Life Extension Magazine®
When it comes to heart failure, the statistics are chilling.
More than 870,000 new cases are diagnosed in the U.S. each year in people aged 55 and older.1-4
One in five people who are currently 40 years old will go on to develop heart failure in their lifetimes. By 2030 it is expected that more than eight million Americans will be affected by the disease.1-3
Heart failure occurs when the heart fails to pump enough blood to support the whole body.1 It is a debilitating and progressive condition.
Clinical trials have shown that supplementation with D-ribose, which is produced in the body, can improve heart function following damage to the heart muscle.
It helps the heart muscle manage energy, offering a potential solution to the slow-motion cardiac energy crisis that is heart failure.5-7
But how does D-ribose achieve these results?
The answer has to do with the way energy is released and converted into adenosine triphosphate (ATP). This universal “energy currency” then transfers energy to cells in a form they can use to do their cellular work.
Here, we review the compelling clinical studies that reveal the power of D-ribose in heart failure, and then explain precisely how it works to feed the energy-hungry, failing heart.
What you need to know
- Heart failure means the heart muscle is failing to pump enough blood to meet the body’s metabolic requirements.
- Its incidence is rising, but there are no good, long-term medications available that truly treat heart failure and reverse its debilitating effects.
- The field of metabolic cardiology suggests that fundamental energy requirements go unmet in muscle cells of a failing heart, leading to significant drops in ATP, the energy-carrying molecule that supports all cellular work.
- One source of low ATP in heart failure is a diminished supply of the sugar D-ribose, which ailing heart cells cannot manufacture fast enough to meet energy requirements.
- Studies now show that supplemental D-ribose, 5 grams three times daily, can significantly improve heart muscle function in heart failure, resulting in better pumping action and reduced workload on heart and lungs.
D-Ribose Improves Heart Function
D-ribose is a building block of ATP,8 the energy source for every cell. Research has demonstrated that D-ribose supplementation can support the heart’s ability to extract energy and store it in the form of ATP, improving the function of the heart even if it’s been damaged.7
Human studies show the following potential of D-ribose to reduce the symptoms of heart failure when given orally at a dose of 5 grams three times daily:
-
Improved blood flow through the heart.
Heart failure results in slower flow of blood through the heart, raising the amount of
work the heart muscle must do to push the
blood through the body. Fifteen patients with chronic coronary artery
disease and heart failure were randomly assigned to receive D-ribose or a
placebo for three weeks,
and after a one-week “washout” period, were switched to the opposite
therapy.7 During the D-ribose supplement phases subjects had
significantly enhanced filling of the left ventricle and other signs of reduced cardiac loading that eased the workload on the ailing heart muscle, and significantly improved measures of quality of life. No such changes were seen during placebo phases. - Improved blood flow in the body. Heart failure reduces the amount of blood the heart can pump with each beat, slowing down the body’s whole circulation, imperiling organs that need ample blood supply. Eleven patients with New York Heart Association Class II-IV (mild to severe) heart failure were supplemented with D-ribose for six weeks.5 At the end of the six-week supplementation period, improved blood flow in tissues was shown by Doppler ultrasound in 64% of patients. This improvement lasted through nine weeks—three weeks after the end of supplementation.
- Improved exchange of oxygen and CO2 through the lungs.
Heart failure increases how hard the heart-lung system must work
to rid the body of carbon dioxide and take in oxygen. Sixteen people with
New York Heart Association Class III-IV heart failure (among the most
severe) were treated in a trial of D-ribose for eight weeks.6
All patients had
a significant improvement in their breathing parameters, which are so often
impaired
in heart failure.
D-ribose supplementation significantly increased ventilatory efficiency (how much air needs to be moved to eliminate metabolically- produced carbon dioxide from the body) by 16%. Ventilatory efficiency is a strong predictor of survival in heart failure patients, so this demonstrates a direct reduction in the risk of dying.6 Measures of oxygen uptake efficiency, oxygen flow through the lungs, and amount of oxygen pumped per heartbeat also improved, by 25%, 19%, and 16%, respectively, demonstrating marked increases in the ability of the heart-lung system to take up oxygen and rid the body of carbon dioxide.
Together, these and other studies show the value of adding a D-ribose supplement, 5 grams three times daily, to improve heart failure symptoms and quality of life in heart failure patients.
