
Stroke
Stroke
Last Section Update: 11/2025
Contributor(s): Maureen Williams, ND; Stephen Tapanes, PhD
1 Overview
Summary and Quick Facts for Stroke
- Stroke is a leading cause of death and disability around the world. A stroke occurs when blood flow to the brain is interrupted, depriving the brain of oxygen and resulting in cell death and tissue damage.
- A stroke is most commonly caused by the blockage of a blood vessel in the head or neck but may also be caused by the rupture of a blood vessel in the brain.
- Immediate treatment can dramatically improve outcomes after stroke and is associated with a greater chance of survival.
- A healthy diet and lifestyle, along with nutrients like olive polyphenols and nattokinase can promote good metabolic and vascular health and may reduce the risk for stroke.
- Emergency treatment, usually within 4.5 hours of the onset of a stroke, is essential. If you or someone you know exhibit any signs of a stroke, call 911 immediately.
What is a Stroke?
A stroke is the result of the loss of blood flow, and consequently oxygen, to part of the brain. Decreased blood flow to parts of the brain can be caused by a blockage, often from blood clots (ischemic stroke), or the rupture of a brain blood vessel and subsequent hemorrhaging (hemorrhagic stroke). Strokes are one of the leading causes of death and disability around the world.
Ischemic and hemorrhagic strokes are severe and life-threatening. Other types of strokes, including transient ischemic attacks (“mini strokes” that resolve within minutes to hours) and silent strokes (strokes that do not cause overt stroke symptoms) are also considered medical emergencies and should receive urgent medical attention.
Nutrients
- Olive oil and olive extracts: Compounds derived from olives, including olive oil, have been found to promote good metabolic health, have antioxidant activity, and have been shown to protect neurons from damage during periods of ischemia.
- Omega-3 fatty acids: Omega-3 polyunsaturated fatty acids, notably eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA), exhibit a host of protective benefits that may lower stroke risk. They have anti-inflammatory properties, help protect against oxidative stress, and promote neuron regeneration and revascularization after stroke.
- Flavonoids: Flavonoids are compounds in fruits, vegetables, grains, and tea. Diets rich in flavonoids may reduce the risk for stroke. Dietary intake of flavanone, a flavonoid found in citrus fruits, has been found to exhibit an inverse relationship with stroke risk.
- Folic acid and B vitamins: Folic acid and other B vitamins reduce levels of homocysteine, an amino acid that promotes inflammation and atherosclerosis. Studies suggest folic acid and vitamin B6 supplementation reduce the risk for stroke.
- Nattokinase: Extracted from fermented soybeans, studies suggest nattokinase exhibits lipid-lowering, antihypertensive, antiplatelet, and anticoagulant activity.
Medical Treatment
Emergency treatment for ischemic stroke may involve:
- Intravenous thrombolysis (breaking down the clot) with alteplase, a tissue plasminogen activator (tPa)
- Mechanical thrombectomy (removal of the clot)
- Blood pressure management
- Antiplatelet therapy (aspirin)
- Cholesterol management (statins)
Emergency treatment for hemorrhagic stroke may involve:
- Reversal of oral anticoagulant therapy (eg, delivery of high-dose intravenous vitamin K in warfarin users)
- Management of intracranial pressure
- Blood pressure management
2 Introduction and Background
Stroke is a leading cause of disability and the second leading cause of death worldwide.2 Globally, more than 13 million people experience a stroke each year, and almost 6 million die as a result.3 Around the world, about one of every four people will experience a stroke from 25 years of age onward.4 Although older adults are most commonly affected by stroke, the incidence of stroke is growing rapidly among young people.5
A stroke occurs when part of the brain is deprived of blood and oxygen, which can cause cells to die.6 This can occur either when a clot blocks blood flow to the brain, known as an ischemic stroke, or when a blood vessel in or around the brain ruptures, known as a hemorrhagic stroke.6 Ischemic strokes are much more common than hemorrhagic strokes. The American Stroke Association (ASA) estimates that 87% of strokes that occur in the United States are ischemic strokes.7
When a stroke occurs, time is of the essence. Treatment of stroke within 4.5 hours is associated with the greatest likelihood of survival and reduced risk for disability.8,9 However, one-third to one-half of stroke patients do not call 911 before going to the hospital.10,11 According to a 2021 report from the American Heart Association (AHA), 64% of stroke deaths occur outside of an acute care hospital setting.12 Early recognition of the symptoms of stroke can mean the difference between life and death.
The ASA estimates that up to 80% of strokes are preventable.6 Elevated blood pressure is the primary stroke risk factor, and almost two-thirds of people who experience a stroke have high blood pressure.13 Blood pressure control is a crucial aspect of cardiovascular health, and maintaining good cardiovascular health can reduce stroke risk by up to 70%.12
General strategies to improve cardiovascular health can also help reduce the risk of stroke. These include consuming a healthy diet (such as the Mediterranean diet), getting regular physical activity, maintaining a healthy weight, managing other health conditions (such as diabetes or high cholesterol), and stopping smoking.2,12,14-16 Dietary and supplemental nutrients including olive extracts, nattokinase, folic acid, and flavonoids can also support metabolic and vascular health and reduce the risk for stroke.
For people with atrial fibrillation (A-fib), certain medications (eg, anticoagulant therapy) may be required to reduce the risk of stroke.17 A-fib is a condition that causes the heart to beat irregularly, which increases the risk of ischemic stroke up to 5-fold. It is estimated that one of every seven strokes are linked to A-fib.18
This protocol will review the different types of strokes and their causes, as well as the risk factors, signs, and symptoms of stroke. Stroke treatment will be discussed, and strategies to mitigate stroke risk through dietary and lifestyle changes, as well as targeted nutrient supplementation, will also be reviewed.
3 Types of Stroke
There are two main types of strokes: ischemic and hemorrhagic.6,19 Strokes are differentiated by type based on clinical presentation and symptoms, as well as brain imaging.19
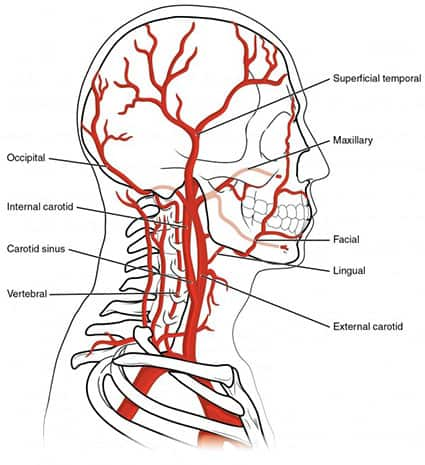
The brain is an energy-intensive organ, using an estimated 20% of the body’s total oxygen while at rest.21 Oxygen is delivered to the brain via two sets of arteries: the left and right carotid arteries, and the left and right vertebral arteries (Figure 1).22 The carotid arteries extend along the front of the neck, whereas the vertebral arteries run more internally along the spinal cord.22 These four arteries supply all of the blood and oxygen to the head and brain, including through a network of smaller vessels that branch off from these four. When blood flow to the brain from any of these vessels is interrupted, it can lead to the death of brain cells and irreversible tissue damage, known as infarction.19,22
Ischemic Stroke
Most ischemic strokes are caused by the obstruction of blood flow through an artery that supplies blood to the brain. There are two main subtypes of ischemic stroke: thrombotic and embolic.22
- A thrombotic stroke occurs when a blood clot, orthrombus, blocks an artery supplying blood to the brain.22 When this blockage occurs in the carotid or vertebral arteries, or in another intracranial large vessel, it is known aslarge vessel thrombosis or large vessel occlusion.23 Strokes can also result from obstructions in the small vessels of the brain, such as those on the surface of the brain.24 Small vessel strokes, also known as lacunar strokes, account for about 25% of all ischemic strokes. Compared with other types of strokes, lacunar strokes have a higher rate of survival and a lower rate of recurrence, and are generally associated with a more favorable prognosis in the early stages after stroke; however, they are still associated with an increased risk for death in the long-term, primarily from cardiovascular events.25
- Embolic strokes occur when a blood clot or fragment of atherosclerotic plaque travels through the bloodstream from another area of the body and becomes lodged in an artery supplying blood to the brain.7,22 These clots typically originate in the arteries of the heart, chest, or neck.7
- Cardioembolic strokes
are those caused by clots originating in the heart or aorta.26 Approximately one in four ischemic strokes are
cardioembolic strokes.27 The risk of cardioembolic stroke is
greater in people with a history of many different kinds of heart
disease or injury, including A-fib, valvular heart disease, myocardial
infarction (heart attack), and heart failure.26,27
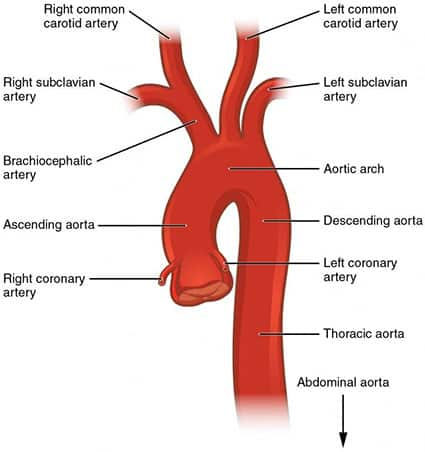
The aorta is the largest artery in the body, and the aortic arch has been identified as a major source of plaque debris associated with embolic stroke (Figure 2). Up to 21% of people with severe aortic plaque may experience a stroke.28 The relationship between aortic atherosclerosis and the risk for stroke remains unclear due to inconsistencies in studies, but researchers have suggested that plaque buildup in this region may be indicative of more widespread atherosclerotic disease, which increases the risk for stroke.29
Hemorrhagic Stroke
A hemorrhagic stroke occurs when a blood vessel in the brain ruptures and bleeds (hemorrhages). While hemorrhagic strokes are less common than ischemic strokes, some studies have shown they are associated with higher rates of disability and death.35-38 Hypertension is the most frequent cause of hemorrhagic stroke, as chronic elevated pressure puts a strain on the blood vessels in the brain and causes damage to their structures. This pressure can eventually cause the blood vessel to leak or burst, which results in pooling of blood outside of blood vessels (hematoma). The enlargement of the hematoma, and associated release in pro-inflammatory factors, increases intracranial pressure, disrupts neuron activity, and leads to brain injury.39
Hemorrhagic strokes can also be caused by cerebral amyloid angiopathy, a condition in which proteins build up along the blood vessel wall and increase the risk for bleeding.40 Cerebral amyloid angiopathy is most often associated with hemorrhagic stroke in the elderly.41
Hemorrhagic strokes can be further classified based on location of the bleeding:
- Intracerebral hemorrhages , the most common type of hemorrhagic stroke,42 occur when an artery or arteriole within the brain bursts and bleeding occurs directly into the brain.22
- Subarachnoid hemorrhages occur into the space between the brain and the tissues that cover it.42 Subarachnoid hemorrhages are commonly caused by the rupture of an aneurysm,19 which occurs when the walls of a blood vessel weaken causing bulging or ballooning.43
4 Stroke Risk Factors
Up to 90% of strokes are caused by modifiable risk factors.19 Addressing these risk factors is critical for reducing the risk for stroke.
High Blood Pressure (Hypertension)
High blood pressure, also known as hypertension, is considered the number one risk factor for both ischemic and hemorrhagic stroke.19,291 Hypertension has been identified in nearly two-thirds of stroke patients, and hypertension is thought to be responsible for over half of strokes globally.13,44 The risk for stroke increases progressively as blood pressure rises over 115/75 mm Hg.44,45 In a meta-analysis of 61 studies comprised of almost 1 million people, every 20 mm Hg increase in systolic blood pressure (and 10 mm Hg increase in diastolic blood pressure) over 115/75 mm Hg increased the risk for death from stroke 2-fold in those aged 40‒69 years.46 Research provides strong evidence that antihypertensive therapy reduces the risk for stroke.13,44
Smoking
The chemicals in cigarette smoke, including nicotine and carbon monoxide, can cause damage to the heart and blood vessels, which increases the risk of stroke.291 In a meta-analysis of 14 studies including over 300,000 people, the risk for stroke was over 90% higher for people who currently smoked compared to those with no history of smoking.47 However, smoking cessation can reduce stroke risk considerably. Exposure to secondhand smoke can also increase stroke risk by 20‒30%.12
Diabetes
Obesity, high cholesterol, and high blood pressure are common in diabetics, raising the risk of stroke.291 However, diabetes itself also increases the risk for stroke, as high blood sugar levels can damage blood vessels.48 According to a pooled analysis of over 775,000 people, diabetes increased the risk for stroke by 83% in men and 128% in women.49
Obesity, Poor Diet, and Physical Inactivity
Research indicates obesity is associated with a greater than 50% increase in stroke risk in younger adults, but this may have to do with the co-occurrence of other risk factors, including hypertension and diabetes.50 A comparative study of approximately 3,300 adults examining the link between stroke and metabolic syndrome, which is characterized by hypertension, elevated blood glucose levels, dyslipidemia, and excess fat around the waistline, found that metabolic syndrome was associated with a 50% increase in the risk for stroke.51,52 Interestingly, an “obesity paradox” exists, in which the likelihood of better outcomes after stroke increases with body mass index (BMI), highlighting the complex interaction between weight and risk for and from stroke.53
Analyses of data from a very large global study of overall disease burden found that unhealthy behaviors such as physical inactivity and poor diet account for nearly half of stroke risk.12 In a paper published in 2009 on an observational trial in nearly 3,300 adults, regular moderate- to high-intensity physical activity was associated with a 35% reduction in the risk for ischemic stroke.54 A poor diet, characterized by low fruit and vegetable intake and high sodium content, has also been linked to increased risk for stroke, and diets rich in whole foods (eg, the Mediterranean diet) may be associated with decreased stroke risk.12
High Cholesterol (Dyslipidemia)
Abnormally high levels of cholesterol and other lipids (fats) in the blood are a key factor in the formation of atherosclerotic plaque in artery linings, including in the brain. This change in the structure and function of arteries is itself a significant contributor to hypertension, cerebrovascular disease, and stroke.55 However, while elevated total cholesterol levels are associated with an increased risk for ischemic stroke, they are associated with a lower risk of hemorrhagic stroke.56,57 Stroke risk may also be associated with specific types of cholesterol in the blood.57 Although results have been somewhat inconsistent, research suggests high-density lipoprotein cholesterol (HDL-C) may be protective against stroke, whereas elevated levels of low-density lipoprotein cholesterol (LDL-C) are associated with increased risk for stroke.12,56,57
Sickle Cell Disease
Sickle cell disease, also known as sickle cell anemia, can increase the risk for stroke.55 Studies have found that about one in nine people with sickle cell disease experience a stroke by 20 years of age, and one in four will have a stroke by 45 years of age.58
Sleep Apnea
Sleep apnea is characterized by episodic lapses in breathing during sleep, and is associated with an increased risk for stroke.57 Several studies found the risk for stroke is approximately 2- to 3-fold higher in people with sleep apnea.12,57 This relationship is especially pronounced for men with severe obstructive sleep apnea.59
High Homocysteine
Elevated levels of the amino acid homocysteine (hyperhomocysteinemia) can be caused by genetic mutations that affect methionine metabolism as well as nutritional deficiencies and are associated with a 2- to 3-fold increased risk for stroke.57 Some data from clinical trials suggest intake of B vitamins, which help lower homocysteine levels, may help decrease the risk for stroke, but there is limited evidence that homocysteine-lowering therapy reduces stroke risk in people with established atherosclerotic disease.57,60
A variety of non-modifiable factors have been identified that increase the risk for stroke.56
- Age. Although a stroke can happen at any age, the risk for stroke significantly increases with age. Older age is the most significant risk factor for stroke, and the incidence of stroke doubles every decade after age 55.56
- Medical history.
- A previous history of stroke or TIA substantially increases the risk for further stroke. People who have had one or more previous TIAs are nearly 10 times more likely to experience a stroke than their counterparts without a history of stroke or TIA.
- People who previously experienced a heart attack are at increased risk for stroke, as both are frequently caused by a buildup of plaque within the blood vessels.61
- Atrial fibrillation, or A-fib, is a heart condition characterized by arrythmia, which causes blood to move improperly through the heart and increases the likelihood of blood clot formation. People with A-fib have a 3- to 5-fold greater risk for stroke, and nearly one in four strokes after age 40 are caused by A-fib.62
- Sex. Risk for stroke is generally higher among females than males, which may be related to the risks associated with pregnancy and hormonal birth control use.56 Women are also more likely to die from stroke.61
- Race or ethnicity. African-Americans in the United States are more likely to experience a stroke compared with Caucasians.61 This may be due to differences in the prevalence of other risk factors, including hypertension, diabetes, and obesity.56,61
- Genetics and family history. Research has identified a number of genetic alterations associated with an increased risk of stroke.56 These may be independent mutations or they may be associated with other disorders that affect blood flow and clotting.56,61 People with a family member who has had a stroke, particularly if the stroke occurred at a young age (<65 years), are at increased risk for having a stroke.61
5 Stroke Prevention
Blood Pressure Control
There is a clear, demonstrated benefit on stroke risk reduction associated with blood pressure-lowering therapy.63 In a review of over 40 studies, use of low-dose diuretics as antihypertensive therapy was associated with a nearly 30% reduced risk for stroke compared with placebo. Other antihypertensive medications were similarly effective.64 Multiple analyses of clinical trials and studies have found that 10 to 12 mm Hg reductions in systolic blood pressure and 5 to 6 mm Hg reductions in diastolic blood pressure are associated with an up to 41% reduced risk for stroke.45,65,66 Antihypertensive therapy can also reduce the risk for another stroke after one has already occurred, lowering risk for a disabling or deadly second stroke by nearly 30%.67
Ideal blood pressure targets and intensity of treatment should be determined on an individual basis. A thorough discussion of blood pressure control strategies can be found in the “High Blood Pressure (Hypertension)” protocol.
