Life Extension Magazine®
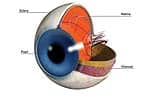
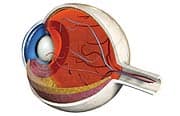
New Research Suggests that B Vitamins May Prevent Macular DegenerationMost individuals will sustain some degree of vision loss as they grow older. This is generally accepted as an “inevitable” part of the aging process. Underlying this seemingly innocuous phenomenon, however, lurks an unseen, debilitating danger: age-related macular degeneration—the leading cause of blindness in people over 50.1 This devastating condition is capable of rendering its victims virtually helpless over time. Blurred vision and the inability to recognize faces gradually progress to legal blindness in many cases. To date, conventional medicine has failed to identify satisfactory interventions. The good news is that advances in clinical nutrition have yielded a broad array of safe, low-cost, natural preventive strategies. Life Extension® has long emphasized the critical importance of such supplements as lutein, zeaxanthin, antioxidants, and omega-3 fatty acids in warding off macular degeneration.2,3 New research has unearthed yet another evidence-based nutritional defense: B vitamins.4 Macular Degeneration: A Link with Vascular Disease?While the exact causes are not fully understood, a growing body of scientific evidence points to chronic vascular disease as a cause of age-related macular degeneration. A growing number of scientists believe that macular degeneration is related to the slow degradation of blood vessels in the eye, specifically in the layer behind the retina known as the choroid, which contains the blood supply to the retina.5 The choroid supports the light-sensitive nerve cells in the retina, and provides them with their nourishment and oxygen supply. As a result, it is a region of high metabolic activity and one where oxidant stress is to be expected. In fact, eye conditions arising from oxidant injury to ocular vessels collectively represent the main causes of vision loss and blindness in developed countries, leading to retinopathy of prematurity in infants, diabetic retinopathy in mature adults, and age-related macular degeneration in older adults.5 The association of macular degeneration with vascular disease in the eye got a number of scientists thinking about whether there might be a common root cause—if macular degeneration shares common features with vascular disease, would cardiovascular risk factors also predict macular degeneration?6-12 Macular and Vascular Disease Share Common Risk Factors
Some of the first work done on this subject came from the ophthalmology laboratories of a group of Israeli researchers in 2004. They were interested in the relationship between plasma levels of the amino acid homocysteine and a particularly aggressive form of age-related macular degeneration known as exudative macular degeneration.6 By that time, homocysteine elevations were increasingly being recognized as a marker for cardiovascular risk. Although the exact mechanism is still unclear, it may be that increased levels of homocysteine cause vascular endothelial injury by promoting free radical release.13 The Israeli researchers studied a group of 59 older adults (average age 78 years) who had exudative or “wet” macular degeneration, a severe form of the disease in which blood vessels grow up from the choroid below the retina, resulting in a sudden loss of central vision. The scientists compared the participants’ homocysteine levels with those of 58 patients who had so-called “dry” macular degeneration (the less aggressive form), and with 56 control patients of similar ages. The results were unequivocal—patients with wet macular degeneration had homocysteine levels 28% higher than in the dry macular degeneration group and 22% higher than the control group. Fully 44% of the exudative macular degeneration patients had clinically elevated homocysteine levels, while only about 22% of the dry macular degeneration patients and controls had such elevations. Similar findings were reported the same year or shortly thereafter by other groups.7,9,14 which meant the hunt was on for more information about this intriguing (and worrisome) relationship. The next logical question, of course, was whether the elevated homocysteine levels might be associated with a deficiency in the B vitamins known to participate in keeping levels under control—particularly vitamin B12 and folate. By 2006, a Turkish research group was making progress in this area, studying 30 patients with exudative macular degeneration, 30 with dry macular degeneration, and 30 healthy controls.8 The researchers measured homocysteine levels as well as levels of B12 and folate.
Homocysteine levels were significantly higher in both macular degeneration groups compared with controls in this study, tending to be higher in the exudative group. Plasma vitamin B12 levels were significantly lower in the exudative group, compared with both controls and dry macular degeneration patients. In this study, no differences in folate levels were found, but the researchers concluded that their work suggested an association between macular degeneration and homocysteine, as well as nutrients that control its levels. In patients with cardiovascular disease, elevations in homocysteine are strongly associated with elevations in markers of inflammation—which makes sense because we now understand cardiovascular disease to be fundamentally a chronic inflammatory state. Would macular degeneration sufferers turn out also to have elevated markers of inflammation? Ophthalmologists at the University of Michigan took aim at that question with a 2005 study of homocysteine and C-reactive protein (CRP), by then a well-known inflammatory marker with an independent effect on cardiovascular disease risk.12 Studying 79 macular degeneration patients and 77 controls, the researchers conducted detailed cardiovascular histories, and then measured the two important biomarkers in subjects’ blood. They found the same elevations in homocysteine as had the previous researchers, and they also found a highly significant elevation in plasma CRP among macular degeneration patients that was absent in the control patients. The scientists noted that their work implicated the role of chronic inflammation and atherosclerosis as causative factors in macular degeneration.
