Life Extension Magazine®

Prostate cancer is the second leading cause of cancer death in American men.1
It is estimated that over 34,000 deaths will occur from metastatic prostate cancer in 2021.1
Low-cost PSA blood testing is one of our most valuable tools for detecting prostate cancer when it is still in its early curable stages.2
Our Dire Prediction Transforms into Lethal Reality
The United States Preventive Services Task Force (USPSTF) is a government-funded group that claims:
“to improve the health of all Americans by making evidence-based recommendations about clinical preventive services.”
In 2012 the USPSTF made a misguided recommendation that compelled me to write an editorial describing the USPSTF as a:
“Federal Death Panel”3
In 2008, the USPSTF recommended that men over age 75 not have their blood routinely screened for PSA.4
In 2012, the USPSTF recommended against routine PSA screening for all men 50 years of age and older.5
The initial effect of the USPSTF’s recommendations were declines in prostate cancer diagnosis. Everyone agreed this would happen because if the number of “PSA tests” go down, so do new cases…at least in the beginning.
Tragically, too many men who followed the USPSTF guidelines to not test their PSA are now facing advanced-stage prostate cancers.
As of 2016, a total of 11,387 more American men were diagnosed with metastatic prostate cancer compared to 2008 levels, when PSA blood test prevalence was robust.6
Few of these metastatic prostate cancer patients will be cured.7 Some are kept alive by grueling chemotherapy, radiation and hormone-ablation regimens, including castration in some cases.
Had the USPSTF not swept prostate cancer “under the rug” by recommending against PSA screening, thousands of lives could have been saved and an enormous amount of human suffering avoided.
As surging numbers of men succumb to advanced disease and harsh treatments, our dire prediction 8-12 years ago has been tragically vindicated.
This is of little value to those not able to recognize that the USPSTF was not acting on behalf of humanity.
PSA stands for: prostate-specific antigen.
When PSA blood levels increase above 1.0-2.0 ng/mL it may indicate a very early-stage cancer that is reversible in some cases by making healthy dietary choices.8-10
PSA is not just a potential prostate cancer marker.
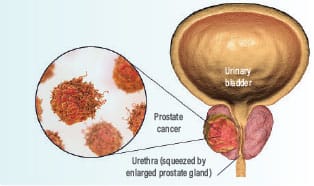
Prostate cells can emit PSA to break down healthy prostate tissues and help malignant cells invade tissues.11,12 This can enable malignant prostate cells to penetrate the prostate capsule and spread to soft tissue, regional lymph nodes and eventually bones.
A PSA reading over 1.0 ng/mL indicates that prostate health is in jeopardy.
One study, published in the New England Journal of Medicine, showed that 17% of the men with PSA levels between 1.1 to 2.0 ng/mL had prostate cancer.13
PSA increases at different rates in different conditions. In benign prostatic hypertrophy (BPH) there is usually a slow PSA increase over time. In prostate cancer, PSA levels can double over a relatively short period.14
How to Lower PSA Levels
PSA levels increase with age, but there are proven ways to reduce it.
These methods range from choosing healthier diets/lifestyles to taking drugs like Avodart® now sold as a generic called dutasteride. The typical dutasteride dose is 0.5 mg/day to improve urinary flow.15
Men who use drugs like dutasteride or finasteride shrink their prostate gland size about 25% and reduce their prostate cancer risk by around 25%.16-18
A minority of men complain about sexual side effects, while others are happy with improved head hair growth.
I often suggest that men with rising PSA levels who don’t want to use dutasteride make dietary changes that may accomplish similar benefits.
Advent of PSA Blood Testing
PSA blood tests became available around year 1990 and American men were quick to utilize them. In the United Kingdom, PSA testing was much less common.
This enabled researchers to study trends in prostate cancer mortality in the United States versus the UK spanning years 1975 to 2004.19 A comparative analysis was done to assess whether more PSA screening resulted in fewer prostate cancer deaths.
This study found that prostate cancer mortality peaked in the early 1990s at almost identical rates in both the USA and UK.