A deeper look into what happens in the muscles of a failing heart has opened an entirely new chapter in metabolic cardiology, the study of how the heart’s own energy flow affects its pumping capacity.9,10
What is heart failure, anyway?
 |
“Heart failure,” despite its dramatic-sounding name, is not a sudden, fatal event.
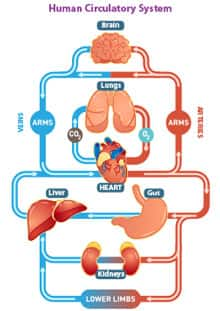
The term refers to a situation in which the heart muscle cannot keep up with the body’s demands for ample blood flow. In other words, the heart “fails” to provide adequate supplies of blood. As a result, a host of organs and systems run on insufficient fuel, leading to gradual, systems-wide malfunctions.
Heart failure doesn’t appear out of nowhere. Generally, either the heart muscle is damaged (by a heart attack, for example), or the workload faced by the heart muscle rises sharply (as with severe high blood pressure).15
Regardless of the cause, heart failure typically results in an overstretched, thickened, and enlarged left ventricle (the main pumping chamber), which overburdens the heart’s ability to work efficiently.9,16
The outcome is that there is a reduction in the volume and pressure the ailing heart muscle can pump with each contraction. That causes both an insufficient forward flow, and a backup of blood that can’t get back to the heart for recirculation.
These factors produce the common symptoms of heart failure, which worsen as the condition becomes more severe.17,18
In early heart failure, patients may experience no symptoms at all. As heart failure progresses, people may be comfortable at rest, but find that ordinary physical activity produces fatigue, heart palpitations, trouble breathing, or chest pain.
In later stages, symptoms markedly limit physical activity. In the most severe stage (Stage D, in the American Heart Association’s classification), people with advanced heart failure may have symptoms at rest and are unable to carry out any physical activity without discomfort or a sharp increase in symptoms. These patients require aggressive medical therapy just to survive.
D-Ribose Supports Cardiac Energy Metabolism

After a hard workout or physical labor, our muscles are tired and weak. That’s because, at the cellular level, they’ve used up much of the available molecules of ATP that provide the energy for the cellular work of moving. We rest after exercise or hard work in order to give our muscles time to burn more glucose to make more ATP.
The same situation occurs in the heart, with one vital difference: The heart muscle can’t stop to rest and re-energize itself with more ATP. When ATP levels fall, the heart muscle simply operates with increasing weakness, pumping less blood with each beat.
If we can figure out a way to boost ATP levels, we can re-energize the heart muscle and may prevent or even reverse the symptoms of heart failure.
To understand how D-ribose benefits the heart, we need to look at the makeup of ATP itself.
The ATP molecule consists of three major parts, as seen in Figure 1 on the next page.
Adenine is a nucleotide, one of the building blocks of DNA.
Adenosine is simply adenine chemically bonded to a molecule of D-ribose.8 D-ribose is a structural component of the vital ATP molecule.9
The D-ribose portion of adenosine binds tightly to a series of phosphate molecules, with each chemical bond between the phosphate groups containing energy extracted from the metabolism of glucose and fat. ATP, with three such bonds, contains more stored energy than adenosine monophosphate (AMP), which has just one.
A maximum of three high-energy phosphate groups can be bound to a single adenosine molecule, producing adenosine triphosphate, or ATP. When cells require energy, they release phosphates from ATP to carry out useful work by harvesting the newly-released energy.8,11
But in heart failure, a cellular energy deficiency arises in which D-ribose production falls in heart muscle cells.12 This leads directly to a decrease in ATP production in the very cells that need energy the most. Without ample D-ribose, cells cannot capture metabolic energy, and almost literally starve themselves into weakness.8
The obvious solution, then, is to provide extra D-ribose in the form of an oral supplement, which bypasses the overwhelmed cellular D-ribose-producing machinery and permits creation of many new ATP molecules.8
And it works. One of the first studies of supplemental D-ribose was done in dogs back in 1989. It showed that ATP levels are depressed by about 50% following loss of blood flow (ischemia) in the heart muscle. But when the dogs were supplemented with D-ribose intravenously, during and after the ischemic event, ATP levels rebounded to 85% of their normal levels within 24 hours, a benefit not seen in the unsupplemented animals.13
In other words, D-ribose replenishes low cardiac muscle energy levels, improving cardiac function during ischemia.6
The evidence for D-ribose as a heart muscle energizer is so great that scientists have proposed treating it as a conditionally essential nutrient. This means that, under certain conditions, like heart failure, D-ribose is so important that its levels must be supported by external supplementation.14
new study to evaluate D-Ribose, CoQ10 Combination in Heart Failure
 |
Metabolic cardiology focuses on preventing and treating cardiovascular disease at the cellular level, by preserving and promoting the production of ATP. It holds the promise of reducing death and disability from heart failure.