Smoking Cessation
Quitting smoking reduces the risk of a stroke, and in those who have already had a stroke, it reduces the risk of another stroke. Smoking doubles the risk of dying in those who have a stroke. Importantly, the contribution of smoking to stroke risk is dose-dependent: the more one smokes, the greater the risk. Compared with a non-smoker, a one pack-per-day smoker is six times more likely to have a stroke. One reason is that smoking makes the blood more susceptible to clotting, increasing the likelihood of ischemic stroke. Smoking also causes blood vessels to narrow, which can raise blood pressure, and reduces the oxygen-carrying capacity of red blood cells.68
In a study of almost 3.8 million adults in Korea, smoking cessation reduced the risk for stroke by about 30%. This benefit was evident even after accounting for age, sex, BMI, alcohol consumption, income, and exercise. The weight gain that often occurs after quitting smoking did not interfere with the cardiovascular benefit of smoking cessation in this study.69 Compared with non-smokers or people who quit smoking more than 10 years prior, current smoking status increases stroke risk about 2- to 4-fold.70 In a study of over 3,000 Chinese adults who experienced stroke, the risk for recurrent stroke was 93% higher for current smokers compared with non-smokers, but the recurrence risk was only 31% higher in those who quit smoking after their stroke, and 16% higher in former smokers.71
Reducing exposure to secondhand smoke may also help reduce the risk for stroke. A meta-analysis of 14 studies involving over 303,000 people found that exposure to secondhand smoke, or passive smoking, was associated with a 45% increased risk for stroke.47
Studies on the effects of “vaping,” or the use of electronic cigarettes (e-cigarettes), are in the early stages, but suggest vaping is not a safe alternative to smoking cessation. One study found that compared with the use of combustible cigarettes alone, the combined use of combustible and e-cigarettes increased the likelihood of cardiovascular disease, including stroke, by 36%.72 A meta-analysis of six studies found no difference in the odds of developing cardiovascular problems, including stroke, among people who switched from smoking to vaping.73
Glycemic Control and Diabetes Management
High blood glucose levels, also known as hyperglycemia, damages the blood vessels and leads to vascular inflammation, endothelial dysfunction, increased arterial stiffness, and atherosclerotic plaque buildup, all of which increase the risk for stroke.74,75 In a meta-analysis of 64 studies, the relative risk of stroke in diabetic women was 2.28-fold greater than for non-diabetics, whereas in men the relative risk was 1.83-fold greater. Comparing diabetic women to diabetic men, women’s risk of stroke was 27% greater.49 In a Swedish observational study involving over 400,000 people with type 2 diabetes, the risk for stroke increased with worsening glycemic control. In this study, the risk for stroke was 27% higher in diabetic individuals with glycated hemoglobin (HbA1c) levels of 7.1–8% than in healthy controls, and at an HbA1c level > 10.1%, stroke risk was 114% higher. For every 3.0% increase in HbA1c, a 71% increase in stroke risk was observed.76
In an observational study that followed 14,856 diabetic participants for four years, those receiving metformin (Glucophage, a blood glucose-lowering drug) were about half as likely to experience a stroke than those not receiving metformin, suggesting this drug may have protective effects against stroke in diabetic patients. Effective glycemic control can also improve outcomes in people with diabetes who have had a stroke.77 A study demonstrated that higher levels of HbA1c were associated with lower cognitive scores over time in patients who had experienced a lacunar stroke.78 Similarly, hyperglycemia at the time of stroke was found to be associated with continued infarction growth, even after successful thrombectomy, in people who had large vessel ischemic stroke.79
Managing blood glucose levels may be even more important in stroke patients using antiplatelet therapy who carry excess body weight. In one study in over 3,000 subjects who had experienced a minor stroke or TIA, the combination of overweight/obesity and poor glycemic control reduced the efficacy of aspirin-clopidogrel treatment. This effect was not observed in subjects with either poor glycemic control or overweight/obesity alone.80
For a comprehensive discussion of glycemic control strategies, please see the “Diabetes and Glucose Control” protocol.
Weight Management
Obesity is a risk factor for stroke. Population studies suggest that obesity increases the risk for ischemic stroke by 50‒100% compared to patients with normal weight.81 The AHA and ASA noted that epidemiological evidence suggests stroke risk increases almost linearly above a BMI of 20 kg/m2, such that each 1 kg/m2 increase above 20 kg/m2 corresponds with a 5% increase in risk of stroke.82 The increase in stroke risk associated with obesity may be related to the increased frequency of cardiometabolic comorbidities typically linked to obesity, such as hypertension and diabetes, as well as poor diet and low physical activity.50,56,83 Losing even small amounts of weight (5‒10 lbs.), eating a healthier diet, and increasing physical activity can have profound effects on metabolic health, which could result in reduced stroke risk.291
The AHA/ASA recommend weight loss for primary stroke prevention in people with a BMI over 30 kg/m2. These organizations also recommend weight loss among individuals with a BMI of 25–29 kg/m2 to reduce blood pressure, which may in turn reduce stroke risk. Importantly, the AHA/ASA noted that stroke risk is more closely related to abdominal obesity than general obesity (which is reflected in BMI).82 Thus, it can be concluded that while generally maintaining a healthy weight is important, focusing on healthy body composition to avoid abdominal obesity may be particularly pertinent for reducing stroke risk.
For a comprehensive discussion of weight management strategies, please see Life Extension’s “Weight Management” protocol.
Healthy Diet
The ASA recommends a heart-healthy diet to reduce stroke risk. High-fat diets can increase cholesterol levels and high sodium intake is associated with elevated blood pressure, both of which increase the risk for stroke.291 Diets rich in fruits, vegetables, nuts, and olive oil, on the other hand, reduce the risk for stroke.12 Examples include the Mediterranean and DASH (Dietary Approaches to Stop Hypertension) diets, both of which focus on intake of fruits, vegetables, and whole grains, as well as lean sources of protein, such as fish, poultry, and low-fat dairy in moderation.84
In a meta-analysis of data from over 680,000 people in Mediterranean and non-Mediterranean populations, greater adherence to a Mediterranean diet was associated with significant reductions in the risk for both ischemic and hemorrhagic stroke.85 Adherence to the Mediterranean diet is associated with improved endothelial function and blood flow, which are critical for good vascular health.86 Overall, scientific research has found that high adherence to the Mediterranean diet can decrease the risk for stroke by 10‒36%.87
A review of 30 clinical trials involving over 5,500 people revealed that compared with a control diet, adherence to the DASH diet was associated with significant reductions in both systolic (mean, 3.2 mm Hg) and diastolic (mean, 2.5 mm Hg) blood pressure.88 Studies involving a total of over 548,000 individuals found that higher levels of adherence to a DASH diet was associated with an approximately 12% reduction in stroke risk over up to 24 years of follow-up, with the greatest benefits observed among Asian populations.89
A modified version of the Mediterranean and DASH diets, known as the MIND (Mediterranean-Dash Intervention for Neurodegenerative Delay) diet, was developed by faculty at Rush University Hospital in Chicago.90 It also emphasizes fresh produce, whole grains, lean meats, and olive oil, and discourages excess salt consumption. Additionally, it encourages only berries as a fruit; restricts potatoes and dairy; limits fish to one serving per week; and allows eggs. Red meat, processed meats, fried fast foods, sweets and pastries, butter, stick margarine, and whole-fat cheese are all discouraged.91 A study in 106 patients with a history of stroke found that a higher rate of adherence to the MIND diet was associated with slower rates of cognitive decline compared with the lowest levels.92
Exercise
Physical inactivity is a clear risk factor for stroke, while physical activity is known to improve vascular function and protect against stroke risk factors including hypertension, obesity, and type 2 diabetes. Because of the long duration that would be needed for randomized controlled trials to definitively prove that exercise prevents a first stroke, epidemiologic and observational trials provide most of the evidence for the role of physical activity in stroke prevention.93
In an observational study in nearly 3,300 adults, moderate- to high-intensity physical exercise was associated with a 35% reduction in stroke risk.54 In a study of over 70,000 Chinese adults with a history of ischemic stroke, TIA, ischemic heart disease, or hypertension, cardiovascular deaths were less frequent among individuals who were more physically active.94 In a meta-analysis of 26 studies, being physically active, as assessed using metabolic equivalent (MET) minutes and taking into account all types of physical exertion throughout the day, was associated with lower ischemic stroke risk. In the study, even those with a low physical activity level, reaching 600–3,999 metabolic equivalent (MET) minutes per week, had a 16% lower ischemic stroke risk than physically inactive individuals. A moderately physically active lifestyle (4,000–7,999 MET min/week) was associated with a 19% lower risk and a highly physically active lifestyle (8,000 MET minutes/week or more) was associated with a 26% lower risk.95 Regular physical activity promotes not only weight loss but also good metabolic health, both of which help reduce the risk for stroke.292
Adults should strive to move more and sit less during the day; even small amounts of physical activity can result in considerable health benefits. For even more health benefits, adults should try to do at least 150‒300 minutes per week of moderate-intensity physical activity or 75‒150 minutes of vigorous-intensity aerobic activity. These activities should be spread throughout the week, and additional physical activity can result in more health benefits.
Lack of physical activity is common among stroke survivors, and exercise and structured physical activity play an essential role in recovery and rehabilitation from stroke. Both aerobic and strength training exercise are indicated for stroke recovery. The AHA and ASA have endorsed exercise training for stroke survivors to improve functional capacity and the ability to perform regular daily activities, as well as quality of life.96 Post-stroke rehabilitative exercise can also aid in improving cognitive ability, psychosocial aspects of recovery, balance, and mobility.97 The promotion of physical activity in stroke survivors should emphasize a reduction in sedentary behavior; muscle-strengthening; and low- to moderate-intensity aerobic exercise. Stretching and flexibility training are also indicated.96,97
Oral Health/Oral Hygiene
Poor oral health and hygiene have been associated with an increased risk of various ailments such as cardiovascular disease.293 Multiple studies have also observed a correlation between poor oral health and higher risk of stroke, which is thought to arise from local infection, oral microbiome dysbiosis, and addition to local and systemic inflammation.294,295 A cohort study identified that individuals with periodontitis, compared to gingivitis, had a higher risk of ischemic stroke and a lower survival rate over a 10-year follow-up period; however, this risk was reduced following integrative dental care.296
The large-scale Atherosclerosis Risk in Communities (ARIC) study examined the relationship between home use of dental floss and incident stroke and A-fib in 6,278 participants without prior history. Among the 65% of participants who reported flossing, 4,092 had not experienced a stroke and 4,050 had not been diagnosed with A-fib. During the 25-year follow-up, 434 participants experienced a stroke and 1,291 participants developed incident A-fib. Flossing was associated with a 22% reduced risk of ischemic stroke, 44% reduced risk of cardioembolic stroke, and 12% reduced risk of A-fib, independent of regular tooth brushing and routine dental visits. A greater reduction in stroke risk was observed with increased frequency of flossing.297 An earlier analysis of 6,326 individuals from the same cohort found that people with one or more cavities had a 90% increased risk of incident ischemic stroke compared to those without cavities.298
Management of Atrial Fibrillation
Atrial fibrillation (A-fib) is a condition characterized by an abnormal heart rhythm that can lead to clot formation and stroke. Studies have found that 20‒30% of ischemic stroke patients have A-fib. Unfortunately, many of these patients are not diagnosed with A-fib until after a stroke has already occurred.98 At that point, proactive management of stroke risk is still needed as more than one in five people with A-fib who experience a stroke will have another stroke within five years.99 Assessment of stroke and bleeding risk using validated tools (CHA2DS2-VASc score and HAS-BLED score, respectively) are needed to assess the proper course of treatment.98 A meta-analysis of 29 randomized controlled trials determined that the use of warfarin or antiplatelet agents was associated with a 64% or 22% reduction, respectively, in total stroke risk in individuals with A-fib.100 Warfarin or other vitamin K antagonists have long been standard therapy for A-fib, though newer direct oral anticoagulants (DOACs) are rapidly becoming first-line therapy.98 According to the results of an analysis of 35 studies involving over 2 million A-fib patients, bleeding side effects occur less frequently with DOAC use compared with warfarin use.101 A study involving over 56,000 patients with A-fib found that use of a DOAC was associated with a 33% lower risk for major bleeding events, as well as a 36% lower risk for ischemic stroke or systemic embolism compared with warfarin.102
Avoid Excessive Alcohol Consumption
The effects of alcohol on stroke risk and other cardiovascular diseases is complex. Heavy alcohol consumption (≥14 drinks/week) is associated with a number of factors that may promote the occurrence of stroke, including inflammation, oxidative stress, increased lipid levels, and elevated blood pressure.103 Additionally, both heavy and moderate alcohol consumption (7‒13 drinks/week) have been identified as significant risk factors for hypertension.104 However, while heavy alcohol intake and binge drinking have a negative effect on stroke risk, low-to-moderate alcohol consumption may be protective against stroke.103 Avoiding excessive amounts of alcohol should be considered a component of stroke prevention interventions. The effects of moderate alcohol intake are unclear, but low alcohol consumption potentially provides beneficial effects.
Lipid-lowering Therapy
Use of a statin to lower cholesterol levels may reduce the risk for recurrent stroke, as well as cardiovascular events. Some, but not all, studies of acute statin administration for ischemic stroke have shown improved outcomes and good safety.105-110 As of this writing it is reasonable to begin statin medication as soon after acute ischemic stroke as is deemed safe and to avoid discontinuing statins after acute ischemic stroke.110-113
6 Nutrients
In addition to the interventions described in this protocol, readers may also want to review the Life Extension protocols on Blood Clot Prevention, Cardiovascular Disease, High Blood Pressure, and Arrhythmias.
Magnesium
Magnesium is a mainly intracellular ion that is crucial for cellular energy production and function. Along with other ions, it helps control nerve and muscle cell activation, and is needed for vascular and neuronal health. Low magnesium levels are common in older people due to lower intake, reduced absorption, and increased excretion in urine. Numerous studies have linked poor magnesium status with a wide range of chronic and age-related disorders, including cardiovascular disease, metabolic syndrome, high blood pressure, and stroke.114
A meta-analysis of 15 observational studies with a combined total of 692,998 participants found people with the highest magnesium intake had a 12% lower risk of ischemic stroke than those with the lowest intake. It was estimated that for every 100 mg of additional magnesium intake a day, the risk for both ischemic stroke and total stroke was reduced by 2%. Magnesium intake was not associated with risk of hemorrhagic stroke in eight studies analyzed.115 Nevertheless, a study that included 79,429 participants found those with higher predicted serum magnesium levels based on genetic profiles had a lower risk of hemorrhagic stroke.116 In other studies, low magnesium status was correlated with increased risk of cerebral hemorrhage following intravenous thrombolytic therapy and post-stroke cognitive impairment in ischemic stroke patients.117,118
A randomized controlled trial included 291 ischemic or hemorrhagic stroke patients who were given either regular sodium-based salt, a potassium-enriched salt, or a magnesium- and potassium-enriched salt to use at mealtimes over the subsequent six months. The intent was to increase magnesium and potassium intake to Daily Recommended Intake levels and reverse possible deficiencies. Compared with those given regular sodium-based salt, those given the magnesium/potassium salt were more than twice as likely to have good neurological performance and improved functional outcome at the end of six months.119
Magnesium may also have a role in acute treatment of some types of stroke. A controlled trial in 36 acute ischemic stroke patients with A-fib being treated with the antiarrhythmic drug amiodarone (Cordarone) found intravenous magnesium sulfate infusions every 24 hours for five days resulted in lower levels of inflammatory markers (eg, C-reactive protein, interleukin-8 [IL-8]), improved levels of immunological and neurological indicators, and reduced disability, indicating a possible attenuation of known adverse side effects of amiodarone.120 In general, however, intravenous magnesium sulfate has not been found to significantly improve outcomes in patients who have experienced ischemic stroke.121,122
It has been proposed that magnesium administration directly into the cerebrospinal fluid may be effective for quickly delivering magnesium to the affected tissues in acute stroke patients, allowing for synergistic approaches with other therapeutic methods such as hypothermia or intravenous magnesium supplementation.123 In a randomized controlled trial in 37 patients with severe subarachnoid hemorrhage, magnesium sulfate infusions (2.5 mg/mL at 20 mL per hour) into the cerebrospinal fluid continuously for 14 days after the hemorrhage delayed cerebral ischemia and resulted in improved clinical outcomes and fewer complications. In addition, intravenous hydrogen therapy was found to enhance the benefits of magnesium in this trial.124
Olive Oil and Olive Extracts
The olive (Olea europaea) is a staple in the diet of many Mediterranean cultures, and olive oil is a primary source of added fat in the Mediterranean diet.125 Olive oil consumption has demonstrated beneficial effects on blood pressure control.126 The benefits of olive oil are attributable in part to its fat content, which primarily consists of healthy monounsaturated fat.126 A 2011 study examining the incidence of stroke among 7,625 older subjects during a median of 5.25 years of monitoring found that people with the highest levels of olive oil use had a 41% lower risk for stroke compared with those who never used olive oil.127 In a meta-analysis of cohort studies examining the association between olive oil intake and stroke risk, each 25 gram increase in olive oil consumption per day was associated with a 24% reduction in the risk of stroke.128
Olive extracts may also play a role in stroke prevention. In a 2008 study involving 40 borderline hypertensive monozygotic twins, supplementing food with 1,000 mg olive leaf extract daily for eight weeks was associated with significant reductions in blood pressure.129 In a gerbil model of ischemic stroke, pretreatment with 100 mg/kg olive leaf extract resulted in reduced damage to the hippocampal region of the brain up to 24 hours after ischemia, potentially due to its antioxidant activity.130
In addition to healthy fats, several compounds in olive oil have been investigated for their neuro- and cardioprotective activity. Hydroxytyrosol, a phenol found in olive oil, exhibits antioxidant activity and acts as a metal chelator.131 In mouse models of ischemic stroke, mice fed a hydroxytyrosol-enriched diet had better grip strength, improved short-term memory, enhanced expression of neural growth factors, and increased presence of anti-inflammatory immune cells in the affected area of the brain compared with control mice, but effects on cerebral blood flow have been inconsistent.132,133 Oleuropein, which is also found in olive oil, has both antioxidant and anti-inflammatory activity.131 In rodent models of ischemic stroke, oleuropein treatment has been found to be protective against neuronal cell death and was associated with significant improvements in cognitive function after stroke.134-136
Maslinic acid, an olive constituent, may also play a neuroprotective role subsequent to stroke. In a mouse model of ischemic stroke, administration of maslinic acid (up to 10 mg/kg per day) for seven days after cerebral ischemia was associated with the development of new synaptic connections and regeneration of neurons in the brain.137
Omega-3 Fatty Acids
The AHA recommends a diet that emphasizes a variety of fish, especially those that are high in omega-3 fatty acids, for heart health and stroke risk reduction.138 Omega-3 polyunsaturated fatty acids, notably eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA), exhibit a host of protective benefits that could be expected to lower risk of stroke, including anti-inflammatory and cholesterol-balancing properties. They also help protect against oxidative stress and promote neuron regeneration and revascularization after stroke.139 Epidemiologic studies have found that lower blood levels of omega-3 fatty acids (a lower “Omega-3 Index”) are associated with increased risk for stroke and other neurological conditions, when compared to an optimal Omega-3 Index. Similarly, a review of clinical trials found EPA and DHA supplementation is more effective in those with low omega-3 status, and the use of blood tests to target supplementation decisions may lead to greater stroke prevention.140 A meta-analysis of 10 studies involving over 20,000 people aged 35 to 79 years found that higher levels of circulating DHA were associated with a 22% reduction in stroke risk. Each 1% higher increment of DHA was associated with an 11% reduced risk of stroke. These results applied to protection from ischemic stroke only; no association was found with hemorrhagic stroke risk.141 A randomized controlled trial of 4 grams of isolated EPA per day in high-risk patients taking statins, followed for 4.9 years, found a 37% reduction in incidence of stroke.142
Maintaining a healthy omega-6/omega-3 ratio after stroke may also be associated with improved outcomes. In a study of 25 older stroke survivors, a higher omega-6/omega-3 ratio was associated with greater physical dysfunction as well as insulin resistance compared with an optimal ratio.143
A prospective observational study of nearly 80,000 women in the United States found those who consumed fish, which is high in omega-3 fatty acids, two to four times per week had a 48% lower risk of thrombotic stroke, and those who ate fish five or more times per week had a 70% lower risk of thrombotic stroke, while hemorrhagic stroke risk was unchanged.144 Another study in over 43,500 U.S. men found that even once monthly fish consumption was associated with a 44% reduction in risk of ischemic stroke.145 A meta-analysis of 17 cohort studies involving over 672,000 people found that higher fish consumption was associated with a 13% reduction in stroke risk and 19% reduction in risk for ischemic stroke. However, while higher omega-3 fatty acid intake was associated with a 21% reduction in risk for stroke in women, in this meta-analysis, no association between omega-3 intake and stroke risk was observed in men.146
Some studies of omega-3 fatty acid supplementation have reported protective effects against cardiovascular disease, but several that have included stroke as one component of multi-outcome endpoints have reported no effect, even among high-risk individuals.147-150 High-quality randomized controlled trials examining the effect of omega-3 supplementation on stroke risk as a primary outcome are urgently needed.148 Tools such as the Omega-3 Index that measure blood levels of omega-3 fatty acids can help guide supplementation and dietary modification; individuals with sub-optimal Omega-3 Index scores can modify their supplementation and dietary regimens appropriately. Life Extension encourages most people to achieve an Omega-3 Index score of 8% or greater.
