
Stress Management
Stress Management
Last Section Update: 02/2025
Contributor(s): Maureen Williams, ND; Debra Gordon, MS; Shayna Sandhaus, PhD; Stephen Tapanes, PhD
Reviewers: Dr. Kathy Wilson, Ph.D., Psychology, NHD; Dr. Vanessa Pavey, ND; Julia Dosik, MPH;
Table of Contents
- Overview
- Introduction
- How Does The Body Respond to Stress?
- How Does Stress Cause Health Problems?
- What are the Health Consequences of Chronic Stress?
- Determining if Stress May be Affecting Your Health
- Medications for Temporary Stress Relief
- Lifestyle and Behavioral Techniques to Relieve Stress
- Food and Stress-How Does Diet Affect Stress?
- Nutrients
- Update History
- References
1 Overview
Summary and Quick Facts for Stress Management
- Stress is meant to be an adaptive response, and in the short term, it is healthy. But chronic, low-level psychological stress, which is so common in the modern world, can cause many health problems.
- This protocol will help you understand how the body reacts to stress and how long-term stress can damage health. You will learn about lab tests that help determine if stress is affecting your health, and discover several nutrients (such as the tea compound theanine), along with dietary and lifestyle changes, that can promote a healthy stress response.
What is Stress?
Stress generally occurs when external stimuli disturb the dynamic balance of the body’s physiological processes. A specialized signaling network called the HPA axis coordinates the body’s stress response.
Acute stress helps prime the body to respond to immediate, transient threats. Intermittent mild stress, such as exercise, is healthy and promotes positive adaptive changes. Chronic stress, however, causes maladaptive responses and dysregulated HPA axis function. This can contribute to many health problems by disrupting the circadian rhythm, promoting inflammation, altering the microbiome, and causing epigenetic changes.
Natural interventions such as adaptogens, L-theanine, B vitamins, and omega-3 fatty acids may help relieve stress and restore normal HPA axis function.
How Can I Determine If Stress is Affecting My Health?
- Lab tests (including cortisol, dehydroepiandrosterone [DHEA], salivary alpha-[α] amylase, and immunoglobulin A [IgA])
- Heart rate variability
What Dietary and Lifestyle Changes Can Help Relieve Stress?
- Cognitive-behavioral therapy
- Meditation and mindfulness
- Exercise
- Maintain good sleep hygiene, sufficient sleep duration, and consistent sleep patterns
- Maintain social connections and interact with friends and loved ones frequently, even using social media platforms to do so if circumstances limit face-to-face interaction
- Maintain sex hormone balance
- Eat more fruits and vegetables
- Eat breakfast regularly
- Minimize caffeine and alcohol intake
Can Medications Help Relieve Stress?
Many cases of stress can be managed with dietary and lifestyle interventions. However, in more severe cases when stress is contributing to other conditions, such as anxiety or insomnia, medications may be appropriate for short-term use to temporarily address the stress-related condition(s). It is important to understand that medications do not eliminate stress or the causes of stress, but simply provide temporary relief from some of the symptoms caused by stress.
- Antidepressants and anti-anxiety medications such as selective serotonin reuptake inhibitors (SSRIs) (eg, Prozac and Zoloft)
- Beta-blockers (eg, propranolol)
- Sedatives such as benzodiazepines (eg, Valium and Klonopin)
- Hydrocortisone
What Natural Interventions May Help Relieve Stress?
- B vitamins. B vitamin deficiencies are linked with multiple neuropsychiatric disorders. Supplementation with B vitamins has been shown to relieve stress and support normal HPA axis function.
- Vitamin C. Low intake and circulating levels of vitamin C are correlated with symptoms of depression and anxiety. Increasing vitamin C levels via supplementation has been shown to reduce symptoms.
- Omega-3 fatty acids. Omega-3 fatty acids, such as eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA) found in fish oil, may help improve various mood- and stress-related phenomena like anxiety, depression, and aggression.
- L-theanine. L-theanine, an amino acid found in tea, has been shown to reduce perceived stress and physiological markers of the stress response.
- Bioactive milk peptides. Peptides found in milk, such as α-lactalbumin and casein, may support healthy neurological function, improve mood, and promote sleep.
- Probiotics and prebiotics. Probiotics and prebiotics can improve the balance of gut bacteria and have a positive impact on the stress response. Probiotics may lower stress reactivity and anxiety, and improve mood, memory, and cognition.
- Adaptogens. Adaptogenic herbs help support homeostasis in the body and can be used to relieve fatigue, improve cognitive function and mood, and support the immune system.
- Magnolia and phellodendron. This herbal combination has been found to reduce stress and stress-related weight gain.
- Holy basil. Several clinical and preclinical studies have demonstrated holy basil’s ability to improve mood and cognition.
- Ashwagandha. Ashwagandha has been shown to relieve stress, improve stress-related eating behaviors, and promote weight loss.
- Lemon balm. Lemon balm has been found to improve mood and cognition and relieve symptoms of anxiety and insomnia.
- Additional adaptogens that may help relieve stress include bacopa, saffron, ginseng, rhodiola, and cordyceps, and others.
- Other natural interventions may help relieve stress, including phosphatidylserine, L-tryptophan, melatonin, and dehydroepiandrosterone (DHEA).
2 Introduction
Over the course of evolutionary time, the human body has become reliant on the acute stress response to overcome short-term adversity. But human physiology is simply not adapted to the relatively modern phenomenon of unrelenting low-level stress. Consequently, we now face a plethora of health problems to which chronic stress is a contributing factor.1,2
Many types of events and circumstances can be perceived as stressful. Events such as natural disasters, violence, war, and traumatic accidents are stressful to everyone they impact and are important causes of stress-related mental health problems that can affect whole communities.393 Other personal events such as divorce, job loss, critical or chronic illness, and bereavement affect people differently but are common causes of chronic stress in individuals.394-397
A key physiological feature of chronic stress is dysregulation of the hypothalamic-pituitary-adrenal (HPA) axis, a network of signaling centers in the brain and body that modulates our physiological response to stress. Normal activation of the HPA axis is necessary for healthy adaptive responses to stressors, but chronic activation leads to a maladaptive stress response marked by changes in the release and activity of the stress hormone, cortisol, which contributes to stress-related illness.2,3 Interactions between the HPA axis and the central nervous system, immune system, and gut microbiome contribute the wide-ranging effects of stress on overall health.4,5
The good news is that making healthy lifestyle decisions and adhering to a healthy diet can enhance resistance to the detrimental effects of chronic stress.4-6 In this protocol, you will learn how chronic stress causes health problems and how you can improve your ability to cope with stress and fortify yourself against the negative health effects of our stressful modern world.
3 How Does The Body Respond to Stress?
The Fight or Flight Response
Stress generally occurs when external stimuli disturb the dynamic balance of the body’s physiological processes.7 The stress, or “fight or flight,” response begins in the brain, where a perceived threat triggers the release of corticotropin releasing hormone (CRH) from the region called the hypothalamus. This stimulates the anterior pituitary, a gland that sits just under the hypothalamus, to increase release of adrenocorticotropic hormone (ACTH) into the bloodstream. ACTH then acts on the adrenal cortex, raising production and release of cortisol and the less active glucocorticoid, corticosterone, as well as another adrenal hormone called dehydroepiandrosterone, or DHEA.8
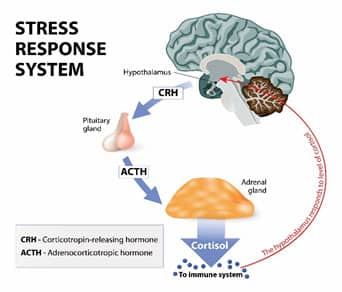
The signaling network between the nervous system and adrenal glands, called the hypothalamic-pituitary-adrenal (HPA) axis, is regulated in part by a negative feedback mechanism, through which rising blood levels of cortisol inhibit release of both CRH and ACTH.3,9
Stress also directly engages sympathetic nervous system signaling in the brain region called the locus coeruleus. Catecholamine neurohormones (epinephrine and norepinephrine, also known as adrenaline and noradrenaline) released by the adrenal medulla and sympathetic nerve endings have physiologic effects intended to help the body respond and adapt to stressful circumstances. Although it tends to work in concert with the HPA axis, the sympathetic nervous system also functions independently to activate the stress response.3,9
Acute Stress
As mediators of the stress response, cortisol and catecholamines have profound effects throughout the body (see Table 1). When acutely elevated, they help prepare the body to escape danger. For example, cardiac output increases to support stronger blood flow; blood sugar levels increase to meet higher energy demands; pupils dilate to allow for greater visual input; alertness and cognition are enhanced; and digestive and reproductive functions are inhibited due to their not being essential in the short term.9
Table 1: Hidden Causes of Acute Stress
|
Physiological Stressor |
Acute Adaptive Stress Response |
|
Low blood glucose level10,11 |
Catecholamines stimulate breakdown of carbohydrate stores and conversion of protein and fat into glucose Cortisol inhibits glucose use by non-central nervous system tissue |
|
Low blood pressure3,12 |
Catecholamines stimulate constriction of blood vessels Cortisol increases sodium and water retention in the kidneys |
|
Low oxygen saturation3,13,14 |
Catecholamines stimulate the respiratory center of the brain to increase breathing, increase heart rate and contraction strength, and selectively constrict blood vessels |
|
Oxidative stress15 |
Catecholamines and cortisol alter cell metabolism to restore reductive-oxidative balance |
|
Inflammatory cytokines1,16 |
Catecholamines and cortisol modulate immune activities |
Chronic Stress
The acute stress response can lead to positive adaptive effects, but when the HPA axis and locus coeruleus are chronically activated, their effects become maladaptive: the response to a chronic or repeated stress may become dull, yet, at the same time, sensitivity to new stressors may be enhanced.12,17 A dysregulated stress response results in altered patterns of cortisol and catecholamine production and/or receptor response to them.3,9 Chronic stress may even alter brain structure.18 In addition, impairment of the HPA axis due to chronic stress appears to suppress DHEA production and its release, even under acutely stressful circumstances.8,19 This is important because DHEA opposes some of the actions of cortisol: it protects nerves and stimulates development of neuronal connections, has immune-regulating effects that oppose and balance those of cortisol, and may prevent cortisol-induced metabolic disturbances.8 The exact nature of the response to chronic stress depends on individual characteristics such as personality traits, gender and age, life experiences, and genetic and epigenetic factors.3
4 How Does Stress Cause Health Problems?
Prolonged stress is associated with many chronic disorders and diseases affecting all of the body’s organ systems. As life’s stressors take their toll on the psyche and body, chronic illness itself becomes a source of stress. The two-way relationship between stress and disease creates a downward spiral in mental and physical health that can become difficult to overcome.2
Stress and the Circadian Rhythm
The HPA axis is closely regulated by circadian signaling in the brain. This circadian signaling is affected by day and night (light and dark) cycles, patterns of eating times, and most likely other factors yet to be discovered. Normally, cortisol levels peak shortly after waking in the morning and are lowest around bedtime. By acting on receptors throughout the body, cortisol imposes diurnal (two-phase; day-night) rhythms to other physiological functions.17,25
Numerous studies have shown that disruption of the circadian clock, such as due to shift work, sleep apnea, and other sleep disorders, is associated with health problems including cardiovascular disease, type 2 diabetes, obesity, and an array of age-related diseases.26,27 Circadian disturbances may even correlate with reduced lifespan.28 Chronic stress appears to impair circadian control of the HPA axis, which can result in either excess evening levels or blunted morning levels of cortisol.29 These dysfunctional patterns of cortisol release may be an underlying factor in the negative physical and mental health consequences of chronic stress and circadian rhythm disruption.30
Stress and the Immune System
One important way that chronic stress affects long-term health is through dysregulated immune signaling. Although cortisol is best known for its immunosuppressive action, its effects on immunity are complex, stimulating some aspects of immunity and inhibiting others.1,25 A phenomenon known as glucocorticoid resistance, in which tissues and cells become less responsive to cortisol, occurs following long-term elevation of cortisol levels due to chronic stress.31,32
Chronic stress-induced immune dysfunction results in reduced immune protection against infections and cancer. Chronic stress, particularly when it involves interpersonal relationships or work, has been consistently correlated with increased risk of respiratory infections such as influenza and the common cold.406-408 Studies have also shown persistently high levels of perceived stress and cortisol are associated with a heightened inflammatory response to pathogens, due at least in part to glucocorticoid resistance. This heightened inflammatory response results in increased susceptibility to infection, tissue damage, and symptom severity.408-410 In one study, participants with higher cortisol production not only had increased risk of the common cold but also more days of viral shedding, indicating longer duration of infection and possibly transmissibility.411
Stress has also been implicated as a contributing factor in inherently inflammatory conditions, such as allergic and autoimmune disorders, and conditions related to low-level systemic inflammation like heart disease and diabetes.1,33 Once inflammation is initiated, it perpetuates the stress response through the actions of cytokines (small signaling proteins of the immune system) on the hypothalamus, pituitary, and adrenal cortex.25,34
Stress and the Microbiome
Chronic stress may impact health through interactions with the gut microbiome—the trillions of microorganisms that reside in the intestines. Through its relationship with nervous system signaling, often referred to as the “gut-microbiota-brain axis,” and its ability to regulate the immune system, a healthy microbiome appears to be essential for modulating stress responsiveness and preventing overstimulation of the HPA axis. Conditions associated with chronic stress have been shown to alter the composition of the gut microbial community. Microbial imbalances, in turn, can cause intestinal and systemic inflammation and abnormal neurological signaling that can trigger HPA activation.35-38
The Epigenetics of Stress
Exposure to stress early in life can alter stress responsiveness and resilience throughout life. Part of this is likely due to effects of stress on brain and adrenal gland development; another important element is epigenetics. Epigenetics refers to environmentally induced modifications to gene expression patterns (as opposed to changes in gene sequence) or factors that control how genes are used to direct protein synthesis in cells. These modifications are lasting but can be reversed by future circumstances.39
The epigenetic changes induced by prenatal and early life stress result in hyperresponsiveness of the HPA axis and increased risk of neuropsychiatric problems in adulthood, such as depression, anxiety, and post-traumatic stress disorder.39-41 Emerging research has shown that stress-induced epigenetic changes can also occur in adulthood, affecting HPA axis responsiveness and increasing vulnerability to stress-related health problems.42 In addition, because the epigenome is passed on to offspring by both parents, exposure to intense or unremitting stress has implications for resilience and health that may span multiple generations.41,43,44
5 What are the Health Consequences of Chronic Stress?
Chronic stress can exert considerable body-wide health effects. It can contribute to the onset or worsening of many types of ailments. The following discussion highlights some of the more common conditions to which chronic stress often contributes.
Cardiovascular Disease
One of the most widely recognized health effects of chronic stress is heart disease. Through the effects of cortisol and catecholamines, and by disrupting circadian rhythms through sleep disturbance, chronic stress has been shown to impair nervous system regulation of cardiac function,49 and can cause high blood pressure, arrhythmia, and vascular inflammation leading to atherosclerosis and blood clots.50 Prolonged stress at home and at work has been clearly linked to increased risk of coronary artery disease and cardiac events including heart attack and stroke.12,51 A recent meta-analysis highlights the influence of work stress on heart disease risk: after analyzing data from more than 740,000 men and women, researchers found that people who work 55 or more hours per week have a 12% increased risk of coronary artery disease and a 21% increased risk of stroke compared with those who work less.52
Acute stress can also pose a threat to the heart. Studies have noted the incidence of heart attack increases following acutely stressful events such as earthquakes and World Cup soccer championships.53 Takotsubo cardiomyopathy, a sudden weakening of the heart muscle that mimics the symptoms of heart attack or angina and is potentially fatal, is another example of the danger of acute stress to the heart. Also known as stress cardiomyopathy, broken heart syndrome, and apical ballooning syndrome, Takotsubo cardiomyopathy typically occurs a few hours after a severe physical or emotional trauma and is most common in postmenopausal women.54,55
Psychiatric and Neurological Disorders
Chronic stress is closely associated with several common neuropsychiatric disorders, including depression, anxiety, dementia, and Alzheimer disease.
Inflammation in the brain triggered by stress-related signaling is an important factor linking stress to neuropsychiatric disorders.57 In Alzheimer disease, stress-related immune dysfunction appears to weaken the brain’s ability to clear amyloid-beta, a protein involved in Alzheimer disease development and progression.58,59 In addition, persistently high cortisol levels, a marker of chronic stress, can trigger changes to neuronal structure and reduce brain plasticity (the ability to make new neuronal connections).56 Early life, repetitive, or chronic stress may also reduce the activity of nerve growth factors, especially brain-derived neurotrophic factor (BDNF), involved in the formation of new nerve connections.60-62 Low levels of BDNF are associated with mood disorders as well as learning and memory deficits.62 Furthermore, these stress-related changes may be encoded epigenetically, altering nerve system plasticity and function in lasting ways.63
Cancer
A growing body of evidence suggests that the neurohormones of the stress response can promote the initiation and progression of cancer.64,65 Furthermore, chronic stress may be associated with behaviors, such as smoking, substance abuse, overeating, and decreased physical activity, that increase the risk of certain cancers.66,67 Coping with a cancer diagnosis, symptoms, and treatment is inherently extremely stressful for some individuals,68,69 yet a high burden of stress may negatively impact response to cancer treatment and prognosis.64,70,71
The mechanism by which stress influences cancer is likely to be multifaceted, but the cornerstone may be immune dysregulation, marked by decreased immune surveillance and systemic inflammation. HPA axis dysregulation suppresses immune defenses against cancer, and chronic systemic inflammation creates conditions that support cancer initiation, progression, and metastasis.72,73 Inflammation may stem from other stress-induced sequelae, including weight gain and metabolic disturbance, disruption of the gut microbiome, and epigenetic alterations72; in turn, inflammation can contribute to these processes.74 In addition, stress may affect cancer development by desynchronizing circadian regulation of biological activities.29,75
Metabolic Disturbance: Why Does Stress Make it Hard to Lose Weight?
One of the most important functions of the stress response is to ensure that adequate energy is available to cope with stressful circumstances. During episodes of acute stress, appetite is suppressed to reserve attention for fight or flight, and extra energy in the form of glucose is freed from stored fats and carbohydrates. Under conditions of chronic stress, however, appetite is typically up-regulated and cravings for high-sugar, high-fat, high-calorie foods can intensify as a result of long-term hyperstimulation of the HPA axis and its complex interactions with appetite-regulating neurohormones such as ghrelin and leptin. For reasons that are not entirely clear, an increased appetite as a reaction to chronic stress is more pronounced in women than men.10,76
To make matters worse, chronic stress and HPA axis dysregulation are associated with insulin resistance and type 2 diabetes, as well as fat tissue growth and obesity.77,78 In one study, salivary cortisol tests showed disturbances in the diurnal rhythm of cortisol release correlated with body mass index (BMI) and waist circumference, a measure of visceral fat and one of the cardiovascular risk factors in metabolic syndrome.79 These metabolic consequences of long-term stress then promote widespread inflammatory signaling that damages blood vessels and increases cardiovascular risk.80,81 Systemic inflammation also affects the nervous system, contributing to mood and cognitive disorders, and creates a vicious cycle of increased HPA axis activation.10,82
Although widely believed that chronic stress can lead to weakened thyroid function, there is little evidence as of the date of this writing to support this notion. In one study, hair cortisol levels were higher in adults with overt hypothyroidism than in healthy adults, and were correlated with higher body weight and BMI; however, in participants with subclinical hypothyroidism, a condition characterized by normal to slightly abnormal lab values and possibly symptoms of hypothyroidism, hair cortisol levels were not significantly different from those of healthy participants.83 Findings from preliminary studies indicate stress may contribute to the onset of autoimmune hypothyroidism; however, a review of these studies was unable to confirm the connection.84 On the other hand, evidence from animal studies suggest hypothyroidism may trigger HPA axis dysregulation and, when chronic, reduce adrenal output.85,86
Additional Health Conditions Stress Can Worsen
Virtually any health condition can be negatively affected by stress. In addition to those already discussed, the following are some of the disorders and diseases that stress may impact:
- Asthma87
- Atopic dermatitis88
- Autoimmune diseases89
- Chronic fatigue syndrome90
- Upper and lower respiratory infections91
- Infertility92
- Irritable bowel syndrome93
- Migraine94
- Pain disorders95,96
- Sexual dysfunction97
6 Determining if Stress May be Affecting Your Health
Although the effects of chronic stress can vary among individuals, several laboratory and clinical assessments can help determine if stress may be contributing to health problems. Objective tests that may be helpful in assessing the extent to which stress is affecting overall health include cortisol, DHEA level, salivary alpha-[α] amylase and immunoglobulin A (IgA) levels, and heart rate variability.