The approach described in this article, providing supplemental D-ribose to boost available ATP in heart muscle, is one of the most important contributions of metabolic cardiology to date. But it is not the only one.
In a planned study by researchers at the University of Kansas School of Nursing and Department of Molecular and Integrative Physiology, subjects with heart failure will be randomly assigned to receive either a placebo, D-ribose (15 grams/daily), a form of coenzyme Q10 (CoQ10) called ubiquinol (600 mg/day), or a combination of both D-ribose and ubiquinol.3
The study will continue for 12 weeks, and will measure multiple outcomes, including symptoms, vigor, echocardiographic measurements of heart chamber sizes and function, and walking endurance. Measures of ATP production in mitochondria will also be taken.
This is just one example of a marked shift in researchers’ attitudes and approaches to heart
failure. Instead of drugs that “whip” the heart muscle to do more work with less energy, supporting
cardiac energy levels with D-ribose and CoQ10 offers the chance to genuinely improve heart muscle
function.
Summary
Heart failure is increasing, with an estimated eight million sufferers expected by 2030.
Currently, drugs for heart failure are only marginally effective and act by forcing the heart muscle to work harder, even as it is being deprived of sufficient ATP to perform extra work.
An alternative approach, called metabolic cardiology, offers a more natural and physiologically sound way to improve heart muscle performance. Researchers have found that we can improve the conditions that lead to ATP production within the heart muscle itself by providing D-ribose as a vital “substrate” for ATP production.
Studies in animals, and now in humans, have shown that increasing available D-ribose, the “scaffold” on which ATP is built, can dramatically restore energy to the heart, enabling it to carry out its vital work with greater power and efficiency.
Regular supplementation with D-ribose is one proven means of feeding the starving heart muscle and producing real improvements in cardiovascular function.
If you have any questions on the scientific content of this article, please call a Life Extension® Wellness Specialist at 1-866-864-3027.
Heart Failure Protocol
 |
Decades ago Life Extension® identified studies in Japan showing heart failure patients improving in response to 3,000 mg a day of the amino acid taurine.19
Japanese research on CoQ10 led a pioneering American cardiologist, Peter Langsjoen, MD, to develop a protocol for heart failure patients that involved high-dose ubiquinol (580 mg on average and after a few months reduce the ubiquinol dose to about 400 mg daily).20
Dr. Langsjoen’s dosing of ubiquinol is based on each patient’s blood levels of CoQ10. Life Extension offers CoQ10 blood testing to help those who need to achieve higher blood concentrations. To inquire about CoQ10 blood testing, call 1-800-208-3444 (24 hours) or visit www.lifeextension.com/blood
For healthy people not supplementing with CoQ10, Dr. Langsjoen suggests starting with 300-400 mg per day for the first month to fully saturate your cells. People can then back down to a daily dose of 100-200 mg per day to maintain high cellular CoQ10 levels.21,22
A recent animal model study indicates that heart failure patients might benefit by boosting the NAD+ levels.23 This can be accomplished by taking 250-500 mg a day of nicotinamide riboside. NAD+ is required for healthy cell energy functions.
There are also indicators that heart failure patients might benefit from taking senolytic compounds that selectively remove senescent cells. The accumulation of senescent cells damages healthier heart cells by spewing protein-degrading enzymes and igniting persistent inflammatory reactions.
