
Vertigo and Dizziness
Vertigo and Dizziness
Last Section Update: 01/2025
Contributor(s): Maureen Williams, ND; Shayna Sandhaus, PhD; Stephen Tapanes, PhD
1 Overview
Summary and Quick Facts for Vertigo and Dizziness
- Vertigo is an unpleasant sensation of spinning, dizziness, or motion that can be quite debilitating. It is more common in older adults and typically arises from problems in the inner ear structures or central nervous system.
- With no treatment, over 60% of patients with the most common type of vertigo (caused by debris in the inner ear) recover within four weeks.
- This protocol summarizes the types and causes of dizziness and vertigo and the different treatment strategies available, including repositioning techniques to remove debris from the inner ear either at home or at the doctor’s office.
- Evidence has been reported for the benefit of vitamin D and calcium supplementation in patients with low vitamin D levels and benign paroxysmal positional vertigo (BPPV).
Vertigo, typically characterized by a sensation of spinning or dizziness, is usually caused by problems involving the inner ear (peripheral vertigo) or, less commonly, the central nervous system (central vertigo). Seeking medical attention quickly for sudden unexplained vertigo is essential, as stroke is an uncommon but life-threatening cause of vertigo.
Dizziness usually falls into one of four categories: vertigo, fainting sensation (presyncope), imbalance sensation (disequilibrium), and lightheadedness.
Some types of vertigo and dizziness are associated with abnormal glucose metabolism, osteoporosis, sleep apnea, and menopause and hormone fluctuations.
The primary treatment for the most common type of vertigo, caused by debris in the inner ear, is repositioning therapy, which can relieve vertigo in a single session when performed by a trained clinician. At-home repositioning techniques may also improve vertigo.
Natural interventions, such as vitamin D, calcium, ginkgo biloba, and coenzyme Q10 (CoQ10) have shown promise for the management of vertigo.
What are Vertigo Causes and Risk Factors?
- Debris in the inner ear causes benign paroxysmal positional vertigo (BPPV), the most common type of vertigo, which accounts for between 17% and 42% of cases.
- Another potential cause of vertigo is Ménière disease, a rare but serious condition associated with progressive episodes of vertigo, hearing loss, and tinnitus (ringing in the ears).
- Migraine sufferers have an elevated risk of developing vertigo, as do older people, women, and people with a family history of the condition.
- Several comorbid conditions increase the risk of vertigo, including diabetes and abnormal glucose metabolism, osteoporosis, high cholesterol, and depression and anxiety.
- Many medications can cause dizziness or vertigo, including some antibiotics, statins, and antidepressants. If a new medication was initiated soon before to the onset of vertigo, it should be more closely scrutinized as a possible factor contributing to symptoms.
How is the Cause of Vertigo Diagnosed?
- Physicians must rule out urgent causes of vertigo and dizziness, such as stroke.
- Several vertigo diagnostic algorithms are available, with most depending on the timing, triggers, and duration of vertigo episodes.
- A physical examination that evaluates for nystagmus or other eye movement abnormalities may help a clinician rule out certain causes of dizziness.
- A specialized maneuver called the Dix-Hallpike test may help diagnose BPPV.
- Emerging findings suggest serum protein S100-beta, a novel diagnostic biomarker, may be useful in differentiating vertigo caused by vascular stroke.
- Generally, laboratory evaluation and imaging are not necessary to identify the cause of vertigo.
How is Vertigo Treated?
- Manual manipulation techniques, including the Semont and Epley maneuvers, are designed to move debris out of the semicircular canals in the inner ear and are effective in the majority of cases of BPPV.
- The half-somersault maneuver to move crystals out of the semicircular canals is a technique developed for at-home use without assistance.
- Diuretic medications are commonly used to treat Ménière disease, but some evidence suggests medication may not be effective.
What Novel and Emerging Strategies May Benefit Those with Vertigo?
- Flunarizine, a calcium channel blocker drug used for migraines in Europe but not approved in the United States, has shown promise as a potential treatment for migraine-associated vertigo. Another calcium channel blocker and antiemetic, cinnarizine, is being explored as a potential vertigo therapy as well. Neither drug is available in the United States as of early 2021.
- Piracetam, a derivative of the neurotransmitter gamma-aminobutyric acid (GABA), has been investigated as a treatment option for Ménière disease.
- Biofeedback techniques incorporated into vestibular rehabilitation programs have appeared promising as well.
What Dietary and Lifestyle Considerations May Benefit Those with Vertigo?
- Follow a consistent low-sodium diet for Ménière disease.
- Avoid migraine trigger foods (including red wine, cheese, and chocolate) if vertigo is experienced with migraines.
- Stress reduction may be helpful.
What Nutrients Can Benefit Vertigo?
- Vitamin D: Vitamin D supplementation may improve positional vertigo, especially in those with low vitamin D status.
- Ginkgo biloba: In a 12-week trial in subjects with vertigo, ginkgo extract daily was more effective and better tolerated than betahistine, a medication sometimes used to treat vertigo related to Ménière disease.
- Ginger root: Some studies suggest ginger may help relieve vertigo and associated symptoms, such as nausea.
- Coenzyme Q10 (CoQ10): Patients with congestive heart failure were treated with CoQ10 and 73% of patients with vertigo reported improvement in their vertigo.
2 Introduction
Vertigo is the perception of movement while not in motion; it typically manifests as a sensation of spinning, swaying, or tilting. Vertigo may be perceived as motion of oneself or one’s environment. It may be accompanied by nausea and vomiting or a lack of physical steadiness or equilibrium.1 Vertigo is a symptom, not a diagnosis. It is usually caused by problems in the inner ear or central nervous system.1,2 Importantly, vertigo can be a symptom of a serious condition, such as stroke. Seeking medical attention quickly for sudden, unexplained vertigo is essential.3
Although many people assume that “vertigo” and “dizziness” are synonymous, this is not the case. Vertigo typically includes a sensation of dizziness, but not all patients with dizziness also complain of a sensation of motion while not moving (vertigo). In addition to vertigo, several other types of dizziness have been identified and can be loosely characterized by how they are perceived: presyncope (fainting sensation), disequilibrium (imbalance sensation), and lightheadedness (feeling faint or about to pass out).2,4,5 Both vertigo and dizziness have underlying causes that must be identified and addressed.6-9
Up to 20% of the population may experience at least one episode of dizziness or vertigo per year.10,11 The prevalence increases with age: about half of people over age 85 years experience periodic vertigo or dizziness.12 Vertigo can interfere with one’s ability to work and live independently, reducing quality of life.13 Vertigo is a common cause of falls among older individuals, and falls are a leading cause of accidental death in seniors.12,14,15 For patients with recurrent vertigo or with functional or quality of life limitations due to vertigo symptoms, treatment will vary with the cause, but may include nonpharmacologic, pharmacologic, and/or integrative interventions.16-22
The most common type of vertigo, benign paroxysmal positional vertigo, or BPPV, accounts for between 17% and 42% of vertigo cases.15,16 BPPV is most commonly caused by displaced particles of calcium debris (called canaliths) in the small canals of the inner ear.1 These canals are important parts of the body’s equilibration system. Most cases of BPPV resolve within four weeks, even without treatment.23 BPPV can often be treated with maneuvers intended to move the particles out of the canals (known as repositioning). The canalith repositioning maneuver (also called the Epley maneuver) is performed by a clinician and can rapidly resolve many cases of vertigo.16 Additionally, some unassisted movement techniques, including the half-somersault maneuver, can be used to self-treat vertigo at home in some cases.24-26
Other causes of vertigo, such as vestibular migraine and Ménière disease, may respond to medication.17,18 Some emerging interventions, such as correction of jugular vein abnormalities and biofeedback therapy, continue to undergo research in the context of vertigo.19-22
Several chronic conditions have been linked with vertigo or dizziness, including anxiety,27 diabetes,28-32 osteoporosis,33,34 migraine,35-38 and sleep apnea.35-38 Therefore, appropriate management includes treatment of chronic predisposing conditions.39 Several natural agents such as vitamin D, calcium, ginkgo biloba, and coenzyme Q10 may be effective adjuvants in the management of vertigo.40-42 Depending on the cause of vertigo, some dietary and lifestyle considerations, such as a low-sodium diet, may reduce the severity or frequency of symptoms as well.
3 Background
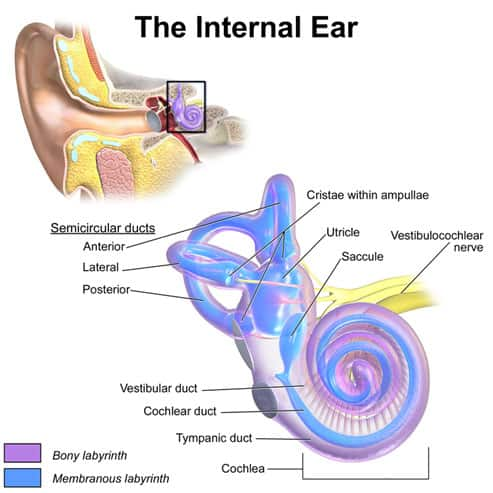
Vertigo can result from disturbances of either the vestibular structures of the inner ear, which sense linear and angular motion, or the regions of the central nervous system that transmit and process signals from the vestibular organs. The key vestibular organs implicated in vertigo are the semicircular canals or ducts, as well as the utricle and saccule, which are often referred to as the otolith organs (Figure 1).43 The brain receives signals from both the right and left inner ears via the vestibulocochlear nerve (also called the eighth cranial nerve [CN VIII]). During movement, differences in nerve signaling from the right and left ears are interpreted as motion. When individuals experience vertigo, asymmetric right-left signaling resulting from inner ear problems or central nervous system issues results in an abnormal sensation of motion.1,44
Vertigo has been classically separated into two main categories: peripheral and central. While there is some overlap between peripheral and central causes of vertigo, peripheral vertigo primarily arises from problems in the vestibular apparatus of the inner ear or the vestibular nerve. Central vertigo arises from problems in the cerebellum or brainstem where signals from the vestibular system are received and interpreted.1,44 The majority—roughly 80%—of cases of vertigo are of the peripheral type.1
Depending on the underlying condition, vertigo and dizziness can present in a variety of ways (see Table 1). Typically, episodes of vertigo can be characterized by their timing, triggers, and associated symptoms.2 Physicians use certain tests to help identify the type of dizziness a patient is experiencing. For example, assessment of nystagmus (rapid, involuntary eye movement) with the Dix-Hallpike maneuver (see Diagnosis) can help rule out vertigo, and monitoring orthostatic blood pressure can help rule out presyncope due to hypotension.8
4 Causes and Risk Factors
Many factors can contribute to vertigo and dizziness, including inner ear problems, medication side effects, or motion sickness. Some of these conditions can be serious, while others may be relatively minor or transient. The underlying causes and risk factors for vertigo are outlined in Table 1.