Cortisol
Measuring cortisol levels can be helpful in assessing HPA axis function. Cortisol levels in saliva, blood, urine, and hair have been shown to be reliable markers of adrenal cortisol output.98,99 These tests are widely available and are sometimes used as indicators of HPA axis function. In general, long-term increased cortisol output, reflecting over-activity of the HPA axis, is typical in major depression, while decreased cortisol output, reflecting under-activity of the HPA axis, is typical in chronic fatigue syndrome and post-traumatic stress disorder.100
- Salivary cortisol is a non-invasive test that may be helpful in determining whether the circadian rhythm of adrenal gland function is intact or disturbed. Late night salivary cortisol is sometimes used to diagnose Cushing syndrome (a condition caused by excess exposure to cortisol or drugs that mimic cortisol). However, tests that measure cortisol levels at multiple times in a day, creating a curve that reflects the diurnal pattern of
cortisol release, may have broader usefulness in assessing stress.101,102 One research review found that flatter diurnal cortisol curves are correlated with poorer health.103
Cortisol levels rise gradually with age and are affected by gender, especially around puberty and in the elderly. Although every lab determines its own reference ranges, peak salivary cortisol levels (within the first hour after waking) in adults appear to range from 1.8 to 26 nmol/L, and evening trough levels (about 16 hours after waking) range from 0.2 to 3.5 nmol/L.104 - Hair cortisol concentration is a novel and non-invasive method of evaluating long-term cortisol exposure over months to years. Because stress levels can fluctuate over time, cortisol is generally measured in the three centimeters of hair closest to the scalp (reflecting HPA axis activity during the previous three months).105 Cortisol concentrations in scalp hair have been found to vary with psychological and physical stressors, and have been correlated with perceived stress and stress-related symptoms and illnesses, including obesity, metabolic syndrome, and cardiovascular disease.99,106
Salivary Alpha [α]-Amylase and Immunoglobulin A (IgA)
Alpha [α]-amylase is a starch-digesting enzyme produced in the salivary glands as well as the pancreas. Production of salivary α-amylase increases under stimulation by the sympathetic nervous system, which triggers the “fight or flight” reaction and has a critical role in the stress response. On the other hand, production of salivary proteins like α-amylase and the antibody immunoglobulin A (IgA) is inhibited by the parasympathetic nervous system, which controls resting body functions. Therefore, salivary α-amylase and salivary IgA have been proposed as markers of the balance of nervous system regulation and objective measures of stress.107-109
Numerous studies show that α-amylase increases as a result of physical and psychological stress, and high levels have been seen in stress-related conditions such as anxiety.107,110 It is sometimes tested along with salivary cortisol, which reflects HPA axis activity, to provide a more comprehensive assessment of stress. Although not performed routinely, evidence suggests this combination of salivary tests may be useful for non-invasively and objectively evaluating the contribution of stress in patients with chronic conditions111 and monitoring the effects of stress-reducing therapies.112
Salivary secretory IgA (sIgA) has also been proposed as a marker of stress. A number of studies have shown that acute stress can increase levels of this important antibody.113-115 With chronic stress, however, sIgA appears to be depleted and salivary levels drop,116,117 possibly increasing risk of oral, gastrointestinal, and respiratory infections.118 Interpretation of salivary sIgA is somewhat challenging due to its sensitivity to other factors in the oral environment.119
Salivary sIgA and α-amylase tests are commercially available and frequently recommended and interpreted by integrative health care providers. In general, standardization of these salivary tests and more information about factors that interfere with their interpretation, such as smoking, food and beverage consumption, and medication use, will help increase their usefulness and acceptance.108,119,120
DHEA
Dehydroepiandrosterone (DHEA) is an adrenal hormone that opposes some of the actions of cortisol in many tissues. Acute stress can increase production of both DHEA and cortisol in healthy individuals, but chronic stress has been correlated with low DHEA and high cortisol output.8 In one study, levels of DHEA-S (DHEA-sulfate, the form of DHEA typically measured in the blood) were 23% lower in healthy adults with the highest perceived work-related stress compared to those with the lowest work-related stress.121 The balance between cortisol and DHEA production also varies dramatically with age: DHEA release is lowest in older age, and it is thought that the unabated action of cortisol in the presence of declining amounts of DHEA may contribute to age- and stress-related diseases.8,122,123
Evidence suggests blood levels of DHEA-S that generally correspond with optimal health are 350–500 µg/dL for men and 275–400 µg/dL for women. Measuring the ratio of serum cortisol to DHEA-S may also provide some insights into the function of the adrenal gland and stress resilience.8
Heart Rate Variability
The heartbeat is not a precisely regular rhythm but instead oscillates unpredictably over time in response to dynamic shifting in the balance of sympathetic and parasympathetic regulation. Heart rate variability is the fluctuation in the length of time between heartbeats.124 In a healthy person at rest, when the parasympathetic nervous system is the predominant heart rhythm regulator, heart rate variability increases, but during times of stress, when the sympathetic nervous system is strongly activated, heart rate variability decreases. Like salivary α-amylase, heart rate variability at rest provides information regarding the stress-related activity of the nervous system.125 Greater variability in heart rate reflects more robust ability to adapt to changing conditions.124
A growing body of evidence shows that resting heart rate variability is a meaningful reflection of cardiac and nervous system activity.124,125 Low heart rate variability has been noted to be closely correlated with other measures of stress and is an indicator of low stress-resilience and increased risk of heart attack and overall mortality.125-128 Furthermore, stress management strategies like exercise and mindfulness practices can improve heart rate variability. 128,129 Taken together, the evidence suggests heart rate variability may prove helpful in predicting risk of stress-related physical and psychological disorders.126,130
Heart rate variability is measured during long (24-hour), short (five-minute), or ultrashort (shorter than five-minute) monitoring periods. At this time, 24-hour data sets are considered the “gold standard” and seem to offer a better reflection of health status. Questions remain about the significance of short- and ultrashort-term heart rate variability measurements, ideal timing of data collection, frequency of oscillations, and the influence of individual factors such as gender, disease status, and medication use on heart rate variability measurements.124 Nevertheless, devices that measure heart rate variability are increasingly commercially available.
7 Medications for Temporary Stress Relief
Although there are no medications specifically indicated to treat stress, it is a major contributor in some individuals to anxiety, depression, insomnia, or other psychological or psychiatric disorders that may be treatable with antidepressants, sedatives, and anti-anxiety medications. In addition, some stress-related health problems may be responsive to treatment with the cortisol analog hydrocortisone.
It is important to note that, in most cases, these medications are not indicated for stress relief specifically and should be used only temporarily. In the majority of people suffering from chronic stress, the stress management techniques and dietary measures described later in this protocol are the best options for reducing stress-related symptoms and increasing stress resilience.
Antidepressants and Anti-Anxiety Medications
Selective serotonin reuptake inhibitors (SSRIs) and serotonin and noradrenaline reuptake inhibitors (SNRIs) are antidepressants widely prescribed to treat depression and anxiety and are a consideration for patients with stress-related mood disorders. For example, the SSRIs paroxetine (Paxil) and sertraline (Zoloft), and the SNRI venlafaxine (Effexor) in particular have demonstrated benefits in treating social anxiety disorder.134 Case studies suggest the SNRI tramadol (Ultram) can effectively reduce psychological stress and may be useful taken as needed rather than daily.135 However, these medications may cause dependence, have low success rates in achieving remission from anxiety or depression, and are associated with side effects such as nausea, sexual dysfunction, weight gain, insomnia, headache, fatigue, and anxiety.136
Buspirone (Buspar) is an anti-anxiety medication that enhances the activation of serotonin receptors known as 5-HT1A receptors. Buspirone has also been found to stimulate the HPA axis and raise catecholamine levels.137 Results from animal research suggest it may have a role in treating stress-related anxiety and depression138; however, buspirone can cause adverse side effects such as restlessness, nervousness, poor concentration, difficulty sleeping, drowsiness, and tiredness or weakness.139
Trazodone (Desyrel) is classified as an atypical antidepressant. Its main adverse effect is sedation, and this has led to its use as a sleep aid.136 Other non-FDA-approved indications for which trazadone is used include anxiety, panic disorder, and post-traumatic stress disorder, although its efficacy in these conditions has not been established.140,141
Beta Blockers
Beta blockers are drugs that inhibit catecholamine receptors called beta-adrenergic receptors, thereby suppressing sympathetic nervous system signaling.142 These medications are mainly used to treat high blood pressure, arrhythmia, angina, and heart failure, and are part of post-heart-attack maintenance. Certain beta blockers are also used to treat glaucoma, migraines, essential tremor, and cardiac symptoms of hyperthyroidism.143,144
Propranolol (Inderal) is a beta blocker sometimes used to prevent acute stress in individuals with situational anxiety such as exam anxiety, stage fright, performance anxiety, and fear of surgery.143,144 For these uses, it is typically taken intermittently and in single doses. It does not appear to be effective in treating long-term anxiety disorders such as stress-induced or generalized anxiety disorder, but controlled trials are lacking.142 Furthermore, there are concerns that long-term propranolol use, even for cardiovascular indications, may increase the risk of depression.145
Sedative Medications
Benzodiazepines are a category of fast-acting sedative medications that, despite limited approved uses, are often prescribed for patients with anxiety disorders including stress-induced anxiety and insomnia.134,146,147 These medications enhance the action of GABA, a neurotransmitter that quiets nerve conduction and may suppress activation of the HPA axis.147 Examples of benzodiazepines are diazepam (Valium), lorazepam (Ativan), and clonazepam (Klonopin). In a rat model of psychosocial stress, both lorazepam and clonazepam reduced stress-related inflammation in the central nervous system and decreased behaviors associated with stress-induced anxiety and depression.148
Benzodiazepines are associated with a host of problems including confusion and falls, cognitive impairment, withdrawal symptoms, dependence, and abuse. Their use also increases pneumonia risk in older patients. In addition, they are known to interact with many medications, alcohol, and other substances. Benzodiazepines are only indicated for short-term use.147,149
Non-benzodiazepine sedatives used for insomnia include zopiclone (Imovane), eszopiclone (Lunesta), zolpidem (Ambien), and suvorexant (Belsomra). While it is thought these options may be less addictive than benzodiazepines, their long-term use for insomnia may still be associated with cognitive impairment, falls, dependence and abuse, decreased quality of life, and increased risk of pneumonia in older adults.149-151
8 Lifestyle and Behavioral Techniques to Relieve Stress
People experiencing high levels of stress and its health effects will undoubtedly fare better by reducing their exposure to high-stress circumstances. For many people, however, stress at home or on the job can seem unavoidable. In such cases, a healthy diet, exercise, and stress management practices can have a strong positive impact on normalizing the stress response and preventing stress-related illness.
Cognitive-Behavioral Therapy
Cognitive-behavioral therapy (CBT) refers to a group of patient-centered techniques focused on changing thought patterns associated with emotional distress and harmful behaviors. A large body of clinical studies show CBT is an effective strategy for managing general stress and relieving anxiety. 155 In a 2018 clinical trial, 100 subjects suffering from chronic stress were assigned to participate in a 12-week internet-based CBT intervention or be placed on a waitlist. After six months, measures of perceived stress and stress-related symptoms were lower in those who received the intervention.156 CBT was found in another study to be similarly effective to mindfulness-based stress reduction (described later in this section) in reducing stress and burnout in parents of children with chronic conditions.157
A recent research review showed CBT is moderately effective for treating stress- and anxiety-related psychological disorders.158 CBT has also been recommended as a treatment strategy for stress-mediated chronic pain.159,160 In a study in 46 women with fibromyalgia (a chronic pain condition), a six-month CBT intervention led to improved sense of control over life and increased coping behaviors, and decreased measures of depression, exhaustion, and stress behaviors; these benefits were maintained and enhanced one year after initiation of the intervention.161
Some stress-affected people may be more likely to benefit than others: researchers have noted that factors such as working night shifts, high burnout scores, and elevated inflammatory marker levels may reduce the efficacy of CBT.162
Meditation and Mindfulness
Meditation helps regulate the stress response, reduce chronic inflammation, and maintain a healthy gut microbiome, and numerous studies indicate its potential benefits in treatment and prevention of diverse health disorders. 4 Studies in veterans with post-traumatic stress disorder have shown practicing meditation not only improves patterns of cortisol release but also triggers epigenetic changes that might also contribute to its positive impacts on the stress response.163,164
A review of 45 studies found that meditation lowers cortisol output, blood pressure, heart rate, triglycerides, and inflammatory marker levels, indicating its potential for protecting cardiovascular health. 165 The American Heart Association issued a statement in 2017 recognizing meditation’s possible role, alongside smoking cessation and treatment of high blood pressure and high cholesterol, in reducing the risk of heart disease.166
Mindfulness-based stress reduction is a structured program that incorporates meditation, body awareness, and gentle yoga, with an emphasis on awareness of the present moment. The benefits of mindfulness-based stress reduction on various psychological and physical health outcomes have been widely reported.6 For example, reviews of studies on healthcare providers and other types of workers have shown that mindfulness-based interventions can increase well-being and reduce anxiety, depression, and burnout, and may improve work performance.167-170 In a controlled trial in overweight and obese women, a four-month mindfulness program led to reductions in stress-related eating behaviors and prevented weight gain.171 Mindfulness programs are usually conducted in person, but the effectiveness of online mindfulness-based stress reduction programs is gaining interest, with positive effects being reported in recent clinical trials.172-174
Exercise
For many people, stress reduces the desire and motivation to engage in physical activity, yet exercise can improve stress resilience175 and has been shown to reduce symptoms in people with anxiety and stress-related disorders.176
Exercise appears to stimulate anti-inflammatory and anti-stress reactions in the body.177 Engaging in regular exercise improves the body’s ability to adapt to stress and has been correlated with better recovery from illness and surgery.175 Exercise is associated with better sleep,178 less anxiety and depression,179,180 and lower stress reactivity in the nervous and cardiovascular systems. 181 A review of the research concluded that approximately 50 minutes per day of moderate intensity exercise is associated with the greatest mental health benefits compared with lower or higher doses; however, sedentary hours erode some of physical activity’s positive mental health effects.182 Clinical evidence also suggests strength training may improve anxiety, depression, and sleep.183,184
Exercise may mitigate stress-related eating behaviors: a number of trials have indicated that even 15-minute bouts of brisk walking can reduce stress-eating in the short term.161 In addition, regular exercise can help prevent or reverse the metabolic, inflammatory, and neurological consequences of chronic stress,66,185,186 and numerous studies support the current World Health Organization recommendation to engage in at least 150 minutes per week of moderate-intensity physical activity as an effective means of reducing death from all causes.187
Activity tracking tools may be useful and effective in incorporating exercise into a stress management protocol.188,189 In a 2016 preliminary study, 35 sedentary overweight participants were enrolled in a 12-week walking program in which they used pedometers to count the number of steps taken each day. The 30 participants who successfully achieved the goal of 10,000 steps per day not only lost weight and decreased their waist circumference, they also had lower scores on tests of anxiety, depression, fatigue, confusion, anger, and overall mood distress than at the beginning of the study.190 In another trial, increasing physical activity by using a step-counting activity tracker plus a goal setting intervention reduced depressive symptoms in female participants.191
Social Support
A strong social support network can buffer perception of stress and is one of the key factors for maintaining stress resilience throughout life.424,425 As a characteristic of resilience, social support helps protect against the negative impacts of stress on immune function and inflammation.425 Although individuals differ in the amount and type of social interaction they benefit from, studies have consistently shown that social integration through contact with friends and family and membership in a religious community and other groups improves physical and mental health and extends lifespan.426 In mothers with stressful occupations, building social networks has been found to improve mental health and cortisol levels.427 In family caregivers of dementia patients, strong social support was linked to lower sense of burden and increased resilience.428 Studies in first responders and intensive care unit nurses have shown that perception of strong social support is associated with reduced symptoms of post-traumatic stress disorder.429-431 In a study examining the effects of a formal social connection program, those who provided social support reported experiencing similar increases in well-being to those receiving support during a period of stress.432
Maintain Sex Hormone Balance
The physiologic stress response is strongly influenced by sex hormones (testosterone, estrogen, and progesterone), and gender-related differences in reactions to stress have been widely documented. Although the relationship is complex, stress-induced activation of the HPA axis, in general, is stronger in women than men. Evidence from animal research suggests this may be due to opposite effects of testosterone and estrogen on HPA axis sensitivity: estrogen increases HPA axis responsiveness while testosterone decreases it.201,202 In addition, progesterone appears to suppress sensitivity of the HPA axis and downregulate anxiety.203,204 Furthermore, while acute stress appears to increase progesterone production,204 chronic stress inhibits release of all sex hormones.202 Higher progesterone levels in the second half of the menstrual cycle have been associated with lower levels of premenstrual aggression, irritability, and fatigue in another study.205
In postmenopausal women, whose estrogen and progesterone levels are naturally low, hormone therapy has been shown to affect regulation of the stress response and may enhance some aspects of cognitive function during stress. In one study, 15 sedentary postmenopausal women who had used long-term hormone replacement therapy were compared with 15 similar women who had never used hormone therapy. Those who had never used hormone therapy were found to have abnormal diurnal salivary α-amylase patterns, while hormone therapy users had normal α-amylase patterns. In addition, hormone therapy non-users had less of a rise in salivary α-amylase concentration in response to exercise than hormone therapy users. This suggests long-term hormone therapy may help maintain normal tone of the sympathetic nervous system.206 On the other hand, another trial found that postmenopausal women using estradiol therapy had a reduced cortisol response and less reduction in working memory after exposure to physical stress compared with women receiving placebo.207
In a preliminary study in 94 postmenopausal women under chronic stress due to caring for a family member with dementia, hormone therapy was correlated with better psychosocial function: those using hormone therapy reported less hostility and fewer negative interactions with members of their support teams than those not using hormone therapy; the greatest benefit was seen in those using both estradiol and progesterone.208
Progesterone therapy alone can help perimenopausal women with symptoms including hot flashes, breast pain, and sleep problems.209,210 Because these symptoms may be a source of stress, progesterone therapy may have anti-stress benefits in peri- and postmenopausal women. Furthermore, animal research suggests progesterone may protect the brain from harmful stress-induced inflammation.211
Taken together, these findings suggest that maintaining balanced sex hormone levels throughout life may be important for regulating stress responsiveness and promoting resilience. Men and women with possible hormone imbalances should review Life Extension’s Male Hormone Restoration and Female Hormone Restoration protocols.
9 Food and Stress-How Does Diet Affect Stress?
Stress is well known to trigger changes in eating behaviors, often increasing appetite for unhealthy “comfort” foods like those high in sugar and fat.212 One reason may be that stress alters levels of appetite-regulating hormones, ghrelin and leptin, producing more hunger signaling.213 Although not everyone eats more in response to stress (about 40% of individuals eat more, 40% eat less, and 20% eat the same number of calories when under stress), a stress-induced rise in preference for high-sugar foods has been consistently observed and may be partly due to a dampening effect of sugar on the stress response.214-217 Compounding the problem, stress appears to increase susceptibility to diet-related metabolic disturbances like abdominal obesity and insulin resistance.218
Countering stress-related appetite changes and food cravings is challenging; however, eating a healthy diet may be even more important during times of stress. Healthy eating habits can help ensure adequate intake of vitamins, minerals, protein, complex carbohydrates, anti-inflammatory fats, fiber, and phytochemicals needed to combat the negative health effects of chronic stress and interrupt the cycle of stress and stress-related behaviors.219,220
Eat More Fruits and Vegetables
Increasing fruit and vegetable intake can help combat stress. A study in young adults showed that increasing fruit and vegetable intake by two servings per day for two weeks resulted in enhanced psychological well-being, vitality, flourishing, and motivation.221 A Mediterranean-style diet, which emphasizes olive oil, whole grains, fruits, vegetables, fish, and nuts and seeds, may improve the stress response and has been associated with better regulation of HPA axis activity. This dietary pattern may also mitigate the effects of stress by reducing systemic inflammation and the risk of many chronic health problems.222-224
Eat Breakfast Regularly
Eating breakfast may help build stress resilience. Compared to breakfast skipping, habitual breakfast eating was associated with lower levels of perceived stress, better cognitive function, and fewer job injuries and accidents in a study that included more than 800 nurses.225 In another study in 65 female participants, habitual breakfast skippers had blunted diurnal cortisol variation, increased overall cortisol output, and higher blood pressure compared with habitual breakfast eaters, suggesting a morning meal may be important for maintaining normal circadian regulation of the HPA axis.226
Minimize Caffeine and Alcohol Intake
Caffeine may seem attractive to those affected by stress-related fatigue, but its effects may aggravate symptoms such as anxiety and poor sleep in susceptible people.227,228 Caffeine stimulates the sympathetic nervous system, and in this way may activate the stress response.229 Even with daily consumption, its intake can raise cortisol levels and has been found to increase the cortisol response to mental stress.230,231 Caffeine can also prolong the effects of physical stress on heart rate and blood pressure.232 In one study, habitual coffee drinking was associated with greater increases in heart rate and vascular inflammation in response to mental stress.233 On the other hand, drinking coffee appears to promote healthy metabolism and may protect against type 2 diabetes, liver cancer, and cognitive decline.234 While sensitive individuals may fare better eliminating caffeine during times of stress, moderate intake may be reasonable for others.227
Alcohol is often used as a relaxant during times of stress235,236; however, excessive intake raises cortisol levels and long-term use leads to dysregulated HPA axis signaling and disrupts the normal function of the stress response.237-239 Individuals experiencing stress-related insomnia frequently turn to alcohol as a form of self-medication, but because alcohol erodes sleep quality and quantity, it may actually exacerbate sleep difficulties.240 In addition, people with a history of early life stress and people who experience intense life stress are more vulnerable to developing problematic drinking habits.239,241 Therefore, it is especially important to avoid stress-related alcohol use.