Starting after 1994, however, age-adjusted prostate cancer death rates in the United States declined four times more compared to those in the United Kingdom after 1992.
Both countries saw declines in prostate cancer deaths because of improved treatments and overall earlier detection, but the decline was four times greater in the United States. The best available explanation for this difference is the earlier PSA detection and better treatment options available in the United States.
The decline in prostate cancer mortality in the United States was greatest and most sustained in men aged 75 or older.
These findings were published in The Lancet Oncology with the following interpretations:19
“The striking decline in prostate cancer mortality in the USA compared with the UK in 1994–2004 coincided with much higher uptake of PSA screening in the USA.”
These data published in May 2008 showed the greatest death rate decline in response to PSA testing occurred in men over age 75.
Despite these findings, the United States Preventive Services Task Force (USPSTF) issued a recommendation in August 2008 (widely disseminated by the media) that older men should not undergo PSA screening.
This specific USPSTF recommendation of August 2008 was:20
“Do not screen for prostate cancer in men age 75 years or older.”
Fighting Back Against USPSTF Guidelines
In 2012, the USPSTF went a step further and recommended against routine PSA screening for all men ages 50 and older.5
This led to an uproar among various medical specialists who argued for and against routine PSA screening.
Life Extension® led a charge against these egregiously misguided USPSTF anti-PSA-testing recommendations.
We persuaded large numbers of men to continue having annual PSA blood tests in order to detect prostate malignancies in early stages when they are curable using minimally invasive therapies like high-resolution image-guided cryo-ablation.
Partial Capitulation
As scientific evidence mounted against the USPSTF’s position on PSA screening, a major concession was made.
In 2018 the United States Preventive Services Task Force (USPSTF) backtracked on its 2012 recommendation against PSA screening. Their new suggestion is that men aged 55–69 should make an individual decision about routine screening in consultation with their physician.21
While this represents a partial capitulation, we vehemently disagree that early diagnosis of prostate cancer should be limited to men aged 55–69.
Prostate cancer risk begins around age 40,22 and this is when men should have their first PSA blood test.
We at Life Extension® don’t write off men over age 69, and we urge these men to have annual PSA blood tests to ascertain prostate cancer risk and take steps to reverse the course of early-stage disease using nutritional and drug interventions.
Diagnoses Decline but then Head Higher

On May 23, 2020, a study was published that evaluated American men who developed regional (outside the prostate capsule) and metastatic prostate cancers since PSA screening was first discouraged in 2008.6
As expected, rates of newly diagnosed prostate cancers declined as fewer men underwent PSA blood tests. But avoiding a PSA test does not make the disease disappear. It only delays the eventual diagnosis to a time when the prostate cancers are more advanced and often incurable.
For example, this study found that for the years 2007 to 2016, the incidence of local-stage, non-advanced prostate cancer decreased by 6.4% per year in men ages 50 to 74, and by 10.7% per year in men ages 75 years and beyond.6
These decreases in early-stage disease reflected fewer PSA tests being performed, which meant fewer men were diagnosed in asymptomatic stages when cure rates are very high.
For regional-stage prostate cancer, where the tumor extends beyond the prostate capsule, but is contained in the pelvic genital-urinary region, incidence rates surged 11.1% per year higher from 2012-2016 after stable rates from 2005-2012.6
For distant-stage, advanced prostate cancer, incidence increased from 2010-2016 by 5.0% per year after declining by 0.9% per year from 2005-2010.6
This means there were increased rates of advanced (regional- and distant-stage disease) prostate cancers in the years (2010-2016) after PSA screening began plummeting.
A major factor likely responsible for this increased incidence per year from 2010-2016 in regional- and distant- stage disease was the USPSTF guidelines recommending against routine PSA screening.
How Many Men Impacted By Year 2016?