Risk Factors for Vertigo
Risk factors associated with vertigo include:
- Older age46,47
- Female gender46,47
- Menopause and associated hormonal fluctuations48
- Low levels of vitamin D47
- Osteoporosis47
- Migraine headache47
- Head and neck trauma47
- High total cholesterol levels47
- Depression and anxiety49,50
- Stress51
- Family history of balance disorders52
| Table 1. Common Origins and Manifestations of Vertigo1,53 | |
| Peripheral Causes of Vertigo | |
|---|---|
| Benign paroxysmal positional vertigo (BPPV)16 |
|
| Herpes zoster oticus (Ramsay Hunt syndrome)54 |
|
| Ménière disease55 |
|
| Vestibular neuritis (also called vestibular neuronitis or peripheral vestibulopathy) and labyrinthitis56 |
|
| Central Causes of Vertigo | |
| Brainstem ischemia (insufficient blood flow), including transient ischemic attack57 |
|
|
Stroke and hemorrhage57 |
|
| Vestibular migraine58 |
|
Causes of Peripheral Vertigo
Approximately 80% of vertigo cases are due to peripheral causes. The most common cause of vertigo overall is benign paroxysmal positional vertigo (BPPV), often shortened to “positional vertigo.” BPPV usually occurs when debris in the inner ear moves during head movement, triggering brief spells of vertigo.1,16
There are two main types of BPPV: posterior semicircular canal BPPV (also known as posterior canal BPPV) and horizontal semicircular canal BPPV (or horizontal canal BPPV). The vast majority of BPPV is posterior canal BPPV, accounting for 85% to 95% of cases. Posterior canal BPPV is usually attributed to canalithiasis, which occurs when fragmented calcium crystals become lodged in the posterior canal. Horizontal BPPV is also believed to be caused by debris particles; however, less is known about the pathology of this form of BPPV.1,16 In certain atypical cases, BPPV can be caused by abnormalities in the brain or nervous system, but this is rare.26
Another common cause of vestibular vertigo is Ménière disease. The precise underlying cause of Ménière disease is not yet clear. Patients with Ménière disease have changes in their inner ear fluid volume, called endolymphatic hydrops, which is believed to lead to swelling, distortion, and small tears in the membrane of the inner ear. These changes lead to progressive symptoms, with both increasing frequency and severity of vertigo and hearing loss. The cause of endolymphatic hydrops is unclear, and while all patients with Ménière disease have endolymphatic hydrops, not all patients with endolymphatic hydrops have Ménière disease, which has led to the suggestion of an array of possible causes including genetic predisposition, viral infection, and multiple other biochemical and immune factors.18,59
Vestibular neuritis and labyrinthitis are other common causes of vertigo. Vestibular neuritis (inner ear inflammation) is usually caused by an infection of the vestibular branch of the eighth cranial nerve (CN VIII) that transmits signals from the inner ear to the brain.56 Labyrinthitis is an inflammatory, typically infectious, condition of the labyrinth.60
Other causes of peripheral vertigo include1,12,68:
- Herpes zoster oticus (reactivation of the virus that causes chicken pox [a condition known as shingles] with lesions affecting the inner ear)
- Otitis media (inflammation [usually of infectious origin] of the middle ear)
- Medication side effects and interactions (see Table 2)
- Concussion with trauma to peripheral vestibular organs
- Otosclerosis (hardening of middle ear structures)
Causes of Central Vertigo
Approximately 20% of vertigo cases are due to central causes of which vestibular migraine is one of the most common. Vestibular migraine is defined as the presence of vertigo episodes and other vestibular symptoms caused by migraine.69 This condition is poorly understood even though one epidemiologic study concluded that it occurs in up to 2.7% of the adult U.S. population.69,70 Numerous possible overlapping mechanisms have been proposed for vestibular migraine. One hypothesis is that in some patients, vestibular migraine is a typical migraine aura, which is caused by an abnormal wave of neuronal signaling in the brainstem. Studies have also reported that calcitonin gene-related peptide, which is known to play a role in the development of migraine and serves as a therapeutic migraine target, may signal vestibular receptors.71,72 In addition, an observational study found migraine sufferers in general were at higher risk of developing BPPV,73 and features of migraine may be present during episodes of Ménière disease.74,75
Other causes of central vertigo include1:
- Cerebrovascular disease, including transient ischemic attack, stroke, or hemorrhage, affecting the medulla or cerebellum
- Multiple sclerosis
- Seizure disorder
- Genetic conditions
- Disembarkment syndrome (a sense of motion and imbalance following a period of being in passive motion)
| Table 2: Medications and Substances That May Cause Peripheral or Central Vertigo or Dizziness76-79 | |
|
|
|
|---|---|
|
Antibiotics Cinoxacin, levoxacin, ciprofloxacin, amoxicillin plus clavulanic acid, aminoglycosides, tetracyclines, amikacin, erythromycin, azithromycin, clarithromycin |
May be ototoxic (cause damage to or dysfunction of inner ear structures or nerves involved in equilibration); aminoglycosides can cause irreversible ototoxicity |
|
Diuretics Ethacrynic acid, furosemide, hydrochlorothiazide |
Related to postural hypotension (low blood pressure upon standing); some are potentially ototoxic |
|
Antihypertensives Enalapril, zofenopril, irbesartan, lacidipine, amlodipine, nifedipine, nicardipine |
Due to hypotension (low blood pressure) |
|
Anti-inflammatories and Pain Relievers Aspirin, acetaminophen, acetylsalicylic acid, ibuprofen, celecoxib, diclofenac, dexketoprofen, ketorolac, naproxen |
Potentially ototoxic |
|
Dopaminergic/Parkinson Disease Medications Bromocriptine, levodopa/carbidopa |
May worsen hypotension when taken with antihypertensives |
|
Antipsychotics Chlorpromazine, clozapine, thioridazine |
May cause hypotension |
|
Antidepressants Mirtazapine, paroxetine, sertraline, trazodone, amitriptyline, doxepin |
May cause vertigo or dizziness with or without hypotension |
|
Anti-seizure Medications Lamotrigine, oxcarbazepine, carbamazepine, lacosamide, clonazepam |
Although these are sometimes used in the treatment of certain types of vertigo they also may have vertigo as a side effect |
|
Platinum-Derived Chemotherapy Cisplatin, carboplatin, oxaliplatin |
A fairly common side effect is irreversible, progressive ototoxicity, with cisplatin being the worst of the three80 |
|
Antifungal and Antimalarial Medications Amphotericin B, fluconazole, itraconazole, flucytosine, chloroquine |
May be ototoxic |
| Oral Contraceptives | Some physiological variations associated with oral contraceptive (OC) use (eg, impaired water and electrolyte balance, variations of endolymphatic pH, and impairment of glucose or lipid metabolism) have been hypothesized to contribute to vertigo in some cases.81 However, this appears to be rare and may vary with type of OC drug, as some OC regimens may be associated with improvements in Meniere’s disease symptoms.82 In general, if vertigo occurs in association with OC use, OC drugs should be considered as apossible contributor. |
| Alcohol | May damage the vestibular system |
| Caffeine | Avoidance may be beneficial in Ménière disease and vestibular migraine83 |
|
Heavy Metals and Metalloids Arsenic, lead, mercury |
May be ototoxic |
| Tobacco | May cause dizziness, vertigo, and tinnitus |
| Note: If vertigo onset occurs shortly after initiation of a new medication, the medication as a potential trigger of vertigo should be ruled out by a qualified healthcare provider. | |
5 Conditions Associated With Vertigo and Dizziness
Vertigo and dizziness are associated with several systemic disorders. While the connections between some particular health conditions and vertigo or dizziness are well understood (eg, orthostatic hypotension and dizziness),88 other associations remain the subject of intriguing ongoing research. Some of these associations will be reviewed here.
Abnormal Glucose Metabolism
Vertigo, particularly that caused by Ménière disease, has been shown to be associated with abnormalities of glucose and insulin metabolism.29-31 In fact, people with diabetes may have up to a 70% higher risk of a balance disorder,15 and high glucose and insulin levels have been associated with increased risk of BPPV recurrence.32
The inner ear is rich in insulin receptors. Chronically elevated insulin levels may affect inner ear blood flow, disrupting the complex chemical balance of inner ear fluids and resulting in vestibular dysfunction.32 More information is available in Life Extension’s Diabetes and Glucose Control protocol.
Osteoporosis
People with osteoporosis and osteopenia (reduced bone mineral density but less severe than osteoporosis) were found in two case control studies to have about a 1.3-fold higher risk of developing BPPV.89 In one study, women with osteoporosis and BPPV were more than three times as likely to have recurrent vertigo than women without osteoporosis, and the rate of recurrence increased as bone mineral density decreased.90 In another study, having been treated for osteoporosis was correlated with a lower risk of BPPV in women 51 to 60 years old.91 Numerous studies have found associations between measures of bone metabolism and bone density, vitamin D levels, and BPPV.92-97 Provisional evidence for a causative contribution of vitamin D deficiency to BPPV comes from a clinical trial that treated severe vitamin D deficiency (<10 ng/mL) and found a highly significant 73% reduction in symptom recurrence.98 This relationship has been hypothesized to result from vitamin D–associated calcium channel proteins in the epithelium that play a role in calcium metabolism of the vestibular organ of the inner ear.96
Studies have also shown that the fracture risk is significantly higher in individuals with BPPV.99,100 This highlights the importance of both BPPV and osteoporosis management, given the elevated risk of falls among people with BPPV.101 For more information about bone health see Life Extension’s Osteoporosis protocol.
Menopause and Associated Hormonal Fluctuations
The average age of menopause in the United States is 51 years, and BPPV incidence has been shown to be relatively high among women aged 40 years and older. Researchers have suggested that a complex interplay between changing hormone levels, aging, and calcium crystals in the inner ear may influence BPPV susceptibility, particularly in perimenopausal women.48,102 Of note, menopause has been strongly linked with the development of osteopenia and osteoporosis (primarily due to decling estrogen levels); however, there are other mechanisms by which hormones, particularly estrogen, may contribute to BPPV.102 Low vitamin D levels have also been reported in postmenopausal women with BPPV.103
In one retrospective population study, women who had taken conventional hormone replacement therapy (HRT) for menopausal symptoms had a 99% lower risk of developing BPPV compared with those who did not.104 In this study, the impact of HRT on bone density was not considered. This population study does not indicate that HRT is indicated as a treatment for BPPV, but suggests a correlation exists. For more information about menopausal symptoms and hormone replacement see Life Extension’s Female Hormone Restoration protocol.
Sleep Apnea
The periodic low blood oxygen levels characteristic of sleep apnea may damage the delicate structures of the vestibular system,37,105 which could increase the risk of peripheral vertigo. In one population study, people with sleep apnea were found to have about 1.7-fold higher risk of experiencing vertigo than those without sleep apnea.38 In another study, people with sleep apnea were found to have higher rates of vestibular migraine, Ménière disease, and hearing loss than the general population.106 Furthermore, patients with more severe obstructive sleep apnea were found to have higher levels of dizziness-related disability than those with mild sleep apnea.37 Patients with sleep apnea and Ménière disease experienced a reduction in Ménière disease symptoms, including dizziness, when their sleep apnea was treated with a continuous positive airway pressure (CPAP) device.36 Refer to Life Extension’s Sleep Apnea protocol for more information.
Depression and Other Mental Health Concerns
There is a high prevalence of anxiety, depression, and other emotional, psychiatric, and cognitive disorders in people with vertigo.107-110 In one study of patients with BPPV, 39% had anxiety or depression, and 28% had a personality disorder.111 One study found canalith repositioning treatment in BPPV was less likely to work in people with anxiety and depression, and the likelihood for recurrence was higher.112 Some researchers have proposed that the vestibular system, in addition to supporting balance control, may participate in perception, cognition, and consciousness. Vestibular dysfunction may therefore play a role in psychiatric and cognitive disorders, even in the absence of vertigo.113 For more information, refer to Life Extension’s protocols on anxiety and depression.