Flavonoids
Flavonoids, naturally occurring substances found in fruits, vegetables, grains, tea, and wine, have antioxidant and anti-inflammatory properties.151 A 2016 meta-analysis of 11 studies involving over 356,000 individuals found that, compared with the lowest dietary intake of flavonoids, those with the highest intake had a stroke risk reduction of 11%. Additionally, for every 100 mg increase in dietary flavonoid intake, there was a 9% decrease in relative risk for stroke.152 The AHA recommends a diet rich in flavonoid-dense foods, including fruits, vegetables, and whole grains—foods that also characterize the Mediterranean and DASH dietary patterns.138
Flavanones, a type of flavonoid found in citrus fruits, may be of particular interest in stroke prevention as a study of over 69,000 women found that the highest levels of flavanone consumption were associated with a 19% lower risk for ischemic stroke.153 Another study in over 20,000 U.S. adults found that, over 6.5 years, flavanone and citrus fruit/juice intake were inversely correlated with incidence of stroke, an association not observed for other flavonoids.154
Folic Acid and B Vitamins
Homocysteine is an amino acid made in the body from a common dietary amino acid, methionine. High levels of homocysteine damage the endothelial lining of blood vessels, and are associated with a two- to three-fold increased risk of cardiovascular disease, including stroke.155 Supplementation with B vitamins, including folic acid (vitamin B9), reduces the amount of homocysteine in the blood and helps protect against stroke.57,60 Meta-analyses of multiple clinical trials and studies concluded that folic acid supplementation was associated with a 10‒15% reduced risk for stroke compared with not receiving folic acid supplementation.156-159 One meta-analysis that included data from eight randomized controlled trials with a combined total of 8,513 participants found B vitamin supplementation (B6, B9, and B12) lowered stroke risk by 13%. In seven of eight trials, the dose of folic acid was 2 mg per day, whereas one trial supplemented with 2.5 mg per day. In all eight trials, B6 was 25 mg per day and B12 was 0.5 mg per day.159 Findings from another meta-analysis suggested daily doses of folic acid under 2 mg may be more effective than higher doses.157
Supplementation with other B vitamins may also be protective against stroke. Results from a 2015 analysis of 17 trials involving over 86,000 patients found folic acid plus vitamin B6 provides better protection against stroke than folic acid alone.160 Additionally, research suggests B vitamin supplementation after stroke reduces the risk for recurrent stroke by nearly one-third.161
Nattokinase
Nattokinase is an enzyme extracted from natto, a traditional Japanese food made by fermenting soybeans with the bacterium Bacillus subtilis. Nattokinase supplementation has been shown to reduce cardiovascular risk factors, and natto consumption has been linked to reduced cardiovascular disease mortality, particularly a decreased risk of mortality from ischemic heart diseases.299,162 In preclinical and clinical studies, nattokinase has been shown to aid in reducing blood viscosity and dissolving clots. It has also demonstrated lipid- and blood pressure-lowering activity, as well as neuroprotective effects.299,163 A study using an animal model of stroke indicated nattokinase reduced inflammatory signaling, oxidative stress, and coagulation factors, and decreased neuronal injury and stroke severity.300
In a randomized controlled trial in 61 stroke patients, 1,200 fibrinolytic units (FUs) of nattokinase alongside standard post-stroke treatment for 60 days resulted in greater improvement in stroke symptoms and physical functioning, blood pressure control, lipid profiles, and quality of life compared with standard treatment alone. Interestingly, the control group exhibited significant improvements from baseline, but nattokinase potentiated these effects.163
An observational study compared long-term outcomes in 191 patients following stroke or transient ischemic attack: 96 participants were given 160 mg/3,000 FUs of nattokinase per day in a product that also contained hydroxytyrosol (a phenolic compound from olives) and 95 received antithrombotic medications (aspirin or clopidogrel) as preventive therapy. After six months, there were no significant differences in incidences of cerebrovascular or cardiovascular events or adverse reactions.301 The same research group reported 12 months of nattokinase therapy, at 3,000–4,000 FUs daily, in 129 patients following stroke or transient ischemic attack was associated with lower blood pressure in men and women and improved cognitive performance in men.302 The findings suggest nattokinase may have a role in preventive therapy following a stroke or transient ischemic attack.
Safety note: Cerebral hemorrhaging was reported in a patient concomitantly using aspirin and nattokinase for secondary stroke prevention.167 Therefore, a risk assessment by a healthcare provider is warranted before individuals taking an antithrombotic agent initiate nattokinase supplementation.
Garlic
Components of garlic have many properties associated with heart health and exhibit a variety of antioxidant and anti-inflammatory effects that protect against atherosclerosis and hypertension.168 According to the results of meta-analyses of studies of garlic supplementation, use of garlic supplements was associated with an average 5.1 mm Hg reduction and 2.5 mm Hg reduction in systolic and diastolic blood pressure, respectively, and may help support reduction in cholesterol levels.169,170
In a study of 125 Chinese individuals with a history of stroke, greater daily garlic intake was associated with improved measures of endothelial function and blood flow, suggesting regular garlic consumption after stroke may help protect against future atherosclerotic events.171 In a 2015 study in a rat model of ischemic stroke, rats injected with 50 mg/kg allicin, a bioactive garlic constituent, every three hours had reduced infarct size, brain edema, and neural cell death.172
Vitamin D
Vitamin D plays a role in lipid metabolism and development of atherosclerosis.173 Supplementation may help lower blood pressure in those with vitamin D deficiency, and in the elderly.174 A 2018 analysis of 19 studies from multiple populations found that lower vitamin D status was associated with an over 2-fold increased risk for ischemic stroke, though no association was found for hemorrhagic stroke.175 A 2019 population-based study involving over 9,300 individuals found that, while no association with low vitamin D status was observed, severe vitamin D deficiency was associated with a 25% increased risk for stroke.176 Additionally, a study of 982 Chinese ischemic stroke patients found that vitamin D deficiency is common in individuals recovering from ischemic stroke, particularly women and those with more severe stroke.177 However, not all data indicates a role for vitamin D as a meta-analysis of randomized controlled trials that included over 83,000 individuals did not find a cardiovascular benefit for vitamin D supplementation.178
In a study of 240 patients with ischemic stroke almost 63% had severe vitamin D deficiency, and the incidence of death after stroke was over 2.5 times higher among individuals with severe vitamin D deficiency compared to those without severe deficiency.179 A randomized controlled trial of 53 ischemic stroke patients with low vitamin D levels (<75 nmol/L) found that compared with conventional care alone, intramuscular injection of vitamin D3 (600,000 IU) followed by daily calcium (1 gram) and once-monthly vitamin D3 (60,000 IU) supplementation for six months was associated with a 90% higher likelihood of a positive outcome.180 These results suggest post-stroke vitamin D supplementation may be beneficial for some individuals, although more research is needed.177,179,180
L-carnitine
L-carnitine is an essential cofactor in the metabolism of lipids into cellular energy.181 In a rat model of ischemic stroke, L-carnitine demonstrated a neuroprotective effect against tissue damage caused by oxygen deprivation.182 In another rat model of ischemic stroke, pretreatment with acetyl-L-carnitine was associated with a decrease in infarct size and prevention of ischemic damage in neural cells.183
A 2019 prospective randomized controlled trial in 100 patients with middle cerebral artery ischemic stroke examined the use of 1 gram per day of oral L-carnitine supplementation in combination with fat emulsion therapy, a key component of nutritional support following stroke that requires large amounts of energy to metabolize. When used in conjunction with standard ischemic stroke treatment, L-carnitine plus fat emulsion therapy resulted in significant reductions in S100B, a biomarker of cellular damage and brain cell damage in particular, suggesting carnitine could be neuroprotective in humans.184
N-acetylcysteine
N-acetylcysteine (NAC) is an amino acid derivative with potent antioxidant activity.185 In a randomized controlled trial involving 68 ischemic stroke patients, oral NAC supplementation, at a dose of 4 grams over 48 hours initiated within 24 hours of stroke, was associated with a significantly lower rate of cognitive deficit at 90 days after stroke.186 Additionally, in a randomized controlled trial in 123 patients with intracranial hemorrhagic stroke, medical researchers examined the effects of daily intravenous injections of 1,000 mg NAC twice daily and 800 mcg selenium twice daily on outcomes after stroke compared with placebo injections. After two weeks, NAC/selenium treatment was associated with a significant reduction in hematoma size, and length of intensive care unit stay was reduced from an average 12.7 days to 6.5 days.187
However, in a single-blinded placebo-controlled trial involving 62 ischemic stroke patients, intravenous NAC infusions of 100 mg/kg upon admission followed by 10 mg/kg/hour for 10 hours was not associated with any measured benefits in clinical and laboratory profiles compared with standard therapy.188 Further research is needed to understand the effects of NAC treatment on stroke outcomes.
Saffron Extract
Saffron (Crocus sativus) is a culinary and medicinal herb that is rich in carotenoid pigments, including crocin and crocetin, that confer a distinctive yellow color and antioxidant properties. Saffron extracts have demonstrated antioxidant, anti-inflammatory, neuroprotective, and antihypertensive effects.189,190 Findings from multiple animal studies suggest saffron and its active constituents may protect against brain injury due to ischemic and hemorrhagic stroke.191-194
In a randomized controlled trial in 40 acute ischemic stroke patients, those who received 400 mg of saffron extract daily (200 mg twice/day) along with routine stroke care had reduced severity of stroke symptoms after four days compared with those who received routine care alone.195 In another controlled trial, 19 acute ischemic stroke patients received routine stroke care plus 200 mg saffron extract per day and 20 received routine care alone for three months. During the first four days of the trial, stroke severity was decreased and levels of brain-derived neurotrophic factor (BDNF, a protein that encourages brain cell growth and repair) were increased in the saffron treated-group relative to the routine care group; furthermore, at the end of three months, those who received saffron had lower disability scores and higher functional independence.196
French Maritime Pine Bark Extract (Pycnogenol)
French maritime pine bark extract (Pycnogenol) is a polyphenolic compound with strong free radical-scavenging effects. Multiple clinical trials have demonstrated its beneficial effects on cardiovascular, metabolic, and brain health.197,198 In animal research, Pycnogenol has been shown to exhibit anti-inflammatory properties, protect brain tissue from damage caused by ischemia, and attenuate oxidative stress following the return of blood flow (reperfusion) after ischemia.199,200
In a randomized controlled trial, 184 participants were randomly assigned to receive either standard care (including diet and lifestyle instructions to control cardiovascular risk factors); standard care plus 100 mg aspirin per day; or standard care plus 100 mg aspirin, 150 mg Pycnogenol, and 450 mg gotu kola (Centella asiatica) extract per day for three years. At the end of the trial, those in the aspirin/Pycnogenol/gotu kola group had less progression of atherosclerosis and fewer cardiac events (stroke and heart attack) than the other two groups.201
Lutein and Other Carotenoids
Lutein, a prominent carotenoid found in green leafy vegetables, egg yolks, and some fruits, has potent antioxidant effects. Lutein has often been examined for its role in visual health, but preclinical evidence also suggests lutein and related carotenoids, such as astaxanthin, may reduce brain damage related to stroke.202-205 A review of 24 meta-analyses found increased green leafy vegetable intake is correlated with lower risks of stroke, heart disease, and mortality.206 One meta-analysis that included data from 67 studies found higher intake and higher blood levels of lutein were both associated with better cardiovascular and metabolic health parameters, including lower risk of stroke, compared to those with lower levels or intake of lutein.207 Furthermore, a systematic research review found high dietary intake of several carotenoids, including lutein, zeaxanthin, astaxanthin, lycopene, α-carotene, and β-carotene, were associated with reduced risk of stroke.208 Clinical trials are needed to verify these observations.
Protein Supplementation
Early clinical data indicate protein supplementation may be beneficial for improving outcomes in patients with a history of stroke who were in an exercise training program. In a pilot study, 20 people with long-term impairments after a stroke underwent eight weeks of cycling ergometric training. The participants received either 20 grams of a protein-rich supplement or a calorie-matched carbohydrate-rich supplement. The protein-supplemented group reached greater aerobic capacity, functional improvements, and total lean mass versus fat mass.209 Additional studies are needed to confirm the benefit of protein supplementation on functional outcomes in patients with stroke.
7 Medical Treatment of Stroke
A rapid response is critical when a stroke occurs to minimize the resulting damage. The current medical standard for ischemic stroke therapy emphasizes treatment within 4.5 hours of stroke for the greatest likelihood of survival and reduced risk for disability.8,9,210,211
Data from the AHA revealed 64% of stroke-related deaths occur outside of acute hospital care, and many people who do not make it to a hospital in time suffer irreparable damage to the brain.9,12 If possible, it is best for stroke victims to be treated at a care center or hospital unit that specializes in treatment of stroke. A 2020 meta-analysis of 29 trials including almost 6,000 stroke victims found that those treated at a stroke unit, as opposed to an alternative—usually a general care ward—had a 23‒25% lower risk for death or poor outcomes after one year.212
Long-term care following stroke includes both secondary stroke prevention and management of medical complications associated with stroke (see “Outcomes and Complications of Stroke”).213,214
Evaluation and Initial Assessment
When a person is admitted to the hospital for stroke, clinicians will work quickly to stabilize the patient and evaluate their stroke. Initial evaluation of stroke involves113:
- Assessment of respiration and vital signs. The healthcare team will work to ensure the airway is open and breathing and circulation are stable. Hypoventilation (shallow or slow breathing) can lead to elevated levels of carbon dioxide in the blood, which can lead to dilation of blood vessels and increased intracranial pressure. Supplemental oxygen or ventilation may be needed for patients with poor respiration.113
- History and physical. A history will be obtained and a physical exam performed to determine what symptoms are occurring and when they started. These will also be used to determine a potential differential diagnosis.113
- Neurologic evaluation. A comprehensive neurologic evaluation will be performed to confirm the results of the history and physical and assess severity of the stroke.112,215
- Laboratory evaluations. Other tests, including an electrocardiogram and assessment of oxygen saturation, blood clotting factors, and blood sugar levels, will be performed.112 Electrocardiography is especially important to determine if underlying cardiac abnormalities may have caused a stroke.113
- Imaging. Brain, head, and neck imaging will be used to evaluate the type of stroke and location of the obstruction. For most patients, a non-contrast computed tomography (CT) scan or magnetic resonance imaging (MRI) can successfully distinguish between an ischemic and hemorrhagic stroke. For people who present greater than 4.5 hours after the onset of symptoms or who wake up with symptoms and are unable to estimate when a stroke may have occurred, additional imaging may be required.112
Management of Ischemic Stroke
For ischemic stroke victims who arrive for treatment within 3 to 4.5 hours of the onset of stroke, current treatment guidelines recommend the immediate use of alteplase (Activase) or tissue plasminogen activator (tPa), commonly referred to as intravenous thrombolysis (IVT).9,112 IVT uses enzymes that break up and dissolve blood clots in order to reestablish blood flow. The use of IVT is associated with better outcomes for ischemic stroke patients, including reduced risk for death, disability, and need for long-term care.8,9 A meta-analysis of three clinical trials found IVT may also improve outcomes if used within nine hours of stroke for those who wake up with stroke symptoms.211
For patients with obstructions in large arteries who arrive for emergency treatment within 24 hours, mechanical thrombectomy may also be used.112,113,216 In a mechanical thrombectomy, a specialized device is threaded through the blood vessels to the site of the stroke-causing clot, which then removes as much of the clot as possible.216 Eligibility for mechanical thrombectomy is based on a number of factors, including size and accessibility of the blood clot.112,216 Mechanical thrombectomy is not used as frequently as IVT, as only about 10% of patients are eligible, and most hospitals outside of stroke centers do not have the specialized equipment or expertise to perform this procedure.217
Current treatment guidelines from the AHA/ASA recommend that, for those eligible for mechanical thrombectomy, IVT may still have benefits if administered within the appropriate time frame.112 IVT may resolve the blood clot quickly in the time it takes to prepare patients for mechanical thrombectomy, or may help dissolve enough of the clot such that it is easier to remove mechanically. A review of studies involving the timing of mechanical thrombectomy demonstrated that outcomes are most promising when treatment is initiated early, and delays are associated with increasing likelihood for disability and death.218 Additionally, older age (≥80 years) has been identified as a predictor of poor outcomes after mechanical thrombectomy.12
Treatment of very high blood pressure is also often a component of ischemic stroke management.3,19 Interestingly, low blood pressure after stroke has also been linked to worse outcomes, possibly due to decreased blood flow within the brain. Some evidence suggests there is a U-shaped relationship between blood pressure and stroke outcomes: people with both very low and very high blood pressure are at increased risk for death and disability after stroke.219
In patients who are eligible for IVT or mechanical thrombectomy, blood pressure treatment is often used to maintain a systolic blood pressure <185 mm Hg and a diastolic blood pressure <110 mm Hg.112 In patients with excessively high blood pressure (≥220/120 mm Hg) who do not receive IVT or mechanical thrombectomy, it is unclear if antihypertensive treatment provides any clinical benefit, but lowering blood pressure by 15% during the first 24 hours after a stroke is considered a reasonable goal.215
Because ischemic strokes are inherently caused by the aggregation of platelets, antiplatelet therapy is a key component of acute ischemic stroke management. Aspirin is most often used, which should be started within 24 to 48 hours after the onset of stroke. However, it is not a substitute for acute treatment with IVT or mechanical thrombectomy.215 A 2014 meta-analysis of eight clinical trials composed of over 41,000 patients found that initiation of aspirin within 48 hours of ischemic stroke onset reduced the risk for death or disability by 5%.220 A 2016 meta-analysis of 12 trials involving almost 16,000 patients studied the use of aspirin to reduce the risk for a second stroke after TIA or ischemic stroke. The analysis found that, in the first six weeks after trial randomization, aspirin reduced the risk of recurrent ischemic stroke by 58% and the risk for a fatal or disabling stroke by 71%. Some additional benefit was noted in the period of 6‒12 weeks, but none after 12 weeks. The greatest benefits were observed in people who experienced a TIA or minor stroke (a stroke with mild but persisting symptoms).221 Early short-term dual antiplatelet therapy with aspirin and clopidogrel (Plavix) is indicated to reduce the risk in select TIA or minor stroke patients.60
Management of Hemorrhagic Stroke
Hemorrhagic stroke is inherently different than ischemic stroke and requires a different approach to treatment. Whereas the goal of ischemic stroke treatment is to disrupt the blockage of the affected blood vessel, emergency treatment of hemorrhagic stroke is focused on controlling bleeding and pressure in the brain. Hemorrhagic stroke cannot be distinguished from ischemic stroke based on clinical presentation alone, and neuroimaging with MRI or CT scan is thus required as an initial step in management.222
Use of oral anticoagulants or antiplatelet therapy is associated with increased risk for hemorrhagic stroke. These agents work to prevent blood clots, which can also increase the risk for bleeding. Up to one in five people who experience intracranial hemorrhaging are taking an oral anticoagulant.213 Prompt discontinuation of antiplatelet and anticoagulant therapy should be undertaken immediately. For people taking the anticoagulant warfarin or another vitamin K antagonist, intravenous vitamin K, intravenous protamine sulfate, and other clotting factors are used to reverse the effects of treatment.223 Non-vitamin K oral anticoagulants, also known as direct oral anticoagulants (DOACs), are associated with reduced risk for hemorrhagic stroke compared with warfarin.213,223 However, increased risk of bleeding may still occur with these medications, but newer agents to reverse their anticoagulant effects, with varying effectiveness, are available.223,224
As with ischemic stroke patients, blood pressure management is an important aspect of hemorrhagic stroke treatment. This may be achieved using beta-blockers (labetalol or esmolol [Brevibloc]), an angiotensin-converting enzyme (ACE) inhibitor (enalapril [Vasotec]), calcium channel blocker (nicardipine [Cardene]), or vasodilator (hydralazine).41 In the 2010 INTERACT study, early and intensive antihypertensive treatment significantly reduced the growth of brain hematomas during intracerebral hemorrhage over the course of 72 hours.225 Reduction of systolic blood pressure to 140 mm Hg is generally considered safe and is recommended to improve functional outcomes. For patients with a systolic blood pressure over 220 mm Hg, more aggressive antihypertensive treatment is needed.213,223
Managing intracranial pressure is another vital consideration in management of acute stroke. For patients requiring intervention to reduce this pressure, a number of strategies can be used, including elevating the head to a 30-degree angle, administration of oxygen, mild sedation, and osmotic therapy (mannitol, hypertonic saline), which can help reduce and redistribute fluid buildup around the hematoma.223,226 Under some conditions, ventricular catheterization may be used to monitor intracranial blood pressure, which can also be used to drain fluid buildup or deliver medication if needed.226
Management of Post-stroke Complications
Venous thromboembolism (VTE). Prevention of future DVT and VTE is complicated in stroke, as the risks for both clotting and bleeding are high. Over one in 10 patients experience DVT or VTE after stroke, including 13% of hemorrhagic stroke victims, so blood clot prevention measures are needed.226,227 Mechanical therapy with an intermittent pneumatic compression device, compression socks, and/or a venous foot pump are recommended as soon as patients are discharged. Low-dose heparin may be initiated if the risk for bleeding in ischemic stroke victims is low, or once bleeding has stopped following hemorrhagic stroke.227,228 Patients who are considered at high risk for DVT and VTE may require both pharmaceutical and mechanical DVT prophylaxis.228
If DVT or pulmonary embolism occurs, more aggressive treatment may be needed. Because a second incidence of pulmonary embolism is fatal in up to 88% of cases, oral or intravenous anticoagulant therapy is likely needed if a DVT or pulmonary embolism occurs.213
Dysphagia and pneumonia. Dysphagia is among the most common complications after stroke, occurring in an estimated one-third to three-quarters of stroke victims, depending on diagnostic method. If swallowing difficulties prevent eating, a feeding tube may be needed to support proper nutrition and hydration until symptoms improve.214
Aspiration due to dysphagia can increase the likelihood of developing pneumonia. In fact, the risk for pneumonia is over three times higher in stroke victims with dysphagia compared to those without dysphagia.214,229 Pneumonia is a common complication after both hemorrhagic and ischemic stroke, occurring in an estimated 4‒10% of patients.213,214 Formal screening for dysphagia can reduce the risk for pneumonia by an estimated 90%.230 Speech therapy may also help improve control of swallowing muscles.