The researchers looked at how many excess cases of metastatic prostate cancer occurred from 2009 through 2016 and compared them to the historically low 2008 rate (before USPSTF advised against PSA screening).6
A total of 11,387 more men aged 50 or greater were diagnosed with distant-stage (metastatic) prostate cancers from 2009-2016 in the U.S. than would have been, had the incidence of advanced-stage/metastatic disease remained at 2008 levels.6
The researchers commented that in 2016 alone, the last year of the analysis, there were 3,590 additional men living with advanced-stage metastatic prostate cancer because of the change in incidence since 2008 (when PSA screening was widespread).
Declining Rates of PSA Testing
The USPSTF’s attack on PSA blood testing had a huge impact on reducing the number of men over age 50 who underwent PSA screenings.
What if Your PSA Blood Level is Elevated?
The “normal” reference range for PSA is 0-4 ng/mL.
The optimal PSA blood level is 1.0 ng/mL and lower for healthy men.
When PSA becomes elevated above 1.0-2.0 ng/mL, this indicates activity in the prostate gland that may relate to inflammation,benign growth, and/or cancer.
Unlike typical cancers, some prostate malignancies appear reversible.
Nutrients like curcumin,26,27 boron,28,29 and vitamin D30-33 have been shown to support prostate health and facilitate PSA reduction.
Drugs like finasteride and dutasteride can cut PSA by 50%.34,35 This is more than just a number-reducing effect. Men taking these drugs reduce their prostate cancer risk by about 25%.16-18
When PSA levels are above 1.0-2.0 ng/mL, this can be an early warning that a problem is developing in the prostate gland. After dietary, nutrient and/or drug therapies are initiated, the PSA should be retested in the next three to six months to ensure the changes are resulting in a reduced PSA level.
Annual (or twice yearly) PSA blood tests thereafter enable an aging man and his physician to monitor the status of his prostate gland, both from a quality-of-life standpoint as it relates to BPH and to catch a malignancy in its early stages when cure rates are virtually 100%.
New minimally invasive techniques can now be done on an outpatient basis. These include enhanced imagery-guided cryo-ablation or laser therapies that seek to destroy only the malignant portion of the prostate gland.
This is a vast improvement over conventional methods involving radical prostatectomy (major surgery) or radiation that damages surrounding healthy tissues.
Table 1. Timeline for PSA Testing
1990s: PSA blood tests become widely available in U.S.
2008: PSA blood testing peaks in U.S.
2008: Study shows PSA testing reduces prostate cancer mortality.
2008: USPSTF urges men over 75 years to avoid PSA screening.
2012: USPSTF urges all men to avoid PSA screening.
2013: Life Extension® alleges USPSTF functions as a “death panel.”
2018: USPSTF says men aged 55-69 may consider PSA screening.
2020: Report reveals relative surge in advanced prostate cancer since 2008.
According to national self-reported survey data, routine PSA testing rates among men age 50 years and over were at 40.6% in 2008. That meant that 40% of American men over age 50 had their blood tested to check PSA levels.23,24
This percent of men aged 50 and over having routine PSA tests dropped to 38.3% in 2010 and then to 31.5% in 2013 and remained unchanged in 2015.23,24
Similar declines in PSA testing have been reported on Medicare claims data.25
This decline in PSA testing correlates with the surge in regional- and advanced-stage (metastatic) incidence for prostate malignancies over this time period.
How Many Men Affected Since Year 2016?
Prostate cancer is often an insidious, slow-growing disease without outward side effects.
The first symptom of metastatic disease can be bone pain (back or pelvic areas) as prostate cancer cells infiltrate into bone and accelerate its breakdown.
Bony metastasis is often termed stage 4 disease. It can be treated with hormone ablation, radiation and chemotherapy drugs to enable a man to live for many years—but while enduring chronic pain and disability inflicted by the malignant cells, the toxic drugs/radiation, and the deprivation of testosterone.
Testosterone deprivation is associated with significant mental and physical health issues such as depression, aggravation of cardiovascular disease, acceleration of frailty, and muscle wasting.
As new data sets emerge, we will learn how many more men who avoided PSA screening are afflicted with advanced malignancies.
Impact of Misguided Recommendations Not Yet Known
I continue to predict that the decline in PSA screening will result in more men being diagnosed with advanced prostate malignancies.