6 Diagnosis
Differential Diagnosis
The most urgent diagnostic priority in patients who present with vertigo and dizziness is ruling out urgent causes, such as stroke.3,57,114 Other neurologic signs and symptoms can be clues that a stroke has occurred, such as numbness or weakness of a limb or face, difficulty swallowing, or speech or language difficulties, but sometimes dizziness or vertigo is the only symptom. Therefore, a thorough evaluation may be undertaken.57
Once urgent causes are ruled out, the next step in diagnosis involves ruling out the most common causes. In general, about 40% of patients with dizziness have peripheral vestibular dysfunction, 10% have central brainstem vestibular lesions, 15% have psychiatric disorders, and 25% have other problems such as presyncope and disequilibrium; in the remaining 10%, the cause is unknown.115
Physical Examination
Clinicians may be able to rule out certain causes of dizziness by observing the presence and pattern of nystagmus (involuntary, rapid eye movements) or other eye movement abnormalities.8 Nystagmus is usually evaluated by slowly moving an object and asking the patient to follow it with their gaze, but not their head. Tests involving movements of the head or covering and uncovering each eye may be used to discern the pattern of nystagmus or other abnormal eye movements.116
BPPV can be diagnosed with a specialized maneuver called the Dix-Hallpike test. A clinician performs this test by assisting the patient in rapidly rotating their head while moving from a seated to lying position. If the maneuver recreates vertigo (with or without nystagmus), it points to BPPV as the cause. However, a negative result does not rule out BPPV.16,116
Blood pressure and heart rate in the standing and sitting positions can be measured to diagnose orthostatic hypotension (the inability to maintain normal blood pressure upon rising from a seated or lying position).116 Balance, gait, and neurologic signs also help a clinician determine whether the vertigo is of peripheral or central origin.2
Other Testing
Blood tests may be ordered to help identify possible causes of dizziness and vertigo such as anemia, infection, and thyroid or autoimmune disease, and hearing tests may be used to detect problems related to the inner ear, or the cranial nerve or brain region involved in hearing. A doctor may order imaging tests such as magnetic resonance imaging (MRI) and computed tomography (CT) scans if central causes are suspected.116
Emerging Diagnostic Strategies
Serum protein S100-beta is a novel diagnostic biomarker of neurological injury, and blood levels may be useful in distinguishing neurological origins from other possible causes.117 Recent findings suggest this protein may someday be used in acute care settings to differentiate vertigo caused by stroke from vertigo due to other causes.118-120
Vestibular evoked myogenic potentials are electrical signals that can be measured in the neck or eye muscles and may provide valuable diagnostic information about the function of the vestibular system. Tests measuring these electrical signals are gaining popularity and may help refine the diagnosis of vertigo, although variability in the different available methods remains a challenge.121,122
7 Treatment
Treatment of vertigo depends upon the cause.
Benign Paroxysmal Positional Vertigo (BPPV)
With no treatment, over 60% of patients with BPPV recover within four weeks.23 However, episodes of vertigo (especially recurrent vertigo) can substantially undermine quality of life and increase the risk of falls in elderly people.123,124 Therefore, treatment is recommended for people who are experiencing BPPV.
Canalith repositioning procedures, which are designed to move debris out of the semicircular canals, are frequently used to treat positional vertigo.16 The Semont and Epley maneuvers are among the most widely used repositioning procedures and are effective in the majority of cases.125 One trial found that a combination of methods, including these two, resolved 98% of cases of one-sided posterior BPPV.126
At-home repositioning maneuvers provide alternatives for patients who are unable to go into the clinic for treatment. The half-somersault maneuver is a technique developed for at-home use without assistance. The half-somersault maneuver was compared with an at-home version of the Epley maneuver in 68 people with positional vertigo. Those who used the half somersault experienced less dizziness and other complications during the procedure. They were also more likely to remain in remission six months after treatment.24 A how-to guide for performing the half-somersault maneuver has been developed by Carol Foster, MD, and is available on her website.
BPPV often occurs in combination with additional vestibular abnormalities. In these cases, symptoms can remain even after successful repositioning treatment and movement of the canaliths or debris which were lodged in the posterior or horizontal semicircular canals. A more complete diagnostic workup may then be necessary to identify the causes of lingering symptoms.16
Vestibular Migraine
Vestibular migraine is managed with similar treatments used for migraine headaches, although their efficacy for vestibular migraine is not well-studied. Preventive management includes avoiding triggers and using migraine prophylactic medication, which can include69:
- Beta-blockers
- Tricyclic antidepressants
- Anti-seizure medications
- Serotonin-norepinephrine reuptake inhibitors (SNRIs), particularly when vestibular symptoms predominate (can worsen headaches)
- Verapamil, when vertigo manifests in the context of migraine aura
For acute attacks of vertigo, the following vestibular suppressants can be considered69:
- Antihistamines
- Antiemetics
- Benzodiazepines
Ménière Disease
Initial therapy in Ménière disease should be dietary and lifestyle adjustments. This includes reduction in salt intake, caffeine, alcohol, and monosodium glutamate (MSG). Environmental and lifestyle triggers should also be addressed, and can include nicotine, stress, and food or environmental allergies.18,59 During Ménière disease attacks, vestibular suppressants (medications that may help attenuate the vertigo and nystagmus associated with vestibular imbalance) such as antihistamines and benzodiazepines can reduce the symptoms of vertigo, while antiemetics also may be needed acutely if nausea and vomiting exist. Anticholinergic drugs (eg, scopolamine, atropine) can also be used to suppress Ménière disease attacks.59 Chronic symptoms can be treated with betahistine (Serc) (a histamine signaling modulator), available as a compounded preparation in the United States, or diuretics. Glucocorticoids such as prednisone are used to treat difficult cases that do not respond adequately to first-line pharmacologic or other treatments. These can be administered orally or directly into the inner ear.18 The American Academy of Otolaryngology recommends inner ear injection of steroids for patients who do not respond to conventional treatment.59
Other Treatment Considerations
Vestibular rehabilitation. Vestibular rehabilitation is an exercise program intended to reduce vertigo and dizziness, instability, and falls. The goal of vestibular rehabilitation is to promote compensation, a process through which other senses, such as vision, are trained to substitute for the vestibular system. Over time, vestibular rehabilitation can encourage the nervous system to adapt to changes in nerve signaling within the balance control network. Vestibular rehabilitation incorporates three types of exercise, which are individualized according to patients’ specific concerns127:
- Habituation. Reduces dizziness or vertigo caused by self-motion or visual stimuli
- Gaze stabilization. Improves control of eye movements to maintain stable vision during movement of the head
- Balance training. Improves steadiness to facilitate daily activities, such as self-care, work, and recreation
Surgery. Surgery is available as a last resort to treat intractable peripheral vertigo. There are two categories of vestibular surgery: corrective and destructive. Corrective surgery is meant to repair or stabilize inner ear function, whereas destructive surgery’s goal is to stop the inner ear from generating sensory information and transmitting it to the brain. The specific surgical procedure used is individualized based on the patient’s condition.128
8 Novel and Emerging Strategies
Calcium Channel Blockers
Flunarizine (Sibelium) is a calcium channel blocker, and cinnarizine has antihistaminic, antiserotonergic, antidopaminergic, and calcium-channel-blocking activites. They are approved in many countries for migraine prevention (flunarizine) and management of vestibular symptoms and prevention of motion sickness (cinnarizine). As of early 2021, neither medication is approved for any indication in the United States.20,21,129 In a randomized controlled trial, flunarizine was an effective adjunct treatment for migraine-associated vertigo. In 48 patients over 12 weeks, treatment with flunarizine, betahistine, and acetaminophen was compared with betahistine and acetaminophen alone. There was a significant decrease in frequency and severity of episodes of migrainous vertigo in the flunarizine group, and no significant difference between the two groups in the incidence of the most frequent adverse effects.22
Cinnarizine has been evaluated in combination with other vestibular suppressants. A combination of dimenhydrinate and cinnarizine significantly improved peripheral vestibular vertigo symptoms after four weeks of therapy compared with betahistine alone.130 Similarly, cinnarizine combined with betahistine improved vertigo symptoms over either treatment alone in a clinical trial of 162 patients.131
Piracetam
Piracetam, a derivative of the neurotransmitter gamma-aminobutyric acid (GABA),132 has been investigated as a treatment option for Ménière disease. In a randomized controlled trial of 100 patients with Ménière disease who presented to the emergency department for vertigo, participants received either betahistine (dosed at 8 mg every eight hours) or piracetam (800 mg every eight hours). After seven days of treatment, vertigo recurrence occurred at a similar rate in patients treated with piracetam and betahistine (6% in both groups).133,134 In an open-label observational study in patients with peripheral vestibular vertigo, over 1,600 patients received either piracetam combined with betahistine or betahistine alone. The effect of the combination was superior across multiple indices, including a reduction in dizziness-related functional deficits by 2.3-fold compared with betahistine alone.135
Biofeedback Therapy
Another promising field of research for individuals with chronic or recurrent vertigo of various etiologies is biofeedback therapy. Specific biofeedback techniques can be integrated into vestibular rehabilitation programs. One innovative proposed method is based on the use of computer-generated cues about posture and position that encourage adaptation and improved balance.136 In one study, five weeks of twice-weekly biofeedback therapy reduced swaying and instability and decreased reaction times in 73% of the 37 vertigo-affected participants.137 Similar positive results have been observed in several other studies.138-142
9 Dietary And Lifestyle Considerations
Diet
A low-sodium diet is a commonly used management strategy for Ménière disease, as is avoidance of caffeine, although conclusive evidence from rigorous controlled trials is still lacking for these interventions.59,143 In a survey of patients with Ménière disease, those who followed a low-sodium and caffeine-free diet for more than six months had a greater improvement in vertigo symptoms.144
Certain food additives or constituents may trigger migraines or worsen symptoms of Ménière disease in susceptible individuals. These include nitrates, nitrites, tyramine, aspartame, and monosodium glutamate, as well as caffeine and alcohol.145 Examples of common foods that may provoke symptoms include red wine, beer, chocolate, fermented dairy products including yogurt, and aged or pickled foods. Some practitioners advise patients younger than 50 years who have Ménière disease to eliminate these foods.146 However, no rigorous controlled trials of dietary changes in Ménière disease have been performed,147 and some clinicians have expressed skepticism of the effectiveness of dietary intervention. Nonetheless, if a pattern of Ménière disease episodes can be attributed to certain dietary intakes, it is reasonable and safe to avoid certain foods. More information about dietary migraine triggers, which may be of interest to individuals with Ménière disease, is available in Life Extension’s Migraine protocol.
Some studies have discovered an association between positional vertigo and abnormalities in glucose and insulin metabolism. A diet rich in whole foods from plants, such as the Mediterranean diet, which helps improve blood sugar metabolism, may have potential as an adjunctive treatment in positional vertigo.15,148-150
Relaxation Techniques
Individuals suffering from vertigo are more likely to experience depression, anxiety, and/or other psychological conditions.110 Two case reports from one team of authors in Japan reported that autogenic training, a body-mind technique that uses imagery and body awareness to induce a relaxed state, has shown benefit in Ménière disease and psychogenic vertigo.151,152 Relaxation techniques such as mindfulness-based stress reduction, relaxation response training, and cognitive-behavioral stress management have shown therapeutic benefits in managing emotional stress,153 and may prove useful for treating vertigo as well as the psychological issues that may be caused by or contribute to it. Life Extension’s Stress Management protocol describes additional relaxation strategies which may be useful for all sufferers of vertigo as the condition can be stressful for all who experience it.