10 Nutrients
A variety of natural, integrative interventions have been shown to help balance HPA axis function and counteract the detrimental effects of chronic stress.
Multivitamins and B-Complex Vitamins
Deficiencies of B vitamins are associated with neuropsychiatric disorders such as depression, Alzheimer disease, schizophrenia, and other types of psychosis and dementia, and adequate amounts of all B vitamins are needed for healthy nervous system function.242,243
The ability of multivitamins to reduce perceived stress and fatigue has been demonstrated in a number of trials.244-248 In one randomized controlled trial in 60 working adults, those receiving a high-dose B-complex vitamin daily for 12 weeks reported lower levels of stress, confusion, and depressed mood compared with those receiving placebo.249 A review of the research concluded that multivitamins, and B-complex supplements in particular, can be effective for lowering perceived stress, reducing mild psychiatric symptoms, and improving everyday mood in healthy individuals.250
B vitamins may also support normal HPA axis function. In a placebo-controlled trial with 138 subjects, 16 weeks of supplementation with a multivitamin containing B vitamins increased the cortisol awakening response. The cortisol awakening response, which occurs about 30 minutes after waking and generally results in the highest cortisol level of the day, is considered a marker of healthy HPA axis tone and has been associated with lower distress levels during the rest of the day.251 Another randomized controlled crossover trial examined the effect of one week of treatment with a multivitamin supplement in 240 Chinese military personnel who underwent intense physical stress. The multivitamin was associated with better recovery of normal HPA axis function and improvements in psychological symptoms.252
Vitamin C (Ascorbic Acid)
The adrenal glands have the highest concentration of vitamin C in the body.253 In addition to its well-known function as a free radical scavenger, vitamin C is a cofactor in the synthesis of catecholamines—neurohormones involved in the stress response—and may help modulate central nervous system activities.253-255 Levels of vitamin C in the blood and white blood cells drop quickly during times of stress or infection,256 and symptoms of depression and anxiety have been correlated with low intake and low circulating levels of vitamin C.254
In a controlled clinical trial, patients with stress-induced anxiety and depression had lower levels of vitamin C, as well as vitamins E and A, than healthy subjects, and the addition of these nutrients (1,000 mg per day vitamin C, 800 mg per day vitamin E, and 600 mg per day vitamin A) to antidepressant therapy led to greater reductions in symptoms of anxiety and depression compared with antidepressant therapy alone.257 Another controlled trial found that supplementing with 500 mg per day of vitamin C reduced anxiety levels and lowered average heart rate in healthy high school students.258 In addition, a review of research indicated high doses of vitamin C may reduce anxiety and mitigate stress-related increases in blood pressure.259
Omega-3 Fatty Acids
Omega-3 fatty acids (primarily EPA [eicosapentaenoic acid] and DHA [docosahexaenoic acid] from fish oil) may help prevent and treat stress, anxiety, and depression.260-262 Low blood levels of EPA and DHA have been correlated with several biological indicators of stress: elevated markers of inflammation, dysregulated nervous system signaling, and HPA axis hyper-reactivity.263,264 Conversely, omega-6 fatty acids, mainly obtained through eating animal fats and processed vegetable oils, promote inflammation and can thereby induce stress signaling and contribute to stress-related illnesses.261
In a randomized controlled trial in participants with high triglyceride levels, taking 3,400 mg of combined EPA and DHA for eight weeks increased heart rate variability, indicating lower stress-related nervous system signaling; however, a lower dose of 850 mg per day had no effect.265 Another controlled trial found that three weeks of treatment with 60 mg EPA and 252 mg DHA daily improved perceived stress and anxiety and reduced cortisol levels in alcoholic subjects in a residential treatment program.266 Evidence from trials in patients with depression suggest omega-3 fatty acids can correct HPA hyperactivity, mitigate symptoms, and may improve responsiveness to antidepressant therapy.264,267
A meta-analysis published in late 2024 evaluated 29 randomized controlled trials that included 35 independent samples comprising 3,918 subjects on omega-3 supplementation to reduce aggression. The study found that omega-3 supplementation led to modest short-term reductions in aggression, regardless of age, gender, and diagnosis. On average, the studies included in the meta-analysis used a dosage of about 1,200 mg of omega-3 fatty acids per day and a treatment duration of about 16 weeks. The study found that omega-3 supplementation was effective in reducing proactive and reactive types of aggression, especially when it was based on subjective reports. The authors concluded “…there is now sufficient evidence to begin to implement omega-3 supplementation to reduce aggression…irrespective of whether the setting is the community, the clinic, or the criminal justice system.”460
L-theanine
L-theanine is an amino acid found in tea that has demonstrated anti-stress effects. Numerous studies have found that tea and theanine reduce perceived stress and physiologic markers of the stress response, including blood pressure, heart rate, cortisol levels, and patterns of brain activity.268 In one trial that included 20 pharmacy students, taking 200 mg L-theanine twice daily for one week decreased morning salivary α-amylase levels more than placebo. Moreover, subjects taking L-theanine reported significantly less subjective stress than those taking placebo.269 A separate study found that L-theanine promoted a calming effect by increasing alpha wave (ie, a type of brain wave associated with wakeful relaxation and alertness) power. Sixteen individuals ranging in age from 19 to 60 years were randomized to receive a single dose of 200 mg L-theanine (as AlphaWave L-theanine) or placebo prior to a mental arithmetic test that elicited increased heart rate, blood pressure, stress, and anxiety. Those in the L-theanine group displayed significantly increased alpha brain wave power and reduced salivary cortisol levels compared with placebo.461
The short-term effects of L-theanine were confirmed in another randomized controlled trial in 36 healthy participants age 18 to 40 years. A single 200 mg dose of L-theanine decreased subjective stress one hour after administration and the cortisol response to a cognitive stressor three hours after administration. In addition, in a subset of participants whose scores on a test of tendency to experience anxiety were high, L-theanine increased brain wave activity associated with relaxation.270 A longer study randomized 30 healthy adults to receive 400 mg L-theanine (as AlphaWave L-theanine) or placebo daily for 28 days. The L-theanine group reported a significant decrease in perceived stress at 28 days compared with baseline. No difference was observed in salivary cortisol levels and L-theanine was well-tolerated with no adverse events reported by the end of the study or upon follow-up.462 In a study of 30 individuals ranging in age from 20 to 69 years, 200 mg L-theanine daily for 28 days significantly improved stress-related symptoms, sleep quality, and executive cognitive function compared with placebo.463 A series of small trials conducted by researchers in Japan found that L-theanine supplementation prevented heart rate elevation in response to stress-inducing arithmetic tests in the lab. Salivary immunoglobulin A (s-IgA) levels were also reduced in response to the stressful tasks in those who took L-theanine. The researchers concluded that reductions in heart rate and s-IgA in subjects taking L-theanine were likely attributable to attenuation of sympathetic nervous system activity.438
Theanine has also been shown to counter the stress-inducing effects of caffeine and enhance focused attention,271 and a two-month clinical trial noted that theanine, in combination with a vitamin/mineral/herbal supplement, lowered perceived stress scores and improved cognitive function in elderly subjects.272
Phosphatidylserine
The phospholipid phosphatidylserine is found in cell membranes and helps facilitate healthy cellular communication. It modulates the tissue response to inflammation and can reduce oxidative stress.273 Several studies have shown that phosphatidylserine can balance HPA axis signaling and may limit the negative consequences of over-activation of the adrenal glands.
In a trial in 75 healthy male volunteers, taking a supplement providing 400 mg each of phosphatidylserine and its precursor phosphatidic acid for 42 days diminished the HPA axis response to acute stress in a subset of men reporting high levels of chronic stress.274 In other clinical research, this same combination was noted to dampen the stress response to mental stress,275 and 300 mg per day of phosphatidylserine alone reduced perceived stress and improved mood in healthy young adults prone to negative emotions like anxiety, worry, and fear.276 Phosphatidylserine has also been found to lower cortisol levels overall and reduce the cortisol response to acute exercise in men, an effect that may help prevent harmful outcomes of overtraining, such as decreased performance, injury, immune suppression, and deterioration of psychological well-being.277
Curcumin
Curcumin is a pigment from turmeric root responsible for its characteristic yellow-orange color. As a polyphenol, curcumin has strong free radical-quenching and anti-inflammatory actions, and has been used historically to treat a range of inflammatory disorders, including musculoskeletal problems, neurological disorders, heart disease, and diabetes.439 Numerous clinical studies indicate curcumin’s potential to reduce the effects of chronic and repetitive stress on cognitive function and mood.440-444 Furthermore, preclinical evidence suggests curcumin’s anti-stress effects may be related to its ability to reduce neuro-inflammation and preserve neuroplasticity. 445-447
Multiple randomized controlled trials and three meta-analyses have shown curcumin can reduce depressive and anxiety symptoms in individuals with depression.448-450 A clinical trial in 60 participants with occupational stress-related anxiety compared a combination of highly absorbable curcumin plus fenugreek, at a dose of 1,000 mg per day, to the same dose of standard curcumin or placebo. After 30 days, participants taking the curcumin/fenugreek combination reported greater reductions in stress, anxiety, and fatigue, as well as greater improvement in quality of life, compared with those taking ordinary curcumin or placebo.451 In another placebo-controlled trial in 80 participants with diabetic neuropathy, taking 80 mg per day of a different highly-absorbable form of curcumin for eight weeks led to reductions in depression and anxiety symptom scores compared with placebo.452 In patients with major depressive disorder, those receiving up to 1,500 mg curcumin daily for 12 weeks had greater improvement in depression compared with those receiving placebo. Moreover, the benefit was still measurable four weeks after the end of the trial.453 Curcumin supplementation was also found to lower perceived stress levels better than placebo in athletes during endurance training.454
L-tryptophan
L-tryptophan is an amino acid precursor to the neurotransmitter serotonin. Serotonin has a complex relationship with the stress response.278 Stress-induced inflammation appears to cause excessive breakdown of tryptophan, which may decrease serotonin production and increase risk of depression279; in addition, tryptophan depletion has been shown to increase stress sensitivity.280 Studies in healthy adults suggest tryptophan supplementation, ranging from 800 to 2,800 mg per day, may reduce the cortisol response to stress, mitigate stress-related negative moods, and prevent stress eating in some individuals.281-283 In a randomized controlled trial, a tryptophan-rich hydrolyzed protein supplement increased positive mood and lowered cortisol release in response to acute stress.284
Bioactive Milk Peptides
Upon ingestion, milk proteins are broken down into peptides (shortened amino acid chains) by enzymes. Some of the resulting peptides can be absorbed intact and exert biological activities.285 For example, α-lactalbumin is a bioactive milk peptide that has a high tryptophan content and has been found to support healthy neurological function, improve mood, and promote sleep.286 An enzyme-treated form of the milk protein, casein, has also demonstrated anti-stress and relaxing properties in animal studies, and appears to work by increasing signaling via receptors for GABA—a neurotransmitter that generally inhibits nervous system activity.287-289
One randomized, controlled, crossover trial included 63 women with stress-related symptoms such as anxiety, sleep problems, and fatigue. Thirty days of treatment with 150 mg per day of α-S1 casein hydrolysate (a form of bioactive milk peptides) was more effective than placebo at relieving symptoms.290 In healthy volunteers, a 200 mg dose of α-S1 casein hydrolysate was found to mitigate increases in blood pressure, heart rate, and cortisol release induced by experimental stress.291
Probiotics and Prebiotics
The gut microbiome, nervous system, and HPA axis are closely connected. Probiotics and prebiotics (indigestible dietary carbohydrates that support the growth of beneficial bacterial colonies) can improve the balance of gut bacteria, and a growing body of evidence points to their potential to have a positive impact on the stress response.35,37,260 Research indicating probiotics may lower stress reactivity and anxiety, and improve mood, memory, and cognition have led some researchers to call probiotics with these effects psychobiotics.292
Fermented milk products made with Lactobacillus casei strain Shirota have been found in several trials to suppress cortisol elevations in response to stress and reduce stress-related health concerns such as depressed or anxious mood, digestive upset, and cold symptoms in healthy medical students.293-295 In a randomized controlled trial, 10 days of supplementation with 10 billion colony forming units (CFUs) of L. plantarum 299v per day decreased salivary cortisol levels in students facing an upcoming exam.296 In other controlled trials, taking a combination of L. helveticus R0052 and Bifidobacterium longum R0175, at a dose of 3 billion CFUs per day, for 30 days lowered scores on scales of perceived stress as well as urinary cortisol levels in healthy volunteers,297 and supplementing with 1 billion CFUs per day of B. longum 1714 for four weeks suppressed the cortisol rise and subjective anxiety associated with an acute stressor.298
Prebiotics are also demonstrating positive effects in clinical research: in a trial in 45 healthy adults, taking 5.5 grams of a prebiotic supplement containing galacto-oligosaccharides for three weeks resulted in lower early-morning cortisol levels and more balanced processing of positive and negative emotional stimuli.299
Melatonin
The hormone melatonin, which is released from the small gland at the base of the brain called the pineal gland, is known for its relationship with the sleep cycle. Melatonin plays a central role in circadian regulation of body systems, including the HPA axis.300 Stress can reduce melatonin levels and destabilize the body’s biological rhythms.301 Chronic disruption of the brain’s internal clock, such as through shift-work or insomnia, harms mental and physical health.302,303
Melatonin supplementation can improve sleep quantity and quality and help restore normal circadian processes,304,305 which may lead to reduced stress and prevention of stress-related deterioration of health.306 In one study, 2 mg of melatonin taken in the evening for six months improved sleep and increased DHEA-S levels in a group of elderly female volunteers.307
Dehydroepiandrosterone (DHEA)
Dehydroepiandrosterone (DHEA) is an adrenal hormone that, like cortisol, is secreted in response to acute stress, but chronic stress has been associated with low levels.8 The effect of stress on DHEA may be one of the factors linking stress to poor health and accelerated aging.121 Low DHEA-S levels have been correlated with conditions such as osteoporosis, cognitive decline and dementia, cardiovascular disease, mood disorders, and sexual dysfunction.123 Findings from preclinical and clinical research suggest DHEA replacement therapy may have a role in protecting aging bone and vasculature and may help in the treatment of depression and sexual disorders.122,123
In a randomized, placebo-controlled, crossover trial that enrolled 13 men and 17 women between ages 40 and 70 years, treatment with 50 mg DHEA daily for six months led to significant improvements in physical and psychological well-being. Subjects in this study reported a better ability to handle stress, improved mood, and being generally relaxed.308 In a different study, 24 healthy young men took high-dose DHEA (150 mg twice daily) for seven days. Subjects reported improved mood, and DHEA treatment led to reduced levels of cortisol on evening measures.309
Supplemental doses of DHEA typically range from 10–25 mg daily for women and 25–75 mg daily for men, but should be based on DHEA-S blood levels. More information is available in Life Extension’s DHEA Restoration Therapy protocol.
