Life Extension Magazine®
Although standard blood cholesterol tests (measuring total cholesterol, LDL, HDL, and triglycerides) have helped doctors to accurately assess heart disease risk in many patients, recent advances in medical science have demonstrated that conventional cholesterol testing provides only limited insight into the multiple factors that underlie cardiovascular disease. In fact, these tests identify only 40% of those at risk for coronary heart disease. The good news is, scientists have developed a more advanced blood test that can far more accurately gauge your risk of heart disease. The Vertical Auto Profile (VAP) test augments the standard cholesterol profile with additional measurements that can identify the risk of cardiovascular disease. Best of all, the VAP test not only offers a comprehensive assessment of cardiovascular risk, but also supplies vital information that can help you and your doctor formulate a customized disease-prevention program and measure its progress over time. This powerful diagnostic tool can help you take the steps necessary to avoid preventable health catastrophes—like heart attack and stroke—today. The baby-boom generation understands that as they age, their risk for heart attacks, strokes, and other cardiovascular events continues to increase.1 Not content to succumb to disease and disability, this population is embracing a proactive, preventive approach to health care that includes advanced techniques of risk assessment such as the Vertical Auto Profile (VAP) cholesterol test. Awareness of the VAP test is important for anyone who wants to stop cardiovascular disease in its tracks, even before signs and symptoms manifest. The VAP test is performed just like a traditional cholesterol panel: a technician or nurse draws blood and submits it to a laboratory. At reasonable cost, the VAP test provides more information than routine cholesterol tests and expands on this data. The comprehensive information derived from the VAP test enables physicians to more accurately predict their patients’ risk of heart disease, and to customize more aggressive, patient-specific treatment plans. Even if your doctor’s office does not yet regularly utilize the VAP test, it is very likely that your physician will recognize the value of this advanced cholesterol screening tool, and will use the more detailed information it provides to devise the best treatment program to reduce your cardiovascular risk.
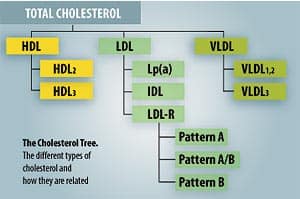
How the VAP Test WorksRoutine cholesterol tests provide only the four following measurements:
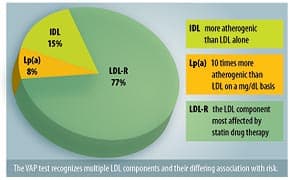
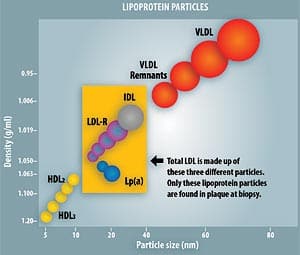
The standard lipid panel above is what physicians have relied on for years to assess their patients’ risk of cardiovascular disease. It has been a successful tool, helping physicians to lower patient cholesterol levels using a variety of medical therapies, including statin drugs, and motivating people to make lifesaving changes in their diet and lifestyle. However, there are serious limitations to relying solely on the standard cholesterol panel. Most important, it can identify only about 40% of patients at risk for coronary heart disease.2 The truth is, many risk factors are involved in the development of heart disease, and for some people, high cholesterol may or may not be one of them. The well-known Framingham Study illustrated that the higher the cholesterol, the higher the statistical risk of a heart attack.3 Nonetheless, a frightening number of heart attacks still occur every day in people whose cholesterol values are seemingly normal. In fact, the American Heart Association reports that 50% of men and 64% of women who died suddenly of coronary heart disease had no previous symptoms!1 Heart disease can lurk silently within, hidden and unsuspected. However, the additional information provided by the VAP test can help identify at-risk patients more accurately than routine cholesterol tests.2 The expanded information from the VAP test includes:
Patients who test “normal” in a routine cholesterol panel often are found to be at risk for heart disease after taking the VAP test. This is crucially important, not only to diagnose a number of lipid disorders and optimize the choice of medications, but also for tracking improvement when patients are working to reduce their numbers, whether with drugs or lifestyle changes. Clearly, more information means more effective treatment, and thus better health outcomes. In addition, VAP is the only cholesterol profile that tests for all the present and emerging risk factors identified in the National Cholesterol Education Program Adult Treatment Panel III (NCEP ATP III) cholesterol guidelines.5