10 Nutrients
Vitamin D and Calcium
Low vitamin D status has been observed in patients with BPPV, especially in those with chronic recurrent vertigo.154,155 In one study, subjects with vitamin D levels between 10 and 20 ng/mL had 3.8-fold greater odds of having positional vertigo compared with controls whose levels were above 20 ng/mL, while among subjects with severe vitamin D deficiency (≤10 ng/mL) the odds of having the condition were dramatically greater than that.156
In a large, multicenter, randomized, controlled trial, 957 patients with BPPV who had received successful treatment with canalith repositioning maneuvers were randomized to ongoing care with a combination of vitamin D and calcium or observation only. Those in the intervention group who were given 400 IU (10 mcg) vitamin D daily along with 500 mg calcium carbonate twice daily for one year had a 24% lower annual risk of BPPV recurrence.41 Similarly, in a meta-analysis of five clinical trials, vitamin D supplementation (as daily or high bolus doses, with or without calcium) was shown to reduce the risk of BPPV recurrence by 63%.157 In a study of 93 participants with BPPV and severe vitamin D deficiency, subjects were given a loading dose of 50,000 IU (1,250 mcg) vitamin D3 three times weekly for one month, then once every two weeks for two more months. The degree of vertigo improvement over a three-month period following initiation of the vitamin D3 loading dose was correlated with the amount of increase in vitamin D level. In those whose vitamin D status improved by 10 ng/mL or more, only 14% experienced vertigo recurrence. However, in those whose vitamin D level improved by less than 10 ng/mL, 43% experienced an episode of vertigo.98
In a double-blind controlled trial, 39 older adults with BPPV and vitamin D levels <30 ng/mL were randomized to receive 2,000 IU (50 mcg) vitamin D daily for 13 weeks, followed by 1,000 IU (25 mcg) vitamin D daily for 13 weeks, or placebo. Fourteen additional individuals with vitamin D levels ≥30 ng/mL at baseline only received dietary advice on maintaining vitamin D levels. At a 12-month follow up, participants in the vitamin D group showed an 87% reduction in recurrence rates of BPPV compared with placebo. Furthermore, there was no significant difference in recurrence rates between those randomized to vitamin D treatment and individuals with vitamin D levels ≥30 ng/mL. These results support the inclusion of vitamin D as standard care in adults with BPPV, particularly those with vitamin D deficiency.191
One study and one meta-analysis failed to find a significant correlation between vitamin D levels and BPPV when comparing patients and controls. However, a subgroup analysis (as part of the meta-analysis) found significantly lower vitamin D levels in those with recurring BPPV compared to those with non-recurring BPPV.158,159 Separate meta-analyses examined the relationship between vitamin D levels and BPPV incidence and recurrence in 19 studies (7,387 individuals) and seven studies (6,220 individuals), respectively, and found a negative correlation between vitamin D levels and BPPV first incidence, but an uncertain relationship with BPPV recurrence.192 Another meta-analysis of seven studies comprised of 1,333 individuals found that vitamin D supplementation reduced the recurrence rate of BPPV by 59% in patients with vitamin D deficiency.193
Ginkgo Biloba
Extracts of ginkgo biloba, one of the oldest living species of trees in the world,160 are used in many countries for the treatment for vertigo.161 In a 12-week randomized controlled trial in 160 subjects with peripheral vertigo, 79% of patients who received 120 mg of a ginkgo standardized extract twice daily (providing 22.0–27.0% ginkgo flavonoids and 5.0–7.0% terpene lactones) rated symptoms as “very much improved” or “much improved” from baseline while only 70% of those treated with 16 mg twice daily of the drug betahistine had the same level of improvement.162 Additionally, ginkgo was better tolerated. In an earlier trial in people with vestibular vertigo, 80 mg of the same ginkgo extract twice per day for three months was approximately as effective as 16 mg of betahistine twice daily.163
Although the precise mechanism of ginkgo biloba’s effectiveness for vertigo is unknown, there is evidence from a rodent model that ginkgo extract enhances neuronal plasticity, and aids reorganization in a variety of central nervous system structures that govern vestibular function. In that study, the administration of ginkgo extract resulted in faster recovery of balance and improved neuronal connectivity following acute inner ear damage.164
Ginger Root
Zingiber officinale (ginger) root has been used traditionally to treat digestive, inflammatory, and infectious ailments.165 A randomized controlled trial found one gram of powdered ginger strongly prevented symptoms of seasickness, including vertigo.166 Another placebo-controlled clinical trial showed ginger prevented vertigo significantly better than placebo in healthy adult subjects who underwent vestibular stimulation to induce vertigo.167 Ginger is an effective remedy for some forms of nausea168 and could be considered for treating nausea resulting from vertigo-related conditions.
Vitamin B12
Vitamin B12 is essential for normal neurological function, and B12 deficiency can cause a wide range of neurological and psychiatric symptoms, including vertigo and dizziness.169,170 In a case-control study, mean vitamin B12 levels were significantly lower in 114 patients newly diagnosed with BPPV compared with controls.171 In a case report, an elderly patient with dizziness and imbalance was found to have vitamin B12 deficiency and elevated homocysteine levels. B12 injection therapy resulted in a dramatic response, including improvement in dizziness, in this patient.172 A study in 100 people with neurological symptoms that included dizziness and instability found that 15% of subjects had deficient or borderline low vitamin B12 levels.173
Vitamin B6
There is some historical record of vitamin B6 supplementation being used to successfully treat vertigo.174,175 Additionally, in two separate double-blind clinical trials, 20 healthy individuals were given the antibiotic minocycline (Minocin) seven times over three days in order to induce vertigo, nystagmus, and nausea. The addition of 40 mg vitamin B6 at each dose markedly reduced these side effects.176
Magnesium
Migraine has been effectively treated with oral magnesium supplementation,177-179 and magnesium supplementation may be beneficial in migraine-associated vertigo. A meta-analysis of randomized clinical trials found that, in cardiac patients, magnesium orotate supplementation reduced risk of dizziness by 78%.180 Magnesium might reduce the incidence of vestibular migraine through modulation of vascular tone and thus cerebral blood flow,181 which plays a role in the development of vestibular migraine.182
Coenzyme Q10
Coenzyme Q10 (CoQ10) is centrally involved in cellular energy production in the mitochondria and has been studied for the treatment of cardiovascular disease.183,184 In one trial, 2,664 patients with congestive heart failure were treated with 50–150 mg CoQ10 daily. After three months of treatment, 73% of participants with vertigo reported improvement in their vertigo.185 CoQ10 was shown in a mouse model to protect delicate inner ear cells from age-related decline and ward off hearing loss, leading one team of scientists to suggest it could also protect against vestibular disorders that can lead to vertigo.186,187
Glutathione and Vitamin C
Glutathione is an antioxidant that plays a critical role in several cellular processes, including scavenging reactive oxygen species and nutrient metabolism.188 Patients with BPPV, Ménière disease, and some types of centrally caused vertigo have been shown to have higher levels of oxidative stress compared with healthy individuals.66,67,189 An uncontrolled trial in 22 treatment-resistant patients with Ménière disease evaluated oral administration of 300 mg per day rebamipide (an oxidative stress medication not available in the United States) along with 600 mg per day vitamin C and/or 300 mg per day glutathione for eight weeks. Twenty-one of the 22 patients with vertigo reported complete recovery or substantial improvement. The authors concluded that oxidative stress reducers could hold potential as a treatment for Ménière disease.190
Disclaimer and Safety Information
This information (and any accompanying material) is not intended to replace the attention or advice of a physician or other qualified health care professional. Anyone who wishes to embark on any dietary, drug, exercise, or other lifestyle change intended to prevent or treat a specific disease or condition should first consult with and seek clearance from a physician or other qualified health care professional. Pregnant women in particular should seek the advice of a physician before using any protocol listed on this website. The protocols described on this website are for adults only, unless otherwise specified. Product labels may contain important safety information and the most recent product information provided by the product manufacturers should be carefully reviewed prior to use to verify the dose, administration, and contraindications. National, state, and local laws may vary regarding the use and application of many of the therapies discussed. The reader assumes the risk of any injuries. The authors and publishers, their affiliates and assigns are not liable for any injury and/or damage to persons arising from this protocol and expressly disclaim responsibility for any adverse effects resulting from the use of the information contained herein.
The protocols raise many issues that are subject to change as new data emerge. None of our suggested protocol regimens can guarantee health benefits. Life Extension has not performed independent verification of the data contained in the referenced materials, and expressly disclaims responsibility for any error in the literature.
- Furman JM. Causes of vertigo. UptoDate. Updated 8/24/2018. Accessed 11/3/2020, https://www.uptodate.com/contents/causes-of-vertigo
- Furman JM, Barton JJ. Evaluation of the patient with vertigo. UptoDate. Updated 2/11/2020. Accessed 11/3/2020, https://www.uptodate.com/contents/evaluation-of-the-patient-with-vertigo
- Kerber KA. Vertigo and dizziness in the emergency department. Emerg Med Clin North Am. Feb 2009;27(1):39-50, viii. doi:10.1016/j.emc.2008.09.002
- Susanto M. Dizziness: if not vertigo could it be cardiac disease? Australian family physician. 5/01 2014;43:264-269.
- Healthwise Staff. Dizziness: Lightheadedness and Vertigo: Topic Overview. Michigan Medicine: University of Michigan. Updated 6/26/2019. Accessed 1/12/2021, https://www.uofmhealth.org/health-library/dizzi
- Wipperman J. Dizziness and vertigo. Primary care. Mar 2014;41(1):115-31. doi:10.1016/j.pop.2013.10.004
- Susanto M. Dizziness: if not vertigo could it be cardiac disease? Aust Fam Physician. May 2014;43(5):264-9.
- Post RE, Dickerson LM. Dizziness: a diagnostic approach. American family physician. Aug 15 2010;82(4):361-8, 369.
- Samuels MA, Pomerantz BJ, Sadow PM. Case records of the Massachusetts General Hospital. Case 14-2010. A 54-year-old woman with dizziness and falls. The New England journal of medicine. May 13 2010;362(19):1815-23. doi:10.1056/NEJMcpc0910070
- Lin HW, Bhattacharyya N. Balance disorders in the elderly: epidemiology and functional impact. The Laryngoscope. Aug 2012;122(8):1858-61. doi:10.1002/lary.23376
- Neuhauser HK. The epidemiology of dizziness and vertigo. Handbook of clinical neurology. 2016;137:67-82. doi:10.1016/B978-0-444-63437-5.00005-4
- Fernandez L, Breinbauer HA, Delano PH. Vertigo and Dizziness in the Elderly. Frontiers in neurology. 2015;6:144. doi:10.3389/fneur.2015.00144
- Ciorba A, Bianchini C, Scanelli G, Pala M, Zurlo A, Aimoni C. The impact of dizziness on quality-of-life in the elderly. European archives of oto-rhino-laryngology : official journal of the European Federation of Oto-Rhino-Laryngological Societies (EUFOS) : affiliated with the German Society for Oto-Rhino-Laryngology - Head and Neck Surgery . Mar 2017;274(3):1245-1250. doi:10.1007/s00405-016-4222-z
- Holmes S, Padgham ND. A review of the burden of vertigo. J Clin Nurs. Oct 2011;20(19-20):2690-701. doi:10.1111/j.1365-2702.2010.03585.x
- Agrawal Y, Ward BK, Minor LB. Vestibular dysfunction: prevalence, impact and need for targeted treatment. Journal of vestibular research : equilibrium & orientation. 2013;23(3):113-7. doi:10.3233/VES-130498
- Bhattacharyya N, Gubbels SP, Schwartz SR, et al. Clinical Practice Guideline: Benign Paroxysmal Positional Vertigo (Update). Otolaryngology--head and neck surgery : official journal of American Academy of Otolaryngology-Head and Neck Surgery . Mar 2017;156(3_suppl):S1-S47. doi:10.1177/0194599816689667
- Furman JM, Barton JJ. Treatment of vertigo. UptoDate. Updated 8/7/2018. Accessed 11/3/2020, https://www.uptodate.com/contents/treatment-of-vertigo
- Moskowitz HS, Dinces EA. Meniere disease: Evaluation, diagnosis, and management. UptoDate. Updated 6/23/2020. Accessed 11/3/2020, https://www.uptodate.com/contents/meniere-disease-evaluation-diagnosis-and-management?search=vertigo&source=search_result&selectedTitle=10~150&usage_type=default&display_rank=10
- Hitier M, Barbier C, Marie-Aude T, Moreau S, Courtheoux P, Patron V. New treatment of vertigo caused by jugular bulb abnormalities. Surg Innov. Aug 2014;21(4):365-71. doi:10.1177/1553350613505918
- Lexicomp. UpToDate. Flunarizine (United States: Not available): Drug information. Accessed 12/3/20, https://www.uptodate.com/contents/flunarizine-united-states-not-available-drug-information
- Lexicomp. UpToDate. Cinnarizine: International drug information (concise). Accessed 12/3/2020, https://www.uptodate.com/contents/cinnarizine-international-drug-information-concise
- Lepcha A, Amalanathan S, Augustine AM, Tyagi AK, Balraj A. Flunarizine in the prophylaxis of migrainous vertigo: a randomized controlled trial. European archives of oto-rhino-laryngology : official journal of the European Federation of Oto-Rhino-Laryngological Societies (EUFOS) : affiliated with the German Society for Oto-Rhino-Laryngology - Head and Neck Surgery . Nov 2014;271(11):2931-6. doi:10.1007/s00405-013-2786-4
- Strupp M, Dieterich M, Brandt T. The treatment and natural course of peripheral and central vertigo. Deutsches Arzteblatt international . Jul 2013;110(29-30):505-15; quiz 515-6. doi:10.3238/arztebl.2013.0505
- Foster CA, Ponnapan A, Zaccaro K, Strong D. A Comparison of Two Home Exercises for Benign Positional Vertigo: Half Somersault versus Epley Maneuver. Audiology and Neurotology Extra. 2012;2(1):16-23. doi:10.1159/000337947
- Brandt T, Steddin S, Daroff RB. Therapy for benign paroxysmal positioning vertigo, revisited. Neurology. May 1994;44(5):796-800. doi:10.1212/wnl.44.5.796
- Barton JJ. UpToDate. Benign paroxysmal positional vertigo. Updated 12/17/2018. Accessed 11/3/2020, https://www.uptodate.com/contents/benign-paroxysmal-positional-vertigo?search=vertigo&source=search_result&selectedTitle=4~150&usage_type=default&display_rank=4
- Kelm Z, Klapchar K, Kieliszak CR, Selinsky C. Psychogenic Dizziness: An Important but Overlooked Differential Diagnosis in the Workup of the Dizzy Patient. J Am Osteopath Assoc. May 1 2018;118(5):e22-e27. doi:10.7556/jaoa.2018.066
- Albernaz PL. Hearing Loss, Dizziness, and Carbohydrate Metabolism. International archives of otorhinolaryngology. Jul 2016;20(3):261-70. doi:10.1055/s-0035-1558450
- Kirtane MV, Medikeri SB, Rao P. Blood levels of glucose and insulin in Meniere's disease. Acta oto-laryngologica Supplementum. 1983/01/01 1984;406(sup406):42-5. doi:10.3109/00016488309123000
- D'Avila C, Lavinsky L. Glucose and insulin profiles and their correlations in Meniere's disease. The international tinnitus journal. 2005;11(2):170-6.