Lychee and Green Tea
A supplement that combines polyphenols from lychee ( Litchi chinensis) fruit and catechins from green tea, called Oligonol, has been found to have strong free-radical quenching and inflammation-suppressing capacity.433 It may also have stress-mediating effects. A pilot study in 19 healthy sedentary men compared 100 mg Oligonol per day for four weeks to placebo. Those receiving Oligonol experienced decreases in levels of cortisol and certain inflammatory markers during the study. In addition, the Oligonol-treated men had a lower cortisol response to exercise compared with placebo.434 In a study of the acute effects of Oligonol in 13 healthy men, a single 100 mg dose reduced the rise in cortisol, as well as inflammatory markers, triggered by a physical stressor.435
Magnesium Acetyl Taurate
Magnesium is an essential mineral that acts as a cofactor in hundreds of biochemical processes, including those involved in the stress response. Magnesium can inhibit glutamate receptors to attenuate excitatory transmission and promote GABA and serotonin activity.455
Preclinical and clinical studies have observed that magnesium levels are negatively affected by stressful stimuli, and that magnesium supplementation can reduce stress.456,457 Low levels of magnesium can further exacerbate stress, as magnesium indirectly reduces cortisol secretion.455
Magnesium acetyl taurate, an organic salt of magnesium, has demonstrated improved bioavailability in the brain compared with other forms of magnesium.458 In an unpublished clinical study including 19 women with stress-like symptoms related to premenstrual syndrome and inadequate magnesium intake from their diet, magnesium acetyl taurate (770 mg/day, providing approximately 45 mg elemental magnesium) was found to decrease stress-like symptoms including anxiety, nervous tension, irritability, headache, fatigue, and depression.459
Adaptogens
Adaptogenic herbs have multi-faceted beneficial effects that support the body’s intrinsic resilience to stressful conditions. They work by regulating biological networks in ways that support homeostasis. For example, adaptogens can raise energy levels, yet also support sound sleep. Some typical reasons adaptogens are used include to relieve fatigue, improve cognitive function and mood, and support the immune system.310-312
Magnolia and phellodendron. Magnolia (Magnolia officinalis) is an important plant in traditional Chinese herbal medicine. Its active constituents, magnolol and honokiol, have been found in preclinical and clinical trials to have a variety of beneficial effects, including stress reduction.313 In rodents exposed to chronic stress, both magnolol and honokiol, as well as their combination, have been found to normalize serotonin and HPA axis activity, increase levels of a brain growth factor (brain-derived neurotrophic factor, or BDNF), reduce neuroinflammation and brain oxidative stress, and prevent behaviors indicative of depression.314-317
A combination of magnolia and phellodendron ( Phellodendron amurense, a tree also known as Amur cork tree and often used in traditional Chinese medicine) has been studied for anti-stress effects as well. In one controlled clinical trial, 56 healthy subjects with moderate stress levels received either a supplement providing 250 mg of magnolia plus phellodendron or placebo twice daily for four weeks. Participants underwent three (morning, noon, and night) salivary cortisol tests and answered mood questionnaires at the beginning and end of the trial. Those receiving the supplement had lower total cortisol exposure and better mood scores than those receiving placebo.318
The same combination supplement was studied for its effect on stress-induced appetite and weight gain. In one controlled trial, magnolia plus phellodendron, at a dose of 250 mg three times daily for six weeks, reduced weight gain compared with placebo in overweight but otherwise healthy premenopausal women who reported stress eating and above-average levels of anxiety.319 In another similarly designed trial, magnolia plus phellodendron reduced temporary anxiety, but did not affect longstanding depression or anxiety, appetite, sleep, or levels of salivary cortisol and amylase.320
Holy basil. Holy basil (Ocimum sanctum, also known as tulsi basil) is an adaptogenic herb from the Ayurvedic tradition. In Hindu spirituality, holy basil is considered a sacred plant and an incarnation of the goddess Tulsi.321 A number of clinical and preclinical studies have demonstrated holy basil’s anti-stress potential by providing evidence that it improves mood and cognition, normalizes metabolism, regulates immune function, reduces oxidative stress, and prevents toxic damage in various tissues by supporting detoxification.321,322
In a randomized controlled trial with 40 participants, 300 mg of holy basil extract per day for 30 days resulted in reduced anxiety symptoms and improved cognitive test scores compared with placebo.323 Findings from another randomized controlled trial, in which 150 participants received 1,200 mg holy basil per day or placebo, indicated that holy basil lowered stress-related symptoms such as anxiety, fatigue, sleep difficulties, and sexual dysfunction.324 A pilot trial in which 35 patients with anxiety were treated with 500 mg holy basil twice daily found that treatment led to reductions in symptoms of anxiety, stress, and depression.325
Ashwagandha. Ashwagandha (Withania somnifera) is another important herb in the Ayurvedic herbal pharmacy, in which it is used as a general tonic and aphrodisiac.326 Numerous preclinical studies show ashwagandha prevents oxidative damage, supports normal mitochondrial activity, modulates central nervous system signaling, and contributes to immune regulation, suggesting it may be useful in the treatment of chronic stress-related, inflammatory, metabolic, cardiovascular, and neurodegenerative disorders.327-329
Several clinical trials further indicate that ashwagandha is effective for relieving stress and anxiety.330 For example, in a trial with 64 participants, 300 mg ashwagandha extract twice daily was more effective for reducing perceived stress scores and lowering blood cortisol levels than placebo after 60 days of treatment.331 Another trial noted the possible beneficial effects of ashwagandha on weight management in people with chronic stress. Fifty-two chronically stressed participants received either 300 mg ashwagandha twice daily or placebo for eight weeks; those receiving ashwagandha had greater reductions in perceived stress and serum cortisol levels, more improvements in food cravings and eating behaviors, and greater weight loss than those receiving placebo.332
Bacopa. Bacopa (Bacopa monnieri) has been used historically in Ayurvedic medicine to support healthy cognitive function.333 A number of animal studies have demonstrated its adaptogenic potential, noting its ability to normalize stress hormone levels and neurotransmitter balance,334 reduce oxidative stress,335 protect against neurodegeneration,336 and prevent or reverse other negative physiologic and behavioral consequences of stress.337-339 Furthermore, in rodent models of chronic stress, bacopa and an active constituent (bacopaside I) have been found to reduce depressive behavior, normalize HPA axis function, reduce brain oxidative stress, and prevent a drop in BDNF and other changes in the brain environment.340-342 Bacopa has also been found to increase stress resilience and lifespan in another laboratory animal model.343
In a preliminary trial in 17 healthy adults, a standardized extract of bacopa, taken in single doses of 320 mg and 640 mg, improved cognitive performance one to two hours later on multitasking mental tests while also reducing cortisol levels, suggesting that part of its cognitive benefits may be related to stress-reducing effects.344 In a randomized controlled trial in 54 elderly subjects, 300 mg per day of bacopa for 12 weeks led to improved cognitive performance, lower depression and anxiety scores, and reduced heart rate compared with placebo.345
Lemon balm. Lemon balm (Melissa officinalis) is a plant in the mint family used in herbal medicine as a relaxing and uplifting nervous system tonic.346,347 Consumed in food or drink, lemon balm was found to generally improve mood and cognitive performance in healthy young adults.348 In healthy subjects exposed to experimental stress, individual doses of lemon balm had acute anti-stress and cognitive-enhancing effects, and increased self-reported calmness and alertness.349
In a pilot trial in 20 stressed volunteers with mild-to-moderate anxiety and insomnia, 15 days of treatment with 300 mg lemon balm extract twice daily led to symptom improvement in 19 (95%) of the participants. In addition, 14 participants had a complete remission of anxiety, 17 had remission of insomnia, and 14 had remission of both anxiety and insomnia.350 In a placebo-controlled clinical trial in 80 patients with stable angina, 3 grams per day of lemon balm for eight weeks reduced anxiety, depression, and stress, and improved sleep.351 In animal research, lemon balm decreased stress-induced symptoms of irritable bowel syndrome.352
Saffron. Saffron (Crocus sativus) is a yellow spice prized for its color and flavor. It also has a long history of use in herbal medicine for its sedative, adaptogenic, and other properties. Several clinical trials have shown that saffron is helpful in treating mild-to-moderate depression.353,354 Saffron and its active constituent crocin have also demonstrated anti-stress and anti-anxiety effects in animal studies, and preclinical evidence suggests it may exert its benefits in part by moderating HPA axis responsiveness.355-358 In addition, crocetin, another active compound from saffron, was found to prevent stress-induced depressive behavior in rats.359
In a randomized controlled trial, subjects without depression but reporting low mood who received treatment with 28 mg per day of saffron extract for four weeks had greater improvement in mood and reductions in symptoms of stress and anxiety than those receiving placebo.360
Ginseng. Ginseng is a common name for a group of similar plants, including Asian ginseng (Panax ginseng), American ginseng (Panax quinquefolius), and Chinese ginseng ( Panax notoginseng). These plants all contain active compounds called ginsenosides. Panax ginseng and its unique ginsenosides have been widely studied for their effects on disease prevention and overall well-being.361 This herb has been used for thousands of years to enhance vitality and longevity, and numerous studies show it has a broad range of actions such as immune-modulating, anti-inflammatory, anti-cancer, free radical scavenging, neuroprotective, and cardioprotective.362-365 With regard to stress physiology, a fermented ginseng extract was found to reduce oxidative stress and HPA axis signaling in response to exercise stress.366
Although unrelated to the Panax species of ginseng, Siberian ginseng (Eleutherococcus or Acanthopanax senticosus) is another popular adaptogenic herb. It contains active compounds called eleutherosides and has demonstrated a range of anti-stress properties.367
Rhodiola. Rhodiola (Rhodiola rosea, also known as roseroot or golden root) is an adaptogenic herb that grows in Arctic regions and is used around the world to enhance physical and mental stamina and relieve stress.368 Rhodiola appears to modulate HPA axis function, reduce oxidative stress, and regulate immune activity.369,370
Pilot trials in patients with chronic fatigue symptoms, burnout, and mild anxiety have found that 400 mg rhodiola extract daily is associated with improvements in measures of energy level, mood, sleep, cognitive function, and general well-being.371-373 Rhodiola has also been found to help patients with stress-induced depression.374 This effect may be due in part to its promotion of new connections in the brain.375
Amla. Amla (Phyllanthus emblica), an adaptogen also known as Indian gooseberry, is used in Ayurvedic medicine to restore strength and good health.376 Some of its active constituents have demonstrated strong oxidative stress-reducing capacity.377 In a preliminary trial in 12 healthy volunteers, 500 mg of a standardized amla extract twice daily for 14 days mitigated acute stress-induced increase in arterial stiffness and decrease in cardiac blood flow.378 Research in animals suggests amla may reduce brain oxidative stress, prevent chronic stress-related damage to testicular tissue, improve stress resilience in general, and lengthen lifespan.379-381
Schisandra. Schisandra (Schisandra chinensis) has been used for centuries in the treatment of depression, anxiety, and insomnia, as well as a wide range of health problems related to fatigue and weakness.382,383 Schisandra and its active constituents have also demonstrated liver-protecting, anti-inflammatory, immunomodulating, anti-proliferative, and cognitive enhancing effects. Schisandra also holds promise as a cardiac and neurological protectant.382-384 Findings from animal research suggest Schisandra may help regulate HPA axis activity and relieve the negative effects of stress.385-387
Cordyceps. Cordyceps (Ophiocordyceps [formerly Cordyceps] sinensis) is a fungal/insect complex used in traditional Chinese medicine to treat fatigue and as a promoter of health, longevity, and physical performance.388,389 Many active compounds from cordyceps have been identified and studies have shown them to possess anti-inflammatory, immune-modulating, and oxidative stress reducing actions.390 Furthermore, preclinical research suggests it has potential as an anti-aging, anti-fatigue, neuroprotective, and aphrodisiac agent.389 In an animal model of chronic stress, cordyceps supplementation alleviated depression-like behavior induced by unpredictable and repeated mild stress. Furthermore, cordyceps treatment reduced some markers of inflammation and upregulated expression of BDNF.391 Preliminary clinical evidence suggests cordyceps may improve athletic performance and suppress the exercise-induced rise in cortisol release, which may help prevent the harmful effects of overtraining.392
Disclaimer and Safety Information
This information (and any accompanying material) is not intended to replace the attention or advice of a physician or other qualified health care professional. Anyone who wishes to embark on any dietary, drug, exercise, or other lifestyle change intended to prevent or treat a specific disease or condition should first consult with and seek clearance from a physician or other qualified health care professional. Pregnant women in particular should seek the advice of a physician before using any protocol listed on this website. The protocols described on this website are for adults only, unless otherwise specified. Product labels may contain important safety information and the most recent product information provided by the product manufacturers should be carefully reviewed prior to use to verify the dose, administration, and contraindications. National, state, and local laws may vary regarding the use and application of many of the therapies discussed. The reader assumes the risk of any injuries. The authors and publishers, their affiliates and assigns are not liable for any injury and/or damage to persons arising from this protocol and expressly disclaim responsibility for any adverse effects resulting from the use of the information contained herein.
The protocols raise many issues that are subject to change as new data emerge. None of our suggested protocol regimens can guarantee health benefits. Life Extension has not performed independent verification of the data contained in the referenced materials, and expressly disclaims responsibility for any error in the literature.
- Dhabhar FS. Effects of stress on immune function: the good, the bad, and the beautiful. Immunol Res. May 2014;58(2-3):193-210.
- Duric V, Clayton S, Leong ML, Yuan LL. Comorbidity Factors and Brain Mechanisms Linking Chronic Stress and Systemic Illness. Neural Plast. 2016;2016:5460732.
- Herman JP, McKlveen JM, Ghosal S, et al. Regulation of the Hypothalamic-Pituitary-Adrenocortical Stress Response. Compr Physiol. Mar 15 2016;6(2):603-621.
- Househam AM, Peterson CT, Mills PJ, Chopra D. The Effects of Stress and Meditation on the Immune System, Human Microbiota, and Epigenetics. Adv Mind Body Med. Fall 2017;31(4):10-25.
- McEwen BS. In pursuit of resilience: stress, epigenetics, and brain plasticity. Ann N Y Acad Sci. Jun 2016;1373(1):56-64.
- Worthen M, Cash E. Stress Management. StatPearls. Treasure Island (FL): StatPearls Publishing LLC.; 2018.
- Dantzer B, Fletcher QE, Boonstra R, Sheriff MJ. Measures of physiological stress: a transparent or opaque window into the status, management and conservation of species? Conservation Physiology. 2014;2(1):cou023-cou023.
- Kamin HS, Kertes DA. Cortisol and DHEA in development and psychopathology. Horm Behav. Mar 2017;89:69-85.
- Tsigos C, Kyrou I, Kassi E, Chrousos GP. Tsigos C, Kyrou I, Kassi E, et al. Stress, Endocrine Physiology and Pathophysiology. [Updated 2016 Mar 10]. In: De Groot LJ, Chrousos G, Dungan K, et al., editors. Endotext [Internet]. South Dartmouth (MA): MDText.com, Inc.; 2000-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK278995/. Accessed 10/26/2018. Endotext. South Dartmouth (MA): MDText.com, Inc.; 2016.
- Harrell CS, Gillespie CF, Neigh GN. Energetic stress: The reciprocal relationship between energy availability and the stress response. Physiol Behav. Nov 1 2016;166:43-55.
- Rao R. Hypothalamic-Pituitary-Adrenal Axis Programming after Recurrent Hypoglycemia during Development. J Clin Med. Sep 2015;4(9):1729-1740.
- Wood SK, Valentino RJ. The brain norepinephrine system, stress and cardiovascular vulnerability. Neurosci Biobehav Rev. Mar 2017;74(Pt B):393-400.
- Kritikou I, Basta M, Vgontzas AN, et al. Sleep apnoea and the hypothalamic-pituitary-adrenal axis in men and women: effects of continuous positive airway pressure. Eur Respir J. Feb 2016;47(2):531-540.
- Shin W, Jen R, Li Y, Malhotra A. Tailored treatment strategies for obstructive sleep apnea. Respir Investig. Jan 2016;54(1):2-7.
- Spiers JG, Chen HJ, Sernia C, Lavidis NA. Activation of the hypothalamic-pituitary-adrenal stress axis induces cellular oxidative stress. Front Neurosci. 2014;8:456.
- Gadek-Michalska A, Tadeusz J, Rachwalska P, Bugajski J. Cytokines, prostaglandins and nitric oxide in the regulation of stress-response systems. Pharmacol Rep. 2013;65(6):1655-1662.
- Spencer RL, Deak T. A users guide to HPA axis research. Physiol Behav. Sep 1 2017;178:43-65.
- McEwen BS, Nasca C, Gray JD. Stress Effects on Neuronal Structure: Hippocampus, Amygdala, and Prefrontal Cortex. Neuropsychopharmacology. Jan 2016;41(1):3-23.
- Charoensri S, Chailurkit L, Muntham D, Bunnag P. Serum dehydroepiandrosterone sulfate in assessing the integrity of the hypothalamic-pituitary-adrenal axis. J Clin Transl Endocrinol. Mar 2017;7:42-46.
- JCCL. Jo Cox Commission of Loneliness: A Call to Action. Available at https://www.jocoxloneliness.org/pdf/a_call_to_action.pdf. Published 2017. Accessed 11/04/2018. 2017.
- Pimlott N. The ministry of loneliness. Can Fam Physician. Mar 2018;64(3):166.
- Leigh-Hunt N, Bagguley D, Bash K, et al. An overview of systematic reviews on the public health consequences of social isolation and loneliness. Public Health. Nov 2017;152:157-171.
- Courtin E, Knapp M. Social isolation, loneliness and health in old age: a scoping review. Health Soc Care Community. May 2017;25(3):799-812.
- Brown EG, Gallagher S, Creaven AM. Loneliness and acute stress reactivity: A systematic review of psychophysiological studies. Psychophysiology. May 2018;55(5):e13031.
- Dumbell R, Matveeva O, Oster H. Circadian Clocks, Stress, and Immunity. Front Endocrinol (Lausanne). 2016;7:37.
- Liyanarachchi K, Ross R, Debono M. Human studies on hypothalamo-pituitary-adrenal (HPA) axis. Best Pract Res Clin Endocrinol Metab. Oct 2017;31(5):459-473.
- Strohmaier S, Devore EE, Zhang Y, Schernhammer ES. A Review of Data of Findings on Night Shift Work and the Development of DM and CVD Events: a Synthesis of the Proposed Molecular Mechanisms. Curr Diab Rep. Oct 20 2018;18(12):132.
- De Nobrega AK, Lyons LC. Aging and the clock: Perspective from flies to humans. Eur J Neurosci. Sep 30 2018.
- Helfrich-Forster C. Interactions between psychosocial stress and the circadian endogenous clock. Psych J. Dec 2017;6(4):277-289.
- Ouakinin SRS, Barreira DP, Gois CJ. Depression and Obesity: Integrating the Role of Stress, Neuroendocrine Dysfunction and Inflammatory Pathways. Front Endocrinol (Lausanne). 2018;9:431.
- Bekhbat M, Rowson SA, Neigh GN. Checks and balances: The glucocorticoid receptor and NFkB in good times and bad. Front Neuroendocrinol. Jul 2017;46:15-31.
- Silverman MN, Sternberg EM. Glucocorticoid regulation of inflammation and its functional correlates: from HPA axis to glucocorticoid receptor dysfunction. Ann N Y Acad Sci. Jul 2012;1261:55-63.
- Nezi M, Mastorakos G, Mouslech Z. Corticotropin Releasing Hormone And The Immune/Inflammatory Response. [Updated 2015 Jul 30]. In: De Groot LJ, Chrousos G, Dungan K, et al., editors. Endotext [Internet]. South Dartmouth (MA): MDText.com, Inc.; 2000-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK279017/. In: De Groot LJ, Chrousos G, Dungan K, et al., eds. Endotext. South Dartmouth (MA): MDText.com, Inc.; 2015.
- Meyer T, Wirtz PH. Mechanisms of Mitochondrial Redox Signaling in Psychosocial Stress-Responsive Systems: New Insights into an Old Story. Antioxid Redox Signal. Mar 20 2018;28(9):760-772.
- Rea K, Dinan TG, Cryan JF. The microbiome: A key regulator of stress and neuroinflammation. Neurobiol Stress. Oct 2016;4:23-33.
- Lerner A, Neidhofer S, Matthias T. The Gut Microbiome Feelings of the Brain: A Perspective for Non-Microbiologists. Microorganisms. Oct 12 2017;5(4).
- Farzi A, Frohlich EE, Holzer P. Gut Microbiota and the Neuroendocrine System. Neurotherapeutics. Jan 2018;15(1):5-22.
- Sudo N. Microbiome, HPA axis and production of endocrine hormones in the gut. Adv Exp Med Biol. 2014;817:177-194.
- van Bodegom M, Homberg JR, Henckens M. Modulation of the Hypothalamic-Pituitary-Adrenal Axis by Early Life Stress Exposure. Front Cell Neurosci. 2017;11:87.
- Reul JM, Collins A, Saliba RS, et al. Glucocorticoids, epigenetic control and stress resilience. Neurobiol Stress. Jan 2015;1:44-59.
- Constantinof A, Moisiadis VG, Matthews SG. Programming of stress pathways: A transgenerational perspective. J Steroid Biochem Mol Biol. Jun 2016;160:175-180.
- Dirven BCJ, Homberg JR, Kozicz T, Henckens M. Epigenetic programming of the neuroendocrine stress response by adult life stress. J Mol Endocrinol. Jul 2017;59(1):R11-r31.
- Jawaid A, Roszkowski M, Mansuy IM. Transgenerational Epigenetics of Traumatic Stress. Prog Mol Biol Transl Sci. 2018;158:273-298.
- Youssef NA, Lockwood L, Su S, Hao G, Rutten BPF. The Effects of Trauma, with or without PTSD, on the Transgenerational DNA Methylation Alterations in Human Offsprings. Brain Sci. May 8 2018;8(5).
- Epel ES, Lithgow GJ. Stress biology and aging mechanisms: toward understanding the deep connection between adaptation to stress and longevity. J Gerontol A Biol Sci Med Sci. Jun 2014;69 Suppl 1:S10-16.
- Peake JM, Markworth JF, Nosaka K, Raastad T, Wadley GD, Coffey VG. Modulating exercise-induced hormesis: Does less equal more? J Appl Physiol (1985). Aug 1 2015;119(3):172-189.
- Testa G, Biasi F, Poli G, Chiarpotto E. Calorie restriction and dietary restriction mimetics: a strategy for improving healthy aging and longevity. Curr Pharm Des. 2014;20(18):2950-2977.
- Ristow M, Schmeisser S. Extending life span by increasing oxidative stress. Free Radic Biol Med. Jul 15 2011;51(2):327-336.
- Lampert R, Tuit K, Hong KI, Donovan T, Lee F, Sinha R. Cumulative stress and autonomic dysregulation in a community sample. Stress. May 2016;19(3):269-279.
- Fioranelli M, Bottaccioli AG, Bottaccioli F, Bianchi M, Rovesti M, Roccia MG. Stress and Inflammation in Coronary Artery Disease: A Review Psychoneuroendocrineimmunology-Based. Front Immunol. 2018;9:2031.
- Kivimaki M, Kawachi I. Work Stress as a Risk Factor for Cardiovascular Disease. Curr Cardiol Rep. Sep 2015;17(9):630.
- Virtanen M, Kivimaki M. Long Working Hours and Risk of Cardiovascular Disease. Curr Cardiol Rep. Oct 1 2018;20(11):123.
- Nahrendorf M, Swirski FK. Lifestyle effects on hematopoiesis and atherosclerosis. Circ Res. Feb 27 2015;116(5):884-894.
- Gopalakrishnan P, Zaidi R, Sardar MR. Takotsubo cardiomyopathy: Pathophysiology and role of cardiac biomarkers in differential diagnosis. World J Cardiol. Sep 26 2017;9(9):723-730.
- Said SM, Saygili E, Rana OR, et al. Takotsubo Cardiomyopathy: What we have Learned in the Last 25 Years? (A Comparative Literature Review). Curr Cardiol Rev. 2016;12(4):297-303.
- Phillips C. Lifestyle Modulators of Neuroplasticity: How Physical Activity, Mental Engagement, and Diet Promote Cognitive Health during Aging. Neural Plast. 2017;2017:3589271.
- Calcia MA, Bonsall DR, Bloomfield PS, Selvaraj S, Barichello T, Howes OD. Stress and neuroinflammation: a systematic review of the effects of stress on microglia and the implications for mental illness. Psychopharmacology (Berl). May 2016;233(9):1637-1650.
- Piirainen S, Youssef A, Song C, et al. Psychosocial stress on neuroinflammation and cognitive dysfunctions in Alzheimer's disease: the emerging role for microglia? Neurosci Biobehav Rev. Jun 2017;77:148-164.
- Bisht K, Sharma K, Tremblay ME. Chronic stress as a risk factor for Alzheimer's disease: Roles of microglia-mediated synaptic remodeling, inflammation, and oxidative stress. Neurobiol Stress. Nov 2018;9:9-21.
- Kumar A, Pareek V, Faiq MA, et al. Regulatory role of NGFs in neurocognitive functions. Rev Neurosci. Jul 26 2017;28(6):649-673.
- Daskalakis NP, De Kloet ER, Yehuda R, Malaspina D, Kranz TM. Early Life Stress Effects on Glucocorticoid-BDNF Interplay in the Hippocampus. Front Mol Neurosci. 2015;8:68.
- Nowacka M, Obuchowicz E. BDNF and VEGF in the pathogenesis of stress-induced affective diseases: an insight from experimental studies. Pharmacol Rep. 2013;65(3):535-546.
- Makhathini KB, Abboussi O, Stein DJ, Mabandla MV, Daniels WMU. Repetitive stress leads to impaired cognitive function that is associated with DNA hypomethylation, reduced BDNF and a dysregulated HPA axis. Int J Dev Neurosci. Aug 2017;60:63-69.
- Eng JW, Kokolus KM, Reed CB, Hylander BL, Ma WW, Repasky EA. A nervous tumor microenvironment: the impact of adrenergic stress on cancer cells, immunosuppression, and immunotherapeutic response. Cancer Immunol Immunother. Nov 2014;63(11):1115-1128.
- Shin KJ, Lee YJ, Yang YR, et al. Molecular Mechanisms Underlying Psychological Stress and Cancer. Curr Pharm Des. 2016;22(16):2389-2402.
- Stults-Kolehmainen MA, Sinha R. The effects of stress on physical activity and exercise. Sports Med. Jan 2014;44(1):81-121.
- Mayo Clinic. Healthy Lifestyle: Stress Management. Available at https://www.mayoclinic.org/healthy-lifestyle/stress-management/in-depth/stress-symptoms/art-20050987. Last updated 04/28/2016. Accessed 11/05/2018. 2016.
- Law E, Girgis A, Sylvie L, Levesque J, Pickett H. Telomeres and Stress: Promising Avenues for Research in Psycho-Oncology. Asia Pac J Oncol Nurs. Apr-Jun 2016;3(2):137-147.
- Pirl WF, Fann JR, Greer JA, et al. Recommendations for the implementation of distress screening programs in cancer centers: report from the American Psychosocial Oncology Society (APOS), Association of Oncology Social Work (AOSW), and Oncology Nursing Society (ONS) joint task force. Cancer. Oct 1 2014;120(19):2946-2954.