So an updated heart failure protocol might include:
- 5,000 mg of D-ribose powder 3 times daily (15,000 mg total per day)
- 3,000 mg a day of taurine (a low-cost supplement)
- 200-600 mg of ubiquinol (dose can be based on blood test results)
- 250-500 mg a day of nicotinamide riboside
- 500 mg a day of magnesium
- 1,000 mg a day of carnosine
- Senolytic protocol of your choice
These approaches are NOT meant to substitute for conventional prescription drugs that are extending lives of heart failure patients. Their efficacy is evidenced by a 44% decline in sudden death rates of heart failure patients that occurred between 1995-2014 with more intelligent use of these drugs by conventional cardiology.24 This period is also associated with surging use of CoQ10 that heart failure patients often take.
The next page features some Power Point slides that were used to describe recent findings on the potential of NAD+ and senolytics to improve heart muscle function, along with a listing of prescription drugs often prescribed for heart failure patients.
Note: Take CoQ10 with a fatty meal to further improve absorption.
Recent Findings on NAD+ and Senolytics Relating to heart failure
Heart Failure Fact Sheet
- Heart failure happens when the heart cannot pump enough blood and oxygen to support other organs in your body.
- About half of people who develop heart failure die within 5 years of diagnosis.
- 8 million Americans suffer heart failure.
CDC January 8, 2019 https://www.cdc.gov/dhdsp/data_statistics/fact_sheets/fs_heart_failure.htm
Newcastle University Scientists are Killing Zombie Cells to Reverse Age-Related Damage in the Heart
“... senescent cells – also known as zombie cells – form in the heart during aging and lead to heart failure.”
”Newcastle scientists, in collaboration with researchers in the Mayo Clinic... have not only discovered how this process takes place in the heart, but also how it can be reversed or treated.”
British Heart Foundation February 8, 2019
NAD+ May Improve Heart Function
“Stabilizing the intracellular NAD+ level represents a promising therapeutic strategy to improve myocardial bioenergetics and cardiac function.”
“In this issue of Circulation, Diguet et al report exciting data suggesting that supplementation with a NAD+ precursor, nicotinamide riboside, reduces cardiac dysfunction in preclinical models of heart failure.”
American Heart Association® May 21, 2018
Sharp Decline in Heart Failure Death Rates
- Clinical trials spanning 1995 to 2014 show:
- 44% decline of sudden death rates in heart failure patients.
- Marked improvement in just 19 years!
The New England Journal of Medicine “Declining Risk of Sudden Death in Heart Failure.” New England Journal of Medicine; 2017;377(1):41-51.
Proper Medication Use Buys Heart Failure Patients Extra Years
Combinations of the following drugs treat heart failure under cardiologist supervision:
- Beta Blockers (carvedilol, metoprolol)
- ACE Inhibitors (lisinopril, captopril)
- Angiotensin Receptor Blockers (losartan)
- Digoxin (Lanoxin)
- Hydralazine and Nitrates (Apresoline, Nitrobid, Imdur, Isordil)
Without innovative approaches, heart failure eventually results in death.
Senolytics to Treat Heart Failure Need Human Validation
What we learned from this 2019 published study:
- Senescence involving cardiomyocytes (i.e. cardiac muscle cells) appears to be associated with age-linked fibrosis and hypertrophy of the heart.
- Pharmacologic and genetic removal of p16-positive (senescent) cells in mice appears to ameliorate (or improve) the level of age-induced fibrosis and hypertrophy in senescent cardiac muscle cells, and may support regeneration of cardiomyocyte.
Clinical trial on existing senolytic compounds urgently needed!
EMBO J. 2019 Mar 1;38(5). pii: e100492.
What Are Senolytics?
- “Seno” refers to senescent cells
- “Lytic” refers to destruction
Senolytics selectively destroy senescent cells.
“Scientists believe it may be possible to reverse the heart damage caused by aging”
“We saw that removing senescent cardiomyocytes from the hearts of aged mice, both genetically and using drugs, was able to restore cardiac health – essentially removing the damage caused by aging.
These data provide critical support for the potential of using medicines to kill zombie cells. If this is validated through clinical trials it would provide us with a new way of treating cardiac diseases.”
Medical Press February 11, 2019 Rhys Anderson et al. Length‐independent telomere damage drives post‐mitotic cardiomyocyte senescence, The EMBO Journal (2019). DOI: 10.15252/embj.2018100492t
References
- Travessa AM, de Menezes Falcao LF. Treatment of Heart Failure With Reduced Ejection Fraction-Recent Developments. Am J Ther. 2016 Mar-Apr;23(2):e531-49.