- Serra AP, Lopes Kde C, Dorigueto RS, Gananca FF. Blood glucose and insulin levels in patients with peripheral vestibular disease. Brazilian journal of otorhinolaryngology. Sep-Oct 2009;75(5):701-5.
- Webster G, Sens PM, Salmito MC, et al. Hyperinsulinemia and hyperglycemia: risk factors for recurrence of benign paroxysmal positional vertigo. Brazilian journal of otorhinolaryngology. Jul-Aug 2015;81(4):347-51. doi:10.1016/j.bjorl.2014.09.008
- Yu S, Liu F, Cheng Z, Wang Q. Association between osteoporosis and benign paroxysmal positional vertigo: a systematic review. BMC Neurol. May 20 2014;14:110. doi:10.1186/1471-2377-14-110
- Byun H, Chung JH, Lee SH, Park CW, Kim EM, Kim I. Increased risk of benign paroxysmal positional vertigo in osteoporosis: a nationwide population-based cohort study. Sci Rep. Mar 5 2019;9(1):3469. doi:10.1038/s41598-019-39830-x
- Sowerby LJ, Rotenberg B, Brine M, George CF, Parnes LS. Sleep apnea, daytime somnolence, and idiopathic dizziness--a novel association. The Laryngoscope. Jun 2010;120(6):1274-8. doi:10.1002/lary.20899
- Nakayama M, Masuda A, Ando KB, et al. A Pilot Study on the Efficacy of Continuous Positive Airway Pressure on the Manifestations of Meniere's Disease in Patients with Concomitant Obstructive Sleep Apnea Syndrome. Journal of clinical sleep medicine : JCSM : official publication of the American Academy of Sleep Medicine . Oct 15 2015;11(10):1101-7. doi:10.5664/jcsm.5080
- Kayabasi S, Iriz A, Cayonu M, et al. Vestibular functions were found to be impaired in patients with moderate-to-severe obstructive sleep apnea. The Laryngoscope. May 2015;125(5):1244-8. doi:10.1002/lary.25021
- Tsai MS, Lee LA, Tsai YT, et al. Sleep apnea and risk of vertigo: A nationwide population-based cohort study. The Laryngoscope. Mar 2018;128(3):763-768. doi:10.1002/lary.26789
- Rea PA, Ronan N. Systemic Disease Considerations in the Management of the Dizzy Patient. Adv Otorhinolaryngol. 2019;82:150-163. doi:10.1159/000490284
- Spiegel R, Kalla R, Mantokoudis G, et al. Ginkgo biloba extract EGb 761((R)) alleviates neurosensory symptoms in patients with dementia: a meta-analysis of treatment effects on tinnitus and dizziness in randomized, placebo-controlled trials. Clin Interv Aging. 2018;13:1121-1127. doi:10.2147/CIA.S157877
- Jeong SH, Kim JS, Kim HJ, et al. Prevention of benign paroxysmal positional vertigo with vitamin D supplementation: A randomized trial. Neurology. Sep 1 2020;95(9):e1117-e1125. doi:10.1212/WNL.0000000000010343
- Kumar A, Kaur H, Devi P, Mohan V. Role of coenzyme Q10 (CoQ10) in cardiac disease, hypertension and Meniere-like syndrome. Pharmacology & therapeutics. Dec 2009;124(3):259-68. doi:10.1016/j.pharmthera.2009.07.003
- Purves D, Augustine GJ, Fitzpatrick D, et al. The Otoligh Organs: The Utricle and Sacculus. Neuroscience. 2nd ed. Sinauer Associates; 2001.
- Stanton M, Freeman AM. Vertigo. StatPearls Publishing. Updated 11/19/2020. Accessed 1/12/2021, https://www.ncbi.nlm.nih.gov/books/NBK482356/
- Blaussen.com staff. EarAnatomy: The Inner Ear. Wikimedia Commons. Updated 10/25/2020. Accessed 2/16/2021, https://en.wikipedia.org/wiki/Inner_ear#/media/File:Blausen_0329_EarAnatomy_InternalEar.png
- Park MK, Lee DY, Kim YH. Risk Factors for Positional Vertigo and the Impact of Vertigo on Daily Life: The Korean National Health and Nutrition Examination Survey. J Audiol Otol. Jan 2019;23(1):8-14. doi:10.7874/jao.2018.00178
- Chen J, Zhao W, Yue X, Zhang P. Risk Factors for the Occurrence of Benign Paroxysmal Positional Vertigo: A Systematic Review and Meta-Analysis. Systematic Review. Frontiers in neurology. 2020-June-23 2020;11(506):506. doi:10.3389/fneur.2020.00506
- Ogun OA, Buki B, Cohn ES, Janky KL, Lundberg YW. Menopause and benign paroxysmal positional vertigo. Menopause (New York, NY). Aug 2014;21(8):886-9. doi:10.1097/GME.0000000000000190
- Chen ZJ, Chang CH, Hu LY, et al. Increased risk of benign paroxysmal positional vertigo in patients with anxiety disorders: a nationwide population-based retrospective cohort study. BMC psychiatry. Jul 15 2016;16(1):238. doi:10.1186/s12888-016-0950-2
- Hsu CL, Tsai SJ, Shen CC, Lu T, Hung YM, Hu LY. Risk of benign paroxysmal positional vertigo in patients with depressive disorders: a nationwide population-based cohort study. BMJ open. Mar 30 2019;9(3):e026936. doi:10.1136/bmjopen-2018-026936
- Monzani D, Genovese E, Rovatti V, Malagoli ML, Rigatelli M, Guidetti G. Life events and benign paroxysmal positional vertigo: a case-controlled study. Acta oto-laryngologica. Sep 2006;126(9):987-92. doi:10.1080/00016480500546383
- Gacek RR. A perspective on recurrent vertigo. ORL; journal for oto-rhino-laryngology and its related specialties . 2013;75(2):91-107. doi:10.1159/000348710
- Jeon Y, Lee H. Ramsay Hunt syndrome. J Dent Anesth Pain Med. Dec 2018;18(6):333-337. doi:10.17245/jdapm.2018.18.6.333
- Albrecht M, Levin M. UpToDate. Epidemiology, clinical manifestations, and diagnosis of herpes zoster. Updated 1/21/2019. Accessed 12/1/2020, https://www.uptodate.com/contents/vestibular-neuritis-and-labyrinthitis?search=vertigo&topicRef=5101&source=see_link
- Wu V, Sykes EA, Beyea MM, Simpson MTW, Beyea JA. Approach to Meniere disease management. Canadian family physician Medecin de famille canadien. Jul 2019;65(7):463-467.
- Furman JM. UpToDate. Vestibular neuritis and labyrinthitis. Updated 7/29/2020. Accessed 12/01/2020, https://www.uptodate.com/contents/vestibular-neuritis-and-labyrinthitis?search=vertigo&topicRef=5101&source=see_link
- Saber Tehrani AS, Kattah JC, Kerber KA, et al. Diagnosing Stroke in Acute Dizziness and Vertigo: Pitfalls and Pearls. Stroke. Mar 2018;49(3):788-795. doi:10.1161/STROKEAHA.117.016979
- International Headache Society. IHS Classification ICHD-3. Accessed 12/1/2020, 2018. https://ichd-3.org/appendix/a1-migraine/a1-6-episodic-syndromes-that-may-be-associated-with-migraine/a1-6-6-vestibular-migraine/
- Basura GJ, Adams ME, Monfared A, et al. Clinical Practice Guideline: Meniere's Disease. Otolaryngology--head and neck surgery : official journal of American Academy of Otolaryngology-Head and Neck Surgery . Apr 2020;162(2_suppl):S1-S55. doi:10.1177/0194599820909438
- Barkwill D, Arora R. Labyrinthitis. StatPearls. StatPearls Publishing Copyright © 2021, StatPearls Publishing LLC.; 2021.
- Brosel S, Laub C, Averdam A, Bender A, Elstner M. Molecular aging of the mammalian vestibular system. Ageing Res Rev. Mar 2016;26:72-80. doi:10.1016/j.arr.2015.12.007
- Güçlütürk MT, Ünal ZN, İsmi O, Çimen MB, Ünal M. The Role of Oxidative Stress and Inflammatory Mediators in Benign Paroxysmal Positional Vertigo. J Int Adv Otol. Apr 2016;12(1):101-5. doi:10.5152/iao.2015.1412
- Şahin E, Deveci İ, Dinç ME, Özker BY, Biçer C, Erel Ö. Oxidative Status in Patients with Benign Paroxysmal Positional Vertigo. J Int Adv Otol . Aug 2018;14(2):299-303. doi:10.5152/iao.2018.4756
- Li J, Wu R, Xia B, Wang X, Xue M. Serum levels of superoxide dismutases in patients with benign paroxysmal positional vertigo. Biosci Rep. May 29 2020;40(5)doi:10.1042/bsr20193917
- Xie KH, Liu LL, Su CY, et al. Low Antioxidant Status of Serum Uric Acid, Bilirubin, Albumin, and Creatinine in Patients With Benign Paroxysmal Positional Vertigo. Front Neurol. 2020;11:601695. doi:10.3389/fneur.2020.601695
- Ishiyama G, Lopez IA, Acuna D, Ishiyama A. Investigations of the Microvasculature of the Human Macula Utricle in Meniere's Disease. Front Cell Neurosci. 2019;13:445. doi:10.3389/fncel.2019.00445
- Qian SX, Gu JX, Guan QB, Zhang XL, Wang YP. Serum oxidative stress, inflammatory response and platelet activation in patients with vascular vertigo. J Biol Regul Homeost Agents. Mar-Apr 2019;33(2):499-504.