- Grassi L, Spiegel D, Riba M. Advancing psychosocial care in cancer patients. F1000Res. 2017;6:2083.
- Lacourt TE, Heijnen CJ. Mechanisms of Neurotoxic Symptoms as a Result of Breast Cancer and Its Treatment: Considerations on the Contribution of Stress, Inflammation, and Cellular Bioenergetics. Curr Breast Cancer Rep. 2017;9(2):70-81.
- Ferrucci L, Fabbri E. Inflammageing: chronic inflammation in ageing, cardiovascular disease, and frailty. Nat Rev Cardiol. Sep 2018;15(9):505-522.
- Ayroldi E, Cannarile L, Adorisio S, Delfino DV, Riccardi C. Role of Endogenous Glucocorticoids in Cancer in the Elderly. Int J Mol Sci. Nov 27 2018;19(12).
- Del Pinto R, Ferri C. Inflammation-Accelerated Senescence and the Cardiovascular System: Mechanisms and Perspectives. Int J Mol Sci. Nov 22 2018;19(12).
- Masri S, Sassone-Corsi P. The emerging link between cancer, metabolism, and circadian rhythms. Nat Med. Dec 2018;24(12):1795-1803.
- Ans AH, Anjum I, Satija V, et al. Neurohormonal Regulation of Appetite and its Relationship with Stress: A Mini Literature Review. Cureus. Jul 23 2018;10(7):e3032.
- Joseph JJ, Golden SH. Cortisol dysregulation: the bidirectional link between stress, depression, and type 2 diabetes mellitus. Ann N Y Acad Sci. Mar 2017;1391(1):20-34.
- Kargi AY, Iacobellis G. Adipose tissue and adrenal glands: novel pathophysiological mechanisms and clinical applications. Int J Endocrinol. 2014;2014:614074.
- Champaneri S, Xu X, Carnethon MR, et al. Diurnal salivary cortisol is associated with body mass index and waist circumference: the Multiethnic Study of Atherosclerosis. Obesity (Silver Spring). Jan 2013;21(1):E56-63.
- Lemche E, Chaban OS, Lemche AV. Neuroendorine and Epigentic Mechanisms Subserving Autonomic Imbalance and HPA Dysfunction in the Metabolic Syndrome. Front Neurosci. 2016;10:142.
- Martocchia A, Stefanelli M, Falaschi GM, Toussan L, Ferri C, Falaschi P. Recent advances in the role of cortisol and metabolic syndrome in age-related degenerative diseases. Aging Clin Exp Res. Feb 2016;28(1):17-23.
- Diz-Chaves Y, Gil-Lozano M, Toba L, et al. Stressing diabetes? The hidden links between insulinotropic peptides and the HPA axis. J Endocrinol. Aug 2016;230(2):R77-94.
- Abdulateef DS, Mahwi TO. Assessment of hair cortisol in euthyroid, hypothyroid, and subclinical hypothyroid subjects. Endocrine. Sep 6 2018.
- Damian L, Ghiciuc CM, Dima-Cozma LC, et al. No definitive evidence for a connection between autoimmune thyroid diseases and stress in women. Neuro Endocrinol Lett. Jul 2016;37(3):155-162.
- Johnson EO, Kamilaris TC, Calogero AE, Konstandi M, Chrousos GP. Effects of short- and long-duration hypothyroidism on function of the rat hypothalamic-pituitary-adrenal axis. J Endocrinol Invest. Feb 2013;36(2):104-110.
- Johnson EO, Calogero AE, Konstandi M, Kamilaris TC, La Vignera S, Chrousos GP. Effects of short- and long-duration hypothyroidism on hypothalamic-pituitary-adrenal axis function in rats: in vitro and in situ studies. Endocrine. Dec 2012;42(3):684-693.
- Rosenberg SL, Miller GE, Brehm JM, Celedon JC. Stress and asthma: novel insights on genetic, epigenetic, and immunologic mechanisms. J Allergy Clin Immunol. Nov 2014;134(5):1009-1015.
- Lin TK, Zhong L, Santiago JL. Association between Stress and the HPA Axis in the Atopic Dermatitis. Int J Mol Sci. Oct 12 2017;18(10).
- Sharif K, Watad A, Coplan L, et al. The role of stress in the mosaic of autoimmunity: An overlooked association. Autoimmun Rev. Oct 2018;17(10):967-983.
- Romano GF, Tomassi S, Russell A, Mondelli V, Pariante CM. Fibromyalgia and chronic fatigue: the underlying biology and related theoretical issues. Adv Psychosom Med. 2015;34:61-77.
- Stover CM. Mechanisms of Stress-Mediated Modulation of Upper and Lower Respiratory Tract Infections. Adv Exp Med Biol. 2016;874:215-223.
- Sharma R, Biedenharn KR, Fedor JM, Agarwal A. Lifestyle factors and reproductive health: taking control of your fertility. Reprod Biol Endocrinol. Jul 16 2013;11:66.
- Pellissier S, Bonaz B. The Place of Stress and Emotions in the Irritable Bowel Syndrome. Vitam Horm. 2017;103:327-354.
- Maleki N, Becerra L, Borsook D. Migraine: maladaptive brain responses to stress. Headache. Oct 2012;52 Suppl 2(Suppl 2):102-106.
- Burke NN, Finn DP, McGuire BE, Roche M. Psychological stress in early life as a predisposing factor for the development of chronic pain: Clinical and preclinical evidence and neurobiological mechanisms. J Neurosci Res. Jun 2017;95(6):1257-1270.
- Buscemi V, Chang WJ, Liston MB, McAuley JH, Schabrun S. The role of psychosocial stress in the development of chronic musculoskeletal pain disorders: protocol for a systematic review and meta-analysis. Syst Rev. Nov 3 2017;6(1):224.
- Brotto L, Atallah S, Johnson-Agbakwu C, et al. Psychological and Interpersonal Dimensions of Sexual Function and Dysfunction. J Sex Med. Apr 2016;13(4):538-571.
- Turpeinen U, Hamalainen E. Determination of cortisol in serum, saliva and urine. Best Pract Res Clin Endocrinol Metab. Dec 2013;27(6):795-801.
- Wosu AC, Valdimarsdottir U, Shields AE, Williams DR, Williams MA. Correlates of cortisol in human hair: implications for epidemiologic studies on health effects of chronic stress. Ann Epidemiol. Dec 2013;23(12):797-811.e792.
- Kim LU, D'Orsogna MR, Chou T. Onset, timing, and exposure therapy of stress disorders: mechanistic insight from a mathematical model of oscillating neuroendocrine dynamics. Biol Direct. 2016;11(1):13.
- Inder WJ, Dimeski G, Russell A. Measurement of salivary cortisol in 2012 - laboratory techniques and clinical indications. Clin Endocrinol (Oxf). Nov 2012;77(5):645-651.
- Golden SH, Wand GS, Malhotra S, Kamel I, Horton K. Reliability of hypothalamic-pituitary-adrenal axis assessment methods for use in population-based studies. Eur J Epidemiol. Jul 2011;26(7):511-525.
- Adam EK, Quinn ME, Tavernier R, McQuillan MT, Dahlke KA, Gilbert KE. Diurnal cortisol slopes and mental and physical health outcomes: A systematic review and meta-analysis. Psychoneuroendocrinology. Sep 2017;83:25-41.
- Miller R, Stalder T, Jarczok M, et al. The CIRCORT database: Reference ranges and seasonal changes in diurnal salivary cortisol derived from a meta-dataset comprised of 15 field studies. Psychoneuroendocrinology. Nov 2016;73:16-23.
- Wright KD, Hickman R, Laudenslager ML. Hair Cortisol Analysis: A Promising Biomarker of HPA Activation in Older Adults. Gerontologist. Jun 2015;55 Suppl 1(Suppl 1):S140-145.
- Wester VL, van Rossum EF. Clinical applications of cortisol measurements in hair. Eur J Endocrinol. Oct 2015;173(4):M1-10.
- Silverman MN, Heim CM, Nater UM, Marques AH, Sternberg EM. Neuroendocrine and immune contributors to fatigue. Pm r. May 2010;2(5):338-346.
- Keremi B, Beck A, Fabian TK, et al. Stress and Salivary Glands. Curr Pharm Des. Oct 30 2017;23(27):4057-4065.
- Nater UM, Rohleder N. Salivary alpha-amylase as a non-invasive biomarker for the sympathetic nervous system: current state of research. Psychoneuroendocrinology. May 2009;34(4):486-496.
- Schumacher S, Kirschbaum C, Fydrich T, Strohle A. Is salivary alpha-amylase an indicator of autonomic nervous system dysregulations in mental disorders?--a review of preliminary findings and the interactions with cortisol. Psychoneuroendocrinology. Jun 2013;38(6):729-743.
- Cozma S, Dima-Cozma LC, Ghiciuc CM, Pasquali V, Saponaro A, Patacchioli FR. Salivary cortisol and alpha-amylase: subclinical indicators of stress as cardiometabolic risk. Braz J Med Biol Res. Feb 6 2017;50(2):e5577.
- Laufer S, Engel S, Knaevelsrud C, Schumacher S. Cortisol and alpha-amylase assessment in psychotherapeutic intervention studies: A systematic review. Neurosci Biobehav Rev. Dec 2018;95:235-262.
- Paszynska E, Dmitrzak-Weglarz M, Tyszkiewicz-Nwafor M, Slopien A. Salivary alpha-amylase, secretory IgA and free cortisol as neurobiological components of the stress response in the acute phase of anorexia nervosa. World J Biol Psychiatry. Jun 2016;17(4):266-273.
- Alaki SM, Safi A, Ouda S, Nadhreen A. Comparing Dental Stress in New Child Patients and Returning Patients Using Salivary Cortisol, Immunoglobulin-A and Alpha- Amylase. J Clin Pediatr Dent. 2017;41(6):462-466.
- Watanabe K, Shirakawa T. Characteristics of Perceived Stress and Salivary Levels of Secretory Immunoglobulin A and Cortisol in Japanese Women With Premenstrual Syndrome. Nurs Midwifery Stud. Jun 2015;4(2):e24795.
- Engeland CG, Hugo FN, Hilgert JB, et al. Psychological distress and salivary secretory immunity. Brain Behav Immun. Feb 2016;52:11-17.
- Romero-Martinez A, Moya-Albiol L. Stress-Induced Endocrine and Immune Dysfunctions in Caregivers of People with Eating Disorders. Int J Environ Res Public Health. Dec 13 2017;14(12).
- Strugnell RA, Wijburg OL. The role of secretory antibodies in infection immunity. Nat Rev Microbiol. Sep 2010;8(9):656-667.
- Obayashi K. Salivary mental stress proteins. Clin Chim Acta. Oct 21 2013;425:196-201.
- Strahler J, Skoluda N, Kappert MB, Nater UM. Simultaneous measurement of salivary cortisol and alpha-amylase: Application and recommendations. Neurosci Biobehav Rev. Dec 2017;83:657-677.
- Lennartsson AK, Theorell T, Rockwood AL, Kushnir MM, Jonsdottir IH. Perceived stress at work is associated with lower levels of DHEA-S. PLoS One. 2013;8(8):e72460.
- Mannic T, Viguie J, Rossier MF. In vivo and in vitro evidences of dehydroepiandrosterone protective role on the cardiovascular system. Int J Endocrinol Metab. Apr 2015;13(2):e24660.
- Samaras N, Samaras D, Frangos E, Forster A, Philippe J. A review of age-related dehydroepiandrosterone decline and its association with well-known geriatric syndromes: is treatment beneficial? Rejuvenation Res. Aug 2013;16(4):285-294.
- Shaffer F, Ginsberg JP. An Overview of Heart Rate Variability Metrics and Norms. Front Public Health. 2017;5:258.
- Kim HG, Cheon EJ, Bai DS, Lee YH, Koo BH. Stress and Heart Rate Variability: A Meta-Analysis and Review of the Literature. Psychiatry Investig. Mar 2018;15(3):235-245.
- Siegrist J, Li J. Work Stress and Altered Biomarkers: A Synthesis of Findings Based on the Effort-Reward Imbalance Model. Int J Environ Res Public Health. Nov 10 2017;14(11).
- Balzarotti S, Biassoni F, Colombo B, Ciceri MR. Cardiac vagal control as a marker of emotion regulation in healthy adults: A review. Biol Psychol. Dec 2017;130:54-66.
- Perez-Quilis C, Kingsley JD, Malkani K, Cervellin G, Lippi G, Sanchis-Gomar F. Modulation of Heart Rate by Acute or Chronic Aerobic Exercise. Potential Effects on Blood Pressure Control. Curr Pharm Des. 2017;23(31):4650-4657.
- Heckenberg RA, Eddy P, Kent S, Wright BJ. Do workplace-based mindfulness meditation programs improve physiological indices of stress? A systematic review and meta-analysis. J Psychosom Res. Nov 2018;114:62-71.
- Carnevali L, Koenig J, Sgoifo A, Ottaviani C. Autonomic and Brain Morphological Predictors of Stress Resilience. Front Neurosci. 2018;12:228.
- Cadegiani FA, Kater CE. Adrenal fatigue does not exist: a systematic review. BMC Endocr Disord. Aug 24 2016;16(1):48.
- Powell DJ, Liossi C, Moss-Morris R, Schlotz W. Unstimulated cortisol secretory activity in everyday life and its relationship with fatigue and chronic fatigue syndrome: a systematic review and subset meta-analysis. Psychoneuroendocrinology. Nov 2013;38(11):2405-2422.
- Munir S, Waseem M. Addison Disease. StatPearls. Treasure Island (FL): StatPearls Publishing LLC.; 2018.
- Koen N, Stein DJ. Pharmacotherapy of anxiety disorders: a critical review. Dialogues Clin Neurosci. 2011;13(4):423-437.
- Rougemont-Bucking A, Gamma F, Panksepp J. Use of tramadol in psychiatric care: A comprehensive review and report of two cases. Swiss Med Wkly. 2017;147:w14428.
- Santarsieri D, Schwartz TL. Antidepressant efficacy and side-effect burden: a quick guide for clinicians. Drugs Context. 2015;4:212290.
- Kirilly E, Gonda X, Bagdy G. [Antidepressants, stressors and the serotonin 1A receptor]. Neuropsychopharmacol Hung. Jun 2015;17(2):81-89.
- Gupta D, Radhakrishnan M, Bhatt S, Kurhe Y. Role of Hypothalamic-pituitary-adrenal-axis in Affective Disorders: Anti-depressant and Anxiolytic Activity of Partial 5-HT1A Agonist in Adrenalectomised Rats. Indian J Psychol Med. Jul 2013;35(3):290-298.
- Mayo Clinic. Buspirone (Oral Route): Side Effects. Available at https://www.mayoclinic.org/drugs-supplements/buspirone-oral-route/side-effects/drg-20062457. Last updated 10/1/2018. Accessed 12/27/2018. 2018.
- Bossini L, Coluccia A, Casolaro I, et al. Off-Label Trazodone Prescription: Evidence, Benefits and Risks. Curr Pharm Des. 2015;21(23):3343-3351.
- Khouzam HR. A review of trazodone use in psychiatric and medical conditions. Postgrad Med. Jan 2017;129(1):140-148.
- Steenen SA, van Wijk AJ, van der Heijden GJ, van Westrhenen R, de Lange J, de Jongh A. Propranolol for the treatment of anxiety disorders: Systematic review and meta-analysis. J Psychopharmacol. Feb 2016;30(2):128-139.
- Mayo Clinic. Beta Blockers. Available at https://www.mayoclinic.org/diseases-conditions/high-blood-pressure/in-depth/beta-blockers/art-20044522. Last updates 4/6/2018. Accessed 12/22/18. 2018.
- Akbar S, Alorainy MS. The current status of beta blockers' use in the management of hypertension. Saudi Med J. Nov 2014;35(11):1307-1317.
- Dudek D, Jaeschke R, Styczen K, Pilecki M. Depression and anxiety in the practice of cardiology. Kardiol Pol. 2013;71(8):781-786.
- Celano CM, Daunis DJ, Lokko HN, Campbell KA, Huffman JC. Anxiety Disorders and Cardiovascular Disease. Curr Psychiatry Rep. Nov 2016;18(11):101.
- Dell'Osso B, Albert U, Atti AR, et al. Bridging the gap between education and appropriate use of benzodiazepines in psychiatric clinical practice. Neuropsychiatr Dis Treat. 2015;11:1885-1909.
- Ramirez K, Niraula A, Sheridan JF. GABAergic modulation with classical benzodiazepines prevent stress-induced neuro-immune dysregulation and behavioral alterations. Brain Behav Immun. Jan 2016;51:154-168.
- Jung S, Spence MM, Escasa NM, Lee EA, Hui RL, Gibbs NE. The Risk of Pneumonia in Older Adults Using Nonbenzodiazepine Hypnotics. J Manag Care Spec Pharm. Aug 2016;22(8):932-938.
- Kuntz J, Kouch L, Christian D, Peterson PL, Gruss I. Barriers and Facilitators to the Deprescribing of Nonbenzodiazepine Sedative Medications Among Older Adults. Perm J. 2018;22.
- Wilt TJ, MacDonald R, Brasure M, et al. Pharmacologic Treatment of Insomnia Disorder: An Evidence Report for a Clinical Practice Guideline by the American College of Physicians. Ann Intern Med. Jul 19 2016;165(2):103-112.
- Cleare AJ, Miell J, Heap E, et al. Hypothalamo-pituitary-adrenal axis dysfunction in chronic fatigue syndrome, and the effects of low-dose hydrocortisone therapy. J Clin Endocrinol Metab. Aug 2001;86(8):3545-3554.
- Blockmans D, Persoons P, Van Houdenhove B, Lejeune M, Bobbaers H. Combination therapy with hydrocortisone and fludrocortisone does not improve symptoms in chronic fatigue syndrome: a randomized, placebo-controlled, double-blind, crossover study. Am J Med. Jun 15 2003;114(9):736-741.
- McKenzie R, O'Fallon A, Dale J, et al. Low-dose hydrocortisone for treatment of chronic fatigue syndrome: a randomized controlled trial. Jama. Sep 23-30 1998;280(12):1061-1066.
- Hofmann SG, Asnaani A, Vonk IJ, Sawyer AT, Fang A. The Efficacy of Cognitive Behavioral Therapy: A Review of Meta-analyses. Cognit Ther Res. Oct 1 2012;36(5):427-440.
- Lindsater E, Axelsson E, Salomonsson S, et al. Internet-Based Cognitive Behavioral Therapy for Chronic Stress: A Randomized Controlled Trial. Psychother Psychosom. 2018;87(5):296-305.
- Anclair M, Lappalainen R, Muotka J, Hiltunen AJ. Cognitive behavioural therapy and mindfulness for stress and burnout: a waiting list controlled pilot study comparing treatments for parents of children with chronic conditions. Scand J Caring Sci. Mar 2018;32(1):389-396.
- Carpenter JK, Andrews LA, Witcraft SM, Powers MB, Smits JAJ, Hofmann SG. Cognitive behavioral therapy for anxiety and related disorders: A meta-analysis of randomized placebo-controlled trials. Depress Anxiety. Jun 2018;35(6):502-514.
- Baker N. Using Cognitive Behavior Therapy and Mindfulness Techniques in the Management of Chronic Pain in Primary Care. Prim Care. Jun 2016;43(2):203-216.
- Eller-Smith OC, Nicol AL, Christianson JA. Potential Mechanisms Underlying Centralized Pain and Emerging Therapeutic Interventions. Front Cell Neurosci. 2018;12:35.
- Karlsson B, Burell G, Anderberg UM, Svardsudd K. Cognitive behaviour therapy in women with fibromyalgia: A randomized clinical trial. Scand J Pain. Oct 1 2015;9(1):11-21.
- Schiller H, Soderstrom M, Lekander M, Rajaleid K, Kecklund G. A randomized controlled intervention of workplace-based group cognitive behavioral therapy for insomnia. Int Arch Occup Environ Health. May 2018;91(4):413-424.
- Bishop JR, Lee AM, Mills LJ, et al. Methylation of FKBP5 and SLC6A4 in Relation to Treatment Response to Mindfulness Based Stress Reduction for Posttraumatic Stress Disorder. Front Psychiatry. 2018;9:418.
- Bergen-Cico D, Possemato K, Pigeon W. Reductions in cortisol associated with primary care brief mindfulness program for veterans with PTSD. Med Care. Dec 2014;52(12 Suppl 5):S25-31.
- Pascoe MC, Thompson DR, Jenkins ZM, Ski CF. Mindfulness mediates the physiological markers of stress: Systematic review and meta-analysis. J Psychiatr Res. Dec 2017;95:156-178.
- Levine GN, Lange RA, Bairey-Merz CN, et al. Meditation and Cardiovascular Risk Reduction: A Scientific Statement From the American Heart Association. J Am Heart Assoc. Sep 28 2017;6(10).
- Guillaumie L, Boiral O, Champagne J. A mixed-methods systematic review of the effects of mindfulness on nurses. J Adv Nurs. May 2017;73(5):1017-1034.