Fever. Fever is common after stroke, particularly among hemorrhagic stroke patients.226,231 Approximately half of patients experience a fever after stroke, and one study found that over 90% of hemorrhagic stroke victims with intracerebral hemorrhage experienced a fever (≥99.5°F) for at least a portion of the 72 hours following hemorrhage.231,232 The presence and duration of fever are associated with worse outcomes following stroke, including poor functional outcomes.232 The majority of post-stroke fevers are thought to be infectious in nature, caused by pneumonia or other bacterial and viral infection. Potential noninfectious causes of fever include widespread tissue death and lysis of blood cells following hemorrhage.232 Treatment of fever may include pharmacological treatment, as well as external cooling systems or intravenous cold saline infusions.226,232 Hypothermia treatment (see “Novel and Emerging Strategies” section) may also reduce fever, but is still considered investigational at this time.226
Seizure. Seizures, while relatively uncommon after stroke, may represent an important complication after hemorrhagic stroke in particular. Depending on the location of the hemorrhage, up to one in six people will experience a seizure within a week after hemorrhagic stroke.226 Anti-seizure treatment is used if seizures occur but is not recommended preventively.213,226
8 Outcomes and Complications of Stroke
The damage to the brain caused by a stroke can lead to long-term neurological complications including impaired cognitive function,233 memory loss and dementia, communication challenges, and reduced problem-solving abilities.234 Impaired motor control, including problems with balance, muscle weakness, and even paralysis, are also possible.235 Although some impairment may persist long-term, rehabilitation can help improve outcomes and independence after stroke.236
According to the ASA, about 40% of stroke patients will experience moderate-to-severe impairments and one in 10 stroke survivors will require long-term supportive care. However, about 25% of patients will recover with only minor impairment, and about 10% of stroke survivors will experience complete recovery.237 Most recovery occurs within the first 3‒6 months after stroke, but some patients may continue to experience some cognitive and physical recovery up to 18 months post-stroke.238
Stroke outcomes and long-term effects depend largely on the brain region affected and extent of brain damage. For example, dementia is frequently observed in people who experience strokes in the left hemisphere of the brain, whereas loss of problem-solving abilities are more common in people who have right-brain strokes.234 Because the left hemisphere controls the right side of the body, people who have left-brain strokes are more likely to experience impaired motor function on the right side of their body, and vice versa.235
Other complications of stroke that may require additional treatment include113,214:
- Dysphagia (difficulty swallowing)
- Deep vein thrombosis and pulmonary embolism
- Pneumonia
- Urinary tract infections and incontinence
- Seizures
- Myocardial infarction and other cardiac injury
- Gastrointestinal bleeding
- Sleep-disordered breathing
- Depression
- Fatigue
- Brain edema (swelling)
Paralysis or Impaired Motor Function
After stroke, some people may experience problems controlling their movements or may even experience paralysis. In a study of over 1,200 people recovering from stroke, over 77% experienced upper limb weakness.239 This loss of muscle control can make it difficult to walk or maintain balance and can cause problems with normal body functions. Most recovery of motor function occurs within the first three months after stroke.240 Additionally, the majority of people who survive stroke experience difficulty swallowing, a condition known as dysphagia.241 Dysphagia can make it difficult to eat or drink and may lead to nutritional deficiencies and illness, including pneumonia.
Sensory Disturbances
Stroke victims may experience pain immediately after stroke or within the following weeks to months. In some people, chronic pain may occur as a result of impaired motor function, which can cause stiffness in the joints. Other sensory issues may emerge, including numbness, tingling, or loss of sensation.235 Loss of sensation, combined with impaired motor function and reduced cognitive awareness, can lead to incontinence after stroke.235,242 About half of stroke survivors experience urinary incontinence, and approximately one-third have loss of bowel control.243,244 These symptoms may improve over time, with just 15% of people experiencing continued urinary incontinence one year post-stroke.242,243
Speech Problems
Up to one in three people who have a stroke will experience problems using or understanding language, a phenomenon known as aphasia.245 Aphasia can result from stroke-induced damage to regions of the brain that are responsible for speech and language processing.246 Aphasia can affect a person’s ability to write and speak.235
Cognitive Impairment or Memory Dysfunction
Cognitive impairment occurs within one year in roughly 30% of those who have experienced a first stroke.247 This may affect many mental functions, both simple and complex, including the ability to learn new things or plan ahead, and may impair a person’s attention span, short-term memory, or ability to comprehend others.235,239 Post-stroke cognitive impairment is different from cognitive decline seen in Alzheimer disease in that it is a more abrupt change in cognitive function.248 In addition to cognitive changes, about one in three patients who experience a large stroke have impaired consciousness at the time of stroke, which, in some cases, persists long-term.249,250 More severe impairment of consciousness has been correlated with poorer functional outcomes for stroke patients.250
In some people, most commonly those who have left-hemisphere strokes, reduced blood flow to the brain can result in vascular dementia.251 Compared with the general population, the risk for all-cause dementia is 69% higher for people with a history of stroke.252 The incidence of vascular dementia varies considerably based on the severity of stroke, with an estimated 5% of people experiencing dementia one year after TIA compared with 34% at one year after severe stroke. Secondary stroke prevention measures are considered a cornerstone of vascular dementia prevention as well.253
Emotional Disturbances
Many people who have a stroke experience emotional distress, including anxiety, fear, frustration, anger, sadness, and grief.235 An analysis of 44 studies involving over 5,700 stroke patients found that approximately one-fifth to one-quarter of stroke survivors experience anxiety, which persists up to six months or longer post-stroke.254 The ASA estimates up to 55% of people will experience depression at some point after stroke.255 Post-stroke emotional disturbances can be treated with a variety of interventions, including medication and counseling. Addressing mental and emotional well-being is a key part of recovery after stroke, as anxiety, apathy, and depression have been linked to poor function and outcomes after stroke.256,257
9 Novel and Emerging Strategies
Uric Acid Therapy
Restoration of blood flow following stroke, known as reperfusion, can lead to the generation of oxidative stress in brain tissue.258 Oxidative stress can cause damage to DNA, cells, and tissues.259 Uric acid can neutralize reactive oxygen species (ROS) and has been examined in clinical trials of ischemic stroke.260-262 In a placebo-controlled trial with 411 participants, 1,000 mg intravenous uric acid therapy administered during IVT infusion doubled the likelihood of having an excellent outcome in women compared with IVT plus placebo. An excellent outcome was defined as no post-stroke symptoms, mild symptoms without disability, or no worsening of an existing slight disability. In contrast, uric acid administration in men had no effect on outcome.261 A second analysis of the trial noted that uric acid therapy was associated with reduced infarct growth and improved outcome in a subgroup of patients with the highest blood glucose levels during acute stroke.262 In a randomized controlled trial evaluating 45 people with ischemic stroke who received both IVT and mechanical thrombectomy, 1,000 mg intravenous uric acid improved functional outcome and reduced mortality compared with placebo. No serious safety concerns regarding uric acid therapy were observed in this study.260
Therapeutic Hypothermia
Therapeutic hypothermia has been investigated as a neuroprotective strategy in several conditions, including cardiac arrest263,264 and traumatic brain injury.265,266 This treatment modality involves lowering the body temperature to below normal, typically 89.6°F to 95°F, and is believed to be a powerful neuroprotectant. It has been proposed that this cooling interrupts a range of cellular signaling cascades that result from ischemia and promote edema, inflammation, cell death, and a breakdown of the blood‒brain barrier. Therapeutic hypothermia may more comprehensively address the ischemic cascade that occurs after stroke than other therapies, which typically only address one aspect.267
It is currently difficult to adequately gauge the benefits and effects of therapeutic hypothermia in ischemic stroke. As of the time of this writing studies have often been small, lacked a control group, and used differing cooling methodologies. Perhaps most challenging for the study of therapeutic hypothermia in stroke is that core body temperature is not necessarily indicative of brain temperature, and there is no reliable way to measure brain temperature.267
Taken as a whole, the body of research points to functional improvement with the application of therapeutic hypothermia in ischemic stroke, but with an increased risk of complications.268 These include cardiovascular complications such as heart attack and arrhythmias; increased risk of infection including pneumonia and urinary tract infection, due to immune suppression; abnormal (insufficient) blood clotting; electrolyte imbalances; and insulin resistance.267,269,270 However, as of mid-2021, existing evidence has not demonstrated robust clinically significant effects related to size of infarct, or mortality. More randomized controlled trials with larger sample sizes are needed to determine if and how therapeutic hypothermia fits into the landscape of treatments for ischemic stroke.267
The effects of therapeutic hypothermia in hemorrhagic stroke have been similarly sporadically studied. In a meta-analysis of nine studies, while some results were mixed, researchers found a 60% lower risk of poor outcomes in hypothermia groups. There was also an almost 40% reduction in occurrence of delayed cerebral ischemia, or the delayed development of new neurological symptoms, in patients who received therapeutic hypothermia. No significant differences in adverse outcomes between hypothermia and usual care were found. Although more research is needed, preliminary results suggest therapeutic hypothermia may improve outcomes after hemorrhagic stroke.271
Intravenous Vinpocetine
Vinpocetine is a synthetic derivative of the chemical apovincamine, which is an extract from the leaves of the lesser periwinkle plant. Vinpocetine has been explored widely in a variety of diseases, from cerebrovascular and cognitive disorders to kidney injury and eye conditions. It is associated with a variety of potentially neuroprotective activities, including vasodilation, inhibition of inflammation, and antioxidant properties. Vinpocetine also inhibits sodium channels in the brain, which may prevent excitotoxicity and damage to brain tissue.272 Studies in animal models of ischemic stroke have found that vinpocetine is able to block several aspects of pro-inflammatory signaling within the brain, both within and between neurons.273-276
In a randomized controlled trial involving 60 people with ischemic stroke, individuals who received standard care plus vinpocetine (30 mg intravenously daily for 14 days) experienced smaller growth of secondary lesions and an attenuated inflammatory response compared with those who received standard care alone. They also had improved clinical outcomes in the weeks after stroke, up to three months later.277 Another small trial involving 30 stroke patients found limited evidence of improvement on a standardized clinical status scale three months post-stroke among patients who received intravenous vinpocetine compared with those who received standard of care. However, there was no statistically significant difference in risk of poor outcomes overall at three months.278
Another clinical trial examined the effects of a single vinpocetine infusion (20 mg intravenously in 500 mL of saline for 60 minutes) followed by three months of oral vinpocetine supplementation (10 mg, three times daily) on outcomes in patients with chronic effects from an ischemic stroke. Those given placebo experienced significant reductions in the digit span backwards test (which measures the ability to repeat a string of numbers backwards), while no worsening in test results was noted in those given vinpocetine. Also, researchers observed no significant changes in any other neuropsychological tests performed and no notable side effects with treatment.279
Additional small clinical trials found that intravenous vinpocetine increased cerebral blood flow in stroke patients, but these studies did not assess functional outcomes.280,281
Nerinetide
Nerinetide is a peptide molecule that interrupts signaling pathways in the brain that can lead to neurotoxic tissue damage, potentially via inhibition of intracellular nitric oxide production. Although nerinetide has exhibited neuroprotective activity in animal models of ischemic stroke, results from the 2020 ESCAPE-NA1 randomized controlled trial did not show significant improvement in outcomes in patients after ischemic stroke.282 However, it was later noted that, among participants who did not receive IVT with alteplase, those treated with nerinetide had significantly better outcomes compared with placebo.283 More research is needed to understand the relationship between nerinetide and alteplase, but these preliminary results suggest nerinetide may play a protective role in ischemic stroke for patients who are not candidates for alteplase. No significant differences in occurrence of adverse events were associated with nerinetide use compared with placebo.282
Intravenous Fisetin
Fisetin, a flavonoid with neuroprotective and anti-inflammatory properties, has inhibited inflammation and prevented tissue injury in several animal models of ischemic stroke, including mice,284 rats,285 and rabbits.286 In a randomized controlled trial that included 192 people with ischemic stroke, the addition of fisetin to standard IVT reduced serum levels of inflammatory markers, including C-reactive protein, and dramatically improved treatment outcomes compared with IVT alone. This was observed in patients for whom treatment was started within three hours after the onset of symptoms as well as in patients whose treatment was delayed (3–5 hours after the onset of symptoms). These findings suggest fisetin may prolong the therapeutic window for IVT in ischemic stroke patients from three hours to five hours.287
Hydrogen Gas Inhalation
Hydrogen therapy may have a role as an adjunct therapy to prevent brain injury due to ischemic stroke and reperfusion,288 which is marked by extreme oxidative stress and is a major contributor to neuronal damage after ischemic stroke. Hydrogen has several beneficial effects, including antioxidative, anti-inflammatory, and antiapoptotic effects.288,289 Hydrogen can be administered as an inhaled gas with a concentration of 2–4%, orally in enriched water, or intravenously in enriched saline.288 In acute circumstances, inhalation appears to be the most efficient means of administration.290 Animal research also suggests hydrogen therapy may reduce hemorrhagic stroke-related brain damage and mortality; in an animal model of hemorrhagic stroke hydrogen therapy reduced brain edema and improved nerve function for 72 hours.288
The effect of hydrogen gas inhalation on brain tissue damage and functional outcome was examined in a randomized controlled trial including 50 patients with acute ischemic stroke of mild-to-moderate severity. Half of the participants received standard care plus hydrogen therapy (3% hydrogen gas inhalation for one hour twice daily for seven days) and half received standard care alone. Those who received hydrogen therapy had greater brain tissue recovery, as visualized by MRI, after seven days; after 14 days, the hydrogen-treated group had almost complete resolution of changes at the site of the ischemia, while the control group showed persistent ischemic damage. In addition, those who received hydrogen had better functional recovery during the 14 days of monitoring.290
Disclaimer and Safety Information
This information (and any accompanying material) is not intended to replace the attention or advice of a physician or other qualified health care professional. Anyone who wishes to embark on any dietary, drug, exercise, or other lifestyle change intended to prevent or treat a specific disease or condition should first consult with and seek clearance from a physician or other qualified health care professional. Pregnant women in particular should seek the advice of a physician before using any protocol listed on this website. The protocols described on this website are for adults only, unless otherwise specified. Product labels may contain important safety information and the most recent product information provided by the product manufacturers should be carefully reviewed prior to use to verify the dose, administration, and contraindications. National, state, and local laws may vary regarding the use and application of many of the therapies discussed. The reader assumes the risk of any injuries. The authors and publishers, their affiliates and assigns are not liable for any injury and/or damage to persons arising from this protocol and expressly disclaim responsibility for any adverse effects resulting from the use of the information contained herein.
The protocols raise many issues that are subject to change as new data emerge. None of our suggested protocol regimens can guarantee health benefits. Life Extension has not performed independent verification of the data contained in the referenced materials, and expressly disclaims responsibility for any error in the literature.
