(4):317-22.
- Zhang X, Li Y, Del Gobbo LC, et al. Effects of Magnesium Supplementation on Blood Pressure: A Meta-Analysis of Randomized Double-Blind Placebo-Controlled Trials. Hypertension. 2016 Aug;68(2):324-33.
- Jee SH, Miller ER, 3rd, Guallar E, et al. The effect of magnesium supplementation on blood pressure: a meta-analysis of randomized clinical trials. Am J Hypertens. 2002 Aug;15(8):691-6.
- Touyz RM. Role of magnesium in the pathogenesis of hypertension. Mol Aspects Med. 2003 Feb-Jun;24(1-3):107-36.
- Resnick LM. Magnesium in the pathophysiology and treatment of hypertension and diabetes mellitus: where are we in 1997? Am J Hypertens. 1997 ar;10(3):368-70.
- Houston M. Magnesium and Hypertension. In: Watson RR, Preedy VR, Zibadi S, editors. Magnesium in Human Health and Disease. New York: Humana Press; 2013:183-9.
- Weaver CM, Bailey RL, McCabe LD, et al. Mineral Intake Ratios Are a Weak but Significant Factor in Blood Pressure Variability in US Adults. J Nutr. 2018 Nov 1;148(11):1845-51.
- Patki PS, Singh J, Gokhale SV, et al. Efficacy of potassium and magnesium in essential hypertension: a double-blind, placebo controlled, crossover study. BMJ. 1990 Sep 15;301(6751):521-3.
- McCarty MF. Complementary vascular-protective actions of magnesium and taurine: a rationale for magnesium taurate. Med Hypotheses. 1996 Feb;46(2):89-100.
- Yamori Y, Taguchi T, Mori H, et al. Low cardiovascular risks in the middle aged males and females excreting greater 24-hour urinary taurine and magnesium in 41 WHO-CARDIAC study populations in the world. J Biomed Sci. 2010 Aug 24;17 Suppl 1:S21.
- Barbagallo M, Dominguez LJ, Galioto A, et al. Oral magnesium supplementation improves vascular function in elderly diabetic patients. Magnes Res. 2010 Sep;23(3):131-7.
- Houston MC. The importance of potassium in managing hypertension. Curr Hypertens Rep. 2011 Aug;13(4):309-17.