- Lamothe M, Rondeau E, Malboeuf-Hurtubise C, Duval M, Sultan S. Outcomes of MBSR or MBSR-based interventions in health care providers: A systematic review with a focus on empathy and emotional competencies. Complement Ther Med. Feb 2016;24:19-28.
- Janssen M, Heerkens Y, Kuijer W, van der Heijden B, Engels J. Effects of Mindfulness-Based Stress Reduction on employees' mental health: A systematic review. PLoS One. 2018;13(1):e0191332.
- Ravalier JM, Wegrzynek P, Lawton S. Systematic review: complementary therapies and employee well-being. Occup Med (Lond). Aug 2016;66(6):428-436.
- Daubenmier J, Kristeller J, Hecht FM, et al. Mindfulness Intervention for Stress Eating to Reduce Cortisol and Abdominal Fat among Overweight and Obese Women: An Exploratory Randomized Controlled Study. J Obes. 2011;2011:651936.
- Fish J, Brimson J, Lynch S. Mindfulness Interventions Delivered by Technology Without Facilitator Involvement: What Research Exists and What Are the Clinical Outcomes? Mindfulness (N Y). 2016;7(5):1011-1023.
- Carolan S, Harris PR, Cavanagh K. Improving Employee Well-Being and Effectiveness: Systematic Review and Meta-Analysis of Web-Based Psychological Interventions Delivered in the Workplace. J Med Internet Res. Jul 26 2017;19(7):e271.
- Heber E, Ebert DD, Lehr D, et al. The Benefit of Web- and Computer-Based Interventions for Stress: A Systematic Review and Meta-Analysis. J Med Internet Res. Feb 17 2017;19(2):e32.
- Huffman DM, Schafer MJ, LeBrasseur NK. Energetic interventions for healthspan and resiliency with aging. Exp Gerontol. Dec 15 2016;86:73-83.
- Stubbs B, Vancampfort D, Rosenbaum S, et al. An examination of the anxiolytic effects of exercise for people with anxiety and stress-related disorders: A meta-analysis. Psychiatry Res. Mar 2017;249:102-108.
- Ortega E. The "bioregulatory effect of exercise" on the innate/inflammatory responses. J Physiol Biochem. Jun 2016;72(2):361-369.
- Kline CE. The bidirectional relationship between exercise and sleep: Implications for exercise adherence and sleep improvement. Am J Lifestyle Med. Nov-Dec 2014;8(6):375-379.
- Asmundson GJ, Fetzner MG, Deboer LB, Powers MB, Otto MW, Smits JA. Let's get physical: a contemporary review of the anxiolytic effects of exercise for anxiety and its disorders. Depress Anxiety. Apr 2013;30(4):362-373.
- Mikkelsen K, Stojanovska L, Polenakovic M, Bosevski M, Apostolopoulos V. Exercise and mental health. Maturitas. Dec 2017;106:48-56.
- Huang CJ, Webb HE, Zourdos MC, Acevedo EO. Cardiovascular reactivity, stress, and physical activity. Front Physiol. Nov 7 2013;4:314.
- Bernard P, Dore I, Romain AJ, Hains-Monfette G, Kingsbury C, Sabiston C. Dose response association of objective physical activity with mental health in a representative national sample of adults: A cross-sectional study. PLoS One. 2018;13(10):e0204682.
- Gordon BR, McDowell CP, Lyons M, Herring MP. The Effects of Resistance Exercise Training on Anxiety: A Meta-Analysis and Meta-Regression Analysis of Randomized Controlled Trials. Sports Med. Dec 2017;47(12):2521-2532.
- Kovacevic A, Mavros Y, Heisz JJ, Fiatarone Singh MA. The effect of resistance exercise on sleep: A systematic review of randomized controlled trials. Sleep Med Rev. Jun 2018;39:52-68.
- Leow S, Jackson B, Alderson JA, Guelfi KJ, Dimmock JA. A Role for Exercise in Attenuating Unhealthy Food Consumption in Response to Stress. Nutrients. Feb 6 2018;10(2).
- van Praag H, Fleshner M, Schwartz MW, Mattson MP. Exercise, energy intake, glucose homeostasis, and the brain. J Neurosci. Nov 12 2014;34(46):15139-15149.
- Wasfy MM, Baggish AL. Exercise Dose in Clinical Practice. Circulation. Jun 7 2016;133(23):2297-2313.
- Mitchell M, White L, Lau E, Leahey T, Adams MA, Faulkner G. Evaluating the Carrot Rewards App, a Population-Level Incentive-Based Intervention Promoting Step Counts Across Two Canadian Provinces: Quasi-Experimental Study. JMIR Mhealth Uhealth. Sep 20 2018;6(9):e178.
- Kramer JN, Tinschert P, Scholz U, Fleisch E, Kowatsch T. A Cluster-Randomized Trial on Small Incentives to Promote Physical Activity. Am J Prev Med. Dec 13 2018.
- Yuenyongchaiwat K. Effects of 10,000 steps a day on physical and mental health in overweight participants in a community setting: a preliminary study. Braz J Phys Ther. Jul-Aug 2016;20(4):367-373.
- Liau AK, Neihart M, Teo CT, Goh LS, Chew P. A Quasi-Experimental Study of a Fitbit-Based Self-Regulation Intervention to Improve Physical Activity, Well-Being, and Mental Health. Cyberpsychol Behav Soc Netw. Nov 2018;21(11):727-734.
- Friedman E, Krause-Parello CA. Companion animals and human health: benefits, challenges, and the road ahead for human-animal interaction. Rev Sci Tech. Apr 2018;37(1):71-82.
- Ogechi I, Snook K, Davis BM, Hansen AR, Liu F, Zhang J. Pet Ownership and the Risk of Dying from Cardiovascular Disease Among Adults Without Major Chronic Medical Conditions. High Blood Press Cardiovasc Prev. Sep 2016;23(3):245-253.
- Qureshi AI, Memon MZ, Vazquez G, Suri MF. Cat ownership and the Risk of Fatal Cardiovascular Diseases. Results from the Second National Health and Nutrition Examination Study Mortality Follow-up Study. J Vasc Interv Neurol. Jan 2009;2(1):132-135.
- Arhant-Sudhir K, Arhant-Sudhir R, Sudhir K. Pet ownership and cardiovascular risk reduction: supporting evidence, conflicting data and underlying mechanisms. Clin Exp Pharmacol Physiol. Nov 2011;38(11):734-738.
- Virues-Ortega J, Buela-Casal G. Psychophysiological effects of human-animal interaction: theoretical issues and long-term interaction effects. J Nerv Ment Dis. Jan 2006;194(1):52-57.
- Pickering TG. Men are from Mars, women are from Venus: stress, pets, and oxytocin. J Clin Hypertens (Greenwich). Jan-Feb 2003;5(1):86-88.
- Lundqvist M, Carlsson P, Sjodahl R, Theodorsson E, Levin LA. Patient benefit of dog-assisted interventions in health care: a systematic review. BMC Complement Altern Med. Jul 10 2017;17(1):358.
- Polheber JP, Matchock RL. The presence of a dog attenuates cortisol and heart rate in the Trier Social Stress Test compared to human friends. J Behav Med. Oct 2014;37(5):860-867.
- Allen K, Blascovich J, Mendes WB. Cardiovascular reactivity and the presence of pets, friends, and spouses: the truth about cats and dogs. Psychosom Med. Sep-Oct 2002;64(5):727-739.
- Oyola MG, Handa RJ. Hypothalamic-pituitary-adrenal and hypothalamic-pituitary-gonadal axes: sex differences in regulation of stress responsivity. Stress. Sep 2017;20(5):476-494.
- Toufexis D, Rivarola MA, Lara H, Viau V. Stress and the reproductive axis. J Neuroendocrinol. Sep 2014;26(9):573-586.
- Stephens MA, Mahon PB, McCaul ME, Wand GS. Hypothalamic-pituitary-adrenal axis response to acute psychosocial stress: Effects of biological sex and circulating sex hormones. Psychoneuroendocrinology. Apr 2016;66:47-55.
- Wirth MM. Beyond the HPA Axis: Progesterone-Derived Neuroactive Steroids in Human Stress and Emotion. Front Endocrinol (Lausanne). 2011;2:19.
- Ziomkiewicz A, Pawlowski B, Ellison PT, Lipson SF, Thune I, Jasienska G. Higher luteal progesterone is associated with low levels of premenstrual aggressive behavior and fatigue. Biol Psychol. Dec 2012;91(3):376-382.
- Patacchioli FR, Ghiciuc CM, Bernardi M, et al. Salivary alpha-amylase and cortisol after exercise in menopause: influence of long-term HRT. Climacteric. 2015;18(4):528-535.
- Herrera AY, Hodis HN, Mack WJ, Mather M. Estradiol Therapy After Menopause Mitigates Effects of Stress on Cortisol and Working Memory. J Clin Endocrinol Metab. Dec 1 2017;102(12):4457-4466.
- Steffen AM, Thompson LW, Gallagher-Thompson D, Koin D. Physical and psychosocial correlates of hormone replacement therapy with chronically stressed postmenopausal women. J Aging Health. Feb 1999;11(1):3-26.
- Prior JC. Progesterone for Symptomatic Perimenopause Treatment - Progesterone politics, physiology and potential for perimenopause. Facts Views Vis Obgyn. 2011;3(2):109-120.
- Leeangkoonsathian E, Pantasri T, Chaovisitseree S, Morakot N. The effect of different progestogens on sleep in postmenopausal women: a randomized trial. Gynecol Endocrinol. Dec 2017;33(12):933-936.
- Espinosa-Garcia C, Sayeed I, Yousuf S, et al. Stress primes microglial polarization after global ischemia: Therapeutic potential of progesterone. Brain Behav Immun. Nov 2017;66:177-192.
- Tomiyama AJ, Dallman MF, Epel ES. Comfort food is comforting to those most stressed: evidence of the chronic stress response network in high stress women. Psychoneuroendocrinology. Nov 2011;36(10):1513-1519.
- Jaremka LM, Belury MA, Andridge RR, et al. Interpersonal stressors predict ghrelin and leptin levels in women. Psychoneuroendocrinology. Oct 2014;48:178-188.
- Yau YH, Potenza MN. Stress and eating behaviors. Minerva Endocrinol. Sep 2013;38(3):255-267.
- Tryon MS, DeCant R, Laugero KD. Having your cake and eating it too: a habit of comfort food may link chronic social stress exposure and acute stress-induced cortisol hyporesponsiveness. Physiol Behav. Apr 10 2013;114-115:32-37.
- Tryon MS, Stanhope KL, Epel ES, et al. Excessive Sugar Consumption May Be a Difficult Habit to Break: A View From the Brain and Body. J Clin Endocrinol Metab. Jun 2015;100(6):2239-2247.
- Errisuriz VL, Pasch KE, Perry CL. Perceived stress and dietary choices: The moderating role of stress management. Eat Behav. Aug 2016;22:211-216.
- Aschbacher K, Kornfeld S, Picard M, et al. Chronic stress increases vulnerability to diet-related abdominal fat, oxidative stress, and metabolic risk. Psychoneuroendocrinology. Aug 2014;46:14-22.
- Wang J, Um P, Dickerman BA, Liu J. Zinc, Magnesium, Selenium and Depression: A Review of the Evidence, Potential Mechanisms and Implications. Nutrients. May 9 2018;10(5).
- Singh K. Nutrient and Stress Management. J Nutr Food Sci. 2016;6(4).
- Conner TS, Brookie KL, Carr AC, Mainvil LA, Vissers MC. Let them eat fruit! The effect of fruit and vegetable consumption on psychological well-being in young adults: A randomized controlled trial. PLoS One. 2017;12(2):e0171206.
- Garcia-Prieto MD, Tebar FJ, Nicolas F, Larque E, Zamora S, Garaulet M. Cortisol secretary pattern and glucocorticoid feedback sensitivity in women from a Mediterranean area: relationship with anthropometric characteristics, dietary intake and plasma fatty acid profile. Clin Endocrinol (Oxf). Feb 2007;66(2):185-191.
- Carvalho KMB, Ronca DB, Michels N, et al. Does the Mediterranean Diet Protect against Stress-Induced Inflammatory Activation in European Adolescents? The HELENA Study. Nutrients. Nov 15 2018;10(11).
- Martucci M, Ostan R, Biondi F, et al. Mediterranean diet and inflammaging within the hormesis paradigm. Nutr Rev. Jun 1 2017;75(6):442-455.
- Chaplin K, Smith AP. Breakfast and snacks: associations with cognitive failures, minor injuries, accidents and stress. Nutrients. May 2011;3(5):515-528.
- Witbracht M, Keim NL, Forester S, Widaman A, Laugero K. Female breakfast skippers display a disrupted cortisol rhythm and elevated blood pressure. Physiol Behav. Mar 1 2015;140:215-221.
- Nehlig A. Effects of coffee/caffeine on brain health and disease: What should I tell my patients? Pract Neurol. Apr 2016;16(2):89-95.
- Yang A, Palmer AA, de Wit H. Genetics of caffeine consumption and responses to caffeine. Psychopharmacology (Berl). Aug 2010;211(3):245-257.
- al'Absi M, & Lovallo, W. R. . Caffeine's effects on the human stress axis. In A. Nehlig (Ed.), Nutrition, brain, and behavior. Coffee, tea, chocolate, and the brain (pp. 113-131). Boca Raton, FL, US: CRC Press. http://dx.doi.org/10.1201/9780203618851.ch8. 2004.
- Lovallo WR, Whitsett TL, al'Absi M, Sung BH, Vincent AS, Wilson MF. Caffeine stimulation of cortisol secretion across the waking hours in relation to caffeine intake levels. Psychosom Med. Sep-Oct 2005;67(5):734-739.
- Lovallo WR, Farag NH, Vincent AS, Thomas TL, Wilson MF. Cortisol responses to mental stress, exercise, and meals following caffeine intake in men and women. Pharmacol Biochem Behav. Mar 2006;83(3):441-447.
- Gonzaga LA, Vanderlei LCM, Gomes RL, Valenti VE. Caffeine affects autonomic control of heart rate and blood pressure recovery after aerobic exercise in young adults: a crossover study. Sci Rep. Oct 26 2017;7(1):14091.
- Hamer M, Williams ED, Vuononvirta R, Gibson EL, Steptoe A. Association between coffee consumption and markers of inflammation and cardiovascular function during mental stress. J Hypertens. Nov 2006;24(11):2191-2197.
- Beaudoin MS, Graham TE. Methylxanthines and human health: epidemiological and experimental evidence. Handb Exp Pharmacol. 2011(200):509-548.
- Schrieks IC, Joosten MM, Klopping-Ketelaars WA, Witkamp RF, Hendriks HF. Moderate alcohol consumption after a mental stressor attenuates the endocrine stress response. Alcohol. Dec 2016;57:29-34.
- Kokavec A, Crowe SF. The effect of a moderate level of white wine consumption on the hypothalamic-pituitary-adrenal axis before and after a meal. Pharmacol Biochem Behav. Oct-Nov 2001;70(2-3):243-250.
- Cupic Z, Stanojevic A, Markovic VM, Kolar-Anic L, Terenius L, Vukojevic V. The HPA axis and ethanol: a synthesis of mathematical modelling and experimental observations. Addict Biol. Nov 2017;22(6):1486-1500.
- Rachdaoui N, Sarkar DK. Pathophysiology of the Effects of Alcohol Abuse on the Endocrine System. Alcohol Res. 2017;38(2):255-276.
- Blaine SK, Sinha R. Alcohol, stress, and glucocorticoids: From risk to dependence and relapse in alcohol use disorders. Neuropharmacology. Aug 1 2017;122:136-147.
- Hipson WE, Fisher DJ. The association between acute stress-related insomnia and alcohol use. Sleep Health. Sep 2016;2(3):246-252.
- Keyes KM, Hatzenbuehler ML, Grant BF, Hasin DS. Stress and alcohol: epidemiologic evidence. Alcohol Res. 2012;34(4):391-400.
- Leahy LG. Vitamin B Supplementation: What's the Right Choice for Your Patients? J Psychosoc Nurs Ment Health Serv. Jul 1 2017;55(7):7-11.
- Kennedy DO. B Vitamins and the Brain: Mechanisms, Dose and Efficacy--A Review. Nutrients. Jan 27 2016;8(2):68.
- Macpherson H, Rowsell R, Cox KH, et al. The Effects of Four-Week Multivitamin Supplementation on Mood in Healthy Older Women: A Randomized Controlled Trial. Evid Based Complement Alternat Med. 2016;2016:3092828.
- Macpherson H, Rowsell R, Cox KH, Scholey A, Pipingas A. Acute mood but not cognitive improvements following administration of a single multivitamin and mineral supplement in healthy women aged 50 and above: a randomised controlled trial. Age (Dordr). Jun 2015;37(3):9782.
- Pipingas A, Camfield DA, Stough C, et al. The effects of multivitamin supplementation on mood and general well-being in healthy young adults. A laboratory and at-home mobile phone assessment. Appetite. Oct 2013;69:123-136.
- Sarris J, Cox KH, Camfield DA, et al. Participant experiences from chronic administration of a multivitamin versus placebo on subjective health and wellbeing: a double-blind qualitative analysis of a randomised controlled trial. Nutr J. Dec 14 2012;11:110.
- Harris E, Kirk J, Rowsell R, et al. The effect of multivitamin supplementation on mood and stress in healthy older men. Hum Psychopharmacol. Dec 2011;26(8):560-567.
- Stough C, Scholey A, Lloyd J, Spong J, Myers S, Downey LA. The effect of 90 day administration of a high dose vitamin B-complex on work stress. Hum Psychopharmacol. Oct 2011;26(7):470-476.
- Long SJ, Benton D. Effects of vitamin and mineral supplementation on stress, mild psychiatric symptoms, and mood in nonclinical samples: a meta-analysis. Psychosom Med. Feb 2013;75(2):144-153.
- Camfield DA, Wetherell MA, Scholey AB, et al. The effects of multivitamin supplementation on diurnal cortisol secretion and perceived stress. Nutrients. Nov 11 2013;5(11):4429-4450.
- Li X, Huang WX, Lu JM, et al. Effects of a multivitamin/multimineral supplement on young males with physical overtraining: a placebo-controlled, randomized, double-blinded cross-over trial. Biomed Environ Sci. Jul 2013;26(7):599-604.
- Figueroa-Méndez R, Rivas-Arancibia S. Vitamin C in Health and Disease: Its Role in the Metabolism of Cells and Redox State in the Brain. Front Physiol. 2015;6:397.
- Kocot J, Luchowska-Kocot D, Kielczykowska M, Musik I, Kurzepa J. Does Vitamin C Influence Neurodegenerative Diseases and Psychiatric Disorders? Nutrients. Jun 27 2017;9(7).
- Han QQ, Shen TT, Wang F, Wu PF, Chen JG. Preventive and Therapeutic Potential of Vitamin C in Mental Disorders. Curr Med Sci. Feb 2018;38(1):1-10.
- Chambial S, Dwivedi S, Shukla KK, John PJ, Sharma P. Vitamin C in disease prevention and cure: an overview. Indian J Clin Biochem. Oct 2013;28(4):314-328.
- Gautam M, Agrawal M, Gautam M, Sharma P, Gautam AS, Gautam S. Role of antioxidants in generalised anxiety disorder and depression. Indian J Psychiatry. Jul 2012;54(3):244-247.
- de Oliveira IJ, de Souza VV, Motta V, Da-Silva SL. Effects of Oral Vitamin C Supplementation on Anxiety in Students: A Double-Blind, Randomized, Placebo-Controlled Trial. Pak J Biol Sci. Jan 2015;18(1):11-18.
- McCabe D, Lisy K, Lockwood C, Colbeck M. The impact of essential fatty acid, B vitamins, vitamin C, magnesium and zinc supplementation on stress levels in women: a systematic review. JBI Database System Rev Implement Rep. Feb 2017;15(2):402-453.
- Taylor AM, Holscher HD. A review of dietary and microbial connections to depression, anxiety, and stress. Nutr Neurosci. Jul 9 2018:1-14.
- Husted KS, Bouzinova EV. The importance of n-6/n-3 fatty acids ratio in the major depressive disorder. Medicina (Kaunas). 2016;52(3):139-147.
- Su KP, Matsuoka Y, Pae CU. Omega-3 Polyunsaturated Fatty Acids in Prevention of Mood and Anxiety Disorders. Clin Psychopharmacol Neurosci. Aug 31 2015;13(2):129-137.
- Thesing CS, Bot M, Milaneschi Y, Giltay EJ, Penninx B. Omega-3 polyunsaturated fatty acid levels and dysregulations in biological stress systems. Psychoneuroendocrinology. Nov 2018;97:206-215.
- Fernandes MF, Mutch DM, Leri F. The Relationship between Fatty Acids and Different Depression-Related Brain Regions, and Their Potential Role as Biomarkers of Response to Antidepressants. Nutrients. Mar 17 2017;9(3).
- Sauder KA, Skulas-Ray AC, Campbell TS, Johnson JA, Kris-Etherton PM, West SG. Effects of omega-3 fatty acid supplementation on heart rate variability at rest and during acute stress in adults with moderate hypertriglyceridemia. Psychosom Med. May 2013;75(4):382-389.