- American Stroke Association. Stroke Symptoms. Accessed 4/19/2022. https://www.stroke.org/en/about-stroke/stroke-symptoms
- Campbell BCV, De Silva DA, Macleod MR, et al. Ischaemic stroke. Nature reviews Disease primers. Oct 10 2019;5(1):70. doi:10.1038/s41572-019-0118-8
- Phipps MS, Cronin CA. Management of acute ischemic stroke. BMJ (Clinical research ed). 2020:l6983. doi:10.1136/bmj.l6983
- Collaborators GBDLRoS, Feigin VL, Nguyen G, et al. Global, Regional, and Country-Specific Lifetime Risks of Stroke, 1990 and 2016. The New England journal of medicine. Dec 20 2018;379(25):2429-2437. doi:10.1056/NEJMoa1804492
- Boot E, Ekker MS, Putaala J, Kittner S, De Leeuw FE, Tuladhar AM. Ischaemic stroke in young adults: a global perspective. J Neurol Neurosurg Psychiatry. Apr 2020;91(4):411-417. doi:10.1136/jnnp-2019-322424
- American Stroke Association. About stroke. Updated 2021. Accessed March 3, 2021. https://www.stroke.org/en/about-stroke
- American Stroke Association. Ischemic stroke (clots). Updated 2021. Accessed March 3, 2021. https://www.stroke.org/en/about-stroke/types-of-stroke/ischemic-stroke-clots
- Filho JO, Samuels OB. Approach to reperfusion therapy for acute ischemic stroke. Updated January 26, 2021. Accessed May 4, 2021. https://www.uptodate.com/contents/approach-to-reperfusion-therapy-for-acute-ischemic-stroke
- Centers for Disease Control and Prevention. Stroke treatment. Updated November 14, 2019. Accessed March 3, 2021. https://www.cdc.gov/stroke/treatments.htm
- Ekundayo OJ, Saver JL, Fonarow GC, et al. Patterns of emergency medical services use and its association with timely stroke treatment: findings from Get With the Guidelines-Stroke. Circulation Cardiovascular quality and outcomes. May 1 2013;6(3):262-9. doi:10.1161/CIRCOUTCOMES.113.000089
- Kamel H, Navi BB, Fahimi J. National trends in ambulance use by patients with stroke, 1997-2008. JAMA. Mar 14 2012;307(10):1026-8. doi:10.1001/jama.2012.285
- Virani SS, Alonso A, Aparicio HJ, et al. Heart Disease and Stroke Statistics-2021 Update: A Report From the American Heart Association. Circulation. Feb 23 2021;143(8):e254-e743. doi:10.1161/CIR.0000000000000950
- Wajngarten M, Silva GS. Hypertension and Stroke: Update on Treatment. European cardiology. Jul 2019;14(2):111-115. doi:10.15420/ecr.2019.11.1
- Centers for Disease Control and Prevention. Preventing Stroke: Healthy Living. Updated January 31, 2020. Accessed March 3, 2021. https://www.cdc.gov/stroke/healthy_living.htm
- Centers for Disease Control and Prevention. Preventing Stroke: Control Medical Conditions. Updated January 31, 2020. Accessed March 3, 2021. https://www.cdc.gov/stroke/medical_conditions.htm
- El-Hajj M, Salameh P, Rachidi S, Al-Hajje A, Hosseini H. Adherence to the Mediterranean diet decreases the risk of stroke in the Lebanese population: a case-control study. Pharm Pract (Granada). Jan-Mar 2021;19(1):2157. doi:10.18549/PharmPract.2021.1.2157
- Saraiva JFK. Stroke Prevention with Oral Anticoagulants: Summary of the Evidence and Efficacy Measures as an Aid to Treatment Choices. Cardiology and therapy. Jun 2018;7(1):15-24. doi:10.1007/s40119-018-0106-1
- Centers for Disease Control and Prevention. Atrial fibrilation. Updated September 8, 2020. Accessed March 3, 2021. https://www.cdc.gov/heartdisease/atrial_fibrillation.htm
- Campbell BCV, Khatri P. Stroke. Lancet. Jul 11 2020;396(10244):129-142. doi:10.1016/S0140-6736(20)31179-X
- Biga LM, Dawson S, Harwell A, et al. Arteries Supplying the Head and Neck. In: Anatomy & Physiology: 20.5 Circulatory Pathways. Oregon State University. Data on file.
- Rink C, Khanna S. Significance of brain tissue oxygenation and the arachidonic acid cascade in stroke. Antioxid Redox Signal. May 15 2011;14(10):1889-903. doi:10.1089/ars.2010.3474
- American Association of Neurological Surgeons. Cerebrovascular disease. Accessed March 5, 2021. https://www.aans.org/en/Patients/Neurosurgical-Conditions-and-Treatments/Cerebrovascular-Disease
- Rennert RC, Wali AR, Steinberg JA, et al. Epidemiology, Natural History, and Clinical Presentation of Large Vessel Ischemic Stroke. Neurosurgery. Jul 1 2019;85(suppl_1):S4-S8. doi:10.1093/neuros/nyz042
- Li Q, Yang Y, Reis C, et al. Cerebral Small Vessel Disease. Cell transplantation. Dec 2018;27(12):1711-1722. doi:10.1177/0963689718795148
- Gore M, Bansal K, Asuncion RMD. Lacunar Stroke. https://www.ncbi.nlm.nih.gov/pubmed/33085363
- Kamel H, Healey JS. Cardioembolic Stroke. Circ Res. Feb 3 2017;120(3):514-526. doi:10.1161/CIRCRESAHA.116.308407
- Pillai AA, Tadi P, Kanmanthareddy A. Cardioembolic Stroke. https://www.ncbi.nlm.nih.gov/pubmed/30725675
- Kronzon I, Tunick PA. Aortic atherosclerotic disease and stroke. Circulation. Jul 4 2006;114(1):63-75. doi:10.1161/CIRCULATIONAHA.105.593418
- Petty GW, Khandheria BK, Meissner I, et al. Population-based study of the relationship between atherosclerotic aortic debris and cerebrovascular ischemic events. Mayo Clin Proc. May 2006;81(5):609-14. doi:10.4065/81.5.609
- Panuganti KK, Tadi P, Lui F. Transient Ischemic Attack. https://www.ncbi.nlm.nih.gov/pubmed/29083778
- Lioutas VA, Ivan CS, Himali JJ, et al. Incidence of Transient Ischemic Attack and Association With Long-term Risk of Stroke. JAMA. Jan 26 2021;325(4):373-381. doi:10.1001/jama.2020.25071
- American Stroke Association. What is a TIA. Updated December 20, 2018. Accessed March 5, 2021. https://www.stroke.org/en/about-stroke/types-of-stroke/tia-transient-ischemic-attack/what-is-a-tia
- Hill MD, Coutts SB. Preventing stroke after transient ischemic attack. CMAJ. Jul 12 2011;183(10):1127-8. doi:10.1503/cmaj.110704
- Fanning JP, Wong AA, Fraser JF. The epidemiology of silent brain infarction: a systematic review of population-based cohorts. BMC Med. 2014;12:119. doi:10.1186/s12916-014-0119-0
- Ojaghihaghighi S, Vahdati SS, Mikaeilpour A, Ramouz A. Comparison of neurological clinical manifestation in patients with hemorrhagic and ischemic stroke. World J Emerg Med. 2017;8(1):34-38. doi:10.5847/wjem.j.1920-8642.2017.01.006
- Bhalla A, Wang Y, Rudd A, Wolfe CD. Differences in outcome and predictors between ischemic and intracerebral hemorrhage: the South London Stroke Register. Stroke. Aug 2013;44(8):2174-81. doi:10.1161/strokeaha.113.001263
- Perna R, Temple J. Rehabilitation Outcomes: Ischemic versus Hemorrhagic Strokes. Behavioural neurology. 2015/07/12 2015;2015:891651. doi:10.1155/2015/891651
- Andersen KK, Olsen TS, Dehlendorff C, Kammersgaard LP. Hemorrhagic and Ischemic Strokes Compared. Stroke. 2009;40(6):2068-2072. doi:doi:10.1161/STROKEAHA.108.540112
- Unnithan AKA, Mehta P. Hemorrhagic Stroke. StatPearls. 2021.
- MedlinePlus. Cerebral amyloid angiopathy. Updated June 23, 2020. Accessed March 5, 2021. https://medlineplus.gov/ency/article/000719.htm
- Unnithan AKA, Mehta P. Hemorrhagic Stroke. https://www.ncbi.nlm.nih.gov/pubmed/32644599
- Centers for Disease Control and Prevention. Types of strokes. Updated January 31, 2020. Accessed March 5, 2021. https://www.cdc.gov/stroke/types_of_stroke.htm#ischemic
- American Heart Association. What is an aneurysm? Updated January 22, 2021. Accessed March 5, 2021. https://www.heart.org/en/health-topics/aortic-aneurysm/what-is-an-aneurysm
- Gaciong Z, Sinski M, Lewandowski J. Blood pressure control and primary prevention of stroke: summary of the recent clinical trial data and meta-analyses. Curr Hypertens Rep. Dec 2013;15(6):559-74. doi:10.1007/s11906-013-0401-0
- Lawes CM, Bennett DA, Feigin VL, Rodgers A. Blood pressure and stroke: an overview of published reviews. Stroke. Apr 2004;35(4):1024.
- Lewington S, Clarke R, Qizilbash N, Peto R, Collins R, Prospective Studies C. Age-specific relevance of usual blood pressure to vascular mortality: a meta-analysis of individual data for one million adults in 61 prospective studies. Lancet. Dec 14 2002;360(9349):1903-13. doi:10.1016/s0140-6736(02)11911-8
- Pan B, Jin X, Jun L, Qiu S, Zheng Q, Pan M. The relationship between smoking and stroke: A meta-analysis. Medicine. Mar 2019;98(12):e14872. doi:10.1097/MD.0000000000014872
- Rask-Madsen C, King GL. Vascular complications of diabetes: mechanisms of injury and protective factors. Cell metabolism. Jan 8 2013;17(1):20-33. doi:10.1016/j.cmet.2012.11.012
- Peters SA, Huxley RR, Woodward M. Diabetes as a risk factor for stroke in women compared with men: a systematic review and meta-analysis of 64 cohorts, including 775,385 individuals and 12,539 strokes. Lancet. Jun 7 2014;383(9933):1973-80. doi:10.1016/S0140-6736(14)60040-4
- Mitchell AB, Cole JW, McArdle PF, et al. Obesity increases risk of ischemic stroke in young adults. Stroke. Jun 2015;46(6):1690-2. doi:10.1161/STROKEAHA.115.008940
- Shi TH, Wang B, Natarajan S. The Influence of Metabolic Syndrome in Predicting Mortality Risk Among US Adults: Importance of Metabolic Syndrome Even in Adults With Normal Weight. Preventing chronic disease. May 21 2020;17:E36. doi:10.5888/pcd17.200020
- Boden-Albala B, Sacco RL, Lee HS, et al. Metabolic syndrome and ischemic stroke risk: Northern Manhattan Study. Stroke. Jan 2008;39(1):30-5. doi:10.1161/STROKEAHA.107.496588
- Oesch L, Tatlisumak T, Arnold M, Sarikaya H. Obesity paradox in stroke - Myth or reality? A systematic review. PLoS One. 2017;12(3):e0171334. doi:10.1371/journal.pone.0171334
- Willey JZ, Moon YP, Paik MC, Boden-Albala B, Sacco RL, Elkind MS. Physical activity and risk of ischemic stroke in the Northern Manhattan Study. Neurology. Nov 24 2009;73(21):1774-9. doi:10.1212/WNL.0b013e3181c34b58
- Centers for Disease Control and Prevention. Conditions that increase risk for stroke. Updated January 31, 2020. Accessed March 8, 2021. https://www.cdc.gov/stroke/conditions.htm
- Murphy SJ, Werring DJ. Stroke: causes and clinical features. Medicine (Abingdon). Sep 2020;48(9):561-566. doi:10.1016/j.mpmed.2020.06.002
- Meschia JF, Bushnell C, Boden-Albala B, et al. Guidelines for the primary prevention of stroke: a statement for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. Dec 2014;45(12):3754-832. doi:10.1161/STR.0000000000000046
- Talahma M, Strbian D, Sundararajan S. Sickle cell disease and stroke. Stroke. Jun 2014;45(6):e98-100. doi:10.1161/STROKEAHA.114.005144
- Redline S, Yenokyan G, Gottlieb DJ, et al. Obstructive sleep apnea-hypopnea and incident stroke: the sleep heart health study. American journal of respiratory and critical care medicine. Jul 15 2010;182(2):269-77. doi:10.1164/rccm.200911-1746OC
- Furie KL, Rost NS. Overview of secondary prevention of ischemic stroke. UpToDate. Updated 2/2/2021. Accessed 2/5/2021, https://www.uptodate.com/contents/overview-of-secondary-prevention-of-ischemic-stroke?search=Overview%20of%20secondary%20prevention%20of%20ischemic%20stroke&source=search_result&selectedTitle=1~150&usage_type=default&display_rank=1
- American Stroke Association. Stroke risk factors not within your control. Updated October 10, 2018. Accessed March 8, 2021. https://www.stroke.org/en/about-stroke/stroke-risk-factors/stroke-risk-factors-not-within-your-control
- Heart and Stroke. Atrial fibrillation. Accessed May 5, 2021. https://www.heartandstroke.ca/heart-disease/conditions/atrial-fibrillation
- Hong KS. Blood Pressure Management for Stroke Prevention and in Acute Stroke. J Stroke. May 2017;19(2):152-165. doi:10.5853/jos.2017.00164
- Psaty BM, Lumley T, Furberg CD, et al. Health outcomes associated with various antihypertensive therapies used as first-line agents: a network meta-analysis. JAMA. May 21 2003;289(19):2534-44. doi:10.1001/jama.289.19.2534
- MacMahon S, Rodgers A. Blood pressure, antihypertensive treatment and stroke risk. Journal of hypertension Supplement : official journal of the International Society of Hypertension . Dec 1994;12(10):S5-14.
- Law MR, Morris JK, Wald NJ. Use of blood pressure lowering drugs in the prevention of cardiovascular disease: meta-analysis of 147 randomised trials in the context of expectations from prospective epidemiological studies. BMJ (Clinical research ed). May 19 2009;338:b1665. doi:10.1136/bmj.b1665
- Katsanos AH, Filippatou A, Manios E, et al. Blood Pressure Reduction and Secondary Stroke Prevention: A Systematic Review and Metaregression Analysis of Randomized Clinical Trials. Hypertension. Jan 2017;69(1):171-179. doi:10.1161/HYPERTENSIONAHA.116.08485
- Stroke Association. Smoking and the risk of stroke. Updated 9/2017. Accessed 5/21/2021, https://www.stroke.org.uk/sites/default/files/smoking_and_the_risk_of_stroke.pdf
- Cho JH, Kwon HM, Park SE, et al. Protective effect of smoking cessation on subsequent myocardial infarction and ischemic stroke independent of weight gain: A nationwide cohort study. PLoS One. 2020;15(7):e0235276. doi:10.1371/journal.pone.0235276
- Shah RS, Cole JW. Smoking and stroke: the more you smoke the more you stroke. Expert review of cardiovascular therapy. Jul 2010;8(7):917-32. doi:10.1586/erc.10.56
- Chen J, Li S, Zheng K, et al. Impact of Smoking Status on Stroke Recurrence. J Am Heart Assoc. Apr 16 2019;8(8):e011696. doi:10.1161/JAHA.118.011696
- Osei AD, Mirbolouk M, Orimoloye OA, et al. Association Between E-Cigarette Use and Cardiovascular Disease Among Never and Current Combustible-Cigarette Smokers. Am J Med. Aug 2019;132(8):949-954 e2. doi:10.1016/j.amjmed.2019.02.016
- Goniewicz ML, Miller CR, Sutanto E, Li D. How effective are electronic cigarettes for reducing respiratory and cardiovascular risk in smokers? A systematic review. Harm Reduct J. Nov 23 2020;17(1):91. doi:10.1186/s12954-020-00440-w
- Zhang Z, Yan J, Shi H. Hyperglycemia as a Risk Factor of Ischemic Stroke. J Drug Metab Toxicol. Jun 29 2013;4(4)doi:10.4172/2157-7609.1000153
- Chen R, Ovbiagele B, Feng W. Diabetes and Stroke: Epidemiology, Pathophysiology, Pharmaceuticals and Outcomes. The American journal of the medical sciences. Apr 2016;351(4):380-6. doi:10.1016/j.amjms.2016.01.011
- Zabala A, Darsalia V, Holzmann MJ, et al. Risk of first stroke in people with type 2 diabetes and its relation to glycaemic control: A nationwide observational study. Diabetes, obesity & metabolism. Feb 2020;22(2):182-190. doi:10.1111/dom.13885
- Cheng Y-Y, Leu H-B, Chen T-J, et al. Metformin-inclusive Therapy Reduces the Risk of Stroke in Patients with Diabetes: A 4-Year Follow-up Study. Journal of Stroke and Cerebrovascular Diseases. 2014/02/01/ 2014;23(2):e99-e105. doi:https://doi.org/10.1016/j.jstrokecerebrovasdis.2013.09.001
- Cukierman-Yaffe T, McClure LA, Risoli T, et al. The Relationship Between Glucose Control and Cognitive Function in People With Diabetes After a Lacunar Stroke. J Clin Endocrinol Metab. Mar 25 2021;106(4):e1521-e1528. doi:10.1210/clinem/dgab022
- Yaghi S, Dehkharghani S, Raz E, et al. The Effect of Hyperglycemia on Infarct Growth after Reperfusion: An Analysis of the DEFUSE 3 trial. J Stroke Cerebrovasc Dis. Jan 2021;30(1):105380. doi:10.1016/j.jstrokecerebrovasdis.2020.105380
- Chen Z, Mo J, Xu J, et al. Combined impact of body mass index and glycemic control on the efficacy of clopidogrel-aspirin therapy in patients with minor stroke or transient ischemic attack. Aging (Albany NY). Jun 16 2020;12(12):12175-12186. doi:10.18632/aging.103394
- Kleindorfer DO, Towfighi A, Chaturvedi S, et al. 2021 Guideline for the Prevention of Stroke in Patients With Stroke and Transient Ischemic Attack: A Guideline From the American Heart Association/American Stroke Association. Stroke. Jul 2021;52(7):e364-e467. doi:10.1161/STR.0000000000000375
- Kernan WN, Ovbiagele B, Black HR, et al. Guidelines for the Prevention of Stroke in Patients With Stroke and Transient Ischemic Attack. Stroke. 2014;45(7):2160-2236. doi:doi:10.1161/STR.0000000000000024
- Benjamin EJ, Blaha MJ, Chiuve SE, et al. Heart Disease and Stroke Statistics-2017 Update: A Report From the American Heart Association. Circulation. Mar 7 2017;135(10):e146-e603. doi:10.1161/CIR.0000000000000485
- Harvard Health Publishing. DASH or Mediterranean: Which diet is better for you? Accessed May 6, 2021. https://www.health.harvard.edu/diet-and-weight-loss/dash-or-mediterranean-which-diet-is-better-for-you