The following year epidemiologists at Harvard’s prestigious Massachusetts Eye and Ear Infirmary demonstrated that both CRP and homocysteine levels are related to dietary and lifestyle factors that are associated with both cardiovascular disease risk and macular degeneration risk.11 This created, for the first time, a tight, logical relationship between dietary and lifestyle risk factors for cardiovascular disease and those for age-related macular degeneration at the population level. The Link with B VitaminsThe Harvard group’s work generated additional interest in dietary factors, and by 2007 a group in Sydney, Australia had published their own work exploring associations between elevated homocysteine levels and B vitamin status.10 Their study was massive, including 2,335 subjects, allowing for powerful statistical interpretations. They found that elevated homocysteine levels were associated with a more than 3-fold increase in risk for macular degeneration, while people with low B12 status had 2.3 times the risk of developing macular degeneration compared to people with normal B12 status. Additional work on the various mechanisms by which lowered nutrient status and elevated homocysteine and inflammatory markers produce age-related macular degeneration has now been conducted by scientists around the world.15,16
B Vitamins May Protect Eye HealthAn exciting development in prevention of macular degeneration came this year from Harvard researchers in the Division of Preventive Medicine at the Brigham and Women’s Hospital in Boston.4 Using 5,205 women 40 years or older who were known to have pre-existing cardiovascular disease or 3 or more cardiovascular risk factors (but who did not have macular degeneration at the start of the study) the researchers conducted a very large, randomized, placebo-controlled trial. Subjects were randomly assigned to receive either a combination of folic acid, pyridoxine (vitamin B6), and vitamin B12, or a placebo, and they were followed over an extended time period.
After an average of 7.3 years, the researchers had identified 55 cases of macular degeneration in the treatment group, but 82 cases in the placebo group—this came out to a risk reduction of 34% in the vitamin supplemented group! That protection level rose to 41% for macular degeneration that was causing visual problems. This is a truly stunning result, particularly since all subjects already had evidence of cardiovascular disease or increased risk, and also since the levels of supplementation were fairly modest—just 2.5 mg (2,500 mcg)/day of folate, 50 mg/day of B6, and 1 mg (1,000 mcg)/day of B12. The publication of this study in early 2009 makes a compelling case that, in the authors’ own words, “daily supplementation with folic acid, pyridoxine, and cyanocobalamin may reduce the risk of age-related macular degeneration.” While further studies are needed to determine if B vitamins protect other populations against macular degeneration, this study provides hope that B vitamins may offer an accessible and low-cost preventive strategy against a leading cause of blindness in older adults. SummaryMajor advances in nutritional science that have linked diet and lifestyle factors with cardiovascular disease are now bearing fruit in virtually every domain of human health. Scientists have now thoroughly documented the close relationship between cardiovascular disease and one of the major causes of blindness in older adults: age-related macular degeneration. Elevations in plasma levels of homocysteine, along with elevations in various markers of inflammation, are strongly correlated with both cardiovascular disease risk and with risk for age-related macular degeneration. Fortunately, we can attack both problems together through the intelligent use of nutritional supplements, particularly those in the B-vitamin family, and specifically folic acid, vitamin B6, and vitamin B12. These supplements, along with responsible attention to lifestyle modifications such as diet, exercise, and elimination of smoking can not only extend the quantity of life, but they can also contribute to a vastly improved quality of life through protection of the precious gift of vision. If you have any questions on the scientific content of this article, please call a Life Extension® Health Advisor at 1-866-864-3027. | |||||||||||
| References | |||||||||||
| 1. Bakalar N. Regimens: Vitamins show promise in protecting eyes. New York Times. 2009 Mar 3. 2. Arch Ophthalmol. 2007 Sep;125(9):1225-32. 3. BMC Ophthalmol. 2007 Feb 26;7:3. 4. Arch Intern Med. Feb 23 2009;169(4):335-41. 5. Prog Retin Eye Res. Jul 2008;27(4):331-71. 6. Am J Ophthalmol. Jan 2004;137(1):84-9. 7. Eye. Feb 2006;20(2):203-7. 8. Graefes Arch Clin Exp Ophthalmol. May 2006;244(5):565-9. 9. Eur J Ophthalmol. Nov-Dec 2005;15(6):764-7. 10. Am J Ophthalmol. Feb 2007;143(2):344-6. 11. Nutrition. Apr 2006;22(4):441-3. 12. Ophthalmology. Dec 2005;112(12):2076-80. 13. Eur Heart J. Jan 2009;30(1):6-15. 14. Am J Ophthalmol. Jan 2006;141(1):201-3. 15. Tohoku J Exp Med. Jan 2009;217(1):17-22. 16. Eur J Ophthalmol. Mar-Apr 2008;18(2):226-32. |