- Cureoglu S, Baylan MY, Paparella MM. Cochlear otosclerosis. Current opinion in otolaryngology & head and neck surgery. Oct 2010;18(5):357-62. doi:10.1097/MOO.0b013e32833d11d9
- Robertson C, Eggers S. UpToDate. Vestibular migraine. Updated 10/30/2020. Accessed 12/1/2020, https://www.uptodate.com/contents/vestibular-migraine
- Formeister EJ, Rizk HG, Kohn MA, Sharon JD. The Epidemiology of Vestibular Migraine: A Population-based Survey Study. Otology & neurotology : official publication of the American Otological Society, American Neurotology Society [and] European Academy of Otology and Neurotology . Sep 2018;39(8):1037-1044. doi:10.1097/MAO.0000000000001900
- Edvinsson L. Role of CGRP in Migraine. Handbook of experimental pharmacology. 2019;255:121-130. doi:10.1007/164_2018_201
- Ohno K, Takeda N, Tanaka-Tsuji M, Matsunaga T. Calcitonin gene-related peptide in the efferent system of the inner ear. A review. Acta oto-laryngologica Supplementum. 1993;501:16-20. doi:10.3109/00016489309126206
- Chu CH, Liu CJ, Lin LY, Chen TJ, Wang SJ. Migraine is associated with an increased risk for benign paroxysmal positional vertigo: a nationwide population-based study. The journal of headache and pain. 2015;16:62. doi:10.1186/s10194-015-0547-z
- Radtke A, Lempert T, Gresty MA, Brookes GB, Bronstein AM, Neuhauser H. Migraine and Meniere's disease: is there a link? Neurology. Dec 10 2002;59(11):1700-4. doi:10.1212/01.wnl.0000036903.22461.39
- Neff BA, Staab JP, Eggers SD, et al. Auditory and vestibular symptoms and chronic subjective dizziness in patients with Meniere's disease, vestibular migraine, and Meniere's disease with concomitant vestibular migraine. Otology & neurotology : official publication of the American Otological Society, American Neurotology Society [and] European Academy of Otology and Neurotology . Sep 2012;33(7):1235-44. doi:10.1097/MAO.0b013e31825d644a
- Chimirri S, Aiello R, Mazzitello C, et al. Vertigo/dizziness as a Drugs' adverse reaction. Journal of pharmacology & pharmacotherapeutics. Dec 2013;4(Suppl 1):S104-9. doi:10.4103/0976-500X.120969
- Altissimi G, Colizza A, Cianfrone G, et al. Drugs inducing hearing loss, tinnitus, dizziness and vertigo: an updated guide. European review for medical and pharmacological sciences. Aug 2020;24(15):7946-7952. doi:10.26355/eurrev_202008_22477
- Lin E, Aligene K. Pharmacology of balance and dizziness. NeuroRehabilitation. 2013;32(3):529-42. doi:10.3233/NRE-130875
- Castellanos MJ, Fuente A. The Adverse Effects of Heavy Metals with and without Noise Exposure on the Human Peripheral and Central Auditory System: A Literature Review. International journal of environmental research and public health. Dec 9 2016;13(12):1223. doi:10.3390/ijerph13121223
- Cassidy J, Misset JL. Oxaliplatin-related side effects: characteristics and management. Seminars in oncology. Oct 2002;29(5 Suppl 15):11-20. doi:10.1053/sonc.2002.35524
- Giacomini PG, Napolitano B, Alessandrini M, Di Girolamo S, Magrini A. Recurrent paroxysmal positional vertigo related to oral contraceptive treatment. Gynecological endocrinology : the official journal of the International Society of Gynecological Endocrinology . Jan 2006;22(1):5-8. doi:10.1080/09513590500441614
- Caruso S, Mauro D, Maiolino L, Grillo C, Rapisarda AMC, Cianci S. Effects of combined oral contraception containing drospirenone on premenstrual exacerbation of Meniere's disease: Preliminary study. European journal of obstetrics, gynecology, and reproductive biology . May 2018;224:102-107. doi:10.1016/j.ejogrb.2018.03.015
- Ledesma AL, Barreto MA, Bahmad F, Jr. Caffeine effect in vestibular system. The international tinnitus journal. 2014;19(1):77-81. doi:10.5935/0946-5448.20140011
- Leung AK, Hon KL. Motion sickness: an overview. Drugs in context. 2019;8:2019-9-4. doi:10.7573/dic.2019-9-4
- Schmal F. Neuronal mechanisms and the treatment of motion sickness. Pharmacology. 2013;91(3-4):229-41. doi:10.1159/000350185
- Marx W, Ried K, McCarthy AL, et al. Ginger-Mechanism of action in chemotherapy-induced nausea and vomiting: A review. Crit Rev Food Sci Nutr. Jan 2 2017;57(1):141-146. doi:10.1080/10408398.2013.865590
- Lazzini S, Polinelli W, Riva A, Morazzoni P, Bombardelli E. The effect of ginger (Zingiber officinalis) and artichoke (Cynara cardunculus) extract supplementation on gastric motility: a pilot randomized study in healthy volunteers. European review for medical and pharmacological sciences. 2016;20(1):146-9.
- Kim HA, Yi HA, Lee H. Recent advances in orthostatic hypotension presenting orthostatic dizziness or vertigo. Neurol Sci. Nov 2015;36(11):1995-2002. doi:10.1007/s10072-015-2363-2
- Kim SY, Kim HJ, Min C, Choi HG. Association between benign paroxysmal positional vertigo and osteoporosis: two nested case-control studies. Osteoporosis international : a journal established as result of cooperation between the European Foundation for Osteoporosis and the National Osteoporosis Foundation of the USA . Oct 2020;31(10):2017-2024. doi:10.1007/s00198-020-05478-x
- Yamanaka T, Shirota S, Sawai Y, Murai T, Fujita N, Hosoi H. Osteoporosis as a risk factor for the recurrence of benign paroxysmal positional vertigo. The Laryngoscope. Nov 2013;123(11):2813-6. doi:10.1002/lary.24099
- Mikulec AA, Kowalczyk KA, Pfitzinger ME, Harris DA, Jackson LE. Negative association between treated osteoporosis and benign paroxysmal positional vertigo in women. The Journal of laryngology and otology. Apr 2010;124(4):374-6. doi:10.1017/S002221510999209X
- Wu Y, Fan Z, Jin H, et al. Assessment of Bone Metabolism in Male Patients With Benign Paroxysmal Positional Vertigo. Frontiers in neurology. 2018;9:742. doi:10.3389/fneur.2018.00742
- Wang Z, Yao G, Tao X, Zhang J, Zhang T, Wu Z. Evaluation of bone mineral density and 25-(OH) vitamin D levels in middle-aged and elderly women with recurrent benign paroxysmal positional vertigo. Acta oto-laryngologica. Feb 2020;140(2):89-93. doi:10.1080/00016489.2019.1692146
- Yang CJ, Kim Y, Lee HS, Park HJ. Bone mineral density and serum 25-hydroxyvitamin D in patients with idiopathic benign paroxysmal positional vertigo. Journal of vestibular research : equilibrium & orientation. 2018;27(5-6):287-294. doi:10.3233/VES-170625
- Bazoni JA, Ciquinato DSA, Marquez AS, Costa VSP, Marchiori GM, Marchiori LLM. Hypovitaminosis D, Low Bone Mineral Density, and Diabetes Mellitus as Probable Risk Factors for Benign Paroxysmal Positional Vertigo in the Elderly. International archives of otorhinolaryngology. Jul 2020;24(3):e272-e277. doi:10.1055/s-0039-1700583
- Rhim GI. Serum vitamin D and recurrent benign paroxysmal positional vertigo. Laryngoscope investigative otolaryngology. Dec 2016;1(6):150-153. doi:10.1002/lio2.35
- Talaat HS, Abuhadied G, Talaat AS, Abdelaal MS. Low bone mineral density and vitamin D deficiency in patients with benign positional paroxysmal vertigo. European archives of oto-rhino-laryngology : official journal of the European Federation of Oto-Rhino-Laryngological Societies (EUFOS) : affiliated with the German Society for Oto-Rhino-Laryngology - Head and Neck Surgery . Sep 2015;272(9):2249-53. doi:10.1007/s00405-014-3175-3
- Talaat HS, Kabel AM, Khaliel LH, Abuhadied G, El-Naga HA, Talaat AS. Reduction of recurrence rate of benign paroxysmal positional vertigo by treatment of severe vitamin D deficiency. Auris, nasus, larynx. Jun 2016;43(3):237-41. doi:10.1016/j.anl.2015.08.009
- Nakada T, Teranishi M, Ueda Y, Sone M. Fracture probability assessed using FRAX((R)) in elderly women with benign paroxysmal positional vertigo. Auris, nasus, larynx. Dec 2018;45(6):1173-1177. doi:10.1016/j.anl.2018.05.002
- Liao WL, Chang TP, Chen HJ, Kao CH. Benign paroxysmal positional vertigo is associated with an increased risk of fracture: a population-based cohort study. J Orthop Sports Phys Ther. May 2015;45(5):406-12. doi:10.2519/jospt.2015.5707
- Jumani K, Powell J. Benign Paroxysmal Positional Vertigo: Management and Its Impact on Falls. Ann Otol Rhinol Laryngol. Aug 2017;126(8):602-605. doi:10.1177/0003489417718847
- Jeong S-H. Benign Paroxysmal Positional Vertigo Risk Factors Unique to Perimenopausal Women. Frontiers in neurology. 2020;11:589605-589605. doi:10.3389/fneur.2020.589605
- Han W, Fan Z, Zhou M, et al. Low 25-hydroxyvitamin D levels in postmenopausal female patients with benign paroxysmal positional vertigo. Acta oto-laryngologica. May 2018;138(5):443-446. doi:10.1080/00016489.2017.1416168
- Liu DH, Kuo CH, Wang CT, et al. Age-Related Increases in Benign Paroxysmal Positional Vertigo Are Reversed in Women Taking Estrogen Replacement Therapy: A Population-Based Study in Taiwan. Frontiers in aging neuroscience. 2017;9:404. doi:10.3389/fnagi.2017.00404
- Gallina S, Dispenza F, Kulamarva G, Riggio F, Speciale R. Obstructive sleep apnoea syndrome (OSAS): effects on the vestibular system. Acta otorhinolaryngologica Italica : organo ufficiale della Societa italiana di otorinolaringologia e chirurgia cervico-facciale . Dec 2010;30(6):281-4.