Prevention Is Key to Cardiovascular HealthI have performed a VAP test for the first time on many patients who have already had heart attacks or strokes, or who have undergone heart procedures such as bypass surgery or placement of a coronary stent. The results have often led me to think that if a VAP test had been performed earlier, maybe the heart attack or stroke could have been prevented, or the surgery would not have been necessary. Too often in the United States, medical care is reactionary. A heart attack or stroke occurs, the sufferer rushes to the emergency room, and then doctors desperately try to rise to the rescue. All the physicians and patients I know appreciate that this is not the best approach. Part of the beauty of the VAP test is that it can help reduce the likelihood of this scenario occurring. Identifying risks for cardiovascular disease—and then working to correct them in order to prevent heart and vascular disease—is a better choice than costly surgical interventions. Baby boomers, who have taken more hands-on responsibility for their health than any previous generation, can be even more strongly motivated to adopt wellness strategies when they better understand the specific risks facing them. It is one thing to tell patients that their cholesterol is high and they need to reduce it by changing their diet and lifestyle or by taking medication. It is something else to tell them that they can decrease their risk of heart attacks and emergency room visits by implementing strategies to adjust their cholesterol particles. The more definitively a health threat can be identified, the greater the patients’ compliance with treatment will be. Since the National Cholesterol Education Program recommends people begin regular cholesterol testing at age 20, young adults can take a VAP test to learn about their cardiovascular disease risk early in life. This will allow them to take aggressive steps now—including diet and exercise—to maintain a healthy heart for life. Taking a VAP test now makes infinitely more sense than waiting until a cardiovascular catastrophe occurs, and then wondering if the event might have been prevented if a more complete cholesterol profile had been obtained earlier.
Should Everyone Take the VAP Test?This question is still being debated in the medical community. It is more expensive than routine cholesterol panels, but it provides more information. It is simply the best way for physicians to learn more about their patients and identify heart disease risk earlier. As time goes by, more physicians are recognizing the limitations of conventional lipid assessment and turning to advanced lipoprotein testing for better answers. Certainly anyone who has reason to believe he or she may be at high risk for cardiovascular disease—because of family history, previously diagnosed coronary or vascular disease, or factors such as high blood pressure, diabetes, obesity, any measure of coronary plaque, or identified abnormalities in cholesterol or triglycerides6—should strongly consider VAP testing. Even if you are simply concerned about heart disease, you can proactively encourage your doctor to perform this advanced test. It is now widely available in diagnostic laboratories around the country. Being proactive means being eager to learn about ways to improve your health, and working with your doctor to create a personalized prevention and treatment plan. However, when it comes to tests that involve risk—such as imaging procedures that deliver radiation—I caution you to be wary. Sometimes, being proactive can lead you down that slippery slope to unnecessary surgical intervention. Fortunately, the VAP test has the distinct advantage of providing added information without added risk.
Conclusion
The VAP cholesterol test provides accurate, detailed results, identifying people at risk for cardiovascular disease—with a detection rate that is more than twice that of routine cholesterol panels. Compared to conventional lipid panels, the sophisticated VAP test enables physicians to more accurately assess their patients’ risks for cardiovascular disease, and thus to better manage their treatment. As we learn more about emerging risk factors for heart disease, advanced lipid testing will become even more crucial in helping to arrest the progression of what remains America’s leading cause of premature death. Michael D. Ozner, MD, FACC, is a board-certified cardiologist specializing in cardiovascular disease prevention, and is author of The Miami Mediterranean Diet. | ||||||||||
| References | ||||||||||
| 1. Heart Disease and Stroke Statistics—2006 Update. Dallas, TX: American Heart Association; 2006. 2. Superko HR. Did grandma give you heart disease? The new battle against coronary artery disease. Am J Cardiol. 1998 Nov 5:82 (9A);34Q-46Q. 3. Castelli WP, Anderson K, Wilson PW, Levy D. Lipids and risk of coronary heart disease. The Framingham Study. Ann Epidemiol. 1992 Jan;2(1-2):23-8. 4. Lamarche B, TchernofA, Moorjani S, et al. Small, dense low-density lipoprotein particles as a predictor of the risk of ischemic heart disease in men. Prospective results from the Quebec Cardiovascular Study. Circulation. 1997 Jan 7;95(1):69-75. 5. Third Report of the National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults. (Adult Treatment Panel III) Final Report. Washington, DC: National Institutes of Health; 2002. NIH Publication No. 02-5215. 6. No author. The rising tide of metabolic syndrome. Foldout Feature. Postgrad Med. Dec 2004;116(6):54I-54VII. |