- Writing Group M, Mozaffarian D, Benjamin EJ, et al. Heart Disease and Stroke Statistics-2016 Update: A Report From the American Heart Association. Circulation. 2016 Jan 26;133(4): e38-360.
- Pierce JD, Mahoney DE, Hiebert JB, et al. Study protocol, randomized controlled trial: reducing symptom burden in patients with heart failure with preserved ejection fraction using ubiquinol and/or D-ribose. BMC Cardiovasc Disord. 2018 Apr 2;18(1):57.
- Farmakis D, Stafylas P, Giamouzis G, et al. The medical and socioeconomic burden of heart failure: A comparative delineation with cancer. Int J Cardiol. 2016 Jan 15;203:279-81.
- Bayram M, St Cyr JA, Abraham WT. D-ribose aids heart failure patients with preserved ejection fraction and diastolic dysfunction: a pilot study. Ther Adv Cardiovasc Dis. 2015 Jun;9(3):56-65.
- MacCarter D, Vijay N, Washam M, et al. D-ribose aids advanced ischemic heart failure patients. Int J Cardiol. 2009 Sep 11;137(1):79-80.
- Omran H, Illien S, MacCarter D, et al. D-Ribose improves diastolic function and quality of life in congestive heart failure patients: a prospective feasibility study. Eur J Heart Fail. 2003 Oct;5(5):615-9.
- Pauly DF, Pepine CJ. D-Ribose as a supplement for cardiac energy metabolism. J Cardiovasc Pharmacol Ther. 2000 Oct;5(4):249-58.
- Sinatra ST. Metabolic cardiology: an integrative strategy in the treatment of congestive heart failure. Altern Ther Health Med. 2009 May-Jun;15(3):44-52.
- Sinatra ST. Metabolic cardiology: the missing link in cardiovascular disease. Altern Ther Health Med. 2009 Mar-Apr;15(2):48-50.
- Klingenberg M. The ADP and ATP transport in mitochondria and its carrier. Biochim Biophys Acta. 2008 Oct;1778(10):1978-2021.
- Mahoney DE, Hiebert JB, Thimmesch A, et al. Understanding D-Ribose and Mitochondrial Function. Adv Biosci Clin Med. 2018;6(1):1-5.
- St Cyr JA, Bianco RW, Schneider JR, et al. Enhanced high energy phosphate recovery with ribose infusion after global myocardial ischemia in a canine model. J Surg Res. 1989 Feb;46(2):157-62.
- Kendler BS. Supplemental conditionally essential nutrients in cardiovascular disease therapy. J Cardiovasc Nurs. 2006 Jan-Feb;21(1):9-16.
- Available at: https://www.mayoclinic.org/diseases-conditions/heart-failure/symptoms-causes/syc-20373142. Accessed March 15, 2019.
- Available at: https://www.mayoclinic.org/diseases-conditions/left-ventricular-hypertrophy/symptoms-causes/syc-20374314. Accessed March 15, 2019.
- Available at: https://www.heart.org/en/health-topics/heart-failure/what-is-heart-failure/classes-of-heart-failure. Accessed 28 December, 2018.
- Writing Committee M, Yancy CW, Jessup M, et al. 2013 ACCF/AHA guideline for the management of heart failure: a report of the American College of Cardiology Foundation/American Heart Association Task Force on practice guidelines. Circulation. 2013 Oct 15;128(16):e240-327
- Available at: https://www.lifeextension.com/magazine/1998/10/medup/page-01. Accessed April 3, 2019.
- Langsjoen PH, Langsjoen AM. Supplemental ubiquinol in patients with advanced congestive heart failure. Biofactors. 2008;32(1-4):119-28.
- Available at: https://www.lifeextension.com/magazine/2015/4/coq10-wars/page-01. Accessed April 4, 2019.
- Available at: https://www.lifeextension.com/magazine/page-01. Accessed April 4, 2019.
- Diguet N, Trammell SAJ, Tannous C, et al. Nicotinamide Riboside Preserves Cardiac Function in a Mouse Model of Dilated Cardiomyopathy. Circulation. 2018 May 22;137(21):2256-73.
- Shen L, Jhund PS, Petrie MC, et al. Declining Risk of Sudden Death in Heart Failure. N Engl J Med. 2017;377(1):41-51.