- Chen GC, Neelakantan N, Martin-Calvo N, et al. Adherence to the Mediterranean diet and risk of stroke and stroke subtypes. European journal of epidemiology. Apr 2019;34(4):337-349. doi:10.1007/s10654-019-00504-7
- Shannon OM, Mendes I, Kochl C, et al. Mediterranean Diet Increases Endothelial Function in Adults: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. J Nutr. May 1 2020;150(5):1151-1159. doi:10.1093/jn/nxaa002
- Saulle R, Lia L, De Giusti M, La Torre G. A systematic overview of the scientific literature on the association between Mediterranean Diet and the Stroke prevention. Clin Ter. Sep-Oct 2019;170(5):e396-e408. doi:10.7417/CT.2019.2166
- Filippou CD, Tsioufis CP, Thomopoulos CG, et al. Dietary Approaches to Stop Hypertension (DASH) Diet and Blood Pressure Reduction in Adults with and without Hypertension: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. Adv Nutr. Sep 1 2020;11(5):1150-1160. doi:10.1093/advances/nmaa041
- Feng Q, Fan S, Wu Y, et al. Adherence to the dietary approaches to stop hypertension diet and risk of stroke: A meta-analysis of prospective studies. Medicine. Sep 2018;97(38):e12450. doi:10.1097/MD.0000000000012450
- Rush University Medical Center. New MIND Diet May Significantly Protect Against Alzheimer's Disease. Updated 2021. Accessed 5/21/2021, https://www.rush.edu/news/new-mind-diet-may-significantly-protect-against-alzheimers-disease
- Cleveland Clinic. Should You Try the MIND Diet to Preserve Your Brain’s Health After a Stroke? Accessed May 6, 2021. https://health.clevelandclinic.org/should-you-try-the-mind-diet-to-preserve-your-brains-health-after-a-stroke/
- Cherian L, Wang Y, Fakuda K, Leurgans S, Aggarwal N, Morris M. Mediterranean-Dash Intervention for Neurodegenerative Delay (MIND) Diet Slows Cognitive Decline After Stroke. The journal of prevention of Alzheimer's disease. 2019;6(4):267-273. doi:10.14283/jpad.2019.28
- Howard VJ, McDonnell MN. Physical Activity in Primary Stroke Prevention. Stroke. 2015;46(6):1735-1739. doi:doi:10.1161/STROKEAHA.115.006317
- Tian X, Du H, Li L, et al. Fruit consumption and physical activity in relation to all-cause and cardiovascular mortality among 70,000 Chinese adults with pre-existing vascular disease. PLoS One. 2017;12(4):e0173054. doi:10.1371/journal.pone.0173054
- Kyu HH, Bachman VF, Alexander LT, et al. Physical activity and risk of breast cancer, colon cancer, diabetes, ischemic heart disease, and ischemic stroke events: systematic review and dose-response meta-analysis for the Global Burden of Disease Study 2013. BMJ (Clinical research ed). Aug 9 2016;354:i3857. doi:10.1136/bmj.i3857
- Billinger SA, Arena R, Bernhardt J, et al. Physical activity and exercise recommendations for stroke survivors: a statement for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. Aug 2014;45(8):2532-53. doi:10.1161/str.0000000000000022
- Han P, Zhang W, Kang L, et al. Clinical Evidence of Exercise Benefits for Stroke. Adv Exp Med Biol. 2017;1000:131-151. doi:10.1007/978-981-10-4304-8_9
- Kirchhof P, Benussi S, Kotecha D, et al. 2016 ESC Guidelines for the management of atrial fibrillation developed in collaboration with EACTS. Eur J Cardiothorac Surg. Nov 2016;50(5):e1-e88. doi:10.1093/ejcts/ezw313
- Hayden DT, Hannon N, Callaly E, et al. Rates and Determinants of 5-Year Outcomes After Atrial Fibrillation-Related Stroke: A Population Study. Stroke. Dec 2015;46(12):3488-93. doi:10.1161/STROKEAHA.115.011139
- Hart RG, Pearce LA, Aguilar MI. Meta-analysis: antithrombotic therapy to prevent stroke in patients who have nonvalvular atrial fibrillation. Ann Intern Med. Jun 19 2007;146(12):857-67. doi:10.7326/0003-4819-146-12-200706190-00007
- Wang YP, Kehar R, Iansavitchene A, Lazo-Langner A. Bleeding Risk in Nonvalvular Atrial Fibrillation Patients Receiving Direct Oral Anticoagulants and Warfarin: A Systematic Review and Meta-Analysis of Observational Studies. TH Open. Jul 2020;4(3):e145-e152. doi:10.1055/s-0040-1714918
- Dawwas GK, Dietrich E, Cuker A, Barnes GD, Leonard CE, Lewis JD. Effectiveness and Safety of Direct Oral Anticoagulants Versus Warfarin in Patients With Valvular Atrial Fibrillation : A Population-Based Cohort Study. Ann Intern Med. Mar 30 2021;doi:10.7326/M20-6194
- Chiva-Blanch G, Badimon L. Benefits and Risks of Moderate Alcohol Consumption on Cardiovascular Disease: Current Findings and Controversies. Nutrients. Dec 30 2019;12(1)doi:10.3390/nu12010108
- American College of Cardiology. Moderate Alcohol Consumption Linked With High Blood Pressure. Accessed May 6, 2021. https://www.acc.org/about-acc/press-releases/2019/03/07/08/34/moderate-alcohol-consumption-linked-with-high-blood-pressure
- Flint AC, Kamel H, Navi BB, et al. Statin use during ischemic stroke hospitalization is strongly associated with improved poststroke survival. Stroke. Jan 2012;43(1):147-54. doi:10.1161/STROKEAHA.111.627729
- Flint AC, Kamel H, Navi BB, et al. Inpatient statin use predicts improved ischemic stroke discharge disposition. Neurology. May 22 2012;78(21):1678-83. doi:10.1212/WNL.0b013e3182575142
- Fang JX, Wang EQ, Wang W, Liu Y, Cheng G. The efficacy and safety of high-dose statins in acute phase of ischemic stroke and transient ischemic attack: a systematic review. Intern Emerg Med. Aug 2017;12(5):679-687. doi:10.1007/s11739-017-1650-8
- Yoshimura S, Uchida K, Daimon T, et al. Randomized Controlled Trial of Early Versus Delayed Statin Therapy in Patients With Acute Ischemic Stroke: ASSORT Trial (Administration of Statin on Acute Ischemic Stroke Patient). Stroke. Nov 2017;48(11):3057-3063. doi:10.1161/STROKEAHA.117.017623
- Liu J, Wang Q, Ye C, et al. Premorbid Use of Statin and Outcome of Acute Ischemic Stroke After Intravenous Thrombolysis: A Meta-Analysis. Frontiers in neurology. 2020;11:585592. doi:10.3389/fneur.2020.585592
- Uchida K, Yoshimura S, Imamura H, et al. Effect of Statin Administration After Onset of Acute Ischemic Stroke With Large Vessel Occlusion: Insights From RESCUE-Japan Registry 2. J Am Heart Assoc. Dec 2020;9(23):e017472. doi:10.1161/JAHA.120.017472
- Jeong HG, Kim BJ, Yang MH, Han MK, Bae HJ. Early Statins after Intravenous or Endovascular Recanalization Is Beneficial Regardless of Timing, Intensity, and Stroke Mechanism. J Stroke. Sep 2017;19(3):370-372. doi:10.5853/jos.2017.00836
- Powers WJ, Rabinstein AA, Ackerson T, et al. Guidelines for the Early Management of Patients With Acute Ischemic Stroke: 2019 Update to the 2018 Guidelines for the Early Management of Acute Ischemic Stroke: A Guideline for Healthcare Professionals From the American Heart Association/American Stroke Association. Stroke. Dec 2019;50(12):e344-e418. doi:10.1161/STR.0000000000000211
- Filho JO, Mullen MT. Initial assessment and management of acute stroke. UpToDate. Updated 11/11/2020. Accessed 2/5/2021, https://www.uptodate.com/contents/initial-assessment-and-management-of-acute-stroke?search=Initial%20assessment%20and%20management%20of%20acute%20stroke&source=search_result&selectedTitle=1~150&usage_type=default&display_rank=1
- Barbagallo M, Veronese N, Dominguez LJ. Magnesium in Aging, Health and Diseases. Nutrients. Jan 30 2021;13(2)doi:10.3390/nu13020463
- Zhao B, Hu L, Dong Y, et al. The Effect of Magnesium Intake on Stroke Incidence: A Systematic Review and Meta-Analysis With Trial Sequential Analysis. Front Neurol. 2019;10:852. doi:10.3389/fneur.2019.00852
- Larsson SC, Gill D. Association of Serum Magnesium Levels With Risk of Intracranial Aneurysm: A Mendelian Randomization Study. Neurology. Jun 22 2021;doi:10.1212/wnl.0000000000012244
- Cheng Z, Huang X, Muse FM, et al. Low Serum Magnesium Levels Are Associated With Hemorrhagic Transformation After Thrombolysis in Acute Ischemic Stroke. Front Neurol. 2020;11:962. doi:10.3389/fneur.2020.00962
- Tu X, Qiu H, Lin S, et al. Low levels of serum magnesium are associated with poststroke cognitive impairment in ischemic stroke patients. Neuropsychiatr Dis Treat. 2018;14:2947-2954. doi:10.2147/ndt.S181948
- Pan W-H, Lai Y-H, Yeh W-T, et al. Intake of potassium- and magnesium-enriched salt improves functional outcome after stroke: a randomized, multicenter, double-blind controlled trial. The American Journal of Clinical Nutrition. 2017;106(5):1267-1273. doi:10.3945/ajcn.116.148536
- Panahi Y, Mojtahedzadeh M, Najafi A, et al. Protective Effects of Intravenous Magnesium Sulfate in Stroke Patients Receiving Amiodarone: A Randomized Controlled Trial. Adv Exp Med Biol. 2021;1308:579-588. doi:10.1007/978-3-030-64872-5_28
- Ortiz JF, Ruxmohan S, Saxena A, et al. Minocycline and Magnesium As Neuroprotective Agents for Ischemic Stroke: A Systematic Review. Cureus. Dec 28 2020;12(12):e12339. doi:10.7759/cureus.12339
- Avgerinos KI, Chatzisotiriou A, Haidich AB, Tsapas A, Lioutas VA. Intravenous Magnesium Sulfate in Acute Stroke. Stroke. Apr 2019;50(4):931-938. doi:10.1161/strokeaha.118.021916
- Xu R, Wang L, Sun L, Dong J. Neuroprotective effect of magnesium supplementation on cerebral ischemic diseases. Life Sci. May 1 2021;272:119257. doi:10.1016/j.lfs.2021.119257
- Takeuchi S, Kumagai K, Toyooka T, Otani N, Wada K, Mori K. Intravenous Hydrogen Therapy With Intracisternal Magnesium Sulfate Infusion in Severe Aneurysmal Subarachnoid Hemorrhage. Stroke. Jan 2021;52(1):20-27. doi:10.1161/strokeaha.120.031260
- Mayo Clinic Staff. Mediterranean diet: A heart-healthy eating plan. Updated June 21, 2019. Accessed March 9, 2021. https://www.mayoclinic.org/healthy-lifestyle/nutrition-and-healthy-eating/in-depth/mediterranean-diet/art-20047801#:~:text=Olive%20oil%20is%20the%20primary,seeds%20also%20contain%20monounsaturated%20fat.
- Massaro M, Scoditti E, Carluccio MA, et al. Effects of Olive Oil on Blood Pressure: Epidemiological, Clinical, and Mechanistic Evidence. Nutrients. May 26 2020;12(6)doi:10.3390/nu12061548
- Samieri C, Feart C, Proust-Lima C, et al. Olive oil consumption, plasma oleic acid, and stroke incidence: the Three-City Study. Neurology. Aug 2 2011;77(5):418-25. doi:10.1212/WNL.0b013e318220abeb
- Martinez-Gonzalez MA, Dominguez LJ, Delgado-Rodriguez M. Olive oil consumption and risk of CHD and/or stroke: a meta-analysis of case-control, cohort and intervention studies. The British journal of nutrition. Jul 28 2014;112(2):248-59. doi:10.1017/s0007114514000713
- Perrinjaquet-Moccetti T, Busjahn A, Schmidlin C, Schmidt A, Bradl B, Aydogan C. Food supplementation with an olive (Olea europaea L.) leaf extract reduces blood pressure in borderline hypertensive monozygotic twins. Phytother Res. Sep 2008;22(9):1239-42. doi:10.1002/ptr.2455
- Dekanski D, Selakovic V, Piperski V, Radulovic Z, Korenic A, Radenovic L. Protective effect of olive leaf extract on hippocampal injury induced by transient global cerebral ischemia and reperfusion in Mongolian gerbils. Phytomedicine. Oct 15 2011;18(13):1137-43. doi:10.1016/j.phymed.2011.05.010
- Karkovic Markovic A, Toric J, Barbaric M, Jakobusic Brala C. Hydroxytyrosol, Tyrosol and Derivatives and Their Potential Effects on Human Health. Molecules (Basel, Switzerland). May 24 2019;24(10)doi:10.3390/molecules24102001
- Calahorra J, Shenk J, Wielenga VH, et al. Hydroxytyrosol, the Major Phenolic Compound of Olive Oil, as an Acute Therapeutic Strategy after Ischemic Stroke. Nutrients. Oct 11 2019;11(10)doi:10.3390/nu11102430
- Barca C, Wiesmann M, Calahorra J, et al. Impact of hydroxytyrosol on stroke: tracking therapy response on neuroinflammation and cerebrovascular parameters using PET-MR imaging and on functional outcomes. Theranostics. 2021;11(9):4030-4049. doi:10.7150/thno.48110
- Shi J, Wu G, Zou X, Jiang K. Oleuropein protects intracerebral hemorrhage-induced disruption of blood-brain barrier through alleviation of oxidative stress. Pharmacological reports : PR. Dec 2017;69(6):1206-1212. doi:10.1016/j.pharep.2017.05.004
- Zhang W, Liu X, Li Q. Protective Effects of Oleuropein Against Cerebral Ischemia/Reperfusion by Inhibiting Neuronal Apoptosis. Med Sci Monit. Sep 19 2018;24:6587-6598. doi:10.12659/MSM.912336
- Gao Y, Li X, Xu R, et al. Oleuropein Improved Post Cerebral Stroke Cognitive Function by Promoting Histone Acetylation and Phosphorylation of cAMP Response Element-Binding Protein in MCAO Rats. Dose-response : a publication of International Hormesis Society. Jul-Sep 2020;18(3):1559325820950102. doi:10.1177/1559325820950102
- Qian Y, Huang M, Guan T, et al. Maslinic acid promotes synaptogenesis and axon growth via Akt/GSK-3beta activation in cerebral ischemia model. European journal of pharmacology. Oct 5 2015;764:298-305. doi:10.1016/j.ejphar.2015.07.028
- American Stroke Association. The American Heart Association Diet and Lifestyle Recommendations. Updated August 15, 2017. Accessed March 10, 2021. https://www.stroke.org/en/healthy-living/healthy-eating/eat-smart/nutrition-basics/aha-diet-and-lifestyle-recommendations
- Bu J, Dou Y, Tian X, Wang Z, Chen G. The Role of Omega-3 Polyunsaturated Fatty Acids in Stroke. Oxid Med Cell Longev. 2016;2016:6906712. doi:10.1155/2016/6906712
- von Schacky C. Importance of EPA and DHA Blood Levels in Brain Structure and Function. Nutrients. Mar 25 2021;13(4)doi:10.3390/nu13041074
- Yang B, Ren XL, Huang H, Guo XJ, Ma AG, Li D. Circulating long-chain n-3 polyunsaturated fatty acid and incidence of stroke: a meta-analysis of prospective cohort studies. Oncotarget. Oct 13 2017;8(48):83781-83791. doi:10.18632/oncotarget.19530
- Bhatt DL, Steg PG, Miller M, et al. Cardiovascular Risk Reduction with Icosapent Ethyl for Hypertriglyceridemia. N Engl J Med. Jan 3 2019;380(1):11-22. doi:10.1056/NEJMoa1812792
- Serra MC, Ryan AS, Hafer-Macko CE, Yepes M, Nahab FB, Ziegler TR. Dietary and Serum Omega-6/Omega-3 Fatty Acids Are Associated with Physical and Metabolic Function in Stroke Survivors. Nutrients. Mar 6 2020;12(3)doi:10.3390/nu12030701
- Iso H, Rexrode KM, Stampfer MJ, et al. Intake of fish and omega-3 fatty acids and risk of stroke in women. JAMA. Jan 17 2001;285(3):304-12. doi:10.1001/jama.285.3.304
- He K, Rimm EB, Merchant A, et al. Fish Consumption and Risk of Stroke in Men. JAMA. 2002;288(24):3130-3136. doi:10.1001/jama.288.24.3130
- Chen C, Huang H, Dai QQ, et al. Fish consumption, long-chain omega-3 fatty acids intake and risk of stroke: An updated systematic review and meta-analysis. Asia Pac J Clin Nutr. 2021;30(1):140-152. doi:10.6133/apjcn.202103_30(1).0017
- Bernasconi AA, Wiest MM, Lavie CJ, Milani RV, Laukkanen JA. Effect of Omega-3 Dosage on Cardiovascular Outcomes: An Updated Meta-Analysis and Meta-Regression of Interventional Trials. Mayo Clin Proc. Feb 2021;96(2):304-313. doi:10.1016/j.mayocp.2020.08.034
- Abdelhamid AS, Brown TJ, Brainard JS, et al. Omega-3 fatty acids for the primary and secondary prevention of cardiovascular disease. The Cochrane database of systematic reviews. Feb 29 2020;3:CD003177. doi:10.1002/14651858.CD003177.pub5
- Nicholls SJ, Lincoff AM, Garcia M, et al. Effect of High-Dose Omega-3 Fatty Acids vs Corn Oil on Major Adverse Cardiovascular Events in Patients at High Cardiovascular Risk: The STRENGTH Randomized Clinical Trial. JAMA. Dec 8 2020;324(22):2268-2280. doi:10.1001/jama.2020.22258
- Hu Y, Hu FB, Manson JE. Marine Omega-3 Supplementation and Cardiovascular Disease: An Updated Meta-Analysis of 13 Randomized Controlled Trials Involving 127 477 Participants. J Am Heart Assoc. Oct 2019;8(19):e013543. doi:10.1161/JAHA.119.013543
- Panche AN, Diwan AD, Chandra SR. Flavonoids: an overview. Journal of nutritional science. 2016;5:e47. doi:10.1017/jns.2016.41
- Tang Z, Li M, Zhang X, Hou W. Dietary flavonoid intake and the risk of stroke: a dose-response meta-analysis of prospective cohort studies. BMJ open. Jun 8 2016;6(6):e008680. doi:10.1136/bmjopen-2015-008680
- Cassidy A, Rimm EB, O'Reilly EJ, et al. Dietary flavonoids and risk of stroke in women. Stroke. Apr 2012;43(4):946-51. doi:10.1161/STROKEAHA.111.637835
- Goetz ME, Judd SE, Hartman TJ, McClellan W, Anderson A, Vaccarino V. Flavanone Intake Is Inversely Associated with Risk of Incident Ischemic Stroke in the REasons for Geographic and Racial Differences in Stroke (REGARDS) Study. J Nutr. Nov 2016;146(11):2233-2243. doi:10.3945/jn.116.230185