- Barbadoro P, Annino I, Ponzio E, et al. Fish oil supplementation reduces cortisol basal levels and perceived stress: a randomized, placebo-controlled trial in abstinent alcoholics. Mol Nutr Food Res. Jun 2013;57(6):1110-1114.
- Mocking RJ, Verburg HF, Westerink AM, et al. Fatty acid metabolism and its longitudinal relationship with the hypothalamic-pituitary-adrenal axis in major depression: Associations with prospective antidepressant response. Psychoneuroendocrinology. Sep 2015;59:1-13.
- Turkozu D, Sanlier N. L-theanine, unique amino acid of tea, and its metabolism, health effects, and safety. Crit Rev Food Sci Nutr. May 24 2017;57(8):1681-1687.
- Unno K, Tanida N, Ishii N, et al. Anti-stress effect of theanine on students during pharmacy practice: positive correlation among salivary alpha-amylase activity, trait anxiety and subjective stress. Pharmacol Biochem Behav. Oct 2013;111:128-135.
- White DJ, de Klerk S, Woods W, Gondalia S, Noonan C, Scholey AB. Anti-Stress, Behavioural and Magnetoencephalography Effects of an L-Theanine-Based Nutrient Drink: A Randomised, Double-Blind, Placebo-Controlled, Crossover Trial. Nutrients. Jan 19 2016;8(1).
- Giles GE, Mahoney CR, Brunye TT, Taylor HA, Kanarek RB. Caffeine and theanine exert opposite effects on attention under emotional arousal. Can J Physiol Pharmacol. Jan 2017;95(1):93-100.
- Cicero AF, Bove M, Colletti A, et al. Short-Term Impact of a Combined Nutraceutical on Cognitive Function, Perceived Stress and Depression in Young Elderly with Cognitive Impairment: A Pilot, Double-Blind, Randomized Clinical Trial. J Prev Alzheimers Dis. 2017;4(1):12-15.
- Kingsley M. Effects of phosphatidylserine supplementation on exercising humans. Sports Med. 2006;36(8):657-669.
- Hellhammer J, Vogt D, Franz N, Freitas U, Rutenberg D. A soy-based phosphatidylserine/ phosphatidic acid complex (PAS) normalizes the stress reactivity of hypothalamus-pituitary-adrenal-axis in chronically stressed male subjects: a randomized, placebo-controlled study. Lipids Health Dis. Jul 31 2014;13:121.
- Hellhammer J, Fries E, Buss C, et al. Effects of soy lecithin phosphatidic acid and phosphatidylserine complex (PAS) on the endocrine and psychological responses to mental stress. Stress. Jun 2004;7(2):119-126.
- Benton D, Donohoe RT, Sillance B, Nabb S. The influence of phosphatidylserine supplementation on mood and heart rate when faced with an acute stressor. Nutr Neurosci. 2001;4(3):169-178.
- Starks MA, Starks SL, Kingsley M, Purpura M, Jager R. The effects of phosphatidylserine on endocrine response to moderate intensity exercise. J Int Soc Sports Nutr. Jul 28 2008;5:11.
- Porter RJ, Gallagher P, Watson S, Young AH. Corticosteroid-serotonin interactions in depression: a review of the human evidence. Psychopharmacology (Berl). Apr 2004;173(1-2):1-17.
- Michels N, Clarke G, Olavarria-Ramirez L, et al. Psychosocial stress and inflammation driving tryptophan breakdown in children and adolescents: A cross-sectional analysis of two cohorts. Psychoneuroendocrinology. Aug 2018;94:104-111.
- Hood SD, Hince DA, Robinson H, Cirillo M, Christmas D, Kaye JM. Serotonin regulation of the human stress response. Psychoneuroendocrinology. Oct 2006;31(9):1087-1097.
- Capello AE, Markus CR. Effect of sub chronic tryptophan supplementation on stress-induced cortisol and appetite in subjects differing in 5-HTTLPR genotype and trait neuroticism. Psychoneuroendocrinology. Jul 2014;45:96-107.
- Cerit H, Jans LA, Van der Does W. The effect of tryptophan on the cortisol response to social stress is modulated by the 5-HTTLPR genotype. Psychoneuroendocrinology. Feb 2013;38(2):201-208.
- Markus CR, Firk C. Differential effects of tri-allelic 5-HTTLPR polymorphisms in healthy subjects on mood and stress performance after tryptophan challenge. Neuropsychopharmacology. Dec 2009;34(13):2667-2674.
- Firk C, Markus CR. Mood and cortisol responses following tryptophan-rich hydrolyzed protein and acute stress in healthy subjects with high and low cognitive reactivity to depression. Clin Nutr. Jun 2009;28(3):266-271.
- Mohanty DP, Mohapatra S, Misra S, Sahu PS. Milk derived bioactive peptides and their impact on human health - A review. Saudi J Biol Sci. Sep 2016;23(5):577-583.
- Layman DK, Lonnerdal B, Fernstrom JD. Applications for alpha-lactalbumin in human nutrition. Nutr Rev. Jun 1 2018;76(6):444-460.
- Yayeh T, Leem YH, Kim KM, et al. Administration of Alphas1-Casein Hydrolysate Increases Sleep and Modulates GABAA Receptor Subunit Expression. Biomol Ther (Seoul). May 1 2018;26(3):268-273.
- Dela Pena IJ, Kim HJ, de la Pena JB, et al. A tryptic hydrolysate from bovine milk alphas1-casein enhances pentobarbital-induced sleep in mice via the GABAA receptor. Behav Brain Res. Oct 15 2016;313:184-190.
- Guesdon B, Messaoudi M, Lefranc-Millot C, Fromentin G, Tome D, Even PC. A tryptic hydrolysate from bovine milk alphaS1-casein improves sleep in rats subjected to chronic mild stress. Peptides. Jun 2006;27(6):1476-1482.
- Kim JH, Desor D, Kim YT, et al. Efficacy of alphas1-casein hydrolysate on stress-related symptoms in women. Eur J Clin Nutr. Apr 2007;61(4):536-541.
- Messaoudi M, Lefranc-Millot C, Desor D, Demagny B, Bourdon L. Effects of a tryptic hydrolysate from bovine milk alphaS1-casein on hemodynamic responses in healthy human volunteers facing successive mental and physical stress situations. Eur J Nutr. Mar 2005;44(2):128-132.
- Misra S, Mohanty D. Psychobiotics: A new approach for treating mental illness? Crit Rev Food Sci Nutr. Nov 30 2017:1-7.
- Takada M, Nishida K, Kataoka-Kato A, et al. Probiotic Lactobacillus casei strain Shirota relieves stress-associated symptoms by modulating the gut-brain interaction in human and animal models. Neurogastroenterol Motil. Jul 2016;28(7):1027-1036.
- Kato-Kataoka A, Nishida K, Takada M, et al. Fermented milk containing Lactobacillus casei strain Shirota prevents the onset of physical symptoms in medical students under academic examination stress. Benef Microbes. 2016;7(2):153-156.
- Kato-Kataoka A, Nishida K, Takada M, et al. Fermented Milk Containing Lactobacillus casei Strain Shirota Preserves the Diversity of the Gut Microbiota and Relieves Abdominal Dysfunction in Healthy Medical Students Exposed to Academic Stress. Appl Environ Microbiol. Jun 15 2016;82(12):3649-3658.
- Andersson H, Tullberg C, Ahrne S, et al. Oral Administration of Lactobacillus plantarum 299v Reduces Cortisol Levels in Human Saliva during Examination Induced Stress: A Randomized, Double-Blind Controlled Trial. Int J Microbiol. 2016;2016:8469018.
- Messaoudi M, Lalonde R, Violle N, et al. Assessment of psychotropic-like properties of a probiotic formulation (Lactobacillus helveticus R0052 and Bifidobacterium longum R0175) in rats and human subjects. Br J Nutr. Mar 2011;105(5):755-764.
- Allen AP, Hutch W, Borre YE, et al. Bifidobacterium longum 1714 as a translational psychobiotic: modulation of stress, electrophysiology and neurocognition in healthy volunteers. Transl Psychiatry. Nov 1 2016;6(11):e939.
- Schmidt K, Cowen PJ, Harmer CJ, Tzortzis G, Errington S, Burnet PW. Prebiotic intake reduces the waking cortisol response and alters emotional bias in healthy volunteers. Psychopharmacology (Berl). May 2015;232(10):1793-1801.
- Gamble KL, Berry R, Frank SJ, Young ME. Circadian clock control of endocrine factors. Nat Rev Endocrinol. Aug 2014;10(8):466-475.
- Hardeland R. Melatonin in aging and disease -multiple consequences of reduced secretion, options and limits of treatment. Aging Dis. Apr 2012;3(2):194-225.
- Tsang AH, Barclay JL, Oster H. Interactions between endocrine and circadian systems. J Mol Endocrinol. Feb 2014;52(1):R1-16.
- Burman D. Sleep Disorders: Circadian Rhythm Sleep-Wake Disorders. FP Essent. Sep 2017;460:33-36.
- Xie Z, Chen F, Li WA, et al. A review of sleep disorders and melatonin. Neurol Res. Jun 2017;39(6):559-565.
- Auld F, Maschauer EL, Morrison I, Skene DJ, Riha RL. Evidence for the efficacy of melatonin in the treatment of primary adult sleep disorders. Sleep Med Rev. Aug 2017;34:10-22.
- Zisapel N. New perspectives on the role of melatonin in human sleep, circadian rhythms and their regulation. Br J Pharmacol. Jan 10 2018.
- Pawlikowski M, Kolomecka M, Wojtczak A, Karasek M. Effects of six months melatonin treatment on sleep quality and serum concentrations of estradiol, cortisol, dehydroepiandrosterone sulfate, and somatomedin C in elderly women. Neuro Endocrinol Lett. Apr 2002;23 Suppl 1:17-19.
- Morales AJ, Nolan JJ, Nelson JC, Yen SS. Effects of replacement dose of dehydroepiandrosterone in men and women of advancing age. J Clin Endocrinol Metab. Jun 1994;78(6):1360-1367.
- Alhaj HA, Massey AE, McAllister-Williams RH. Effects of DHEA administration on episodic memory, cortisol and mood in healthy young men: a double-blind, placebo-controlled study. Psychopharmacology (Berl). Nov 2006;188(4):541-551.
- Liao LY, He YF, Li L, et al. A preliminary review of studies on adaptogens: comparison of their bioactivity in TCM with that of ginseng-like herbs used worldwide. Chin Med. 2018;13:57.
- Panossian A. Understanding adaptogenic activity: specificity of the pharmacological action of adaptogens and other phytochemicals. Ann N Y Acad Sci. Aug 2017;1401(1):49-64.
- Panossian A, Wikman G. Effects of Adaptogens on the Central Nervous System and the Molecular Mechanisms Associated with Their Stress-Protective Activity. Pharmaceuticals (Basel). Jan 19 2010;3(1):188-224.
- Lee YJ, Lee YM, Lee CK, Jung JK, Han SB, Hong JT. Therapeutic applications of compounds in the Magnolia family. Pharmacol Ther. May 2011;130(2):157-176.
- Xu Q, Yi LT, Pan Y, et al. Antidepressant-like effects of the mixture of honokiol and magnolol from the barks of Magnolia officinalis in stressed rodents. Prog Neuropsychopharmacol Biol Psychiatry. Apr 1 2008;32(3):715-725.
- Li LF, Lu J, Li XM, et al. Antidepressant-like effect of magnolol on BDNF up-regulation and serotonergic system activity in unpredictable chronic mild stress treated rats. Phytother Res. Aug 2012;26(8):1189-1194.
- Wang C, Gan D, Wu J, Liao M, Liao X, Ai W. Honokiol Exerts Antidepressant Effects in Rats Exposed to Chronic Unpredictable Mild Stress by Regulating Brain Derived Neurotrophic Factor Level and Hypothalamus-Pituitary-Adrenal Axis Activity. Neurochem Res. Aug 2018;43(8):1519-1528.
- Cheng J, Dong S, Yi L, Geng D, Liu Q. Magnolol abrogates chronic mild stress-induced depressive-like behaviors by inhibiting neuroinflammation and oxidative stress in the prefrontal cortex of mice. Int Immunopharmacol. Jun 2018;59:61-67.
- Talbott SM, Talbott JA, Pugh M. Effect of Magnolia officinalis and Phellodendron amurense (Relora(R)) on cortisol and psychological mood state in moderately stressed subjects. J Int Soc Sports Nutr. 2013;10(1):37.
- Garrison R, Chambliss WG. Effect of a proprietary Magnolia and Phellodendron extract on weight management: a pilot, double-blind, placebo-controlled clinical trial. Altern Ther Health Med. Jan-Feb 2006;12(1):50-54.
- Kalman DS, Feldman S, Feldman R, Schwartz HI, Krieger DR, Garrison R. Effect of a proprietary Magnolia and Phellodendron extract on stress levels in healthy women: a pilot, double-blind, placebo-controlled clinical trial. Nutr J. Apr 21 2008;7:11.
- Cohen MM. Tulsi - Ocimum sanctum: A herb for all reasons. J Ayurveda Integr Med. Oct-Dec 2014;5(4):251-259.
- Jamshidi N, Cohen MM. The Clinical Efficacy and Safety of Tulsi in Humans: A Systematic Review of the Literature. Evid Based Complement Alternat Med. 2017;2017:9217567.
- Sampath S, Mahapatra SC, Padhi MM, Sharma R, Talwar A. Holy basil (Ocimum sanctum Linn.) leaf extract enhances specific cognitive parameters in healthy adult volunteers: A placebo controlled study. Indian J Physiol Pharmacol. Jan-Mar 2015;59(1):69-77.
- Saxena RC, Singh R, Kumar P, et al. Efficacy of an Extract of Ocimum tenuiflorum (OciBest) in the Management of General Stress: A Double-Blind, Placebo-Controlled Study. Evid Based Complement Alternat Med. 2012;2012:894509.
- Bhattacharyya D, Sur TK, Jana U, Debnath PK. Controlled programmed trial of Ocimum sanctum leaf on generalized anxiety disorders. Nepal Med Coll J. Sep 2008;10(3):176-179.
- Singh N, Bhalla M, de Jager P, Gilca M. An overview on ashwagandha: a Rasayana (rejuvenator) of Ayurveda. Afr J Tradit Complement Altern Med. 2011;8(5 Suppl):208-213.
- Yenisetti SC, Manjunath MJ, Muralidhara C. Neuropharmacological Properties of Withania somnifera - Indian Ginseng: An Overview on Experimental Evidence with Emphasis on Clinical Trials and Patents. Recent Pat CNS Drug Discov. 2016;10(2):204-215.
- Dar PA, Singh LR, Kamal MA, Dar TA. Unique Medicinal Properties of Withania somnifera: Phytochemical Constituents and Protein Component. Curr Pharm Des. 2016;22(5):535-540.
- Dar NJ, Hamid A, Ahmad M. Pharmacologic overview of Withania somnifera, the Indian Ginseng. Cell Mol Life Sci. Dec 2015;72(23):4445-4460.
- Pratte MA, Nanavati KB, Young V, Morley CP. An alternative treatment for anxiety: a systematic review of human trial results reported for the Ayurvedic herb ashwagandha (Withania somnifera). J Altern Complement Med. Dec 2014;20(12):901-908.
- Chandrasekhar K, Kapoor J, Anishetty S. A prospective, randomized double-blind, placebo-controlled study of safety and efficacy of a high-concentration full-spectrum extract of ashwagandha root in reducing stress and anxiety in adults. Indian J Psychol Med. Jul 2012;34(3):255-262.
- Choudhary D, Bhattacharyya S, Joshi K. Body Weight Management in Adults Under Chronic Stress Through Treatment With Ashwagandha Root Extract: A Double-Blind, Randomized, Placebo-Controlled Trial. J Evid Based Complementary Altern Med. Jan 2017;22(1):96-106.
- Aguiar S, Borowski T. Neuropharmacological review of the nootropic herb Bacopa monnieri. Rejuvenation Res. Aug 2013;16(4):313-326.
- Sheikh N, Ahmad A, Siripurapu KB, Kuchibhotla VK, Singh S, Palit G. Effect of Bacopa monniera on stress induced changes in plasma corticosterone and brain monoamines in rats. J Ethnopharmacol. May 22 2007;111(3):671-676.
- Liu X, Liu F, Yue R, et al. The antidepressant-like effect of bacopaside I: possible involvement of the oxidative stress system and the noradrenergic system. Pharmacol Biochem Behav. Sep 2013;110:224-230.
- Kumar SS, Saraswathi P, Vijayaraghavan R. Effect of bacopa monniera on cold stress induced neurodegeneration in hippocampus of wistar rats: a histomorphometric study. J Clin Diagn Res. Jan 2015;9(1):Af05-07.
- Rai D, Bhatia G, Palit G, Pal R, Singh S, Singh HK. Adaptogenic effect of Bacopa monniera (Brahmi). Pharmacol Biochem Behav. Jul 2003;75(4):823-830.
- Chowdhuri DK, Parmar D, Kakkar P, Shukla R, Seth PK, Srimal RC. Antistress effects of bacosides of Bacopa monnieri: modulation of Hsp70 expression, superoxide dismutase and cytochrome P450 activity in rat brain. Phytother Res. Nov 2002;16(7):639-645.
- Banerjee R, Hazra S, Ghosh AK, Mondal AC. Chronic administration of bacopa monniera increases BDNF protein and mRNA expressions: a study in chronic unpredictable stress induced animal model of depression. Psychiatry Investig. Jul 2014;11(3):297-306.
- Hazra S, Kumar S, Saha GK, Mondal AC. Reversion of BDNF, Akt and CREB in Hippocampus of Chronic Unpredictable Stress Induced Rats: Effects of Phytochemical, Bacopa Monnieri. Psychiatry Investig. Jan 2017;14(1):74-80.
- Zu X, Zhang M, Li W, et al. Antidepressant-like Effect of Bacopaside I in Mice Exposed to Chronic Unpredictable Mild Stress by Modulating the Hypothalamic-Pituitary-Adrenal Axis Function and Activating BDNF Signaling Pathway. Neurochem Res. Nov 2017;42(11):3233-3244.
- Kumar S, Mondal AC. Neuroprotective, Neurotrophic and Anti-oxidative Role of Bacopa monnieri on CUS Induced Model of Depression in Rat. Neurochem Res. Nov 2016;41(11):3083-3094.
- Phulara SC, Shukla V, Tiwari S, Pandey R. Bacopa monnieri promotes longevity in Caenorhabditis elegans under stress conditions. Pharmacogn Mag. Apr-Jun 2015;11(42):410-416.
- Benson S, Downey LA, Stough C, Wetherell M, Zangara A, Scholey A. An acute, double-blind, placebo-controlled cross-over study of 320 mg and 640 mg doses of Bacopa monnieri (CDRI 08) on multitasking stress reactivity and mood. Phytother Res. Apr 2014;28(4):551-559.
- Calabrese C, Gregory WL, Leo M, Kraemer D, Bone K, Oken B. Effects of a standardized Bacopa monnieri extract on cognitive performance, anxiety, and depression in the elderly: a randomized, double-blind, placebo-controlled trial. J Altern Complement Med. Jul 2008;14(6):707-713.
- Shakeri A, Sahebkar A, Javadi B. Melissa officinalis L. - A review of its traditional uses, phytochemistry and pharmacology. J Ethnopharmacol. Jul 21 2016;188:204-228.
- Miraj S, Rafieian K, Kiani S. Melissa officinalis L: A Review Study With an Antioxidant Prospective. J Evid Based Complementary Altern Med. Jul 2017;22(3):385-394.
- Scholey A, Gibbs A, Neale C, et al. Anti-stress effects of lemon balm-containing foods. Nutrients. Oct 30 2014;6(11):4805-4821.
- Kennedy DO, Little W, Scholey AB. Attenuation of laboratory-induced stress in humans after acute administration of Melissa officinalis (Lemon Balm). Psychosom Med. Jul-Aug 2004;66(4):607-613.
- Cases J, Ibarra A, Feuillere N, Roller M, Sukkar SG. Pilot trial of Melissa officinalis L. leaf extract in the treatment of volunteers suffering from mild-to-moderate anxiety disorders and sleep disturbances. Med J Nutrition Metab. Dec 2011;4(3):211-218.
- Haybar H, Javid AZ, Haghighizadeh MH, Valizadeh E, Mohaghegh SM, Mohammadzadeh A. The effects of Melissa officinalis supplementation on depression, anxiety, stress, and sleep disorder in patients with chronic stable angina. Clin Nutr ESPEN. Aug 2018;26:47-52.
- Dolatabadi F, Abdolghaffari AH, Farzaei MH, et al. The Protective Effect of Melissa officinalis L. in Visceral Hypersensitivity in Rat Using 2 Models of Acid-induced Colitis and Stress-induced Irritable Bowel Syndrome: A Possible Role of Nitric Oxide Pathway. J Neurogastroenterol Motil. Jul 30 2018;24(3):490-501.
- Gohari AR, Saeidnia S, Mahmoodabadi MK. An overview on saffron, phytochemicals, and medicinal properties. Pharmacogn Rev. Jan-Jun 2013;7(13):61-66.