Compare the tragedy of delayed diagnosis to far gentler procedures like precise imaging-guided cryo-ablation that is often curative when the disease is caught in localized (early) stages.
I am gratified to those who stood up to the USPSTF and unwarranted media attacks on PSA screening so that at least 30% of men over age 50 today are likely having regular PSA blood tests.
There are historic examples of effective procedures falling out of favor with a corresponding increase in the numbers of people who needlessly suffer and die.
One such example is scurvy, the disease that sickened and killed millions, long after a citrus cure was discovered. (See Table 2 below for a brief chronology.)
Table 2. How Scurvy Relates to PSA Test Debates
1497: Citrus shown to cure scurvy.
1747: James Lind proves citrus cures scurvy.
1799: Britain mandates sailors ingest citrus.
1870: Citrus cure officially discredited.
1911: Dr. Robert Scott loses crew to scurvy.
1932: Vitamin C proven to cure scurvy.
Thousands of Deaths After Cure is Discovered
Most male readers of Life Extension® magazine screen for PSA and make adjustments if levels are higher than optimal.
As you can see on the next page, PSA testing is included in the popular Male Blood Test Panel that many of our readers utilize each year.
For longer life,
William Faloon
References
- Available at: https://www.cancer.org/cancer/prostate-cancer/about/key-statistics.html. Accessed March 16, 2021.
- Schroder FH, Hugosson J, Roobol MJ, et al. Screening and prostate cancer mortality: results of the European Randomised Study of Screening for Prostate Cancer (ERSPC) at 13 years of follow-up. Lancet. 2014 Dec 6;384(9959):2027-35.
- Available at: https://www.lifeextension.com/Magazine/2013/5/Federal-Death-Panels/Page-01. Accessed March 16, 2021.
- Available at: https://www.uspreventiveservicestaskforce.org/uspstf/recommendation/prostate-cancer-screening-2008. Accessed March 16, 2021.
- Available at: https://www.uspreventiveservicestaskforce.org/uspstf/recommendation/prostate-cancer-screening-2012. Accessed March 16, 2021.
- Jemal A, Culp MB, Ma J, et al. Prostate Cancer Incidence 5 Years After US Preventive Services Task Force Recommendations Against Screening. J Natl Cancer Inst. 2021 Jan 4;113(1):64-71.
- Available at: https://www.cancer.org/cancer/prostate-cancer/detection-diagnosis-staging/survival-rates.html. Accessed March 22, 2021.
- Available at: https://www.lifeextension.com/magazine/2013/12/impact-of-diet-on-prostate-cancer-risk-and-mortality. Accessed April 12, 2021.
- Available at: https://www.lifeextension.com/magazine/2016/6/how-to-reverse-markers-of-prostate-cancer. Accessed April 12, 2021.
- Available at: https://www.lifeextension.com/magazine/2018/12/dietary-approaches-reduce-prostate-cancer-risk. Accessed April 12, 2021.
- Cumming AP, Hopmans SN, Vukmirovic-Popovic S, et al. PSA affects prostate cancer cell invasion in vitro and induces an osteoblastic phenotype in bone in vivo. Prostate Cancer Prostatic Dis. 2011 Dec;14(4):286-94.
- Webber MM, Waghray A, Bello D. Prostate-specific antigen, a serine protease, facilitates human prostate cancer cell invasion. Clin Cancer Res. 1995 Oct;1(10):1089-94.
- Thompson IM, Pauler DK, Goodman PJ, et al. Prevalence of prostate cancer among men with a prostate-specific antigen level < or =4.0 ng per milliliter. N Engl J Med. 2004 May 27;350(22):2239-46.
- Descotes JL. Diagnosis of prostate cancer. Asian J Urol. 2019 Apr;6(2):129-36.
- Available at: https://www.accessdata.fda.gov/drugsatfda_docs/label/2011/021319s023s025lbl.pdf. Accessed March 17, 2021.
- Wu Y, Wang Y, Gu Y, et al. Prostate Cancer Risk and Prognostic Influence Among Users of 5-Alpha-Reductase Inhibitors and Alpha-Blockers: A Systematic Review and Meta-Analysis. Urology. 2020 Nov;145:216-23.