- Meschia JF, Bushnell C, Boden-Albala B, et al. Guidelines for the primary prevention of stroke: a statement for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. 2014;45(12):3754-3832. doi:10.1161/STR.0000000000000046
- Wang Y, Jin Y, Wang Y, et al. The effect of folic acid in patients with cardiovascular disease: A systematic review and meta-analysis. Medicine. Sep 2019;98(37):e17095. doi:10.1097/MD.0000000000017095
- Tian T, Yang KQ, Cui JG, Zhou LL, Zhou XL. Folic Acid Supplementation for Stroke Prevention in Patients With Cardiovascular Disease. The American journal of the medical sciences. Oct 2017;354(4):379-387. doi:10.1016/j.amjms.2017.05.020
- Zhao M, Wu G, Li Y, et al. Meta-analysis of folic acid efficacy trials in stroke prevention: Insight into effect modifiers. Neurology. May 9 2017;88(19):1830-1838. doi:10.1212/WNL.0000000000003909
- Kataria N, Yadav P, Kumar R, et al. Effect of Vitamin B6, B9, and B12 Supplementation on Homocysteine Level and Cardiovascular Outcomes in Stroke Patients: A Meta-Analysis of Randomized Controlled Trials. Cureus. May 11 2021;13(5):e14958. doi:10.7759/cureus.14958
- Dong H, Pi F, Ding Z, et al. Efficacy of Supplementation with B Vitamins for Stroke Prevention: A Network Meta-Analysis of Randomized Controlled Trials. PLoS One. 2015;10(9):e0137533. doi:10.1371/journal.pone.0137533
- Dai G, Du H, Wang H, Wei Y, Xie Y, Li Z. [Preventive effect of Vitamin B supplementation on recurrent stroke: a Meta-analysis]. Zhonghua Wei Zhong Bing Ji Jiu Yi Xue. May 2017;29(5):419-424. doi:10.3760/cma.j.issn.2095-4352.2017.05.007
- Chen H, McGowan EM, Ren N, et al. Nattokinase: A Promising Alternative in Prevention and Treatment of Cardiovascular Diseases. Biomark Insights. 2018;13:1177271918785130. doi:10.1177/1177271918785130
- Pham PT, Han B, Hoang BX. Nattospes as Effective and Safe Functional Supplements in Management of Stroke. Journal of medicinal food. Aug 2020;23(8):879-885. doi:10.1089/jmf.2019.0183
- Hsia CH, Shen MC, Lin JS, et al. Nattokinase decreases plasma levels of fibrinogen, factor VII, and factor VIII in human subjects. Nutr Res. Mar 2009;29(3):190-6. doi:10.1016/j.nutres.2009.01.009
- Chang YY, Liu JS, Lai SL, Wu HS, Lan MY. Cerebellar hemorrhage provoked by combined use of nattokinase and aspirin in a patient with cerebral microbleeds. Intern Med. 2008;47(5):467-9. doi:10.2169/internalmedicine.47.0620
- Zhu Y, Anand R, Geng X, Ding Y. A mini review: garlic extract and vascular diseases. Neurol Res. Jun 2018;40(6):421-425. doi:10.1080/01616412.2018.1451269
- Ried K, Frank OR, Stocks NP, Fakler P, Sullivan T. Effect of garlic on blood pressure: a systematic review and meta-analysis. BMC cardiovascular disorders. Jun 16 2008;8:13. doi:10.1186/1471-2261-8-13
- Ried K. Garlic Lowers Blood Pressure in Hypertensive Individuals, Regulates Serum Cholesterol, and Stimulates Immunity: An Updated Meta-analysis and Review. J Nutr. Feb 2016;146(2):389s-396s. doi:10.3945/jn.114.202192
- Lau KK, Chan YH, Wong YK, et al. Garlic intake is an independent predictor of endothelial function in patients with ischemic stroke. The journal of nutrition, health & aging. Jul 2013;17(7):600-4. doi:10.1007/s12603-013-0043-6
- Zhang B, Li F, Zhao W, Li J, Li Q, Wang W. Protective effects of allicin against ischemic stroke in a rat model of middle cerebral artery occlusion. Molecular medicine reports. Sep 2015;12(3):3734-3738. doi:10.3892/mmr.2015.3883
- Surdu AM, Pinzariu O, Ciobanu DM, et al. Vitamin D and Its Role in the Lipid Metabolism and the Development of Atherosclerosis. Biomedicines. Feb 9 2021;9(2)doi:10.3390/biomedicines9020172
- Farapti F, Fadilla C, Yogiswara N, Adriani M. Effects of vitamin D supplementation on 25(OH)D concentrations and blood pressure in the elderly: a systematic review and meta-analysis. F1000Research. 2020;9:633. doi:10.12688/f1000research.24623.3
- Zhou R, Wang M, Huang H, Li W, Hu Y, Wu T. Lower Vitamin D Status Is Associated with an Increased Risk of Ischemic Stroke: A Systematic Review and Meta-Analysis. Nutrients. Feb 28 2018;10(3)doi:10.3390/nu10030277
- Berghout BP, Fani L, Heshmatollah A, et al. Vitamin D Status and Risk of Stroke: The Rotterdam Study. Stroke. Sep 2019;50(9):2293-2298. doi:10.1161/STROKEAHA.119.025449
- Miao H, Zhu H, Luan X, et al. Risk Factors of Vitamin D Deficiency in Chinese Ischemic Stroke Patients: A Cross-Sectional Study. Frontiers in aging neuroscience. 2020;12:613498. doi:10.3389/fnagi.2020.613498
- Barbarawi M, Kheiri B, Zayed Y, et al. Vitamin D Supplementation and Cardiovascular Disease Risks in More Than 83000 Individuals in 21 Randomized Clinical Trials: A Meta-analysis. JAMA Cardiol. Aug 1 2019;4(8):765-776. doi:10.1001/jamacardio.2019.1870
- Wajda J, Swiat M, Owczarek AJ, Brzozowska A, Olszanecka-Glinianowicz M, Chudek J. Severity of Vitamin D Deficiency Predicts Mortality in Ischemic Stroke Patients. Disease markers. 2019;2019:3652894. doi:10.1155/2019/3652894
- Gupta A, Prabhakar S, Modi M, et al. Effect of Vitamin D and calcium supplementation on ischaemic stroke outcome: a randomised controlled open-label trial. International journal of clinical practice. Sep 2016;70(9):764-70. doi:10.1111/ijcp.12866
- Longo N, Frigeni M, Pasquali M. Carnitine transport and fatty acid oxidation. Biochim Biophys Acta. Oct 2016;1863(10):2422-35. doi:10.1016/j.bbamcr.2016.01.023
- Wainwright MS, Mannix MK, Brown J, Stumpf DA. L-carnitine reduces brain injury after hypoxia-ischemia in newborn rats. Pediatric research. Nov 2003;54(5):688-95. doi:10.1203/01.PDR.0000085036.07561.9C
- Zhang R, Zhang H, Zhang Z, et al. Neuroprotective effects of pre-treatment with l-carnitine and acetyl-L-carnitine on ischemic injury in vivo and in vitro. International journal of molecular sciences. 2012;13(2):2078-90. doi:10.3390/ijms13022078
- Kazemian K, Ala S, Mojtahedzadeh M, et al. Evaluation of Neuroprtective Effects of L-Carnitine and Fat Emulsion in the CVA Patients: A Prospective, Randomized, Double Blind, Clinical Trial. Iranian journal of pharmaceutical research : IJPR. Winter 2020;19(1):111-119. doi:10.22037/ijpr.2020.1100952
- Arakawa M, Ito Y. N-acetylcysteine and neurodegenerative diseases: basic and clinical pharmacology. Cerebellum (London, England). 2007;6(4):308-14. doi:10.1080/14734220601142878
- Sabetghadam M, Mazdeh M, Abolfathi P, Mohammadi Y, Mehrpooya M. Evidence for a Beneficial Effect of Oral N-acetylcysteine on Functional Outcomes and Inflammatory Biomarkers in Patients with Acute Ischemic Stroke. Neuropsychiatr Dis Treat. 2020;16:1265-1278. doi:10.2147/NDT.S241497
- Kim M, Byun J, Chung Y, et al. Reactive Oxygen Species Scavenger in Acute Intracerebral Hemorrhage Patients: A Multicenter, Randomized Controlled Trial. Stroke. Apr 2021;52(4):1172-1181. doi:10.1161/STROKEAHA.120.032266
- Ashayeriahmadabad R, Mirzaasgari Z, Eshraghi A, et al. A randomized controlled trial of neuroprotective effects of n-acetyl-cysteine in patients with acute ischemic stroke. Journal of the Neurological Sciences. 2019;405:44-45. doi:https://doi.org/10.1016/j.jns.2019.10.295
- Verma T, Sinha M, Bansal N, Yadav SR, Shah K, Chauhan NS. Plants Used as Antihypertensive. Nat Prod Bioprospect. Apr 2021;11(2):155-184. doi:10.1007/s13659-020-00281-x
- Azami S, Shahriari Z, Asgharzade S, et al. Therapeutic Potential of Saffron (Crocus sativus L.) in Ischemia Stroke. Evid Based Complement Alternat Med. 2021;2021:6643950. doi:10.1155/2021/6643950
- Zhong K, Wang RX, Qian XD, et al. Neuroprotective effects of saffron on the late cerebral ischemia injury through inhibiting astrogliosis and glial scar formation in rats. Biomed Pharmacother. Jun 2020;126:110041. doi:10.1016/j.biopha.2020.110041
- Zhang Y, Liu J, Yao M, et al. Sailuotong Capsule Prevents the Cerebral Ischaemia-Induced Neuroinflammation and Impairment of Recognition Memory through Inhibition of LCN2 Expression. Oxid Med Cell Longev. 2019;2019:8416105. doi:10.1155/2019/8416105
- Duan Z, Li H, Qi X, et al. Crocin attenuation of neurological deficits in a mouse model of intracerebral hemorrhage. Brain Res Bull. Aug 2019;150:186-195. doi:10.1016/j.brainresbull.2019.05.023
- Sadeghnia HR, Shaterzadeh H, Forouzanfar F, Hosseinzadeh H. Neuroprotective effect of safranal, an active ingredient of Crocus sativus , in a rat model of transient cerebral ischemia. Folia Neuropathol. 2017;55(3):206-213. doi:10.5114/fn.2017.70485
- Gudarzi S, Jafari M, Pirzad Jahromi G, Eshrati R, Asadollahi M, Nikdokht P. Evaluation of modulatory effects of saffron (Crocus sativus L.) aqueous extract on oxidative stress in ischemic stroke patients: a randomized clinical trial. Nutr Neurosci. Nov 5 2020:1-10. doi:10.1080/1028415x.2020.1840118
- Asadollahi M, Nikdokht P, Hatef B, et al. Protective properties of the aqueous extract of saffron (Crocus sativus L.) in ischemic stroke, randomized clinical trial. Journal of ethnopharmacology. Jun 28 2019;238:111833. doi:10.1016/j.jep.2019.111833
- Rohdewald P. Pleiotropic Effects of French Maritime Pine Bark Extract to Promote Healthy Aging. Rejuvenation Res. Jun 2019;22(3):210-217. doi:10.1089/rej.2018.2095
- Malekahmadi M, Moradi Moghaddam O, Firouzi S, et al. Effects of pycnogenol on cardiometabolic health: A systematic review and meta-analysis of randomized controlled trials. Pharmacol Res. Dec 2019;150:104472. doi:10.1016/j.phrs.2019.104472
- Kim B, Lee TK, Park CW, et al. Pycnogenol(®) Supplementation Attenuates Memory Deficits and Protects Hippocampal CA1 Pyramidal Neurons via Antioxidative Role in a Gerbil Model of Transient Forebrain Ischemia. Nutrients. Aug 17 2020;12(8)doi:10.3390/nu12082477
- Ozoner B, Yuceli S, Aydin S, et al. Effects of pycnogenol on ischemia/reperfusion-induced inflammatory and oxidative brain injury in rats. Neurosci Lett. Jun 21 2019;704:169-175. doi:10.1016/j.neulet.2019.04.010
- Belcaro G, Cesarone MR, Scipione C, et al. Delayed progression of atherosclerosis and cardiovascular events in asymptomatic patients with atherosclerotic plaques: 3-year prevention with the supplementation with Pycnogenol®+Centellicum®. Minerva Cardioangiol. Feb 2020;68(1):15-21. doi:10.23736/s0026-4725.19.05051-5
- Lai AKW, Ng DTC, Tam BKC, Fung FKC, Chung SK, Lo ACY. Lutein for alleviating early high mortality and brain pathology after experimental stroke in a genetic type I diabetic mouse model: abridged secondary publication. Hong Kong Med J. Dec 2020;26 Suppl 7(6):37-41.
- Nai Y, Liu H, Bi X, Gao H, Ren C. Protective effect of astaxanthin on acute cerebral infarction in rats. Hum Exp Toxicol. Sep 2018;37(9):929-936. doi:10.1177/0960327117745693
- Ji X, Peng D, Zhang Y, et al. Astaxanthin improves cognitive performance in mice following mild traumatic brain injury. Brain research. Mar 15 2017;1659:88-95. doi:10.1016/j.brainres.2016.12.031
- Giordano P, Scicchitano P, Locorotondo M, et al. Carotenoids and cardiovascular risk. Curr Pharm Des. 2012;18(34):5577-89. doi:10.2174/138161212803307527
- Li N, Wu X, Zhuang W, et al. Green leafy vegetable and lutein intake and multiple health outcomes. Food Chem. Oct 30 2021;360:130145. doi:10.1016/j.foodchem.2021.130145
- Leermakers ET, Darweesh SK, Baena CP, et al. The effects of lutein on cardiometabolic health across the life course: a systematic review and meta-analysis. Am J Clin Nutr. Feb 2016;103(2):481-94. doi:10.3945/ajcn.115.120931
- Bahonar A, Saadatnia M, Khorvash F, Maracy M, Khosravi A. Carotenoids as Potential Antioxidant Agents in Stroke Prevention: A Systematic Review. Int J Prev Med. 2017;8:70. doi:10.4103/ijpvm.IJPVM_112_17
- Cheng YH, Wei L, Chan WP, et al. Effects of protein supplementation on aerobic training-induced gains in cardiopulmonary fitness, muscle mass, and functional performance in chronic stroke: A randomized controlled pilot study. Clin Nutr. Sep 2020;39(9):2743-2750. doi:10.1016/j.clnu.2019.12.013
- Pan Y, Shi G. Silver Jubilee of Stroke Thrombolysis With Alteplase: Evolution of the Therapeutic Window. Frontiers in neurology. 2021;12:593887. doi:10.3389/fneur.2021.593887
- Campbell BCV, Ma H, Ringleb PA, et al. Extending thrombolysis to 4.5-9 h and wake-up stroke using perfusion imaging: a systematic review and meta-analysis of individual patient data. Lancet. Jul 13 2019;394(10193):139-147. doi:10.1016/S0140-6736(19)31053-0
- Langhorne P, Ramachandra S, Stroke Unit Trialists C. Organised inpatient (stroke unit) care for stroke: network meta-analysis. The Cochrane database of systematic reviews. Apr 23 2020;4:CD000197. doi:10.1002/14651858.CD000197.pub4
- Hemphill JC, 3rd, Greenberg SM, Anderson CS, et al. Guidelines for the Management of Spontaneous Intracerebral Hemorrhage: A Guideline for Healthcare Professionals From the American Heart Association/American Stroke Association. Stroke. Jul 2015;46(7):2032-60. doi:10.1161/STR.0000000000000069
- Ishida K. Complications of stroke: An overview. UpToDate. Updated 11/11/2020. Accessed 2/5/2021, https://www.uptodate.com/contents/complications-of-stroke-an-overview?search=complications%20of%20stroke%20-%20an%20overview&source=search_result&selectedTitle=1~150&usage_type=default&display_rank=1
- Powers WJ, Rabinstein AA, Ackerson T, et al. 2018 Guidelines for the Early Management of Patients With Acute Ischemic Stroke: A Guideline for Healthcare Professionals From the American Heart Association/American Stroke Association. Stroke. Mar 2018;49(3):e46-e110. doi:10.1161/STR.0000000000000158
- Tawil SE, Muir KW. Thrombolysis and thrombectomy for acute ischaemic stroke. Clinical medicine (London, England). Apr 2017;17(2):161-165. doi:10.7861/clinmedicine.17-2-161
- Filho JO, Samuels OB. Mechanical thrombectomy for acute ischemic stroke. Updated May 3, 2021. Accessed May 6, 2021. https://www.uptodate.com/contents/mechanical-thrombectomy-for-acute-ischemic-stroke
- Saver JL, Adeoye O. Intravenous Thrombolysis Before Endovascular Thrombectomy for Acute Ischemic Stroke. JAMA. 2021;325(3):229-231. doi:10.1001/jama.2020.22388
- Ouyang M, Munoz-Venturelli P, Billot L, et al. Low blood pressure and adverse outcomes in acute stroke: HeadPoST study explanations. Journal of hypertension. Feb 1 2021;39(2):273-279. doi:10.1097/HJH.0000000000002649
- Sandercock PA, Counsell C, Tseng MC, Cecconi E. Oral antiplatelet therapy for acute ischaemic stroke. The Cochrane database of systematic reviews. Mar 26 2014;(3):CD000029. doi:10.1002/14651858.CD000029.pub3
- Rothwell PM, Algra A, Chen Z, Diener HC, Norrving B, Mehta Z. Effects of aspirin on risk and severity of early recurrent stroke after transient ischaemic attack and ischaemic stroke: time-course analysis of randomised trials. Lancet. Jul 23 2016;388(10042):365-375. doi:10.1016/S0140-6736(16)30468-8
- Harvard Health Publishing. Hemorrhagic stroke. Accessed May 5, 2021. https://www.health.harvard.edu/a_to_z/hemorrhagic-stroke-a-to-z
- Rordrof G, McDonald C. Spontaneous intracerebral hemorrhage: Treatment and prognosis. Updated March 29, 2021. Accessed May 5, 2021. https://www.uptodate.com/contents/spontaneous-intracerebral-hemorrhage-treatment-and-prognosis
- Gómez-Outes A, Alcubilla P, Calvo-Rojas G, et al. Meta-Analysis of Reversal Agents for Severe Bleeding Associated With Direct Oral Anticoagulants. J Am Coll Cardiol. Jun 22 2021;77(24):2987-3001. doi:10.1016/j.jacc.2021.04.061
- Anderson CS, Huang Y, Arima H, et al. Effects of early intensive blood pressure-lowering treatment on the growth of hematoma and perihematomal edema in acute intracerebral hemorrhage: the Intensive Blood Pressure Reduction in Acute Cerebral Haemorrhage Trial (INTERACT). Stroke. Feb 2010;41(2):307-12. doi:10.1161/STROKEAHA.109.561795
- Kim JY, Bae HJ. Spontaneous Intracerebral Hemorrhage: Management. J Stroke. Jan 2017;19(1):28-39. doi:10.5853/jos.2016.01935
- Ishida K. Prevention and treatment of venous thromboembolism in patients with acute stroke. Updated August 28, 2019. Accessed May 6, 2021. https://www.uptodate.com/contents/prevention-and-treatment-of-venous-thromboembolism-in-patients-with-acute-stroke
- Badireddy M, Mudipalli VR. Deep Venous Thrombosis Prophylaxis. StatPearls. 2021.