- Shafiee M, Arekhi S, Omranzadeh A, Sahebkar A. Saffron in the treatment of depression, anxiety and other mental disorders: Current evidence and potential mechanisms of action. J Affect Disord. Feb 2018;227:330-337.
- Pitsikas N. Constituents of Saffron (Crocus sativus L.) as Potential Candidates for the Treatment of Anxiety Disorders and Schizophrenia. Molecules. Mar 02 2016;21(3):303.
- Ghadrdoost B, Vafaei AA, Rashidy-Pour A, et al. Protective effects of saffron extract and its active constituent crocin against oxidative stress and spatial learning and memory deficits induced by chronic stress in rats. Eur J Pharmacol. Sep 30 2011;667(1-3):222-229.
- Dastgerdi AH, Radahmadi M, Pourshanazari AA, Dastgerdi HH. Effects of Crocin on Learning and Memory in Rats Under Chronic Restraint Stress with Special Focus on the Hippocampal and Frontal Cortex Corticosterone Levels. Adv Biomed Res. 2017;6:157.
- Bandegi AR, Rashidy-Pour A, Vafaei AA, Ghadrdoost B. Protective Effects of Crocus Sativus L. Extract and Crocin against Chronic-Stress Induced Oxidative Damage of Brain, Liver and Kidneys in Rats. Adv Pharm Bull. Dec 2014;4(Suppl 2):493-499.
- Farkhondeh T, Samarghandian S, Samini F, Sanati AR. Protective Effects of Crocetin on Depression-like Behavior Induced by Immobilization in Rat. CNS Neurol Disord Drug Targets. 2018;17(5):361-369.
- Kell G, Rao A, Beccaria G, Clayton P, Inarejos-Garcia AM, Prodanov M. affron((R)) a novel saffron extract (Crocus sativus L.) improves mood in healthy adults over 4 weeks in a double-blind, parallel, randomized, placebo-controlled clinical trial. Complement Ther Med. Aug 2017;33:58-64.
- Xu W, Choi HK, Huang L. State of Panax ginseng Research: A Global Analysis. Molecules. Sep 11 2017;22(9).
- Kim JH, Yi YS, Kim MY, Cho JY. Role of ginsenosides, the main active components of Panax ginseng, in inflammatory responses and diseases. J Ginseng Res. Oct 2017;41(4):435-443.
- Kim KH, Lee D, Lee HL, Kim CE, Jung K, Kang KS. Beneficial effects of Panax ginseng for the treatment and prevention of neurodegenerative diseases: past findings and future directions. J Ginseng Res. Jul 2018;42(3):239-247.
- Kim JH. Pharmacological and medical applications of Panax ginseng and ginsenosides: a review for use in cardiovascular diseases. J Ginseng Res. Jul 2018;42(3):264-269.
- Lee YM, Yoon H, Park HM, Song BC, Yeum KJ. Implications of red Panax ginseng in oxidative stress associated chronic diseases. J Ginseng Res. Apr 2017;41(2):113-119.
- Flanagan SD, DuPont WH, Caldwell LK, et al. The Effects of a Korean Ginseng, GINST15, on Hypo-Pituitary-Adrenal and Oxidative Activity Induced by Intense Work Stress. J Med Food. Jan 2018;21(1):104-112.
- Huang L, Zhao H, Huang B, Zheng C, Peng W, Qin L. Acanthopanax senticosus: review of botany, chemistry and pharmacology. Pharmazie. Feb 2011;66(2):83-97.
- Ishaque S, Shamseer L, Bukutu C, Vohra S. Rhodiola rosea for physical and mental fatigue: a systematic review. BMC Complement Altern Med. May 29 2012;12:70.
- Li Y, Pham V, Bui M, et al. Rhodiola rosea L.: an herb with anti-stress, anti-aging, and immunostimulating properties for cancer chemoprevention. Curr Pharmacol Rep. Dec 2017;3(6):384-395.
- Chiang HM, Chen HC, Wu CS, Wu PY, Wen KC. Rhodiola plants: Chemistry and biological activity. J Food Drug Anal. Sep 2015;23(3):359-369.
- Kasper S, Dienel A. Multicenter, open-label, exploratory clinical trial with Rhodiola rosea extract in patients suffering from burnout symptoms. Neuropsychiatr Dis Treat. 2017;13:889-898.
- Lekomtseva Y, Zhukova I, Wacker A. Rhodiola rosea in Subjects with Prolonged or Chronic Fatigue Symptoms: Results of an Open-Label Clinical Trial. Complement Med Res. 2017;24(1):46-52.
- Cropley M, Banks AP, Boyle J. The Effects of Rhodiola rosea L. Extract on Anxiety, Stress, Cognition and Other Mood Symptoms. Phytother Res. Dec 2015;29(12):1934-1939.
- Amsterdam JD, Panossian AG. Rhodiola rosea L. as a putative botanical antidepressant. Phytomedicine. Jun 15 2016;23(7):770-783.
- Concerto C, Infortuna C, Muscatello MRA, et al. Exploring the effect of adaptogenic Rhodiola Rosea extract on neuroplasticity in humans. Complement Ther Med. Dec 2018;41:141-146.
- Variya BC, Bakrania AK, Patel SS. Emblica officinalis (Amla): A review for its phytochemistry, ethnomedicinal uses and medicinal potentials with respect to molecular mechanisms. Pharmacol Res. Sep 2016;111:180-200.
- Tahir I, Khan MR, Shah NA, Aftab M. Evaluation of phytochemicals, antioxidant activity and amelioration of pulmonary fibrosis with Phyllanthus emblica leaves. BMC Complement Altern Med. Oct 24 2016;16(1):406.
- Fatima N, Pingali U, Pilli R. Evaluation of Phyllanthus emblica extract on cold pressor induced cardiovascular changes in healthy human subjects. Pharmacognosy Res. Jan 2014;6(1):29-35.
- Bhattacharya A, Ghosal S, Bhattacharya SK. Antioxidant activity of tannoid principles of Emblica officinalis (amla) in chronic stress induced changes in rat brain. Indian J Exp Biol. Sep 2000;38(9):877-880.
- Arun S, Burawat J, Yannasithinon S, Sukhorum W, Limpongsa A, Iamsaard S. Phyllanthus emblica leaf extract ameliorates testicular damage in rats with chronic stress. J Zhejiang Univ Sci B. Dec. 2018;19(12):948-959.
- Dwivedi V, Lakhotia SC. Ayurvedic Amalaki Rasayana promotes improved stress tolerance and thus has anti-aging effects in Drosophila melanogaster. J Biosci. Dec 2016;41(4):697-711.
- Szopa A, Ekiert R, Ekiert H. Current knowledge of Schisandra chinensis (Turcz.) Baill. (Chinese magnolia vine) as a medicinal plant species: a review on the bioactive components, pharmacological properties, analytical and biotechnological studies. Phytochem Rev. 2017;16(2):195-218.
- Zhang M, Xu L, Yang H. Schisandra chinensis Fructus and Its Active Ingredients as Promising Resources for the Treatment of Neurological Diseases. Int J Mol Sci. Jul 6 2018;19(7).
- Sowndhararajan K, Deepa P, Kim M, Park SJ, Kim S. An overview of neuroprotective and cognitive enhancement properties of lignans from Schisandra chinensis. Biomed Pharmacother. Jan 2018;97:958-968.
- Chen WW, He RR, Li YF, Li SB, Tsoi B, Kurihara H. Pharmacological studies on the anxiolytic effect of standardized Schisandra lignans extract on restraint-stressed mice. Phytomedicine. Oct 15 2011;18(13):1144-1147.
- Xia N, Li J, Wang H, Wang J, Wang Y. Schisandra chinensis and Rhodiola rosea exert an anti-stress effect on the HPA axis and reduce hypothalamic c-Fos expression in rats subjected to repeated stress. Exp Ther Med. Jan 2016;11(1):353-359.
- Yan T, Xu M, Wan S, et al. Schisandra chinensis produces the antidepressant-like effects in repeated corticosterone-induced mice via the BDNF/TrkB/CREB signaling pathway. Psychiatry Res. Sep 30 2016;243:135-142.
- Zhou X, Gong Z, Su Y, Lin J, Tang K. Cordyceps fungi: natural products, pharmacological functions and developmental products. J Pharm Pharmacol. Mar 2009;61(3):279-291.
- Olatunji OJ, Tang J, Tola A, Auberon F, Oluwaniyi O, Ouyang Z. The genus Cordyceps: An extensive review of its traditional uses, phytochemistry and pharmacology. Fitoterapia. Sep 2018;129:293-316.
- Liu Y, Wang J, Wang W, Zhang H, Zhang X, Han C. The Chemical Constituents and Pharmacological Actions of Cordyceps sinensis. Evid Based Complement Alternat Med. 2015;2015:575063.
- Tianzhu Z, Shihai Y, Juan D. Antidepressant-like effects of cordycepin in a mice model of chronic unpredictable mild stress. Evid Based Complement Alternat Med. 2014;2014:438506.
- Rossi P, Buonocore D, Altobelli E, et al. Improving Training Condition Assessment in Endurance Cyclists: Effects of Ganoderma lucidum and Ophiocordyceps sinensis Dietary Supplementation. Evid Based Complement Alternat Med. 2014;2014:979613.
- Javidi H, Yadollahie M. Post-traumatic Stress Disorder. Int J Occup Environ Med. 2012;3(1):2-9.
- Strada EA. Psychosocial Issues and Bereavement. Primary care. 2019;46(3):373-386.
- Cohen GJ, Weitzman CC. Helping Children and Families Deal With Divorce and Separation. Pediatrics. 2016;138(6).
- Linden M, Rotter M. Unemployment and embitterment in contrast to general psychological distress. Work. 2019;62(1):133-138.
- King J, O'Neill B, Ramsay P, et al. Identifying patients' support needs following critical illness: a scoping review of the qualitative literature. Crit Care. 2019;23(1):187.
- Cohen S, Janicki-Deverts D, Turner RB, Doyle WJ. Does hugging provide stress-buffering social support? A study of susceptibility to upper respiratory infection and illness. Psychol Sci. 2015;26(2):135-147.
- Cohen S, Tyrrell DA, Smith AP. Psychological stress and susceptibility to the common cold. The New England journal of medicine. 1991;325(9):606-612.
- Takkouche B, Regueira C, Gestal-Otero JJ. A cohort study of stress and the common cold. Epidemiology (Cambridge, Mass). 2001;12(3):345-349.
- Cohen S. Keynote Presentation at the Eight International Congress of Behavioral Medicine: the Pittsburgh common cold studies: psychosocial predictors of susceptibility to respiratory infectious illness. International journal of behavioral medicine. 2005;12(3):123-131.
- Cohen S, Janicki-Deverts D, Doyle WJ, et al. Chronic stress, glucocorticoid receptor resistance, inflammation, and disease risk. Proc Natl Acad Sci U S A. 2012;109(16):5995-5999.
- Cohen S, Doyle WJ, Skoner DP. Psychological stress, cytokine production, and severity of upper respiratory illness. Psychosomatic medicine. 1999;61(2):175-180.
- Janicki-Deverts D, Cohen S, Turner RB, Doyle WJ. Basal salivary cortisol secretion and susceptibility to upper respiratory infection. Brain Behav Immun. 2016;53:255-261.
- Gaffey AE, Bergeman CS, Clark LA, Wirth MM. Aging and the HPA axis: Stress and resilience in older adults. Neuroscience and biobehavioral reviews. 2016;68:928-945.
- Dantzer R, Cohen S, Russo SJ, Dinan TG. Resilience and immunity. Brain Behav Immun. 2018;74:28-42.
- Ditzen B, Heinrichs M. Psychobiology of social support: the social dimension of stress buffering. Restor Neurol Neurosci. 2014;32(1):149-162.
- Luthar SS, Kumar NL, Benoit R. Toward fostering resilience on a large scale: Connecting communities of caregivers. Dev Psychopathol. 2019;31(5):1813-1825.
- Ruisoto P, Contador I, Fernandez-Calvo B, et al. Mediating effect of social support on the relationship between resilience and burden in caregivers of people with dementia. Arch Gerontol Geriatr. 2020;86:103952.
- Lee JS. Perceived social support functions as a resilience in buffering the impact of trauma exposure on PTSD symptoms via intrusive rumination and entrapment in firefighters. PLoS One. 2019;14(8):e0220454.
- Motreff Y, Baubet T, Pirard P, et al. Factors associated with PTSD and partial PTSD among first responders following the Paris terror attacks in November 2015. Journal of psychiatric research. 2020;121:143-150.
- Zhang J, Guo F, Chen ZY, He HW, Long Y, Li Q. [Relationship between social support, resilience, self-esteem and post-traumatic stress disorder in intensive care unit nurses]. Zhonghua yi xue za zhi. 2020;100(1):32-36.
- Blake L, Bray L, Carter B. "It's a lifeline": Generating a sense of social connectedness through befriending parents of disabled children or children with additional need. Patient Educ Couns. 2019;102(12):2279-2285.
- Park SK, Seong RK, Kim JA, et al. Oligonol promotes anti-aging pathways via modulation of SIRT1-AMPK-Autophagy Pathway. Nutrition research and practice. 2016;10(1):3-10.
- Lee JB, Shin YO, Min YK, Yang HM. The effect of Oligonol intake on cortisol and related cytokines in healthy young men. Nutrition research and practice. 2010;4(3):203-207.
- Shin Y-O, Lee J-B, Min Y-K, Yang H-M. Effect of oligonol intake on cortisol and cytokines, and body temperature after leg immersion into hot water. Food Science and Biotechnology. 2011;20(3):659-663.
- Kaszkin-Bettag M, Ventskovskiy BM, Kravchenko A, et al. The special extract ERr 731 of the roots of Rheum rhaponticum decreases anxiety and improves health state and general well-being in perimenopausal women. Menopause (New York, NY). 2007;14(2):270-283.
- Heger M, Ventskovskiy BM, Borzenko I, et al. Efficacy and safety of a special extract of Rheum rhaponticum (ERr 731) in perimenopausal women with climacteric complaints: a 12-week randomized, double-blind, placebo-controlled trial. Menopause (New York, NY). 2006;13(5):744-759.
- Kimura K, Ozeki M, Juneja LR, Ohira H. L-Theanine reduces psychological and physiological stress responses. Biol Psychol. 2007;74(1):39-45.
- Kocaadam B, Sanlier N. Curcumin, an active component of turmeric (Curcuma longa), and its effects on health. Crit Rev Food Sci Nutr. 2017;57(13):2889-2895.
- Naqvi F, Saleem S, Naqvi F, et al. Curcumin lessens unpredictable chronic mild stress-induced depression and memory deficits by modulating oxidative stress and cholinergic activity. Pakistan journal of pharmaceutical sciences. 2019;32(4(Supplementary)):1893-1900.
- Aubry AV, Khandaker H, Ravenelle R, et al. A diet enriched with curcumin promotes resilience to chronic social defeat stress. Neuropsychopharmacology. 2019;44(4):733-742.
- Lee B, Lee H. Systemic Administration of Curcumin Affect Anxiety-Related Behaviors in a Rat Model of Posttraumatic Stress Disorder via Activation of Serotonergic Systems. Evidence-based complementary and alternative medicine : eCAM. 2018;2018:9041309.
- Shen JD, Wei Y, Li YJ, Qiao JY, Li YC. Curcumin reverses the depressive-like behavior and insulin resistance induced by chronic mild stress. Metabolic brain disease. 2017;32(4):1163-1172.
- Haider S, Naqvi F, Batool Z, et al. Pretreatment with curcumin attenuates anxiety while strengthens memory performance after one short stress experience in male rats. Brain research bulletin. 2015;115:1-8.
- Fan C, Song Q, Wang P, et al. Curcumin Protects Against Chronic Stress-induced Dysregulation of Neuroplasticity and Depression-like Behaviors via Suppressing IL-1beta Pathway in Rats. Neuroscience. 2018;392:92-106.
- Choi GY, Kim HB, Hwang ES, et al. Curcumin Alters Neural Plasticity and Viability of Intact Hippocampal Circuits and Attenuates Behavioral Despair and COX-2 Expression in Chronically Stressed Rats. Mediators Inflamm. 2017;2017:6280925.
- Liu D, Wang Z, Gao Z, et al. Effects of curcumin on learning and memory deficits, BDNF, and ERK protein expression in rats exposed to chronic unpredictable stress. Behavioural brain research. 2014;271:116-121.
- Fusar-Poli L, Vozza L, Gabbiadini A, et al. Curcumin for depression: a meta-analysis. Crit Rev Food Sci Nutr. 2019:1-11.
- Ng QX, Koh SSH, Chan HW, Ho CYX. Clinical Use of Curcumin in Depression: A Meta-Analysis. Journal of the American Medical Directors Association. 2017;18(6):503-508.
- Al-Karawi D, Al Mamoori DA, Tayyar Y. The Role of Curcumin Administration in Patients with Major Depressive Disorder: Mini Meta-Analysis of Clinical Trials. Phytother Res. 2016;30(2):175-183.
- Pandaran Sudheeran S, Jacob D, Natinga Mulakal J, et al. Safety, Tolerance, and Enhanced Efficacy of a Bioavailable Formulation of Curcumin With Fenugreek Dietary Fiber on Occupational Stress: A Randomized, Double-Blind, Placebo-Controlled Pilot Study. Journal of clinical psychopharmacology. 2016;36(3):236-243.
- Asadi S, Gholami MS, Siassi F, Qorbani M, Sotoudeh G. Beneficial effects of nano-curcumin supplement on depression and anxiety in diabetic patients with peripheral neuropathy: A randomized, double-blind, placebo-controlled clinical trial. Phytother Res. 2020;34(4):896-903.
- Kanchanatawan B, Tangwongchai S, Sughondhabhirom A, et al. Add-on Treatment with Curcumin Has Antidepressive Effects in Thai Patients with Major Depression: Results of a Randomized Double-Blind Placebo-Controlled Study. Neurotoxicity research. 2018;33(3):621-633.
- Sciberras JN, Galloway SD, Fenech A, et al. The effect of turmeric (Curcumin) supplementation on cytokine and inflammatory marker responses following 2 hours of endurance cycling. Journal of the International Society of Sports Nutrition. 2015;12(1):5.
- Pickering G, Mazur A, Trousselard M, et al. Magnesium Status and Stress: The Vicious Circle Concept Revisited. Nutrients. Nov 28 2020;12(12)doi:10.3390/nu12123672. https://www.ncbi.nlm.nih.gov/pubmed/33260549
- Noah L, Pickering G, Mazur A, et al. Impact of magnesium supplementation, in combination with vitamin B6, on stress and magnesium status: secondary data from a randomized controlled trial. Magnes Res. Aug 1 2020;33(3):45-57. doi:10.1684/mrh.2020.0468. https://www.ncbi.nlm.nih.gov/pubmed/33210604
- Boyle NB, Lawton C, Dye L. The Effects of Magnesium Supplementation on Subjective Anxiety and Stress-A Systematic Review. Nutrients. 2017;9(5):429. doi:10.3390/nu9050429. https://pubmed.ncbi.nlm.nih.gov/28445426
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5452159/ - Ates M, Kizildag S, Yuksel O, et al. Dose-Dependent Absorption Profile of Different Magnesium Compounds. Biol Trace Elem Res. Dec 2019;192(2):244-251. doi:10.1007/s12011-019-01663-0. https://www.ncbi.nlm.nih.gov/pubmed/30761462
- Rousseau C. Efficiency of a magnesium salt (ATA MG® 770mg) on premenopausal syndrome: a clinical study report. Synapharm (Company supplied data). 2021;
- Raine A, Brodrick L. Omega-3 supplementation reduces aggressive behavior: A meta-analytic review of randomized controlled trials. Aggression and Violent Behavior. 2024;78:101956. doi:https://doi.org/10.1016/j.avb.2024.101956. https://pubmed.ncbi.nlm.nih.gov/38911617/
- Evans M, McDonald AC, Xiong L, Crowley DC, Guthrie N. A Randomized, Triple-Blind, Placebo-Controlled, Crossover Study to Investigate the Efficacy of a Single Dose of AlphaWave((R)) L-Theanine on Stress in a Healthy Adult Population. Neurol Ther. Dec 2021;10(2):1061-1078. doi:10.1007/s40120-021-00284-x. https://www.ncbi.nlm.nih.gov/pubmed/34562208
- Moulin M, Crowley DC, Xiong L, Guthrie N, Lewis ED. Safety and Efficacy of AlphaWave((R)) L-Theanine Supplementation for 28 Days in Healthy Adults with Moderate Stress: A Randomized, Double-Blind, Placebo-Controlled Trial. Neurol Ther. Aug 2024;13(4):1135-1153. doi:10.1007/s40120-024-00624-7. https://www.ncbi.nlm.nih.gov/pubmed/38758503
- Hidese S, Ogawa S, Ota M, et al. Effects of L-Theanine Administration on Stress-Related Symptoms and Cognitive Functions in Healthy Adults: A Randomized Controlled Trial. Nutrients. Oct 3 2019;11(10)doi:10.3390/nu11102362. https://www.ncbi.nlm.nih.gov/pubmed/31623400