- Chau CH, Figg WD. Revisiting 5alpha-reductase inhibitors and the risk of prostate cancer. Nat Rev Urol. 2018 Jul;15(7):400-1.
- Available at: https://www.sciencedirect.com/topics/medicine-and-dentistry/dutasteride. Accessed March 17, 2021.
- Collin SM, Martin RM, Metcalfe C, et al. Prostate-cancer mortality in the USA and UK in 1975-2004: an ecological study. Lancet Oncol. 2008 May;9(5):445-52.
- Force USPST. Screening for prostate cancer: U.S. Preventive Services Task Force recommendation statement. Ann Intern Med. 2008 Aug 5;149(3):185-91.
- Force USPST, Grossman DC, Curry SJ, et al. Screening for Prostate Cancer: US Preventive Services Task Force Recommendation Statement. JAMA. 2018 May 8;319(18):1901-13.
- Bleyer A, Spreafico F, Barr R. Prostate cancer in young men: An emerging young adult and older adolescent challenge. Cancer. 2020 Jan 1;126(1):46-57.
- Negoita S, Feuer EJ, Mariotto A, et al. Annual Report to the Nation on the Status of Cancer, part II: Recent changes in prostate cancer trends and disease characteristics. Cancer. 2018 Jul 1;124(13):2801-14.
- Available at: http://pressroom.cancer.org/JemalUSPSTF2020. Accessed March 22, 2021.
- Cooper GS, Kou TD, Schluchter MD, et al. Use of prostate-specific antigen testing in Medicare beneficiaries: Association with previous evaluation. Family Medicine and Community Health. 2017;5(2):109-18.
- Fabiani A, Morosetti C, Filosa A, et al. Effect on prostatic specific antigen by a short time treatment with a Curcuma extract: A real life experience and implications for prostate biopsy. Arch Ital Urol Androl. 2018 Jun 30;90(2):107-11.
- Choi YH, Han DH, Kim SW, et al. A randomized, double-blind, placebo-controlled trial to evaluate the role of curcumin in prostate cancer patients with intermittent androgen deprivation. Prostate. 2019 May;79(6):614-21.
- Gallardo-Williams MT, Chapin RE, King PE, et al. Boron supplementation inhibits the growth and local expression of IGF-1 in human prostate adenocarcinoma (LNCaP) tumors in nude mice. Toxicol Pathol. 2004 Jan-Feb;32(1):73-8.
- Cui Y, Winton MI, Zhang ZF, et al. Dietary boron intake and prostate cancer risk. Oncol Rep. 2004 Apr;11(4):887-92.
- Xie DD, Chen YH, Xu S, et al. Low vitamin D status is associated with inflammation in patients with prostate cancer. Oncotarget. 2017 Mar 28;8(13):22076-85.
- Beer TM, Ryan CW, Venner PM, et al. Double-blinded randomized study of high-dose calcitriol plus docetaxel compared with placebo plus docetaxel in androgen-independent prostate cancer: a report from the ASCENT Investigators. J Clin Oncol. 2007 Feb 20;25(6):669-74.
- Vijayakumar S, Mehta RR, Boerner PS, et al. Clinical trials involving vitamin D analogs in prostate cancer. Cancer J. 2005 Sep-Oct;11(5):362-73.
- Petrou S, Mamais I, Lavranos G, et al. Effect of Vitamin D Supplementation in Prostate Cancer: A Systematic Review of Randomized Control Trials. Int J Vitam Nutr Res. 2018 Feb;88(1-2):100-12.
- Pannek J, Marks LS, Pearson JD, et al. Influence of finasteride on free and total serum prostate specific antigen levels in men with benign prostatic hyperplasia. J Urol. 1998 Feb;159(2):449-53.
- Choi YH, Cho SY, Cho IR. The different reduction rate of prostate-specific antigen in dutasteride and finasteride. Korean J Urol. 2010 Oct;51(10):704-8.