- Foster CA, Machala M. The Clinical Spectrum of Dizziness in Sleep Apnea. Otology & neurotology : official publication of the American Otological Society, American Neurotology Society [and] European Academy of Otology and Neurotology . Dec 2020;41(10):1419-1422. doi:10.1097/MAO.0000000000002824
- Peluso ET, Quintana MI, Gananca FF. Anxiety and depressive disorders in elderly with chronic dizziness of vestibular origin. Brazilian journal of otorhinolaryngology. Mar-Apr 2016;82(2):209-14. doi:10.1016/j.bjorl.2015.04.015
- Bigelow RT, Semenov YR, du Lac S, Hoffman HJ, Agrawal Y. Vestibular vertigo and comorbid cognitive and psychiatric impairment: the 2008 National Health Interview Survey. J Neurol Neurosurg Psychiatry. Apr 2016;87(4):367-72. doi:10.1136/jnnp-2015-310319
- Ketola S, Havia M, Appelberg B, Kentala E. Psychiatric symptoms in vertiginous patients. Nordic journal of psychiatry. May 2015;69(4):287-91. doi:10.3109/08039488.2014.972976
- Lahmann C, Henningsen P, Brandt T, et al. Psychiatric comorbidity and psychosocial impairment among patients with vertigo and dizziness. J Neurol Neurosurg Psychiatry. Mar 2015;86(3):302-8. doi:10.1136/jnnp-2014-307601
- Kozak HH, Dundar MA, Uca AU, et al. Anxiety, Mood, and Personality Disorders in Patients with Benign Paroxysmal Positional Vertigo. Noro Psikiyatr Ars. Mar 2018;55(1):49-53. doi:10.5152/npa.2016.18143
- Wei W, Sayyid ZN, Ma X, Wang T, Dong Y. Presence of Anxiety and Depression Symptoms Affects the First Time Treatment Efficacy and Recurrence of Benign Paroxysmal Positional Vertigo. Frontiers in neurology. 2018;9:178. doi:10.3389/fneur.2018.00178
- Gurvich C, Maller JJ, Lithgow B, Haghgooie S, Kulkarni J. Vestibular insights into cognition and psychiatry. Brain research. Nov 6 2013;1537:244-59. doi:10.1016/j.brainres.2013.08.058
- von Brevern M. Acute dizziness and vertigo: The bedside testing is essential. Journal of neurosciences in rural practice. Apr-Jun 2015;6(2):133-4. doi:10.4103/0976-3147.153213
- Branch WT, Barton JJ. Approach to the patient with dizziness. UptoDate. Updated 2/12/2020. Accessed 11/3/2020, https://www.uptodate.com/contents/approach-to-the-patient-with-dizziness?search=vertigo&source=search_result&selectedTitle=6~150&usage_type=default&display_rank=6
- Muncie HL, Sirmans SM, James E. Dizziness: Approach to Evaluation and Management. American family physician. Feb 1 2017;95(3):154-162.
- Yardan T, Erenler AK, Baydin A, Aydin K, Cokluk C. Usefulness of S100B protein in neurological disorders. J Pak Med Assoc. Mar 2011;61(3):276-81.
- Sohn JH, Kim CH, Lee SH, Kim JH, Lee JJ. Diagnostic Value of Serum Biomarkers for Differentiating Central and Peripheral Causes of Acute Vertigo. Original Research. Front Med (Lausanne). 2020-March-19 2020;7(84):84. doi:10.3389/fmed.2020.00084
- Kartal AG, Yilmaz S, Yaka E, et al. Diagnostic value of S100B protein in the differential diagnosis of acute vertigo in the emergency department. Academic emergency medicine : official journal of the Society for Academic Emergency Medicine . Jul 2014;21(7):736-41. doi:10.1111/acem.12420
- Purrucker JC, Herrmann O, Lutsch JK, et al. Serum protein S100beta is a diagnostic biomarker for distinguishing posterior circulation stroke from vertigo of nonvascular causes. European neurology. 2014;72(5-6):278-84. doi:10.1159/000363569
- Rosengren SM, Colebatch JG, Young AS, Govender S, Welgampola MS. Vestibular evoked myogenic potentials in practice: Methods, pitfalls and clinical applications. Clin Neurophysiol Pract. 2019;4:47-68. doi:10.1016/j.cnp.2019.01.005
- Venhovens J, Meulstee J, Verhagen WIM. Vestibular evoked myogenic potentials (VEMPs) in central neurological disorders. Clinical neurophysiology : official journal of the International Federation of Clinical Neurophysiology . Jan 2016;127(1):40-49. doi:10.1016/j.clinph.2014.12.021
- Oghalai JS, Manolidis S, Barth JL, Stewart MG, Jenkins HA. Unrecognized benign paroxysmal positional vertigo in elderly patients. Otolaryngology--head and neck surgery : official journal of American Academy of Otolaryngology-Head and Neck Surgery . May 2000;122(5):630-4. doi:10.1067/mhn.2000.105415
- Gamiz MJ, Lopez-Escamez JA. Health-related quality of life in patients over sixty years old with benign paroxysmal positional vertigo. Gerontology. Mar-Apr 2004;50(2):82-6. doi:10.1159/000075558
- Mandala M, Salerni L, Nuti D. Benign Positional Paroxysmal Vertigo Treatment: a Practical Update. Curr Treat Options Neurol. Dec 5 2019;21(12):66. doi:10.1007/s11940-019-0606-x
- Gaur S, Awasthi SK, Bhadouriya SK, Saxena R, Pathak VK, Bisht M. Efficacy of Epley's Maneuver in Treating BPPV Patients: A Prospective Observational Study. International journal of otolaryngology. 2015;2015:487160. doi:10.1155/2015/487160
- VeDA. Vestibular rehabilitation therapy (VRT). Accessed 12/3/20, https://vestibular.org/article/diagnosis-treatment/treatments/vestibular-rehabilitation-therapy-vrt/
- VeDA. Surgical procedures for vestibular dysfunction. Accessed 12/3/20, https://vestibular.org/article/diagnosis-treatment/treatments/surgical-procedures-for-vestibular-dysfunction/
- Haress NG. Cinnarizine: Comprehensive Profile. Profiles Drug Subst Excip Relat Methodol. 2015;40:1-41. doi:10.1016/bs.podrm.2015.01.001
- Scholtz AW, Hahn A, Stefflova B, et al. Efficacy and Safety of a Fixed Combination of Cinnarizine 20 mg and Dimenhydrinate 40 mg vs Betahistine Dihydrochloride 16 mg in Patients with Peripheral Vestibular Vertigo: A Prospective, Multinational, Multicenter, Double-Blind, Randomized, Non-inferiority Clinical Trial. Clinical drug investigation. Nov 2019;39(11):1045-1056. doi:10.1007/s40261-019-00858-6
- Asadi P, Zia Ziabari SM, Majdi A, Vatanparast K, Naseri Alavi SA. Cinnarizine/betahistine combination vs. the respective monotherapies in acute peripheral vertigo: a randomized triple-blind placebo-controlled trial. Eur J Clin Pharmacol. Nov 2019;75(11):1513-1519. doi:10.1007/s00228-019-02741-x
- PubChem, Natinoal Library of Medicine. Compound Summary: Piracetam. Accessed 2/5/2021, https://pubchem.ncbi.nlm.nih.gov/compound/Piracetam
- Arhami Dolatabadi A, Larimi SR, Safaie A. Oral Piracetam vs Betahistine in Outpatient Management of Peripheral Vertigo; a Randomized Clinical Trial. Arch Acad Emerg Med. 2019;7(1):e9-e9.
- Dyhrfjeld-Johnsen J, Attali P. Management of peripheral vertigo with antihistamines: New options on the horizon. Br J Clin Pharmacol. Oct 2019;85(10):2255-2263. doi:10.1111/bcp.14046
- Melnikov OA, Lilenko SV, Nauta J, Ouwens MJ. Betahistine plus piracetam dual therapy versus betahistine monotherapy for peripheral vestibular vertigo: a confounder-corrected subanalysis of the OSVaLD study. Curr Med Res Opin. Nov 2015;31(11):1951-62. doi:10.1185/03007995.2015.1067193
- Kornilova LN, Temnikova VV, Naumov IA, Ekimovskii GA, Solov'eva AD. [Computer-aided techniques for the treatment and rehabilitation of patients suffering vertigo and balance disorders]. Vestnik otorinolaringologii. 2010;(6):38-43.
- Perez N, Santandreu E, Benitez J, Rey-Martinez J. Improvement of postural control in patients with peripheral vestibulopathy. European archives of oto-rhino-laryngology : official journal of the European Federation of Oto-Rhino-Laryngological Societies (EUFOS) : affiliated with the German Society for Oto-Rhino-Laryngology - Head and Neck Surgery . May 2006;263(5):414-20. doi:10.1007/s00405-005-1027-x
- Mraz M, Curzytek M, Mraz MA, Gawron W, Czerwosz L, Skolimowski T. Body balance in patients with systemic vertigo after rehabilitation exercise. Journal of physiology and pharmacology : an official journal of the Polish Physiological Society . Nov 2007;58 Suppl 5(Pt 1):427-36.
- Luchikhin LA, Ganichkina I, Doronina OM. [Biological feedback techniques in rehabilitation of patients with impaired equilibrium function]. Vestnik otorinolaringologii. 2002;(2):18-20. Metodika biologicheskoi obratnoi sviazi v reabilitatsii bol'nykh s narusheniem funktsii ravnovesiia.
- Bittar RS, Barros Cde G. Vestibular rehabilitation with biofeedback in patients with central imbalance. Brazilian journal of otorhinolaryngology. Jun 2011;77(3):356-61. doi:10.1590/s1808-86942011000300014
- Moasa G, Amer H, El-Nasag B, Bahrawy S, M Ahmed G. Biofeedback Training in Treatment of Vertigo Secondary to Cervical Lesions. 03/01 2017:147-153.