- Wastfelt M, Cao Y, Strom JO. Predictors of post-stroke fever and infections: a systematic review and meta-analysis. BMC Neurol. Apr 23 2018;18(1):49. doi:10.1186/s12883-018-1046-z
- Hinchey JA, Shephard T, Furie K, et al. Formal dysphagia screening protocols prevent pneumonia. Stroke. Sep 2005;36(9):1972-6. doi:10.1161/01.STR.0000177529.86868.8d
- Schwarz S, Hafner K, Aschoff A, Schwab S. Incidence and prognostic significance of fever following intracerebral hemorrhage. Neurology. Jan 25 2000;54(2):354-61. doi:10.1212/wnl.54.2.354
- Wrotek SE, Kozak WE, Hess DC, Fagan SC. Treatment of fever after stroke: conflicting evidence. Pharmacotherapy. Nov 2011;31(11):1085-91. doi:10.1592/phco.31.11.1085
- Al-Qazzaz NK, Ali SH, Ahmad SA, Islam S, Mohamad K. Cognitive impairment and memory dysfunction after a stroke diagnosis: a post-stroke memory assessment. Neuropsychiatr Dis Treat. 2014;10:1677-91. doi:10.2147/NDT.S67184
- American Stroke Association. Cognitive challenges post stroke. Accessed March 5, 2021. https://www.stroke.org/en/about-stroke/effects-of-stroke/cognitive-and-communication-effects-of-stroke
- National Institute of Neurological Disorders and Stroke. Post-stroke rehabilition fact sheet. Updated May 13, 2020. Accessed March 5, 2021. https://www.ninds.nih.gov/Disorders/Patient-Caregiver-Education/Fact-Sheets/Post-Stroke-Rehabilitation-Fact-Sheet
- Gunnes M, Indredavik B, Langhammer B, et al. Associations Between Adherence to the Physical Activity and Exercise Program Applied in the LAST Study and Functional Recovery After Stroke. Archives of physical medicine and rehabilitation. Dec 2019;100(12):2251-2259. doi:10.1016/j.apmr.2019.04.023
- American Stroke Association. Rehab therapy after a stroke. Accessed May 4, 2021. https://www.stroke.org/en/life-after-stroke/stroke-rehab/rehab-therapy-after-a-stroke
- Edwardson MA. Overview of ischemic stroke prognosis in adults. UpToDate. Updated 12/18/2020. Accessed 2/5/2021, https://www.uptodate.com/contents/overview-of-ischemic-stroke-prognosis-in-adults?search=Overview%20of%20ischemic%20stroke%20prognosis%20in%20adults&source=search_result&selectedTitle=1~150&usage_type=default&display_rank=1
- Lawrence ES, Coshall C, Dundas R, et al. Estimates of the prevalence of acute stroke impairments and disability in a multiethnic population. Stroke. Jun 2001;32(6):1279-84. doi:10.1161/01.str.32.6.1279
- Grefkes C, Fink GR. Recovery from stroke: current concepts and future perspectives. Neurol Res Pract. 2020;2:17. doi:10.1186/s42466-020-00060-6
- Gonzalez-Fernandez M, Ottenstein L, Atanelov L, Christian AB. Dysphagia after Stroke: an Overview. Curr Phys Med Rehabil Rep. Sep 2013;1(3):187-196. doi:10.1007/s40141-013-0017-y
- Stroke Association. Continence problems after stroke. Accessed March 5, 2021. https://www.stroke.org.uk/sites/default/files/continence_problems_after_stroke.pdf
- Thomas LH, Cross S, Barrett J, et al. Treatment of urinary incontinence after stroke in adults. The Cochrane database of systematic reviews. Jan 23 2008;(1):CD004462. doi:10.1002/14651858.CD004462.pub3
- Harari D, Coshall C, Rudd AG, Wolfe CD. New-onset fecal incontinence after stroke: prevalence, natural history, risk factors, and impact. Stroke. Jan 2003;34(1):144-50.
- National Aphasia Association. Aphasia statistics. Accessed March 8, 2021. https://www.aphasia.org/aphasia-resources/aphasia-statistics/
- National Institute on Deafness and Other Communication Disorders. Aphasia. Updated March 6, 2017. Accessed May 4, 2021. https://www.nidcd.nih.gov/health/aphasia
- Chohan SA, Venkatesh PK, How CH. Long-term complications of stroke and secondary prevention: an overview for primary care physicians. Singapore Med J. Dec 2019;60(12):616-620. doi:10.11622/smedj.2019158
- Mijajlović MD, Pavlović A, Brainin M, et al. Post-stroke dementia - a comprehensive review. BMC Med. Jan 18 2017;15(1):11. doi:10.1186/s12916-017-0779-7
- Li J, Zhang P, Wu S, et al. Impaired consciousness at stroke onset in large hemisphere infarction: incidence, risk factors and outcome. Sci Rep. Aug 5 2020;10(1):13170. doi:10.1038/s41598-020-70172-1
- Tsai YH, Yuan R, Huang YC, Yeh MY, Lin CP, Biswal BB. Disruption of brain connectivity in acute stroke patients with early impairment in consciousness. Front Psychol. 2014;4:956. doi:10.3389/fpsyg.2013.00956
- American Stroke Association. Vascular dementia. Updated November 21, 2018. Accessed March 8, 2021. https://www.stroke.org/en/about-stroke/effects-of-stroke/cognitive-and-communication-effects-of-stroke/vascular-dementia
- Kuzma E, Lourida I, Moore SF, Levine DA, Ukoumunne OC, Llewellyn DJ. Stroke and dementia risk: A systematic review and meta-analysis. Alzheimer's & dementia : the journal of the Alzheimer's Association . Nov 2018;14(11):1416-1426. doi:10.1016/j.jalz.2018.06.3061
- Wolters FJ, Ikram MA. Epidemiology of Vascular Dementia. Arteriosclerosis, thrombosis, and vascular biology. Aug 2019;39(8):1542-1549. doi:10.1161/ATVBAHA.119.311908
- Campbell Burton CA, Murray J, Holmes J, Astin F, Greenwood D, Knapp P. Frequency of anxiety after stroke: a systematic review and meta-analysis of observational studies. Int J Stroke. Oct 2013;8(7):545-59. doi:10.1111/j.1747-4949.2012.00906.x
- Towfighi A, Ovbiagele B, El Husseini N, et al. Poststroke Depression: A Scientific Statement for Healthcare Professionals From the American Heart Association/American Stroke Association. Stroke. Feb 2017;48(2):e30-e43. doi:10.1161/STR.0000000000000113
- Lopatkiewicz AM, Pera J, Slowik A, Dziedzic T. Early apathetic, but not depressive, symptoms are associated with poor outcome after stroke. European journal of neurology : the official journal of the European Federation of Neurological Societies . Feb 22 2021;doi:10.1111/ene.14785
- Williams OA, Demeyere N. Association of Depression and Anxiety With Cognitive Impairment 6 Months After Stroke. Neurology. Apr 13 2021;96(15):e1966-e1974. doi:10.1212/WNL.0000000000011748
- Li W, Yang S. Targeting oxidative stress for the treatment of ischemic stroke: Upstream and downstream therapeutic strategies. Brain Circ . Oct-Dec 2016;2(4):153-163. doi:10.4103/2394-8108.195279
- Pizzino G, Irrera N, Cucinotta M, et al. Oxidative Stress: Harms and Benefits for Human Health. Oxid Med Cell Longev. 2017;2017:8416763. doi:10.1155/2017/8416763
- Chamorro A, Amaro S, Castellanos M, et al. Uric acid therapy improves the outcomes of stroke patients treated with intravenous tissue plasminogen activator and mechanical thrombectomy. Int J Stroke. Jun 2017;12(4):377-382. doi:10.1177/1747493016684354
- Llull L, Laredo C, Renu A, et al. Uric Acid Therapy Improves Clinical Outcome in Women With Acute Ischemic Stroke. Stroke. Aug 2015;46(8):2162-7. doi:10.1161/STROKEAHA.115.009960
- Amaro S, Llull L, Renu A, et al. Uric acid improves glucose-driven oxidative stress in human ischemic stroke. Ann Neurol. May 2015;77(5):775-83. doi:10.1002/ana.24378
- Bernard SA, Gray TW, Buist MD, et al. Treatment of comatose survivors of out-of-hospital cardiac arrest with induced hypothermia. The New England journal of medicine. Feb 21 2002;346(8):557-63. doi:10.1056/NEJMoa003289
- Hypothermia after Cardiac Arrest Study G. Mild therapeutic hypothermia to improve the neurologic outcome after cardiac arrest. The New England journal of medicine. Feb 21 2002;346(8):549-56. doi:10.1056/NEJMoa012689
- Zhi D, Zhang S, Lin X. Study on therapeutic mechanism and clinical effect of mild hypothermia in patients with severe head injury. Surgical neurology. May 2003;59(5):381-5. doi:10.1016/s0090-3019(03)00148-4
- Polderman KH, Tjong Tjin Joe R, Peerdeman SM, Vandertop WP, Girbes AR. Effects of therapeutic hypothermia on intracranial pressure and outcome in patients with severe head injury. Intensive care medicine. Nov 2002;28(11):1563-73. doi:10.1007/s00134-002-1511-3
- Kuczynski AM, Demchuk AM, Almekhlafi MA. Therapeutic hypothermia: Applications in adults with acute ischemic stroke. Brain Circ. Apr-Jun 2019;5(2):43-54. doi:10.4103/bc.bc_5_19
- Su Y, Fan L, Zhang Y, et al. Improved Neurological Outcome With Mild Hypothermia in Surviving Patients With Massive Cerebral Hemispheric Infarction. Stroke. Feb 2016;47(2):457-63. doi:10.1161/STROKEAHA.115.009789
- Hemmen TM, Raman R, Guluma KZ, et al. Intravenous thrombolysis plus hypothermia for acute treatment of ischemic stroke (ICTuS-L): final results. Stroke. Oct 2010;41(10):2265-70. doi:10.1161/STROKEAHA.110.592295
- Geurts M, Petersson J, Brizzi M, et al. COOLIST (Cooling for Ischemic Stroke Trial): A Multicenter, Open, Randomized, Phase II, Clinical Trial. Stroke. Jan 2017;48(1):219-221. doi:10.1161/STROKEAHA.116.014757
- Yao Z, You C, He M. Effect and Feasibility of Therapeutic Hypothermia in Patients with Hemorrhagic Stroke: A Systematic Review and Meta-Analysis. World neurosurgery. Mar 2018;111:404-412 e2. doi:10.1016/j.wneu.2018.01.020
- Al-Kuraishy HM, Al-Gareeb AI, Naji MT, Al-Mamorry F. Role of vinpocetine in ischemic stroke and poststroke outcomes: A critical review. Brain Circ. Jan-Mar 2020;6(1):1-10. doi:10.4103/bc.bc_46_19
- Zang J, Wu Y, Su X, et al. Inhibition of PDE1-B by Vinpocetine Regulates Microglial Exosomes and Polarization Through Enhancing Autophagic Flux for Neuroprotection Against Ischemic Stroke. Frontiers in cell and developmental biology. 2020;8:616590. doi:10.3389/fcell.2020.616590
- Han D, Wang J, Wen L, Sun M, Liu H, Gao Y. Vinpocetine Attenuates Ischemic Stroke Through Inhibiting NLRP3 Inflammasome Expression in Mice. Journal of cardiovascular pharmacology. Dec 22 2020;77(2):208-216. doi:10.1097/FJC.0000000000000945
- Zhao M, Hou S, Feng L, et al. Vinpocetine Protects Against Cerebral Ischemia-Reperfusion Injury by Targeting Astrocytic Connexin43 via the PI3K/AKT Signaling Pathway. Front Neurosci. 2020;14:223. doi:10.3389/fnins.2020.00223
- Wu LR, Liu L, Xiong XY, et al. Vinpocetine alleviate cerebral ischemia/reperfusion injury by down-regulating TLR4/MyD88/NF-kappaB signaling. Oncotarget. Oct 6 2017;8(46):80315-80324. doi:10.18632/oncotarget.20699
- Zhang F, Yan C, Wei C, et al. Vinpocetine Inhibits NF-kappaB-Dependent Inflammation in Acute Ischemic Stroke Patients. Transl Stroke Res. Apr 2018;9(2):174-184. doi:10.1007/s12975-017-0549-z
- Feigin VL, Doronin BM, Popova TF, Gribatcheva EV, Tchervov DV. Vinpocetine treatment in acute ischaemic stroke: a pilot single-blind randomized clinical trial. European journal of neurology : the official journal of the European Federation of Neurological Societies . Jan 2001;8(1):81-5. doi:10.1046/j.1468-1331.2001.00181.x
- Kemeny V, Molnar S, Andrejkovics M, Makai A, Csiba L. Acute and chronic effects of vinpocetine on cerebral hemodynamics and neuropsychological performance in multi-infarct patients. J Clin Pharmacol. Sep 2005;45(9):1048-54. doi:10.1177/0091270005279363
- Bonoczk P, Panczel G, Nagy Z. Vinpocetine increases cerebral blood flow and oxygenation in stroke patients: a near infrared spectroscopy and transcranial Doppler study. Eur J Ultrasound. Jun 2002;15(1-2):85-91. doi:10.1016/s0929-8266(02)00006-x
- Szilagyi G, Nagy Z, Balkay L, et al. Effects of vinpocetine on the redistribution of cerebral blood flow and glucose metabolism in chronic ischemic stroke patients: a PET study. J Neurol Sci. Mar 15 2005;229-230:275-84. doi:10.1016/j.jns.2004.11.053
- Hill MD, Goyal M, Menon BK, et al. Efficacy and safety of nerinetide for the treatment of acute ischaemic stroke (ESCAPE-NA1): a multicentre, double-blind, randomised controlled trial. Lancet. Mar 14 2020;395(10227):878-887. doi:10.1016/S0140-6736(20)30258-0
- Slomski A. Alteplase Inhibits Nerinetide, a Novel Stroke Drug. JAMA. Apr 28 2020;323(16):1543. doi:10.1001/jama.2020.5631
- Gelderblom M, Leypoldt F, Lewerenz J, et al. The flavonoid fisetin attenuates postischemic immune cell infiltration, activation and infarct size after transient cerebral middle artery occlusion in mice. Journal of cerebral blood flow and metabolism : official journal of the International Society of Cerebral Blood Flow and Metabolism . May 2012;32(5):835-43. doi:10.1038/jcbfm.2011.189
- Rivera F, Urbanavicius J, Gervaz E, Morquio A, Dajas F. Some aspects of the in vivo neuroprotective capacity of flavonoids: bioavailability and structure-activity relationship. Neurotoxicity research. 2004;6(7-8):543-53. doi:10.1007/BF03033450
- Maher P, Salgado KF, Zivin JA, Lapchak PA. A novel approach to screening for new neuroprotective compounds for the treatment of stroke. Brain research. Oct 10 2007;1173:117-25. doi:10.1016/j.brainres.2007.07.061
- Wang L, Cao D, Wu H, Jia H, Yang C, Zhang L. Fisetin Prolongs Therapy Window of Brain Ischemic Stroke Using Tissue Plasminogen Activator: A Double-Blind Randomized Placebo-Controlled Clinical Trial. Clinical and Applied Thrombosis/Hemostasis. 2019;25:107602961987135. doi:10.1177/1076029619871359
- Liu CL, Zhang K, Chen G. Hydrogen therapy: from mechanism to cerebral diseases. Med Gas Res. Mar 2016;6(1):48-54. doi:10.4103/2045-9912.179346
- Li H, Luo Y, Yang P, Liu J. Hydrogen as a complementary therapy against ischemic stroke: A review of the evidence. J Neurol Sci. Jan 15 2019;396:240-246. doi:10.1016/j.jns.2018.11.004
- Ono H, Nishijima Y, Ohta S, et al. Hydrogen Gas Inhalation Treatment in Acute Cerebral Infarction: A Randomized Controlled Clinical Study on Safety and Neuroprotection. J Stroke Cerebrovasc Dis. Nov 2017;26(11):2587-2594. doi:10.1016/j.jstrokecerebrovasdis.2017.06.012
- American Stroke Association. Risk Factors Under Your Control. 6/17/2021. Accessed 4/19/2022. https://www.stroke.org/en/about-stroke/stroke-risk-factors/risk-factors-under-your-control
- Centers for Disease Control and Prevention. Physical Activity for Healthy Weight. 3/9/2022. Accessed 4/19/2022. https://www.cdc.gov/healthyweight/physical_activity/index.html
- Shahi S, Farhoudi M, Dizaj SM, et al. The Link between Stroke Risk and Orodental Status-A Comprehensive Review. J Clin Med. Oct 2 2022;11(19)doi:10.3390/jcm11195854. https://pubmed.ncbi.nlm.nih.gov/36233721/
- Chang Y, Woo HG, Lee JS, Song TJ. Better oral hygiene is associated with lower risk of stroke. J Periodontol. Jan 2021;92(1):87-94. doi:10.1002/JPER.20-0053. https://pubmed.ncbi.nlm.nih.gov/32432793/
- Leonov G, Salikhova D, Starodubova A, et al. Oral Microbiome Dysbiosis as a Risk Factor for Stroke: A Comprehensive Review. Microorganisms. Aug 22 2024;12(8)doi:10.3390/microorganisms12081732. https://pubmed.ncbi.nlm.nih.gov/39203574/
- Lin HW, Chen CM, Yeh YC, et al. Dental treatment procedures for periodontal disease and the subsequent risk of ischaemic stroke: A retrospective population-based cohort study. J Clin Periodontol. Jun 2019;46(6):642-649. doi:10.1111/jcpe.13113. https://pubmed.ncbi.nlm.nih.gov/30989681/
- Sen S, Marchesan J, Wood S, et al. Abstract 19: Dental flossing may lower the risk for incident ischemic stroke, cardioembolic stroke subtype and AF. Stroke. 2025;56(Suppl_1):A19-A19. doi:doi:10.1161/str.56.suppl_1.19. https://www.ahajournals.org/doi/10.1161/str.56.suppl_1.19
- Sen S, Curtis J, Hicklin D, et al. Dental Caries Associated with Incident Ischemic Stroke: Atherosclerosis Risk In Communities Study (4329). Neurology. 2021;96(15_supplement):4329. doi:doi:10.1212/WNL.96.15_supplement.4329. https://www.neurology.org/doi/abs/10.1212/WNL.96.15_supplement.4329
- Muric M, Nikolic M, Todorovic A, Jakovljevic V, Vucicevic K. Comparative Cardioprotective Effectiveness: NOACs vs. Nattokinase-Bridging Basic Research to Clinical Findings. Biomolecules. Aug 7 2024;14(8)doi:10.3390/biom14080956. https://pubmed.ncbi.nlm.nih.gov/39199344/
- Yang XY, Wang SL, Xue WC, et al. Nattokinase's Neuroprotective Mechanisms in Ischemic Stroke: Targeting Inflammation, Oxidative Stress, and Coagulation. Antioxid Redox Signal. Feb 2025;42(4-6):228-248. doi:10.1089/ars.2023.0527. https://pubmed.ncbi.nlm.nih.gov/39135387/
- Maslarov DD, D. Use of Nattokinase in Patients with Ischemic Stroke and Transient Ischemis Attacks. Neurol Neurosci. 2020;1(2). https://www.researchgate.net/publication/343905280_Use_of_Nattokinase_in_patients_with_ischemic_stroke_and_transient_ischemic_attacks
- Maslarov D, Drenska D, Maslarova-Gelov J, Gelov I. Understanding the concept of Nattokinase use: a few years after beginning. Biotechnology & Biotechnological Equipment. 2023/08/17 2023;37(1):2249552. doi:10.1080/13102818.2023.2249552 https://doi.org/10.1080/13102818.2023.2249552. https://www.tandfonline.com/doi/pdf/10.1080/13102818.2023.2249552