- Antonenko LM, Parfenov VA. [Non-drug therapy of vertigo]. Zh Nevrol Psikhiatr Im S S Korsakova. 2018;118(8):38-42. Nelekarstvennye metody lecheniia golovokruzheniia. doi:10.17116/jnevro201811808138
- Shim T, Strum DP, Mudry A, Monfared A. Hold the Salt: History of Salt Restriction as a First-line Therapy for Meniere's Disease. Otology & neurotology : official publication of the American Otological Society, American Neurotology Society [and] European Academy of Otology and Neurotology . Jul 2020;41(6):855-859. doi:10.1097/MAO.0000000000002635
- Luxford E, Berliner KI, Lee J, Luxford WM. Dietary modification as adjunct treatment in Meniere's disease: patient willingness and ability to comply. Otology & neurotology : official publication of the American Otological Society, American Neurotology Society [and] European Academy of Otology and Neurotology . Oct 2013;34(8):1438-43. doi:10.1097/MAO.0b013e3182942261
- Sun-Edelstein C, Mauskop A. Foods and supplements in the management of migraine headaches. Clin J Pain. Jun 2009;25(5):446-52. doi:10.1097/AJP.0b013e31819a6f65
- Foster CA. Optimal management of Meniere's disease. Therapeutics and clinical risk management. 2015;11:301-7. doi:10.2147/TCRM.S59023
- Hussain K, Murdin L, Schilder AG. Restriction of salt, caffeine and alcohol intake for the treatment of Meniere's disease or syndrome. The Cochrane database of systematic reviews. Dec 31 2018;12(12):CD012173. doi:10.1002/14651858.CD012173.pub2
- Schultz AR, Neves-Souza RD, Costa Vde S, Meneses-Barriviera CL, Franco PP, Marchiori LL. Is There a Possible Association between Dietary Habits and Benign Paroxysmal Positional Vertigo in the Elderly? The Importance of Diet and Counseling. International archives of otorhinolaryngology. Oct 2015;19(4):293-7. doi:10.1055/s-0035-1551551
- De Natale C, Annuzzi G, Bozzetto L, et al. Effects of a plant-based high-carbohydrate/high-fiber diet versus high-monounsaturated fat/low-carbohydrate diet on postprandial lipids in type 2 diabetic patients. Diabetes Care. Dec 2009;32(12):2168-73. doi:10.2337/dc09-0266
- Esposito K, Maiorino MI, Bellastella G, Chiodini P, Panagiotakos D, Giugliano D. A journey into a Mediterranean diet and type 2 diabetes: a systematic review with meta-analyses. BMJ open. 2015;5(8):e008222. doi:10.1136/bmjopen-2015-008222
- Goto F, Nakai K, Kunihiro T, Ogawa K. Phobic postural vertigo treated with autogenic training: a case report. Cases journal. Sep 30 2008;1(1):189. doi:10.1186/1757-1626-1-189
- Goto F, Nakai K, Kunihiro T, Ogawa K. Case report: a case of intractable Meniere's disease treated with autogenic training. BioPsychoSocial medicine. Jan 25 2008;2:3. doi:10.1186/1751-0759-2-3
- Crawford C, Wallerstedt DB, Khorsan R, Clausen SS, Jonas WB, Walter JA. A systematic review of biopsychosocial training programs for the self-management of emotional stress: potential applications for the military. Evidence-based complementary and alternative medicine : eCAM. 2013/09/23 2013;2013:747694. doi:10.1155/2013/747694
- Yang B, Lu Y, Xing D, et al. Association between serum vitamin D levels and benign paroxysmal positional vertigo: a systematic review and meta-analysis of observational studies. European archives of oto-rhino-laryngology : official journal of the European Federation of Oto-Rhino-Laryngological Societies (EUFOS) : affiliated with the German Society for Oto-Rhino-Laryngology - Head and Neck Surgery . Jan 2020;277(1):169-177. doi:10.1007/s00405-019-05694-0
- Buki B, Ecker M, Junger H, Lundberg YW. Vitamin D deficiency and benign paroxysmal positioning vertigo. Med Hypotheses. Feb 2013;80(2):201-4. doi:10.1016/j.mehy.2012.11.029
- Jeong SH, Kim JS, Shin JW, et al. Decreased serum vitamin D in idiopathic benign paroxysmal positional vertigo. J Neurol. Mar 2013;260(3):832-8. doi:10.1007/s00415-012-6712-2
- Jeong SH, Lee SU, Kim JS. Prevention of recurrent benign paroxysmal positional vertigo with vitamin D supplementation: a meta-analysis. J Neurol. Aug 7 2020;doi:10.1007/s00415-020-09952-8
- AlGarni MA, Mirza AA, Althobaiti AA, Al-Nemari HH, Bakhsh LS. Association of benign paroxysmal positional vertigo with vitamin D deficiency: a systematic review and meta-analysis. European archives of oto-rhino-laryngology : official journal of the European Federation of Oto-Rhino-Laryngological Societies (EUFOS) : affiliated with the German Society for Oto-Rhino-Laryngology - Head and Neck Surgery . Nov 2018;275(11):2705-2711. doi:10.1007/s00405-018-5146-6
- Karatas A, Acar Yuceant G, Yuce T, Haci C, Cebi IT, Salviz M. Association of Benign Paroxysmal Positional Vertigo with Osteoporosis and Vitamin D Deficiency: A Case Controlled Study. J Int Adv Otol. Aug 2017;13(2):259-265. doi:10.5152/iao.2016.2640
- Klein J. The Secret That Helps Some Trees Live More Than 1,000 Years. New York Times. Accessed 12/3/2020, January 13, 2020. https://www.nytimes.com/2020/01/13/science/oldest-trees-ginkgos.html
- Agus S, Benecke H, Thum C, Strupp M. Clinical and Demographic Features of Vertigo: Findings from the REVERT Registry. Frontiers in neurology . 2013;4:48. doi:10.3389/fneur.2013.00048
- Sokolova L, Hoerr R, Mishchenko T. Treatment of Vertigo: A Randomized, Double-Blind Trial Comparing Efficacy and Safety of Ginkgo biloba Extract EGb 761 and Betahistine. International journal of otolaryngology. 2014;2014:682439. doi:10.1155/2014/682439
- Cesarani A, Meloni F, Alpini D, Barozzi S, Verderio L, Boscani PF. Ginkgo biloba (EGb 761) in the treatment of equilibrium disorders. Adv Ther. Sep-Oct 1998;15(5):291-304.
- Lindner M, Gosewisch A, Eilles E, et al. Ginkgo biloba Extract EGb 761 Improves Vestibular Compensation and Modulates Cerebral Vestibular Networks in the Rat. Frontiers in neurology. 2019;10:147. doi:10.3389/fneur.2019.00147
- Haniadka R, Saldanha E, Sunita V, Palatty PL, Fayad R, Baliga MS. A review of the gastroprotective effects of ginger (Zingiber officinale Roscoe). Food Funct. Jun 2013;4(6):845-55. doi:10.1039/c3fo30337c
- Grontved A, Brask T, Kambskard J, Hentzer E. Ginger root against seasickness. A controlled trial on the open sea. Acta oto-laryngologica. Jan-Feb 1988;105(1-2):45-9. doi:10.3109/00016488809119444
- Grontved A, Hentzer E. Vertigo-reducing effect of ginger root. A controlled clinical study. ORL; journal for oto-rhino-laryngology and its related specialties . 1986;48(5):282-6. doi:10.1159/000275883
- Giacosa A, Morazzoni P, Bombardelli E, Riva A, Bianchi Porro G, Rondanelli M. Can nausea and vomiting be treated with ginger extract? European review for medical and pharmacological sciences. Apr 2015;19(7):1291-6.
- Clarke R, Refsum H, Birks J, et al. Screening for vitamin B-12 and folate deficiency in older persons. Am J Clin Nutr. May 2003;77(5):1241-7. doi:10.1093/ajcn/77.5.1241
- Briani C, Dalla Torre C, Citton V, et al. Cobalamin deficiency: clinical picture and radiological findings. Nutrients. Nov 15 2013;5(11):4521-39. doi:10.3390/nu5114521
- Tekesin A, Tunc A. Inflammatory biomarkers in benign paroxysmal positional vertigo: A Turkey case-control study. Ideggyogyaszati szemle. Nov 30 2018;71(11-12):411-416. Gyulladasos biomarkerek benignus paroxysmalis pozicionalis vertigoban: torokorszagi eset-kontroll vizsgalat. doi:10.18071/isz.71.0411
- Singh B, Arora S. Acute presentation of dizziness in vitamin B12 deficient old patient of cardiac disease: a case report. Clin Chim Acta. Dec 14 2010;411(23-24):2104-6. doi:10.1016/j.cca.2010.08.022
- Mahajan SK, Aundhakar SC. A study of the prevalence of serum vitamin B12 and folic Acid deficiency in Western maharashtra. Journal of family medicine and primary care. Jan-Mar 2015;4(1):64-8. doi:10.4103/2249-4863.152255
- Lewy A, Fox N. Pyridoxine (B6) used in the treatment of vertigo. Arch Otolaryngol. Nov 1947;46(5):681-3. doi:10.1001/archotol.1947.00690020697010
- Lewy A, Fox N. The use of pyridoxin (B-6) in vertigo; clinical note. Ann Otol Rhinol Laryngol. Mar 1948;57(1):258-61.
- Claussen CF, Claussen E. [Antivertiginous action of vitamin B 6 on experimental minocycline-induced vertigo in man]. Arzneimittel-Forschung. Mar 1988;38(3):396-9. Antivertiginose Wirkung von Vitamin B 6 beim experimentellen, durch Minocyclin ausgelosten Schwindel des Menschen.
- Obermann M, Strupp M. Current treatment options in vestibular migraine. Mini Review. Frontiers in neurology. 2014-December-04 2014;5(257):257. doi:10.3389/fneur.2014.00257
- Peikert A, Wilimzig C, Kohne-Volland R. Prophylaxis of migraine with oral magnesium: results from a prospective, multi-center, placebo-controlled and double-blind randomized study. Cephalalgia. Jun 1996;16(4):257-63. doi:10.1046/j.1468-2982.1996.1604257.x
- Chiu HY, Yeh TH, Huang YC, Chen PY. Effects of Intravenous and Oral Magnesium on Reducing Migraine: A Meta-analysis of Randomized Controlled Trials. Pain physician. Jan 2016;19(1):E97-112.
- Torshin IY, Gromova OA, Kalacheva AG, Oshchepkova EV, Martynov AI. [Meta-analysis of clinical trials of cardiovascular effects of magnesium orotate]. Terapevticheskii arkhiv. 2015;87(6):88-97. doi:10.17116/terarkh201587688-97
- Kolte D, Vijayaraghavan K, Khera S, Sica DA, Frishman WH. Role of magnesium in cardiovascular diseases. Cardiology in review. Jul-Aug 2014;22(4):182-92. doi:10.1097/CRD.0000000000000003
- Furman JM, Marcus DA, Balaban CD. Vestibular migraine: clinical aspects and pathophysiology. The Lancet Neurology. 2013/07/01/ 2013;12(7):706-715. doi:https://doi.org/10.1016/S1474-4422(13)70107-8
- Genova ML, Lenaz G. New developments on the functions of coenzyme Q in mitochondria. BioFactors (Oxford, England). Sep-Oct 2011;37(5):330-54. doi:10.1002/biof.168
- Yang YK, Wang LP, Chen L, et al. Coenzyme Q10 treatment of cardiovascular disorders of ageing including heart failure, hypertension and endothelial dysfunction. Clin Chim Acta. Oct 23 2015;450:83-9. doi:10.1016/j.cca.2015.08.002
- Baggio E, Gandini R, Plancher AC, Passeri M, Carmosino G. Italian multicenter study on the safety and efficacy of coenzyme Q10 as adjunctive therapy in heart failure. CoQ10 Drug Surveillance Investigators. Molecular aspects of medicine. 1994;15 Suppl:s287-94. doi:10.1016/0098-2997(94)90040-x
- Someya S, Xu J, Kondo K, et al. Age-related hearing loss in C57BL/6J mice is mediated by Bak-dependent mitochondrial apoptosis. Proc Natl Acad Sci U S A. Nov 17 2009;106(46):19432-7. doi:10.1073/pnas.0908786106
- Iwasaki S, Yamasoba T. Dizziness and Imbalance in the Elderly: Age-related Decline in the Vestibular System. Aging Dis. Feb 2015;6(1):38-47. doi:10.14336/AD.2014.0128
- Aquilano K, Baldelli S, Ciriolo MR. Glutathione: new roles in redox signaling for an old antioxidant. Review. Frontiers in Pharmacology. 2014-August-26 2014;5(196)doi:10.3389/fphar.2014.00196
- Sahin E, Deveci I, Dinc ME, Ozker BY, Bicer C, Erel O. Oxidative Status in Patients with Benign Paroxysmal Positional Vertigo. J Int Adv Otol . Aug 2018;14(2):299-303. doi:10.5152/iao.2018.4756
- Takumida M, Anniko M, Ohtani M. Radical scavengers for Meniere's disease after failure of conventional therapy: a pilot study. Acta oto-laryngologica. Aug 2003;123(6):697-703. doi:10.1080/00016480310000728a
- Chua KW, Huang X, Koh XH, et al. Randomized Controlled Trial Assessing Vitamin D's Role in Reducing BPPV Recurrence in Older Adults. Otolaryngology--head and neck surgery : official journal of American Academy of Otolaryngology-Head and Neck Surgery. Jan 2025;172(1):127-136. doi:10.1002/ohn.954. https://www.ncbi.nlm.nih.gov/pubmed/39194424
- Wood H, Kluk K, BinKhamis G. Association between vitamin D deficiency and benign paroxysmal positional vertigo (BPPV) incidence and recurrence: a systematic review and meta-analysis. BMJ open. Apr 22 2024;14(4):e077986. doi:10.1136/bmjopen-2023-077986. https://www.ncbi.nlm.nih.gov/pubmed/38653514
- Yang Z, Li J, Zhu Z, He J, Wei X, Xie M. Effect of vitamin D supplementation on benign paroxysmal positional vertigo recurrence: A meta-analysis. Sci Prog. Apr-Jun 2021;104(2):368504211024569. doi:10.1177/00368504211024569. https://www.ncbi.nlm.nih.gov/pubmed/34128742
